Final ID: 16
Cardiorespiratory Fitness, Coronary Artery Calcium, and Later-Life Dementia: The Cooper Center Longitudinal Study
Abstract Body: Introduction: Cardiorespiratory fitness (CRF) and coronary artery calcium (CAC) score, both established cardiovascular risk markers, may be interrelated; however, their individual and joint associations with dementia risk remain unclear. We examined midlife CRF and CAC in relation to later-life dementia in a large prospective cohort.
Methods: Individual participant data from the Cooper Center Longitudinal Study (CCLS; 1998–2018) were linked to Medicare claims records (1999–2019). CAC was measured by cardiac computed tomography and dichotomized as <100 or ≥100 Agatston units (AU). CRF was estimated using a maximal treadmill exercise test following a modified Balke protocol. Participants were categorized into low, moderate, or high CRF based on age- and sex-specific cutoffs. Incident all-cause dementia was identified via Medicare surveillance using the Chronic Condition Warehouse. Pertinent participant characteristics were assessed at the baseline clinic visit, and stroke or transient ischemic attack (TIA) during follow-up was recorded as an interim event. Illness-death models with semi-competing risks were used to estimate hazard ratios for dementia associated with CAC and CRF categories, adjusting for demographic and clinical covariates.
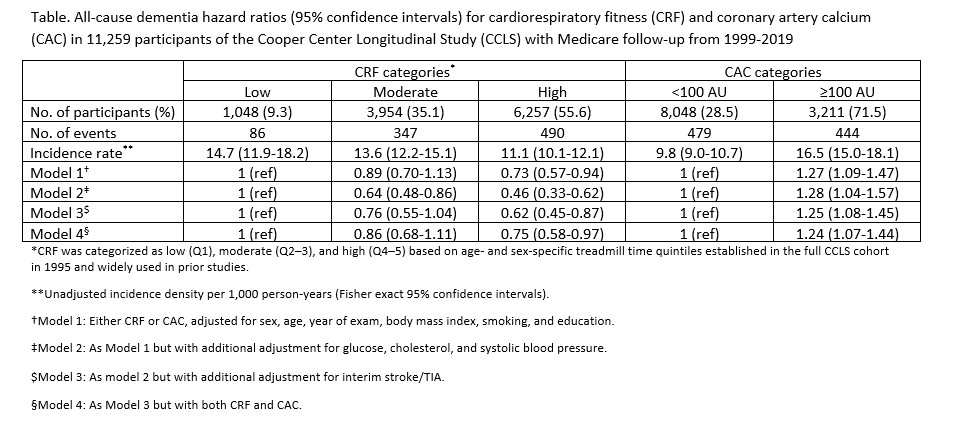
Results: Participants free of cardiovascular disease and dementia with complete exposure and outcome data were analyzed [n=11,259; mean (SD) baseline age, 56.8 (7.0) years; 3,400 (30.2%) women]. The prevalence of clinically-meaningful CAC (≥100 AU) decreased across CRF categories, from 34.4% in the low CRF group to 29.6% in the moderate group and 26.8% in the high CRF group. The mean (SD) time between the clinic visit and the start of Medicare surveillance was 8.6 (5.6) years. During a mean (SD) Medicare follow-up of 6.7 (5.0) years, 923 cases of dementia were identified. Higher CRF was associated with a lower risk of dementia, whereas higher CAC was associated with a higher risk. These associations persisted across models with hierarchical adjustment for demographics, cardiovascular risk factors, interim stroke/TIA, and the other primary exposure (CAC or CRF; see Table).
Conclusions: In this cohort of generally healthy adults, higher CRF and lower CAC in midlife were associated with a reduced risk of later-life dementia. These associations were independent of traditional cardiovascular risk factors and interim cerebrovascular events, highlighting the potential importance of fitness and vascular health in dementia prevention.
Methods: Individual participant data from the Cooper Center Longitudinal Study (CCLS; 1998–2018) were linked to Medicare claims records (1999–2019). CAC was measured by cardiac computed tomography and dichotomized as <100 or ≥100 Agatston units (AU). CRF was estimated using a maximal treadmill exercise test following a modified Balke protocol. Participants were categorized into low, moderate, or high CRF based on age- and sex-specific cutoffs. Incident all-cause dementia was identified via Medicare surveillance using the Chronic Condition Warehouse. Pertinent participant characteristics were assessed at the baseline clinic visit, and stroke or transient ischemic attack (TIA) during follow-up was recorded as an interim event. Illness-death models with semi-competing risks were used to estimate hazard ratios for dementia associated with CAC and CRF categories, adjusting for demographic and clinical covariates.
Results: Participants free of cardiovascular disease and dementia with complete exposure and outcome data were analyzed [n=11,259; mean (SD) baseline age, 56.8 (7.0) years; 3,400 (30.2%) women]. The prevalence of clinically-meaningful CAC (≥100 AU) decreased across CRF categories, from 34.4% in the low CRF group to 29.6% in the moderate group and 26.8% in the high CRF group. The mean (SD) time between the clinic visit and the start of Medicare surveillance was 8.6 (5.6) years. During a mean (SD) Medicare follow-up of 6.7 (5.0) years, 923 cases of dementia were identified. Higher CRF was associated with a lower risk of dementia, whereas higher CAC was associated with a higher risk. These associations persisted across models with hierarchical adjustment for demographics, cardiovascular risk factors, interim stroke/TIA, and the other primary exposure (CAC or CRF; see Table).
Conclusions: In this cohort of generally healthy adults, higher CRF and lower CAC in midlife were associated with a reduced risk of later-life dementia. These associations were independent of traditional cardiovascular risk factors and interim cerebrovascular events, highlighting the potential importance of fitness and vascular health in dementia prevention.
More abstracts on this topic:
4D Flow MRI Evaluation of Cardiovascular Risk-Related Alterations in Heart-Brain Hemodynamics in Cognitively Healthy Aging Adults
Najafi Anahita, Rogalski Emily, Jarvis Kelly, Richter Adam, Lytchakov Anna, Benson Theresa, Jin Ning, Davids Rachel, Schnell Susanne, Ragin Ann, Weintraub Sandra
Higher Allostatic Load Is Associated With Lower Cardiorespiratory Fitness Among U.S. Adults: NHANES 1999–2004Daneii Padideh, Sabina Michael, Khan Sana, Kadariya Dinesh