Final ID: MPTH73
Gut microbiome, blood metabolome and incident hypertension in Hispanic Community Health Study/Study of Latinos
Abstract Body: Background: While gut dysbiosis is linked to prevalent hypertension (HTN), microbial features associated with incident HTN and the mediating role of circulating metabolites remain poorly understood.
Methods: We conducted a prospective analysis of 1,265 HTN-free adults with concurrently profiling of gut metagenomics (440 core species with prevalance >10% and relative abundance >0.01%) and serum metabolomics (767 named metabolites) from HCHS/SOL (mean age 53 yrs; 65.8% female; 358 incident HTN over a median of 7 yrs of follow-up). Cox proportional hazard models were used to identify gut microbial species and metabolites associated with incident HTN. Mediation analysis was used to quantify the extent to which metabolites explain the microbiome-HTN relationship.
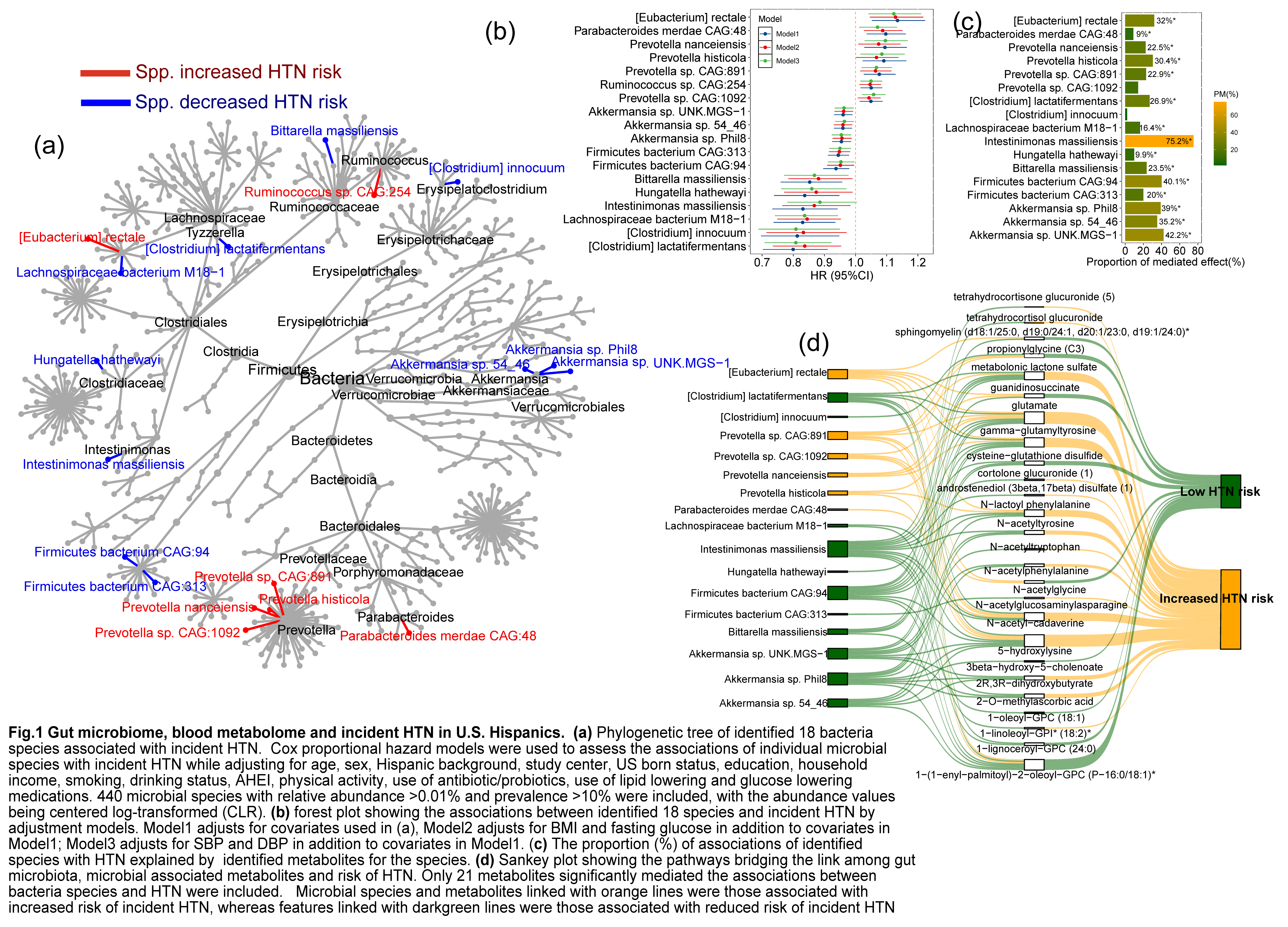
Results: We identified 18 bacterial species associated with incident HTN (FDR<0.25, Fig1.a), largely independent of baseline cardiometabolic traits (Fig1.b). Seven species, predominantly Prevotella spp. (e.g., P. nanceiensis and P. histicola), were associated with higher HTN risk, whereas the other 11 species showed inverse associations, including three Akkermansia spp., two Firmicutes spp., and multiple Clostridiales spp. (e.g., Intestinimonas massiliensis). We further identified 224 metabolites (FDR<0.05) that were associated with both at least one HTN-related species and incident HTN. These metabolites collectively mediated a substantial portion of the observed microbiota-HTN associations, with the proportion of mediated effect ranging from 9% for Parabacteroides merdae to 75.2% for Intestinimonas massiliensis (Fig.1c). Key metabolites with significant mediating effects, especially on the protective association between Intestinimonas massiliensis and incident HTN, included microbially influenced steroids (e.g., androstenediol disulfate, tetrahydrocortisol glucuronide), N-acetyl-amino acids (e.g., N-acetylphenylalanine, N-acetyltyrosine), and markers of endothelial dysfunction and vascular stiffness (e.g., cysteine-glutathione disulfide, 5-hydroxylysine) (Fig1.d). A combined panel of the identified gut microbiota and metabolites significantly improved HTN risk prediction beyond conventional risk factors (AUC improved from 0.77 to 0.84, p<0.001).
Conclusion: Our study characterizes multiple bacterial species associated with incident HTN, and the associations might be partly mediated by circulating metabolites. Inclusion of gut microbiome and associated metabolites facilitates the risk prediction of HTN.
Methods: We conducted a prospective analysis of 1,265 HTN-free adults with concurrently profiling of gut metagenomics (440 core species with prevalance >10% and relative abundance >0.01%) and serum metabolomics (767 named metabolites) from HCHS/SOL (mean age 53 yrs; 65.8% female; 358 incident HTN over a median of 7 yrs of follow-up). Cox proportional hazard models were used to identify gut microbial species and metabolites associated with incident HTN. Mediation analysis was used to quantify the extent to which metabolites explain the microbiome-HTN relationship.
Results: We identified 18 bacterial species associated with incident HTN (FDR<0.25, Fig1.a), largely independent of baseline cardiometabolic traits (Fig1.b). Seven species, predominantly Prevotella spp. (e.g., P. nanceiensis and P. histicola), were associated with higher HTN risk, whereas the other 11 species showed inverse associations, including three Akkermansia spp., two Firmicutes spp., and multiple Clostridiales spp. (e.g., Intestinimonas massiliensis). We further identified 224 metabolites (FDR<0.05) that were associated with both at least one HTN-related species and incident HTN. These metabolites collectively mediated a substantial portion of the observed microbiota-HTN associations, with the proportion of mediated effect ranging from 9% for Parabacteroides merdae to 75.2% for Intestinimonas massiliensis (Fig.1c). Key metabolites with significant mediating effects, especially on the protective association between Intestinimonas massiliensis and incident HTN, included microbially influenced steroids (e.g., androstenediol disulfate, tetrahydrocortisol glucuronide), N-acetyl-amino acids (e.g., N-acetylphenylalanine, N-acetyltyrosine), and markers of endothelial dysfunction and vascular stiffness (e.g., cysteine-glutathione disulfide, 5-hydroxylysine) (Fig1.d). A combined panel of the identified gut microbiota and metabolites significantly improved HTN risk prediction beyond conventional risk factors (AUC improved from 0.77 to 0.84, p<0.001).
Conclusion: Our study characterizes multiple bacterial species associated with incident HTN, and the associations might be partly mediated by circulating metabolites. Inclusion of gut microbiome and associated metabolites facilitates the risk prediction of HTN.
More abstracts on this topic:
A Novel Machine Learning Strategy to Integrate Multi-Omics Data and Detect Genomic Loci and Gene-Environment Interactions for LDL Cholesterol
Li Changwei, Zhang Ruiyuan, Sun Yixi, Chen Jing, Wang Tao, Bazzano Lydia, Kelly Tanika, He Jiang
ACS-Specific Gut Microbial and Metabolic Profiles Reveal Diagnostic and Recovery MarkersXu Jing, Fu Jingyuan, Dai Die, Yang Yanan, Yang Jingang, Gao Shanshan, Wu Chongming, He Jiumin, Chen Weihua, Yang Yue-jin