Final ID: MP1500
Discordantly Elevated Small Dense LDL-C Increases Risk of Cardiovascular Events in Hypertensive Adults: Insights from SPRINT
Abstract Body (Do not enter title and authors here): Background: Small dense low-density lipoprotein cholesterol (sdLDL-C) is highly atherogenic, yet its role in predicting cardiovascular disease (CVD) among individuals with hypertension is not well characterized.
Objective: To examine the association of sdLDL-C, its discordance with low-density lipoprotein cholesterol (LDL-C) and CVD risk in adults with hypertension.
Methods: In this analysis of the Systolic Blood Pressure Intervention Trial (SPRINT), baseline sdLDL-C was estimated using Sampson’s method, calculated by subtracting large buoyant LDL-C (estimated from LDL-C and ln[triglycerides]) from total LDL-C. Participants were stratified by cohort percentiles of sdLDL-C and LDL-C. Discordance was defined as a ≥10 percentile point difference between sdLDL-C and LDL-C. Participants were categorized as discordantly high (sdLDL-C ≥10 points higher), discordantly low (sdLDL-C ≥10 points lower), or concordant. Multivariable Cox regression estimated hazard ratios (HRs) and 95% confidence intervals (CIs) for associations with the primary composite outcome: myocardial infarction, stroke, acute coronary syndrome, acute heart failure, and CVD death. Analyses were repeated using clinical cutoffs: LDL-C ≥130 mg/dL and an aligned sdLDL-C threshold of 40.1 mg/dL based on cohort percentiles.
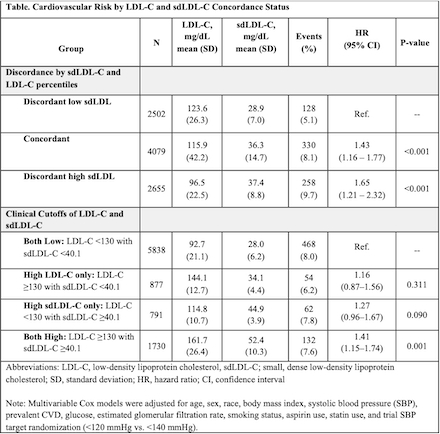
Results: Among 9,236 participants (mean age 67 years), 716 primary outcome events (7.8%) occurred over a median follow-up of 3.8 years. Each 1-SD increase in log-transformed sdLDL-C was independently associated with higher CVD risk (HR = 1.17; 95% CI: 1.08–1.26). Compared to the discordantly low group, concordant and discordantly high groups had 43% (HR = 1.43; 95% CI: 1.16–1.77) and 65% (HR = 1.65; 95% CI: 1.21–2.32) greater risk, respectively. Using clinical cutoffs, high sdLDL-C alone was associated with a 27% increased risk (HR = 1.27; 95% CI: 0.96–1.67), while those with both elevated LDL-C and sdLDL-C had a 41% higher risk (HR = 1.41; 95% CI: 1.15–1.74) compared to participants with both markers below threshold(Table).
Conclusion: In adults with hypertension, elevated sdLDL-C was associated with increased CVD risk. Discordantly high sdLDL-C conferred the highest risk. Using a clinical LDL-C threshold of 130 mg/dL, the greatest risk was seen in individuals with both high LDL-C and sdLDL-C, while those with low LDL-C but high sdLDL-C had a suggestive increase in risk. These findings highlight the potential role of sdLDL-C in identifying residual CVD risk not captured by LDL-C alone.
Objective: To examine the association of sdLDL-C, its discordance with low-density lipoprotein cholesterol (LDL-C) and CVD risk in adults with hypertension.
Methods: In this analysis of the Systolic Blood Pressure Intervention Trial (SPRINT), baseline sdLDL-C was estimated using Sampson’s method, calculated by subtracting large buoyant LDL-C (estimated from LDL-C and ln[triglycerides]) from total LDL-C. Participants were stratified by cohort percentiles of sdLDL-C and LDL-C. Discordance was defined as a ≥10 percentile point difference between sdLDL-C and LDL-C. Participants were categorized as discordantly high (sdLDL-C ≥10 points higher), discordantly low (sdLDL-C ≥10 points lower), or concordant. Multivariable Cox regression estimated hazard ratios (HRs) and 95% confidence intervals (CIs) for associations with the primary composite outcome: myocardial infarction, stroke, acute coronary syndrome, acute heart failure, and CVD death. Analyses were repeated using clinical cutoffs: LDL-C ≥130 mg/dL and an aligned sdLDL-C threshold of 40.1 mg/dL based on cohort percentiles.
Results: Among 9,236 participants (mean age 67 years), 716 primary outcome events (7.8%) occurred over a median follow-up of 3.8 years. Each 1-SD increase in log-transformed sdLDL-C was independently associated with higher CVD risk (HR = 1.17; 95% CI: 1.08–1.26). Compared to the discordantly low group, concordant and discordantly high groups had 43% (HR = 1.43; 95% CI: 1.16–1.77) and 65% (HR = 1.65; 95% CI: 1.21–2.32) greater risk, respectively. Using clinical cutoffs, high sdLDL-C alone was associated with a 27% increased risk (HR = 1.27; 95% CI: 0.96–1.67), while those with both elevated LDL-C and sdLDL-C had a 41% higher risk (HR = 1.41; 95% CI: 1.15–1.74) compared to participants with both markers below threshold(Table).
Conclusion: In adults with hypertension, elevated sdLDL-C was associated with increased CVD risk. Discordantly high sdLDL-C conferred the highest risk. Using a clinical LDL-C threshold of 130 mg/dL, the greatest risk was seen in individuals with both high LDL-C and sdLDL-C, while those with low LDL-C but high sdLDL-C had a suggestive increase in risk. These findings highlight the potential role of sdLDL-C in identifying residual CVD risk not captured by LDL-C alone.
More abstracts on this topic:
A drug target Mendelian randomization study of triglyceride lowering therapies for aortic stenosis
Ciofani Jonathan, Han Daniel, Gill Dipender, Rao Karan, Allahwala Usaid, Bhindi Ravinay
Marine N-3 Fatty Acids Improve Carotid Atherosclerosis in Diabetic PatientsJiao Jingjing, Zhang Yu, Zhuang Pan, Liu Xiaohui, Wan Xuzhi