Final ID: 32
Sleep Characteristics and Plasma Biomarkers of Alzheimer’s Disease Pathology, Neurodegeneration, and Neuroinflammation: The Atherosclerosis Risk in Communities Neurocognitive Study (ARIC-NCS)
Abstract Body: Introduction: Abnormal sleep has been linked to increased dementia risk, but the pathophysiological processes driving this connection are unclear. To provide insight into the biological pathways underlying the relationship between sleep and brain health, we tested the hypothesis that increased obstructive sleep apnea (OSA) severity and shorter habitual sleep duration are associated with a higher burden of Alzheimer’s disease (AD) pathology, neurodegeneration, and neuroinflammation measured through plasma biomarkers.
Methods: ARIC participants who took part in the Sleep Heart Health Study at Visit 4 (1996-98) with stored plasma samples at Visit 3 (1993-95) and Visit 5 (2011-13) were examined (n=261; mean age 61.3 years; 43.3% male). OSA severity, categorized based on the number of apneas and hypopneas per hour of sleep (<5 events/hour [Normal], 5 to <15 events/hour [Mild OSA], or ≥15 events/hour [Moderate/Severe OSA]) was assessed via in-home polysomnography, and average habitual sleep duration (<7 hours, 7 to <8 hours, or ≥8 hours) was self-reported. Plasma biomarkers of amyloid beta (Aβ) 42 and 40, phosphorylated Tau 181 (p-Tau181), neurofilament light chain (NfL), and glial fibrillary acidic protein (GFAP) were measured using Quanterix Simoa immunoassays. Covariate-adjusted linear regression models estimated associations of sleep indices in 1996-98 with standardized plasma biomarker measurements in 1993-95 (3 years earlier) and in 2011-13 (15 years later). Covariate-adjusted linear mixed effects models quantified associations of sleep measures with the 5-year rates of change in standardized biomarker levels (1993-2013).
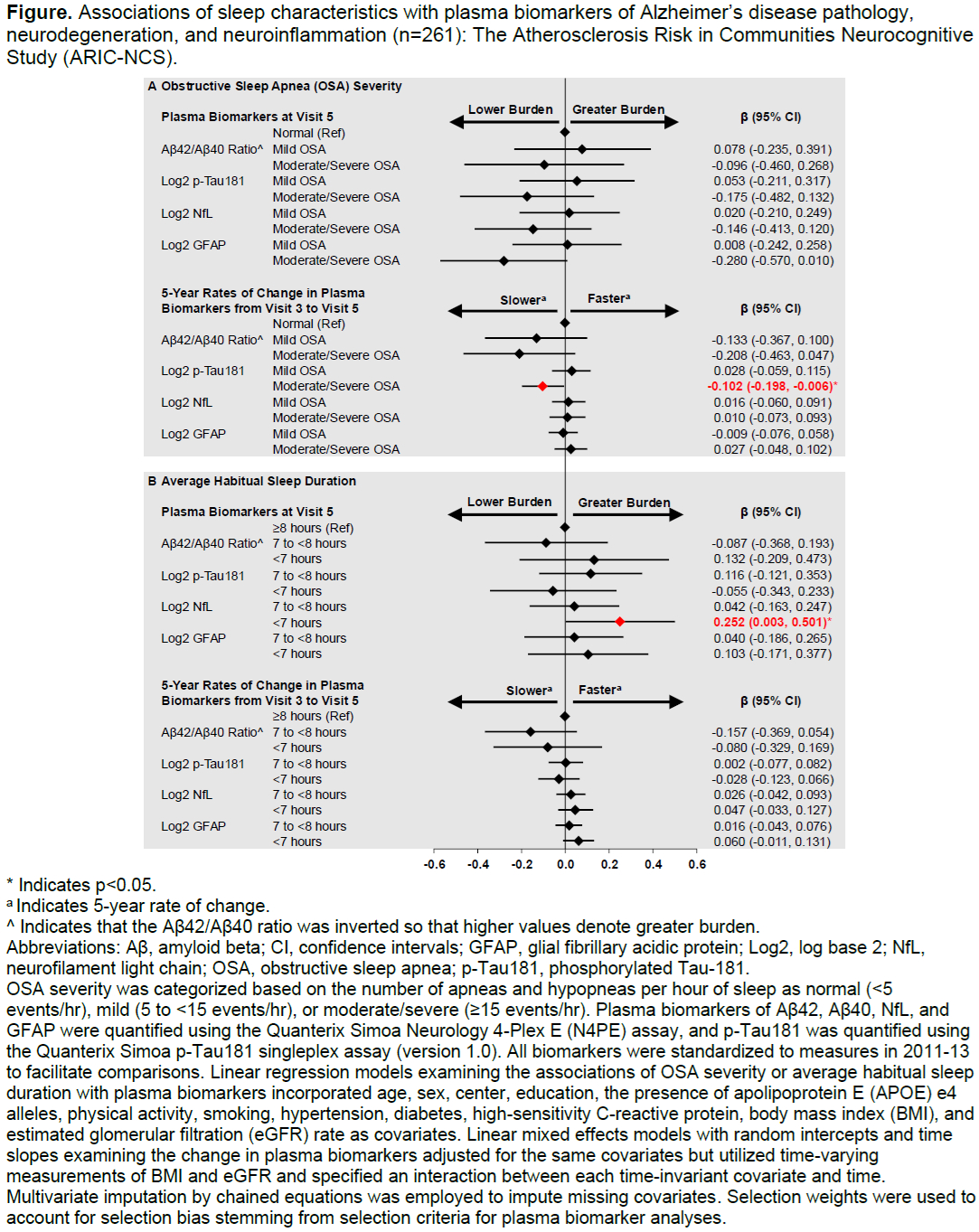
Results: Compared to a habitual sleep duration of 8 hours or more, sleeping less than 7 hours per night was associated with higher NfL, a biomarker of neurodegeneration, 15 years later (β = 0.252; 95% confidence interval [CI]: 0.003, 0.501). Sleep indices were not associated with biomarker levels 3 years earlier. Counter to our hypothesis, Moderate/Severe OSA was associated with slower increases in p-Tau181 (β = -0.102; 95% CI: -0.198, -0.006), a biomarker of AD pathology, over a median of 17.9 years.
Conclusions: Short habitual sleep duration may impact dementia outcomes through neurodegenerative and other processes rather than through pathways specific to AD pathology or neuroinflammation. Longitudinal studies with sleep measurements in larger, more diverse samples are needed to further distinguish the pathways linking sleep to dementia.
Methods: ARIC participants who took part in the Sleep Heart Health Study at Visit 4 (1996-98) with stored plasma samples at Visit 3 (1993-95) and Visit 5 (2011-13) were examined (n=261; mean age 61.3 years; 43.3% male). OSA severity, categorized based on the number of apneas and hypopneas per hour of sleep (<5 events/hour [Normal], 5 to <15 events/hour [Mild OSA], or ≥15 events/hour [Moderate/Severe OSA]) was assessed via in-home polysomnography, and average habitual sleep duration (<7 hours, 7 to <8 hours, or ≥8 hours) was self-reported. Plasma biomarkers of amyloid beta (Aβ) 42 and 40, phosphorylated Tau 181 (p-Tau181), neurofilament light chain (NfL), and glial fibrillary acidic protein (GFAP) were measured using Quanterix Simoa immunoassays. Covariate-adjusted linear regression models estimated associations of sleep indices in 1996-98 with standardized plasma biomarker measurements in 1993-95 (3 years earlier) and in 2011-13 (15 years later). Covariate-adjusted linear mixed effects models quantified associations of sleep measures with the 5-year rates of change in standardized biomarker levels (1993-2013).
Results: Compared to a habitual sleep duration of 8 hours or more, sleeping less than 7 hours per night was associated with higher NfL, a biomarker of neurodegeneration, 15 years later (β = 0.252; 95% confidence interval [CI]: 0.003, 0.501). Sleep indices were not associated with biomarker levels 3 years earlier. Counter to our hypothesis, Moderate/Severe OSA was associated with slower increases in p-Tau181 (β = -0.102; 95% CI: -0.198, -0.006), a biomarker of AD pathology, over a median of 17.9 years.
Conclusions: Short habitual sleep duration may impact dementia outcomes through neurodegenerative and other processes rather than through pathways specific to AD pathology or neuroinflammation. Longitudinal studies with sleep measurements in larger, more diverse samples are needed to further distinguish the pathways linking sleep to dementia.
More abstracts on this topic:
Geographic and Demographic Disparities and Trends in Hypertension and Sleep Disorder Related Mortality in United States Adults Aged 25 Years and Older From 1999 to 2020
Humayun Zainab, Majeed Mir Wajid, Imran Nur, Asif Talal
Accumulation of Skeletal Muscle Adiposity over 18-years is Associated with Lower Cognitive Functioning: The Tobago Health StudyGrant Alex, Roe Lauren, Cvejkus Ryan, Snitz Beth, Zmuda Joseph, Wheeler Victor, Gordon Christopher, Rosano Caterina, Miljkovic Iva