Final ID: TU273
Early Life Exposures and Age at Menopause in the REasons for Geographic and Racial Differences in Stroke (REGARDS) Study
Abstract Body: Background: Younger age at menopause (premature and early menopause) occurs more often in Black women than in White women and is associated with an increased cardiovascular disease risk. Traditional risk factors for early onset are well studied, but the role of adverse childhood experiences (ACEs) is unclear. This study examined the association between ACEs and age at menopause. We hypothesized that women reporting ACEs are more likely to experience menopause at younger ages compared to those reporting no ACEs.
Methods: A cross-sectional analysis was conducted in 4,491 Black and White women aged 45 years from the REasons for Geographic and Racial Differences in Stroke Study. ACEs were assessed in the Childhood and Family Life Factors ancillary study using the Childhood SES Factors questionnaire and categorized into groups (0, 1, 2-3, and 4+ ACEs) for analyses. Age at menopause was measured as the self-reported age at last menstrual period, and categorized as premature (<40), early (40- 45), normal (45- 55), and late menopause (>55). Multinomial logistic regression was used to estimate separate odds ratios (OR) and 95% confidence intervals (CI) for early, premature, and late versus normal menopause. A crude (model 1) and four sequentially adjusted models, for demographic (model 2), socioeconomic (model 3), behavioral (model 4), and reproductive (model 5) covariates, were fit.
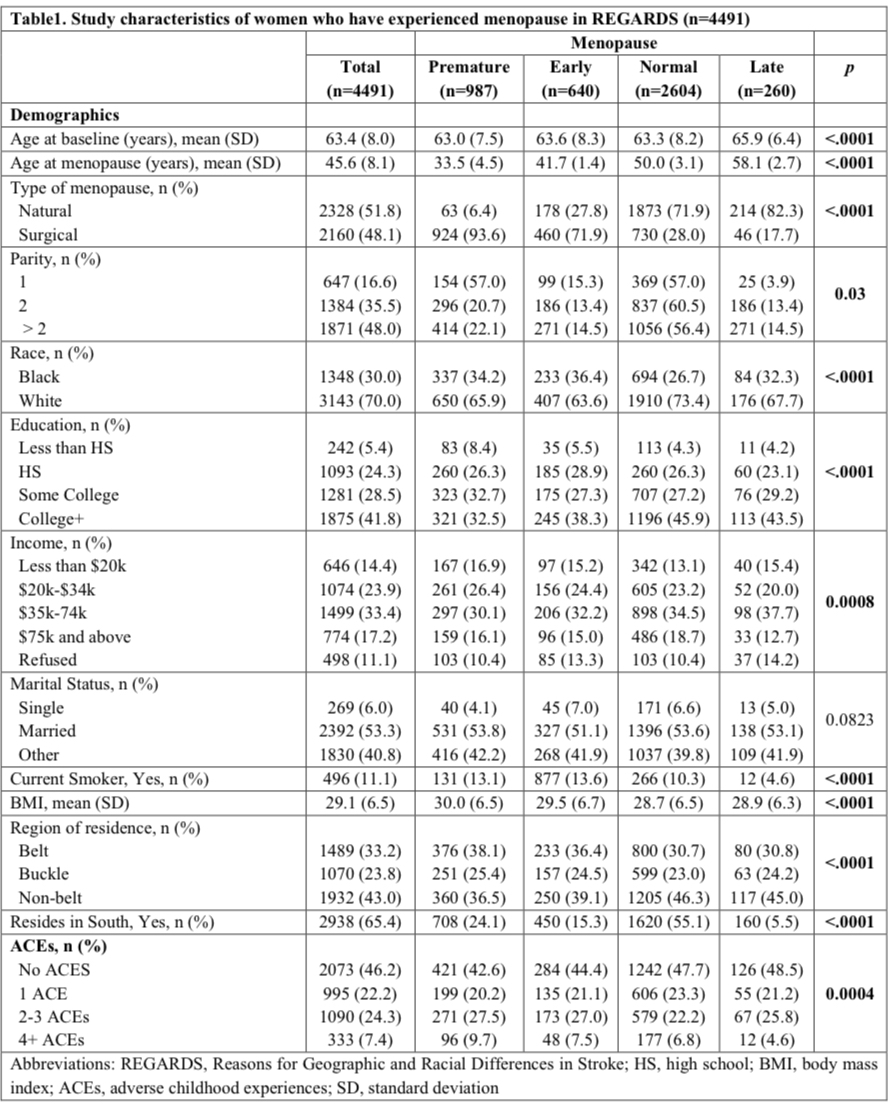
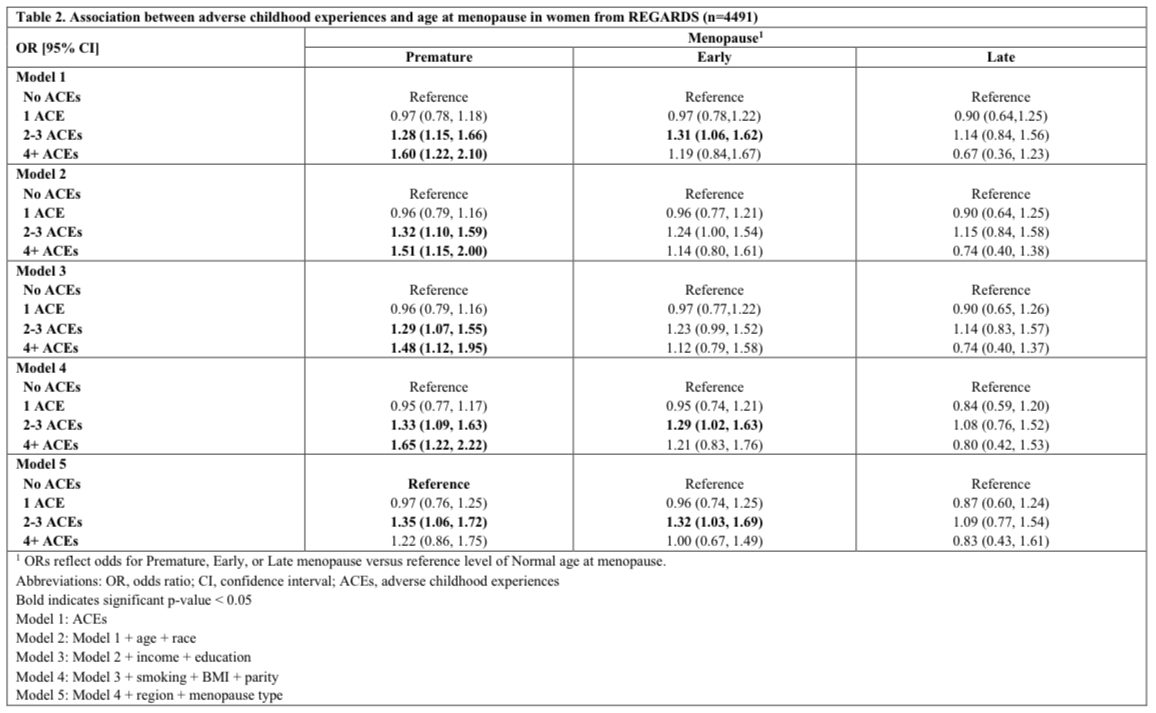
Results: Women were primarily White (70%), with a mean age at menopause of 45.6 years (± 8.1). Most women (58%) experienced a normal age at menopause, whereas 22% experienced premature, 14% experienced early, and 6% experienced late menopause. Approximately 22% reported 1 ACE, 24% reported 2-3 ACEs, and 7% reported 4+ ACEs. Reporting 2–3 ACEs (versus no ACEs) was associated with higher odds of premature menopause (fully adjusted OR [95% CI] = 1.33 [1.09–1.63]) and early menopause (fully adjusted OR [95% CI] = 1.32 [1.03–1.69]). Reporting ≥4 ACEs (versus no ACEs) was associated with higher odds of premature menopause in models 1-4 (model 4 OR [95% CI] = 1.65 [1.22–2.22], but this effect was attenuated in the fully adjusted model. No associations were observed for late menopause.
Conclusion: Women with 2–3 ACEs were more likely to experience premature and early menopause, while associations for ≥4 ACEs with premature were inconsistent. Further research is needed to understand how ACEs contribute to differences in reproductive aging and menopause timing.
Methods: A cross-sectional analysis was conducted in 4,491 Black and White women aged 45 years from the REasons for Geographic and Racial Differences in Stroke Study. ACEs were assessed in the Childhood and Family Life Factors ancillary study using the Childhood SES Factors questionnaire and categorized into groups (0, 1, 2-3, and 4+ ACEs) for analyses. Age at menopause was measured as the self-reported age at last menstrual period, and categorized as premature (<40), early (40- 45), normal (45- 55), and late menopause (>55). Multinomial logistic regression was used to estimate separate odds ratios (OR) and 95% confidence intervals (CI) for early, premature, and late versus normal menopause. A crude (model 1) and four sequentially adjusted models, for demographic (model 2), socioeconomic (model 3), behavioral (model 4), and reproductive (model 5) covariates, were fit.
Results: Women were primarily White (70%), with a mean age at menopause of 45.6 years (± 8.1). Most women (58%) experienced a normal age at menopause, whereas 22% experienced premature, 14% experienced early, and 6% experienced late menopause. Approximately 22% reported 1 ACE, 24% reported 2-3 ACEs, and 7% reported 4+ ACEs. Reporting 2–3 ACEs (versus no ACEs) was associated with higher odds of premature menopause (fully adjusted OR [95% CI] = 1.33 [1.09–1.63]) and early menopause (fully adjusted OR [95% CI] = 1.32 [1.03–1.69]). Reporting ≥4 ACEs (versus no ACEs) was associated with higher odds of premature menopause in models 1-4 (model 4 OR [95% CI] = 1.65 [1.22–2.22], but this effect was attenuated in the fully adjusted model. No associations were observed for late menopause.
Conclusion: Women with 2–3 ACEs were more likely to experience premature and early menopause, while associations for ≥4 ACEs with premature were inconsistent. Further research is needed to understand how ACEs contribute to differences in reproductive aging and menopause timing.
More abstracts on this topic:
Adherence to the Mediterranean diet and some related serum metabolites are strongly associated with epigenetic biomarkers of aging in Mediterranean subjects
Corella Dolores, Sorli Jose, Fernandez Carrion Rebeca, Coltell Oscar, Portoles Olga, Barragan Rocio, Asensio Eva Maria
Advanced Age Increases Susceptibility to Ischemic Myopathy after Murine Hindlimb IschemiaKulkarni Deepali, Massie Pierce, Justus Matthew, Mazloumibakhshayesh Milad, Coffman Brittany, Pace Carolyn, Clark Ross