Final ID: Mo2014
Low Rates Of Escalation Of Lipid Lowering Therapy Amongst Atherosclerotic Cardiovascular Disease Patients With Uncontrolled LDL-C
Abstract Body (Do not enter title and authors here): Background: In patients with atherosclerotic cardiovascular disease (ASCVD), guidelines recommend a reduction in low-density lipoprotein cholesterol (LDL-C) to target levels with statin therapy as required. Where targets are not achieved, escalation to higher intensity statin +/- additional lipid-lowering therapy (LLT) is recommended. It is unknown to what extent adjustments in LLT are made after LLT initiation in routine practice, in relation to measured LDL-C levels.
Aims: To document (i) testing and (ii) achievement of ESC guideline-recommended LDL-C levels (<1.8 mmol/L), in relation to (iii) prescribed LLT regimen during the first two years post-ASCVD diagnosis.
Methods: A retrospective, population-level, observational study using linked anonymised population electronic health record (EHR) data amongst 178696 patients diagnosed with ASCVD between 2010-22, with at least one year of follow-up data. Patients were followed up for two years post-diagnosis, and censored at the point of death, migration, or loss of linked primary care data.
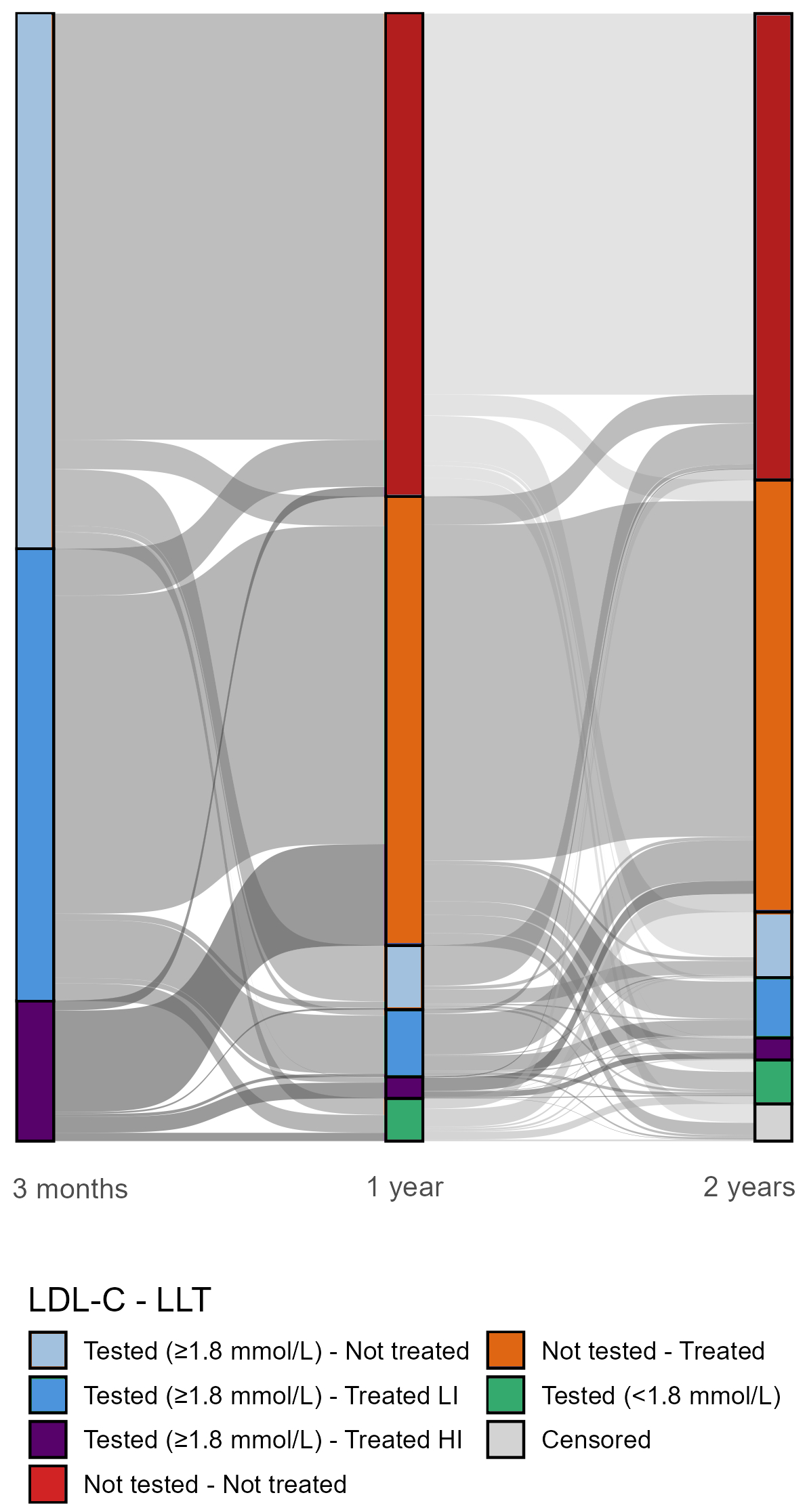
Results: Within 90-days post-diagnosis only 36318 (20.3%) patients had LDL-C levels documented in their EHR, of which 7.3% were <1.8 mmol/L. Of those 23446 (13.1%) patients with LDL-C ≥1.8 mmol/L, 12.7% were receiving high-intensity statin therapy or combination LLT (HI), 40% had lower-intensity statin therapy or other LLT monotherapy (LI) and 47.3% were not treated (Figure 1). During the first-year post-diagnosis, only 4222 (2.4%) had LDL-C tested and 929 (22%) of these achieved target. Of those not achieving target, 15.9% were prescribed HI-LLT, 43.4% LI-LLT, and 40.7% were not treated (Figure 1). Among patients with no test at one-year, 48.1% were prescribed LLT and 51.9% were not treated. Of those not treated, 78.7% received no test or treatment by two-years post-diagnosis. By two-years post-ASCVD diagnosis, 12.5%, 27.2%, and 54.5% were prescribed HI, LI, and no LLT respectively. Figure 1 illustrates that most patients were not tested following 90-days post-diagnosis and remained on the initial LLT regime over the subsequent two-years.
Conclusions: Management of lipids was below guideline-recommended standards in the early years following ASCVD diagnosis in the population, with low levels of testing and escalation in lipid treatment regimen uncommon, even when indicated by documented LDL-C levels. A more rigorous system-wide approach to LLT is required to maximise the potential benefits among these very high-risk patients.
Aims: To document (i) testing and (ii) achievement of ESC guideline-recommended LDL-C levels (<1.8 mmol/L), in relation to (iii) prescribed LLT regimen during the first two years post-ASCVD diagnosis.
Methods: A retrospective, population-level, observational study using linked anonymised population electronic health record (EHR) data amongst 178696 patients diagnosed with ASCVD between 2010-22, with at least one year of follow-up data. Patients were followed up for two years post-diagnosis, and censored at the point of death, migration, or loss of linked primary care data.
Results: Within 90-days post-diagnosis only 36318 (20.3%) patients had LDL-C levels documented in their EHR, of which 7.3% were <1.8 mmol/L. Of those 23446 (13.1%) patients with LDL-C ≥1.8 mmol/L, 12.7% were receiving high-intensity statin therapy or combination LLT (HI), 40% had lower-intensity statin therapy or other LLT monotherapy (LI) and 47.3% were not treated (Figure 1). During the first-year post-diagnosis, only 4222 (2.4%) had LDL-C tested and 929 (22%) of these achieved target. Of those not achieving target, 15.9% were prescribed HI-LLT, 43.4% LI-LLT, and 40.7% were not treated (Figure 1). Among patients with no test at one-year, 48.1% were prescribed LLT and 51.9% were not treated. Of those not treated, 78.7% received no test or treatment by two-years post-diagnosis. By two-years post-ASCVD diagnosis, 12.5%, 27.2%, and 54.5% were prescribed HI, LI, and no LLT respectively. Figure 1 illustrates that most patients were not tested following 90-days post-diagnosis and remained on the initial LLT regime over the subsequent two-years.
Conclusions: Management of lipids was below guideline-recommended standards in the early years following ASCVD diagnosis in the population, with low levels of testing and escalation in lipid treatment regimen uncommon, even when indicated by documented LDL-C levels. A more rigorous system-wide approach to LLT is required to maximise the potential benefits among these very high-risk patients.
More abstracts on this topic:
A Nationwide Italian Network for the Clinical and Genetic Diagnosis of Familial Dyslipidemias: The LIPIGEN registry
Casula Manuela, Galimberti Federica, Olmastroni Elena, Arca Marcello, Averna Maurizio, Catapano Alberico
Absence of standard modifiable risk factors (SMuRF-less) among 5002 Middle Eastern patients with atherosclerotic cardiovascular disease: (Interim analysis from the Jo-SMuRF Study)Aldalal'ah Mo'men, Hammoudeh Ayman, Hamza Ibrahem, Alqudah Mohammad, Khasawneh Hasan, Alomari Sawsan, Alomari Ahmad, H. Assaf Sarah, Zaqqa Ayah, Khatatbeh Moawiah