Final ID: 37
Associations of Prenatal Per- and Polyfluoroalkyl Substances (PFAS) Exposures and Childhood Blood Pressure in the Environmental influences on Child Health Outcomes (ECHO) Cohort
Hypothesis: We hypothesized that prenatal PFAS exposure is associated with higher childhood BP.
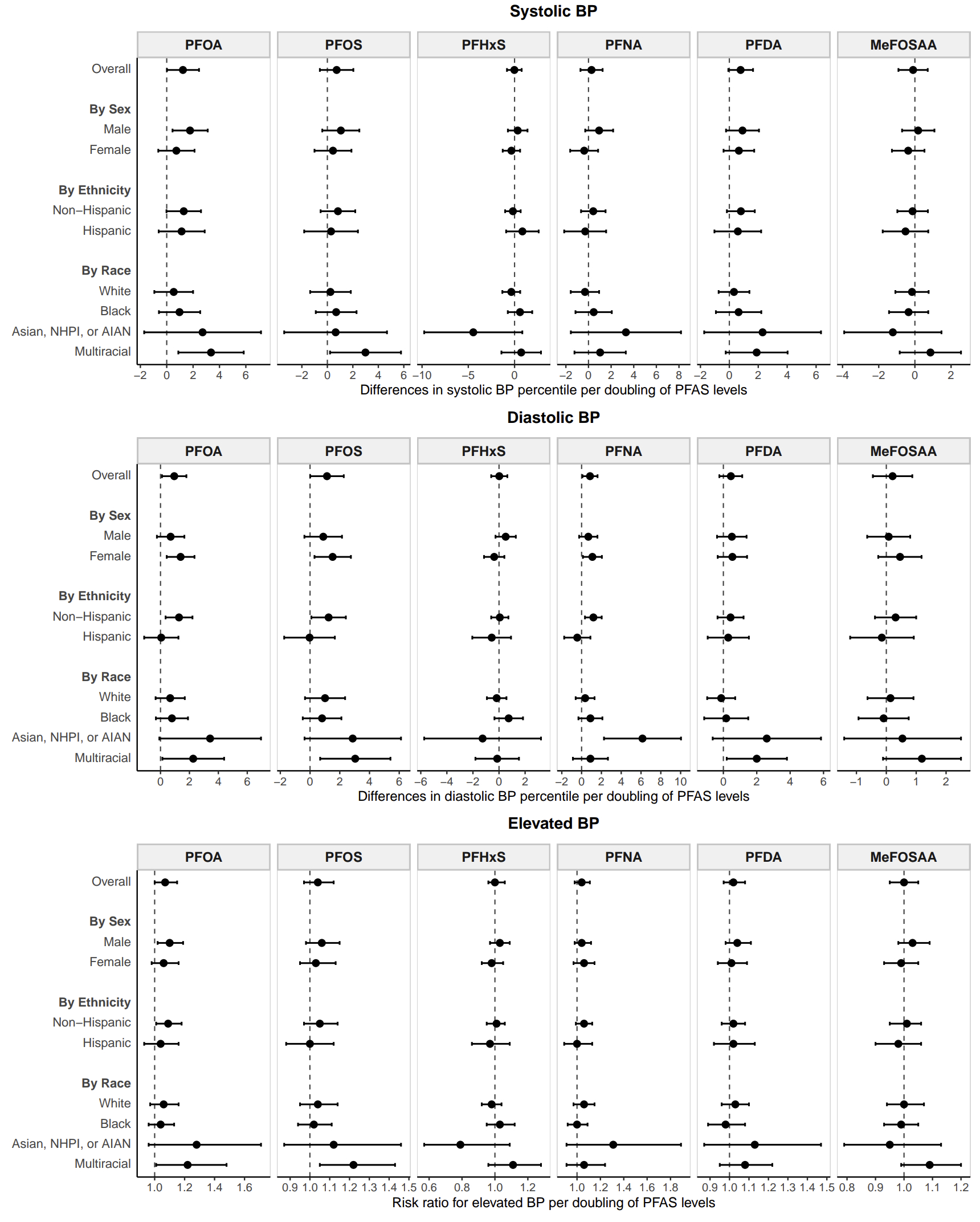
Methods: We included children aged 3-13 years in the U.S. ECHO Cohort with data on gestational plasma or serum concentrations of PFOA, PFOS, PFHxS, PFNA, PFDA, and MeFOSAA. Children’s BP was obtained from study visits or medical records. We derived age-, sex-, and height-specific BP percentiles according to the 2017 American Academy of Pediatrics Guidelines and defined elevated BP as systolic BP (SBP) or diastolic BP (DBP) ≥90th percentile. We used multivariable linear and modified Poisson models with generalized estimating equations and repeated BP measures clustered by participant (adjustment variables shown in Figure 1 footnotes) and addressed missing data using multiple imputation by chained equations. We conducted subgroup analyses by child sex, ethnicity, and race, and we examined trimester-specific associations.
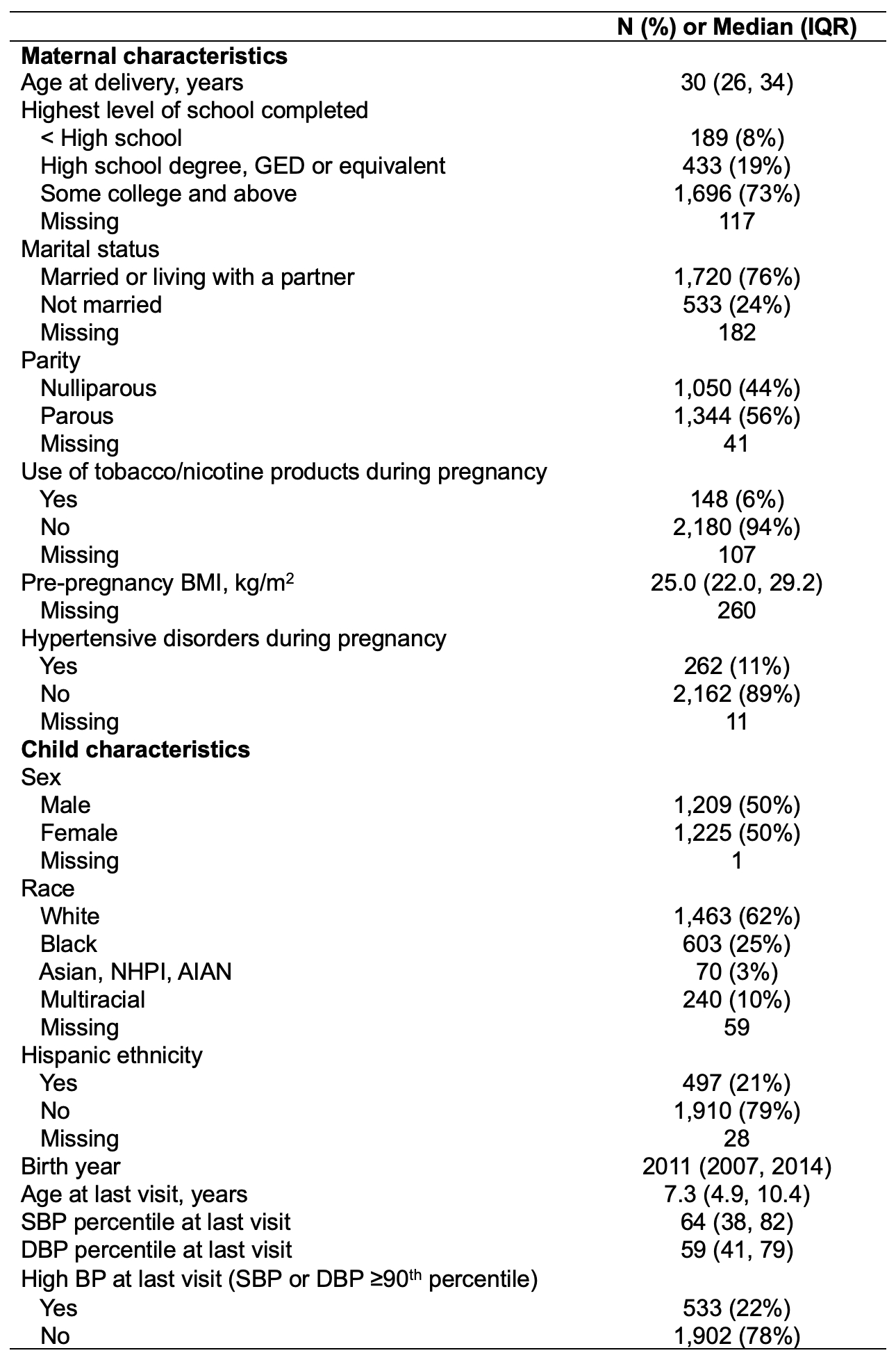
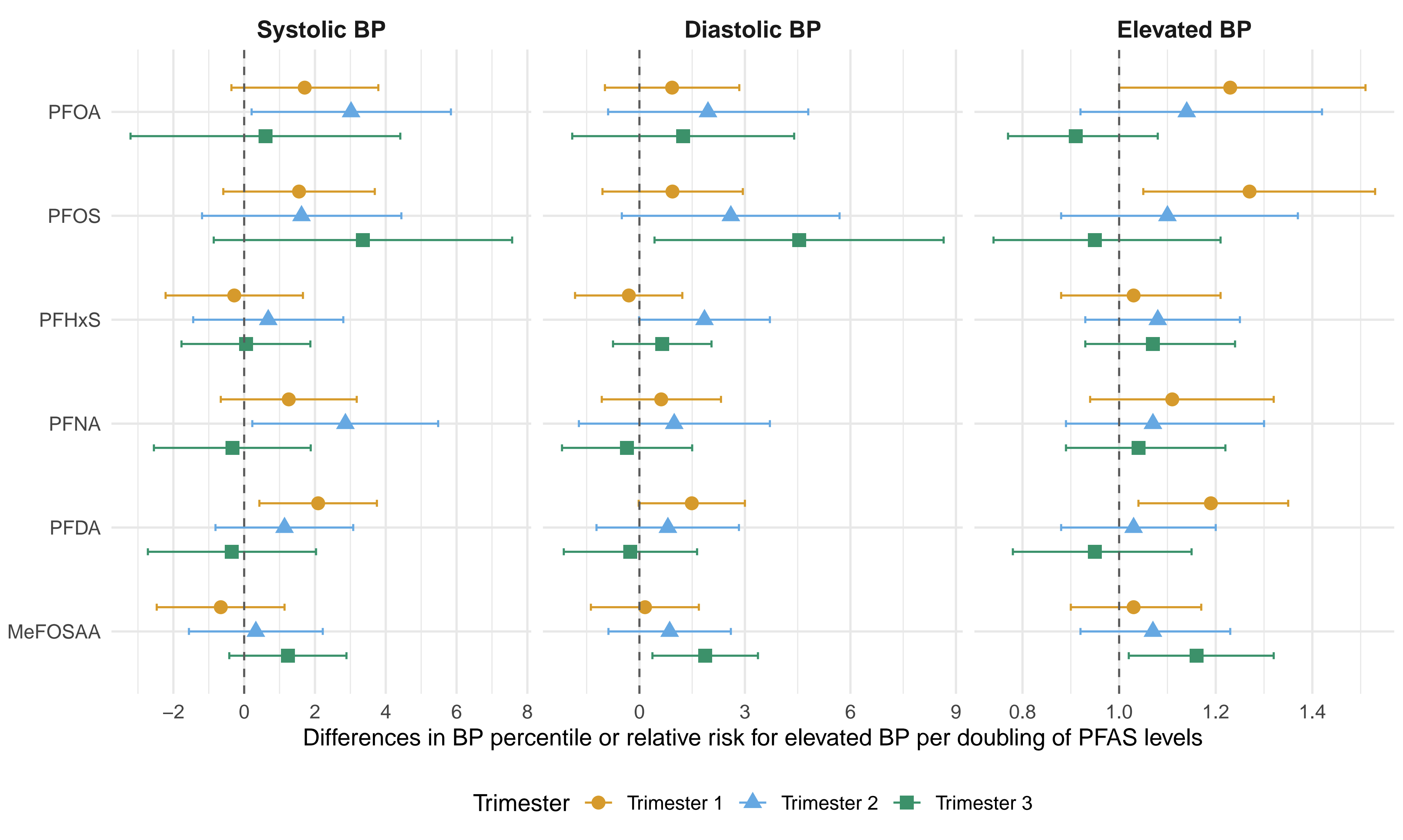
Results: Among 2,435 children (50% female, 21% Hispanic, 25% Black), 22% had elevated BP at their last visit at a median age of 7.3 years (Table 1). In adjusted analyses (Figure 1), each doubling of PFOA was associated with a 1.23 (95% CI: 0.02, 2.45) higher SBP percentile, a 0.95 (0.10, 1.79) higher DBP percentile, and 1.07 (1.00, 1.15) times the risk of elevated BP. Each doubling of PFOS and PFNA was associated with a 1.14 (0.01, 2.27) and 0.85 (0.09, 1.61) higher DBP percentile, respectively. The PFOA-SBP association was stronger in males, and associations of PFOA, PFOS, and PFNA with DBP were stronger in females and non-Hispanic children. In trimester-specific analyses (Figure 2), first-trimester PFOA, PFOS, and PFDA were associated with elevated BP; second-trimester PFOA and PFNA were associated with higher SBP percentiles; and third-trimester PFOS and MeFOSAA were associated with higher DBP percentiles.
Conclusions: Prenatal exposure to PFOA, PFOS, and PFNA was associated with higher childhood BP. The trimester-specific associations should be interpreted with caution as they may also reflect cohort differences in PFAS profiles. PFAS may contribute to early-life programming of elevated lifelong cardiovascular risk, reinforcing the importance of population-level prevention.
- Wang, Frances ( Beth Israel Deaconess Med Center , Boston , Massachusetts , United States )
- Lin, Pi-i ( Harvard Medical School and Harvard Pilgrim Health Care Institute , Boston , Massachusetts , United States )
- Aris, Izzuddin ( Harvard Medical School and Harvard Pilgrim Health Care Institute , Boston , Massachusetts , United States )
- Bastain, Theresa ( University of Southern California , Los Angeles , California , United States )
- Carignan, Courtney ( Michigan State University , East Lansing , Michigan , United States )
- Cassidy-bushrow, Andrea ( Henry Ford Health , Detroit , Michigan , United States )
- Cowell, Whitney ( NYU Grossman School of Medicine , New York , New York , United States )
- Croen, Lisa ( Kaiser Permanente Northern California , Pleasanton , California , United States )
- Dabelea, Dana ( University of Colorado Anschutz , Denver , Colorado , United States )
- Dunlop, Anne ( Emory University , Atlanta , Georgia , United States )
- Ferrara, Assiamira ( Kaiser Permanente Northern California , Pleasanton , California , United States )
- Farzan, Shohreh ( University of Southern California , Los Angeles , California , United States )
- Geiger, Sarah ( University of Illinois , Urbana , Illinois , United States )
- Kelly, Rachel ( Brigham and Women’s Hospital and Harvard Medical School , Boston , Massachusetts , United States )
- Karagas, Margaret ( Dartmouth College , Lebanon , New Hampshire , United States )
- Levine, Michele ( University Of Pittsburgh , Pittsburgh , Pennsylvania , United States )
- Li, Zeyu ( Johns Hopkins Bloomberg School of Public Health , Baltimore , Maryland , United States )
- Liang, Donghai ( Emory University , Atlanta , Georgia , United States )
- Niu, Zhongzheng ( University at Buffalo , Buffalo , New York , United States )
- Oconnor, Thomas ( University of Rochester Medical Center , Rochester , New York , United States )
- Oh, Jiwon ( University of California Davis School of Medicine , Davis , California , United States )
- Peterson, Alicia ( Kaiser Permanente Northern California , Pleasanton , California , United States )
- Porucznik, Christina ( University of Utah , Salt Lake City , Utah , United States )
- Romano, Megan ( Dartmouth College , Lebanon , New Hampshire , United States )
- Starling, Anne ( University of North Carolina at Chapel Hill , Chapel Hill , North Carolina , United States )
- Varshavsky, Julia ( Northeastern University , Boston , Massachusetts , United States )
- Zhao, Qi ( UNIVERSITY of TENNESSEE , Memphis , Tennessee , United States )
- Hivert, Marie-france ( Harvard Medical School , Boston , Massachusetts , United States )
- Oken, Emily ( HPHC Institute , Boston , Massachusetts , United States )
- Zhang, Mingyu ( Harvard Medical School , Boston , Massachusetts , United States )
Meeting Info:
Session Info:
The Jeremiah and Rose Stamler Research Award Finalist Presentations
Thursday, 03/19/2026 , 01:30PM - 03:00PM
Oral Abstract Session
More abstracts on this topic:
Rajasekaran Snekha, Foksinska Aleksandra, Crowder Camerron, Might Matthew
Early Pregnancy Mood is Associated with Postpartum Weight Retention in a Cohort of Californian Pregnant Women with Overweight and ObesitySimmons Leigh Ann, Gilliland Paige, Phipps Jennifer, Castro-alvarez Sebastian, Smith Paige, Nicholas Phoebe, Patrikeyeva Alina, Overstreet Courtney, Keeton Victoria
More abstracts from these authors:
Grobman Benjamin, Zhang Mingyu, Rifas-shiman Sheryl L., Aris Izzuddin, Lin Pi-i, James-todd Tamarra, Fleisch Abby, Juraschek Stephen, Oken Emily, Hivert Marie-france
Associations of Diet during Pregnancy with Cardiovascular Health (Life’s Essential 8) among Women in MidlifeRifas-shiman Sheryl, Aris Izzuddin, Hivert Marie-france, Zhang Mingyu, Chavarro Jorge, Oken Emily