Final ID: 71
Replacing Sedentary Time by Moderate-to-Vigorous Physical Activity or Sleep on a 24h Period in Early Adolescence Is Associated with Lower Insulin Resistance Five Years Later: Prospective Analysis Within the Project Viva Cohort
Abstract Body: Introduction. Physical activity, sedentary time and sleep are determinants of adolescent cardiometabolic health. However, few studies have examined the interrelatedness of these behaviors in a 24h period, which is more applicable to the real world and could better inform public health policies.
Hypothesis. Reallocation of time from sedentary behaviors to physical activity over 24h in early adolescence is associated with the most cardiometabolic health benefits in late adolescence.
Methods. We used data from the ongoing Project Viva prebirth cohort (Eastern Massachusetts, USA, births 1999-2002). In early adolescence (median age 12.9 years), participants wore a wrist accelerometer for 7-10 consecutive days and completed sleep logs. We determined the average minutes spent in sleep, sedentary time, light physical activity (LPA), and moderate-to-vigorous physical activity (MVPA) using validated cut points. In late adolescence (median age 17.5 years), we collected fasting blood for adiponectin, glucose, and insulin and calculated HOMA-IR. We analyzed how proportion of time spent in each of the four activity categories in early adolescence was associated with glucose, insulin, and adiponectin in late adolescence using compositional data analysis, adjusting for participants’ age, sex, and season of actigraphy in early adolescence and maternal education and household income at enrollment.
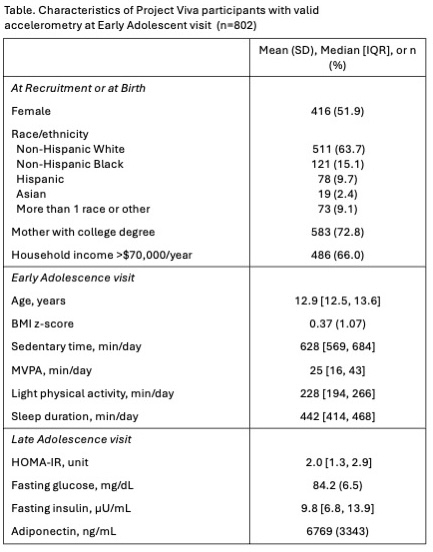
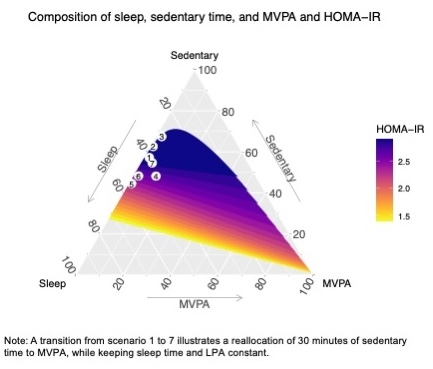
Results. A total of 802 adolescents (n=394 with outcome data) had valid accelerometer data, with 51.9% female and 63.7% non-Hispanic white (Table). The sample average 24h time composition was 33% for sleep, 48% for sedentary activities, 17% for LPA and 2% for MVPA. Allocating time towards sleep or MVPA at the expense of sedentary time in early adolescence was associated with lower HOMA-IR in late adolescence (Figure). More specifically, reallocating 30 minutes of sedentary time to MVPA or to sleep was associated with a 14.8% (95%CI: -23.3; -5.1) and 4.7% (95%CI: -7.8; -0.6) reduction in HOMA-IR, respectively, while reallocating to LPA would yield no significant change in HOMA-IR (2.9%, 95%CI: -0.9; 7.4). Our results did not support associations of activity 24h composition with adiponectin or fasting glucose.
Conclusions. Allocating more time in MVPA and sleep on a 24h period in early adolescence is associated with lower insulin resistance in late adolescence. Public health strategies should focus on promoting MVPA and sleep to preserve optimal cardiometabolic health in adolescents.
Hypothesis. Reallocation of time from sedentary behaviors to physical activity over 24h in early adolescence is associated with the most cardiometabolic health benefits in late adolescence.
Methods. We used data from the ongoing Project Viva prebirth cohort (Eastern Massachusetts, USA, births 1999-2002). In early adolescence (median age 12.9 years), participants wore a wrist accelerometer for 7-10 consecutive days and completed sleep logs. We determined the average minutes spent in sleep, sedentary time, light physical activity (LPA), and moderate-to-vigorous physical activity (MVPA) using validated cut points. In late adolescence (median age 17.5 years), we collected fasting blood for adiponectin, glucose, and insulin and calculated HOMA-IR. We analyzed how proportion of time spent in each of the four activity categories in early adolescence was associated with glucose, insulin, and adiponectin in late adolescence using compositional data analysis, adjusting for participants’ age, sex, and season of actigraphy in early adolescence and maternal education and household income at enrollment.
Results. A total of 802 adolescents (n=394 with outcome data) had valid accelerometer data, with 51.9% female and 63.7% non-Hispanic white (Table). The sample average 24h time composition was 33% for sleep, 48% for sedentary activities, 17% for LPA and 2% for MVPA. Allocating time towards sleep or MVPA at the expense of sedentary time in early adolescence was associated with lower HOMA-IR in late adolescence (Figure). More specifically, reallocating 30 minutes of sedentary time to MVPA or to sleep was associated with a 14.8% (95%CI: -23.3; -5.1) and 4.7% (95%CI: -7.8; -0.6) reduction in HOMA-IR, respectively, while reallocating to LPA would yield no significant change in HOMA-IR (2.9%, 95%CI: -0.9; 7.4). Our results did not support associations of activity 24h composition with adiponectin or fasting glucose.
Conclusions. Allocating more time in MVPA and sleep on a 24h period in early adolescence is associated with lower insulin resistance in late adolescence. Public health strategies should focus on promoting MVPA and sleep to preserve optimal cardiometabolic health in adolescents.
More abstracts on this topic:
Associations of joint pain and intermittent claudication with objectively measured physical activity: the Hispanic Community Health Study/Study of Latinos (HCHS/SOL)
Mok Yejin, Gallo Linda, Matsushita Kunihiro, Sotres-alvarez Daniela, Kaplan Robert, Allison Matthew, Martinez-amezcua Pablo, Schrack Jennifer, Liu Hairong, Garcia-bedoya Olga, Cordero Christina
Androgenic Profile and Cardiometabolic Health among Post-Menopausal Women: the Buffalo OsteoPerio StudyNiu Zhongzheng, Wactawski-wende Jean, Millen Amy, Lamonte Michael