Final ID: TU108
Orthostatic Blood Pressure Phenotypes are Associated with Night-Time Blood Pressure Non-Dipping in Older Adults: The Atherosclerosis Risk in Communities (ARIC) Study
Abstract Body: Introduction: Nighttime blood pressure (BP) non-dipping (i.e., a blunted reduction in BP during sleep) is associated with higher risk of cardiovascular disease, stroke, cognitive decline and early death among older adults. Orthostatic hypotension (OH) may share a related physiological pattern, marked by higher supine and lower standing BP (resembling night- and daytime BP respectively). Whether measured or symptomatic OH or orthostatic symptoms could identify people with nighttime non-dipping is unknown.
Hypothesis: Very old adults with OH would be more likely to have nighttime non-dipping.
Methods: Participants in the ARIC study (2021-23) underwent in-office OH assessments (3 supine followed by 6 standing BP measurements, 1 minute apart) and ABPM monitoring (≥20 daytime and ≥7 nighttime BP measurements over 24 hours). Non-dipping was defined as night/day BP ratio >0.9 (reduction in BP of <10%). OH was defined as a drop in average systolic BP (SBP) of ≥20 mm Hg or diastolic BP (DBP) of ≥10 mm Hg from supine to standing, at 1, 3, or 6 minutes after standing (SBP or DBP OH were examined with corresponding non-dipping). Orthostatic symptoms included lightheadedness, dizziness, imbalance, or fainting during the standing maneuver or while in the standing position. We used logistic regression to examine associations of OH and orthostatic symptoms with non-dipping, adjusting for age, sex, race-study center, and antihypertensive medication use.
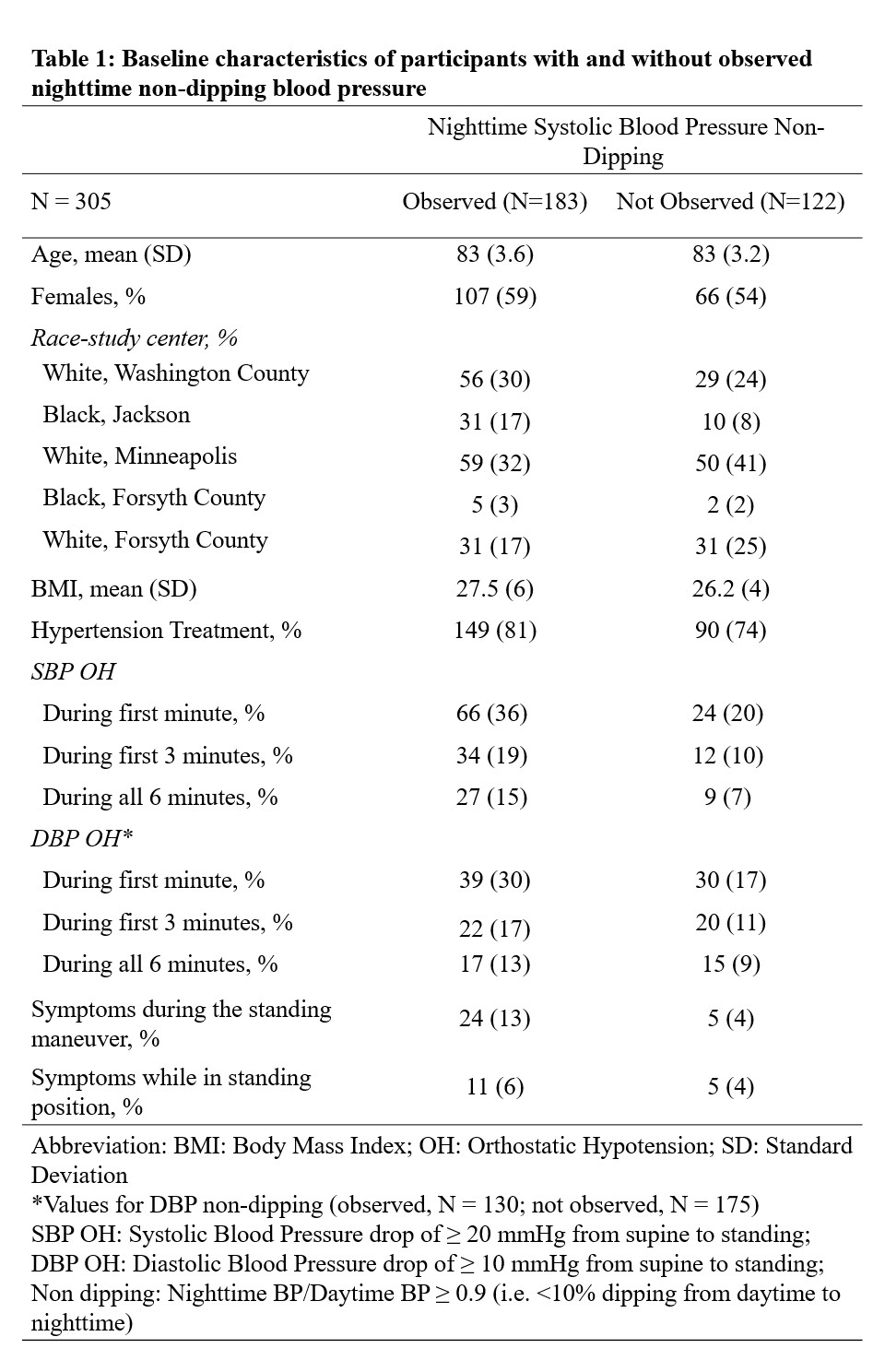
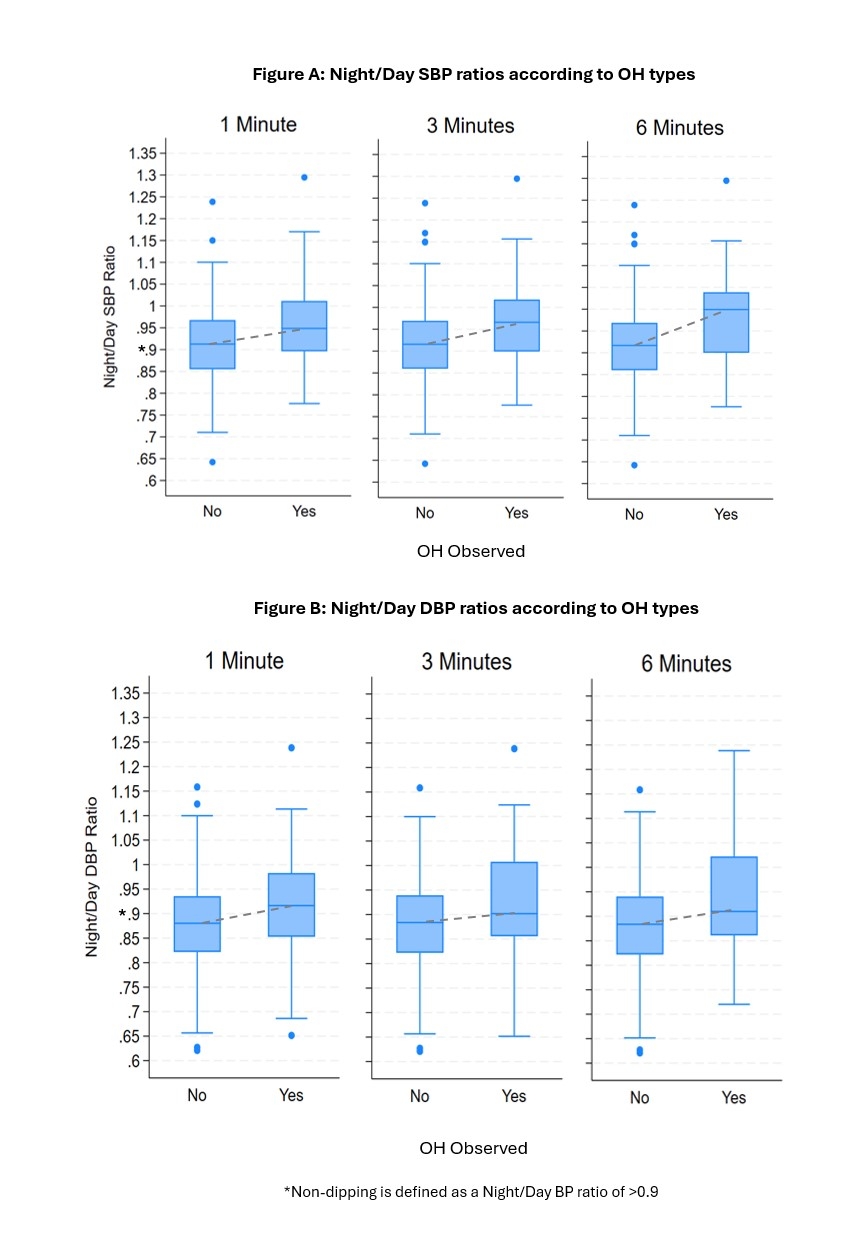
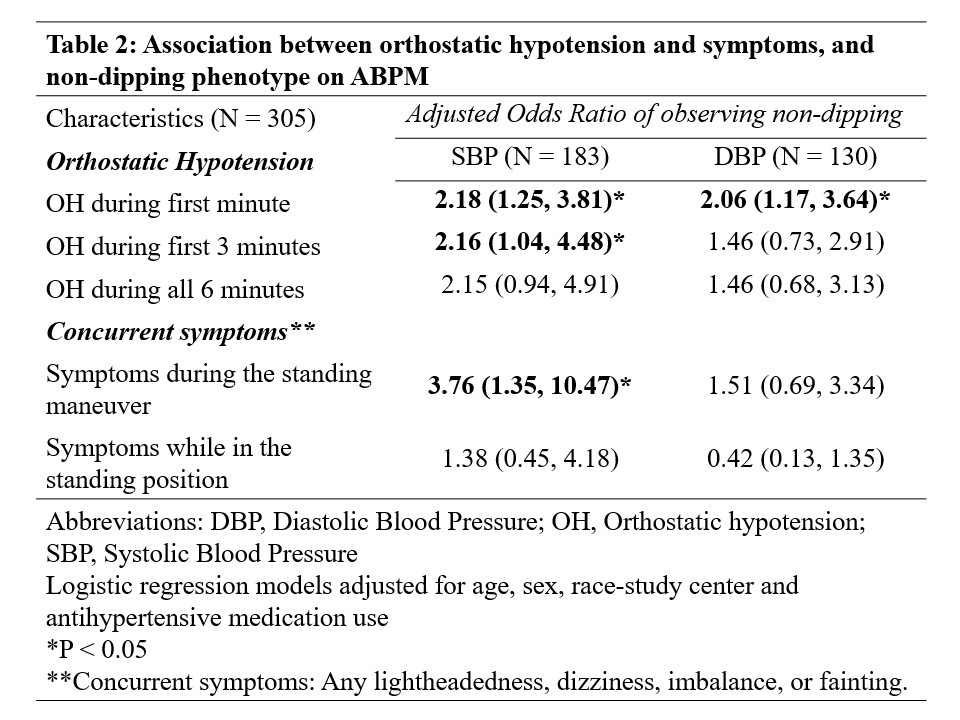
Results: Of the 305 study participants (57% female, mean age 83.3 [SD: 3.5] years), 60% had non-dipping based on SBP and 43% had non-dipping based on DBP. Mean ABPM daytime SBP was 129.7 (SD: 13.3) mm Hg and nighttime SBP was 119.5 (SD: 15.5) mm Hg; 78% used antihypertensive medications (Table 1). People with OH had higher mean night/day BP ratio compared to people without OH for SBP (0.96 vs 0.91) and DBP (0.92 vs 0.88) (Figure). OH during the first minute was associated with non-dipping for both SBP (OR: 2.18 [CI: 1.25, 3.81]) and DBP (2.06 [1.17, 3.64]), whereas OH during the first 3 minutes was associated with SBP non-dipping (2.16 [1.04, 4.48]). Symptoms during the standing maneuver were associated with SBP non-dipping (3.76 [1.35, 10.47]) (Table 2).
Conclusion: In this population of very old, community-dwelling adults, OH soon after standing up (both measured and symptomatic) was associated with nighttime non-dipping on ABPM. Performing ABPM could be valuable in patients with early OH to identify nighttime non-dipping.
Hypothesis: Very old adults with OH would be more likely to have nighttime non-dipping.
Methods: Participants in the ARIC study (2021-23) underwent in-office OH assessments (3 supine followed by 6 standing BP measurements, 1 minute apart) and ABPM monitoring (≥20 daytime and ≥7 nighttime BP measurements over 24 hours). Non-dipping was defined as night/day BP ratio >0.9 (reduction in BP of <10%). OH was defined as a drop in average systolic BP (SBP) of ≥20 mm Hg or diastolic BP (DBP) of ≥10 mm Hg from supine to standing, at 1, 3, or 6 minutes after standing (SBP or DBP OH were examined with corresponding non-dipping). Orthostatic symptoms included lightheadedness, dizziness, imbalance, or fainting during the standing maneuver or while in the standing position. We used logistic regression to examine associations of OH and orthostatic symptoms with non-dipping, adjusting for age, sex, race-study center, and antihypertensive medication use.
Results: Of the 305 study participants (57% female, mean age 83.3 [SD: 3.5] years), 60% had non-dipping based on SBP and 43% had non-dipping based on DBP. Mean ABPM daytime SBP was 129.7 (SD: 13.3) mm Hg and nighttime SBP was 119.5 (SD: 15.5) mm Hg; 78% used antihypertensive medications (Table 1). People with OH had higher mean night/day BP ratio compared to people without OH for SBP (0.96 vs 0.91) and DBP (0.92 vs 0.88) (Figure). OH during the first minute was associated with non-dipping for both SBP (OR: 2.18 [CI: 1.25, 3.81]) and DBP (2.06 [1.17, 3.64]), whereas OH during the first 3 minutes was associated with SBP non-dipping (2.16 [1.04, 4.48]). Symptoms during the standing maneuver were associated with SBP non-dipping (3.76 [1.35, 10.47]) (Table 2).
Conclusion: In this population of very old, community-dwelling adults, OH soon after standing up (both measured and symptomatic) was associated with nighttime non-dipping on ABPM. Performing ABPM could be valuable in patients with early OH to identify nighttime non-dipping.
More abstracts on this topic:
Characterization of Cardiac, Autonomic, and Exercise Physiology in Patients with Long COVID
Suckow Emmett, Mcdonnell Barry, Stöhr Eric, Cornwell William, Pierce Kate, Wulff Kyla, Arent Chelsea, Kreye Shelanna, Rosenberg Michael, Sabin Katie, Parker Hugh, Forbes Lindsay
Cardiorenal Dysfunction Caused by High Fat Diet and Sodium Oxalate Gavage in MiceSilva Amanda, Irigoyen Maria, Nascimento-carvalho Bruno, Jimenez Alessandra, Silva Maikon, De Oliveira Silva Tábatha, Lunardon Guilherme, Souza Felipe, Andrade Lucia, Diniz Gabriela