Final ID: TU250
Racial Disparities in Mortality Trend of Pulmonary Heart Disease in the United States from 2018:2023: A Comprehensive Benchmarking Analysis
Abstract Body: Background: Pulmonary heart disease (PHD), often driven by chronic pulmonary vascular remodeling (ICD-10: I27), represents a critical and under-recognized cause of cardiopulmonary mortality in the U.S. While aggregate national trends show a slow rise, this masks acute, multi-level socio-geographic inequalities in risk.
Method: U.S. mortality data (ICD-10: I27) for 2018–2023 was extracted from CDC WONDER to estimate PHD deaths. Racial disparities were quantified using Average Annual Percent Change (AAPC) via log-linear regression, stratified by race, age, gender, Hispanic origin, education attainment, U.S. Census region, and 2013 urbanization classification
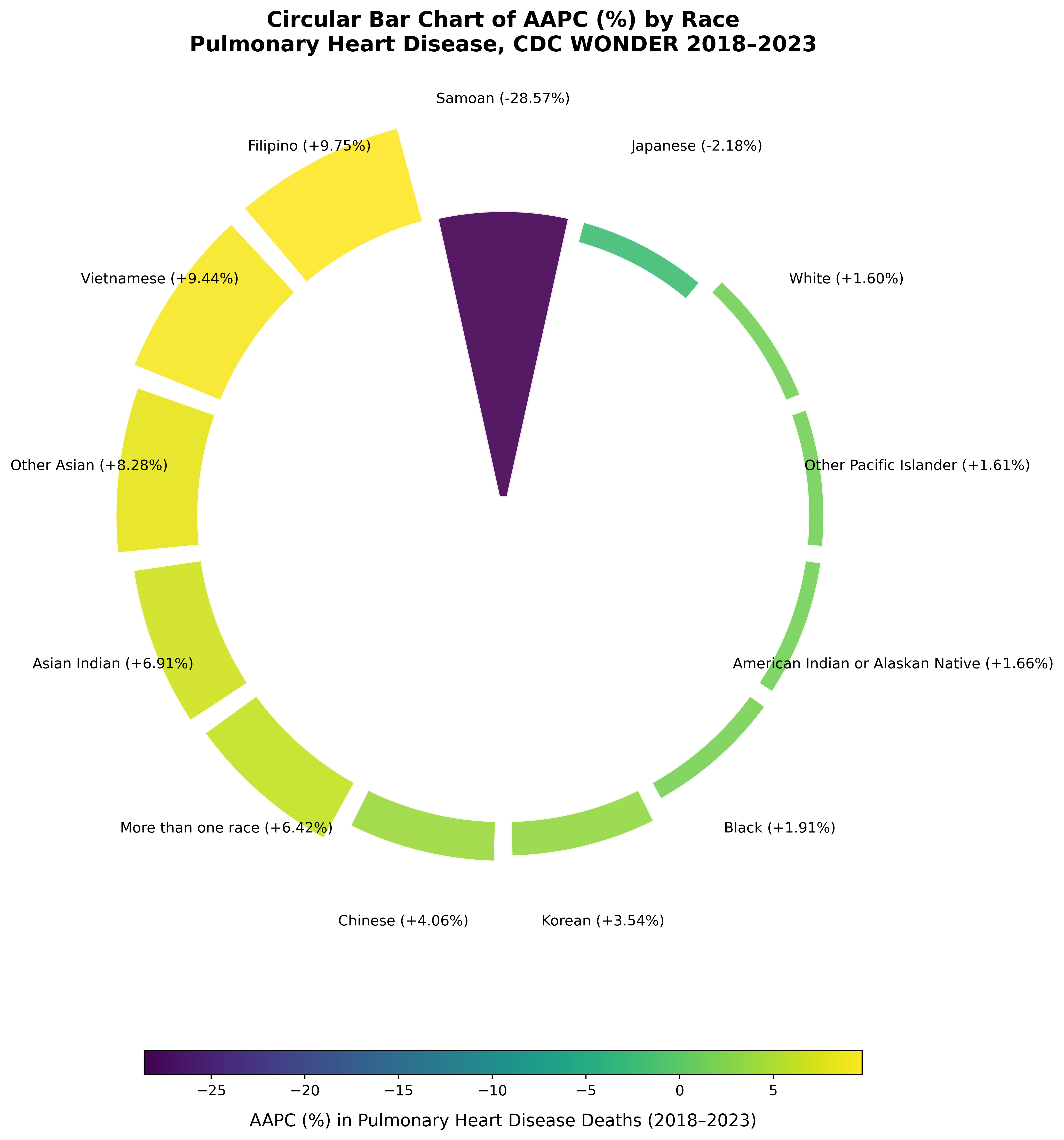
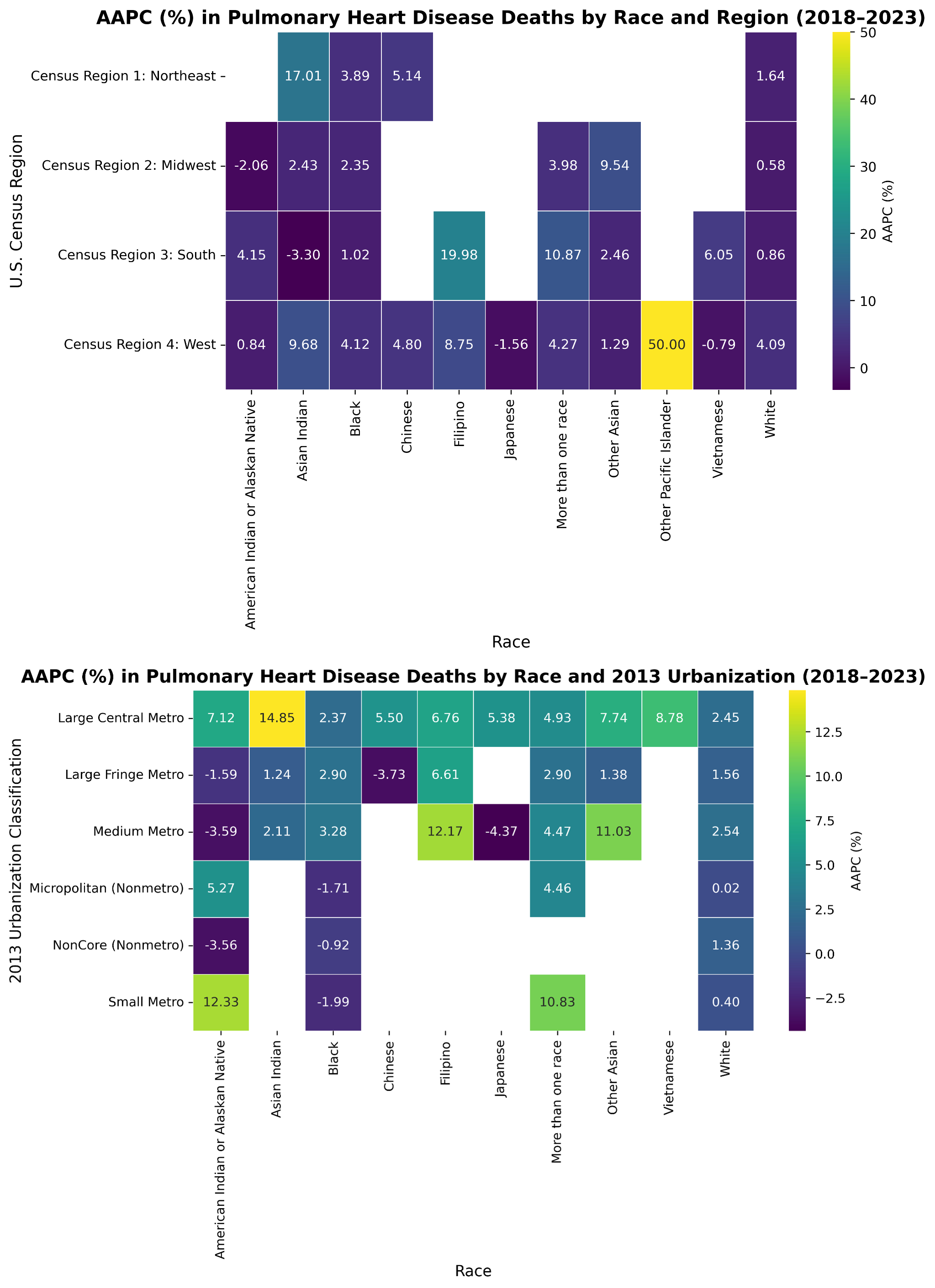
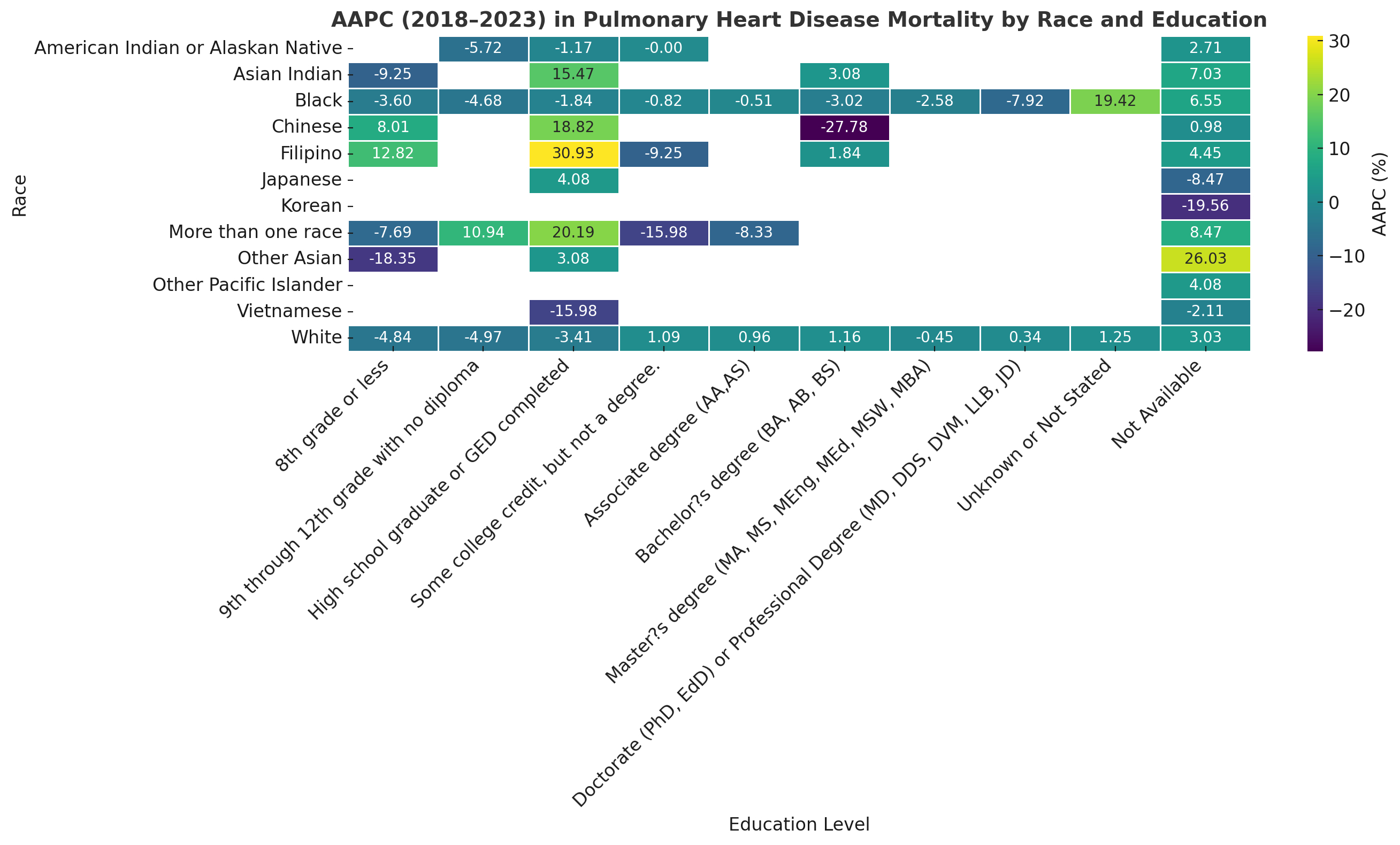
Results: Overall AAPC acceleration was driven by Asian and Pacific Islander (API) populations: Filipino (+12.82%), Vietnamese (+9.44%), and Asian Indian (+6.91%), contrasting sharply with overall declines for White (–4.84%) and Black (–3.60%) groups. Intersecting disparities were stark. By Region/Urbanization, the steepest rises were among Western Other Pacific Islanders (+50.0%), Southern Filipinos (+19.98%), and Asian Indians in large central metros (+14.85%), while Blacks in non-core rural areas declined (–0.92%). By Age/Education, the highest AAPC was found in Asian Indians aged 65–74 (+15.39%) and Non-Hispanic Filipinos with some college (+30.93%). Conversely, Black adults aged 85+ (–13.28%) and Chinese with bachelor’s degrees (–27.78%) showed significant mortality compression.
Conclusions: PHD mortality is not uniformly increasing; it is sharply accelerating in structurally marginalized API communities, younger age bands, and those in lower educational strata. These findings underscore the profound role of structural racism, differential care access, and urban-environmental exposure. Urgent disaggregation of national metrics and targeted, upstream preventive strategies for at-risk race-region-education cohorts are required.
Method: U.S. mortality data (ICD-10: I27) for 2018–2023 was extracted from CDC WONDER to estimate PHD deaths. Racial disparities were quantified using Average Annual Percent Change (AAPC) via log-linear regression, stratified by race, age, gender, Hispanic origin, education attainment, U.S. Census region, and 2013 urbanization classification
Results: Overall AAPC acceleration was driven by Asian and Pacific Islander (API) populations: Filipino (+12.82%), Vietnamese (+9.44%), and Asian Indian (+6.91%), contrasting sharply with overall declines for White (–4.84%) and Black (–3.60%) groups. Intersecting disparities were stark. By Region/Urbanization, the steepest rises were among Western Other Pacific Islanders (+50.0%), Southern Filipinos (+19.98%), and Asian Indians in large central metros (+14.85%), while Blacks in non-core rural areas declined (–0.92%). By Age/Education, the highest AAPC was found in Asian Indians aged 65–74 (+15.39%) and Non-Hispanic Filipinos with some college (+30.93%). Conversely, Black adults aged 85+ (–13.28%) and Chinese with bachelor’s degrees (–27.78%) showed significant mortality compression.
Conclusions: PHD mortality is not uniformly increasing; it is sharply accelerating in structurally marginalized API communities, younger age bands, and those in lower educational strata. These findings underscore the profound role of structural racism, differential care access, and urban-environmental exposure. Urgent disaggregation of national metrics and targeted, upstream preventive strategies for at-risk race-region-education cohorts are required.
More abstracts on this topic:
Dual Inhibition of Glutaminolysis and Pyruvate Carboxylase Attenuates Pulmonary Arterial Hypertension
Valuparampil Varghese Mathews, James Joel, Bharti Dinesh, Niihori Maki, Rafikova Olga, Rafikov Ruslan
BMP10 as novel marker for right atrial dilatation and pressure in precapillary pulmonary hypertensionLlucia-valldeperas Aida, Van Wezenbeek Jessie, Groeneveldt Joanne, Sanchez-duffhues Gonzalo, Vonk Noordegraaf Anton, Bogaard Harm, Goumans Marie Jose, De Man Frances