Final ID: MP1223
Waitlist Outcomes in Patients on VA-ECMO With and Without Left Ventricular Unloading as a Bridge to Heart Transplantation
Abstract Body (Do not enter title and authors here):
Background:
Venoarterial extracorporeal membrane oxygenation (VA-ECMO) is increasingly used to bridge patients to heart transplantation following the 2018 UNOS heart allocation policy that prioritized patients on VA-ECMO support due to their high waitlist mortality. Many VA-ECMO patients employ concomitant left ventricular (LV) unloading strategies, such as intra-aortic balloon pump (IABP) or Impella (ECPella); however, the clinical utility of these methods in improving waitlist outcomes remains unclear.
Research Question:
To compare clinical outcomes of waitlisted patients between those who received an LV unloading strategy and those who did not while being supported by VA-ECMO as a bridge to heart transplantation.
Methods:
Using the UNOS registry, we retrospectively analyzed adult first-time heart transplant candidates supported by VA-ECMO alone (Loading) versus VA-ECMO plus LV unloading (Unloading) from October 18, 2018, to March 30, 2022. Competing risks analysis and multivariable Cox proportional hazards models were used to evaluate outcomes of death/deterioration and transplantation on the waitlist while adjusting for age, gender, ethnicity, and mechanical ventilation.
Results:
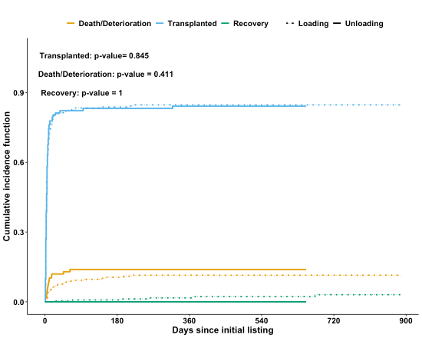
In total, 369 patients were included: 252 in the Loading group, and 117 in Unloading. Baseline differences indicated higher illness severity in the Unloading group (more mechanical ventilation [35.9% vs. 22.2%, p=0.008] and inotrope use [64.1% vs. 48.0%, p=0.006]). Despite this, there was no statistically significant difference in waitlist death/deterioration between groups (adjusted subdistribution hazard ratio [sdHR]: 1.304; 95% CI: 0.709–2.398; p=0.39). However, the adjusted cause-specific hazard ratio (csHR) was 1.618 (95% CI: 0.860–3.043; p=0.14), suggests a nonsignificant trend toward higher instantaneous risk of death/deterioration in the ECMO unloading alone group. Subgroup analysis comparing ECMO only, ECMO+IABP, and ECPella also showed no significant differences.
Conclusion:
LV unloading in patients supported by VA-ECMO did not significantly alter waitlist outcomes in this cohort despite being used in sicker patients. Nonetheless, we did identify a trend towards increased risk of death/deterioration on the waitlist among the Unloading group. Larger studies are warranted to determine if an unloading device should be considered in waitlist prioritization for future organ allocation policy iterations.
Background:
Venoarterial extracorporeal membrane oxygenation (VA-ECMO) is increasingly used to bridge patients to heart transplantation following the 2018 UNOS heart allocation policy that prioritized patients on VA-ECMO support due to their high waitlist mortality. Many VA-ECMO patients employ concomitant left ventricular (LV) unloading strategies, such as intra-aortic balloon pump (IABP) or Impella (ECPella); however, the clinical utility of these methods in improving waitlist outcomes remains unclear.
Research Question:
To compare clinical outcomes of waitlisted patients between those who received an LV unloading strategy and those who did not while being supported by VA-ECMO as a bridge to heart transplantation.
Methods:
Using the UNOS registry, we retrospectively analyzed adult first-time heart transplant candidates supported by VA-ECMO alone (Loading) versus VA-ECMO plus LV unloading (Unloading) from October 18, 2018, to March 30, 2022. Competing risks analysis and multivariable Cox proportional hazards models were used to evaluate outcomes of death/deterioration and transplantation on the waitlist while adjusting for age, gender, ethnicity, and mechanical ventilation.
Results:
In total, 369 patients were included: 252 in the Loading group, and 117 in Unloading. Baseline differences indicated higher illness severity in the Unloading group (more mechanical ventilation [35.9% vs. 22.2%, p=0.008] and inotrope use [64.1% vs. 48.0%, p=0.006]). Despite this, there was no statistically significant difference in waitlist death/deterioration between groups (adjusted subdistribution hazard ratio [sdHR]: 1.304; 95% CI: 0.709–2.398; p=0.39). However, the adjusted cause-specific hazard ratio (csHR) was 1.618 (95% CI: 0.860–3.043; p=0.14), suggests a nonsignificant trend toward higher instantaneous risk of death/deterioration in the ECMO unloading alone group. Subgroup analysis comparing ECMO only, ECMO+IABP, and ECPella also showed no significant differences.
Conclusion:
LV unloading in patients supported by VA-ECMO did not significantly alter waitlist outcomes in this cohort despite being used in sicker patients. Nonetheless, we did identify a trend towards increased risk of death/deterioration on the waitlist among the Unloading group. Larger studies are warranted to determine if an unloading device should be considered in waitlist prioritization for future organ allocation policy iterations.
More abstracts on this topic:
ANALYSIS OF GUIDELINES IN VASCULAR NEUROLOGY AND STROKE PUBLISHED BETWEEN 2012 AND 2023.
Martins Hanna, Peixoto Vitória, De Souza Jorge Luiz, Gomes Gustavo, Andrade Joao, Sampaio Gisele, Lopes Renato, Santos Marcella, Ikeda Raissa, Sanchez Nascimento Paula, Romera Lopes Carlos Felipe, Mauricio Rebeca
Clinical Outcomes in Peripartum Cardiomyopathy Complicated by Cardiogenic Shock: A Retrospective Multi-Center Cohort StudyParcha Vibhu, Joly Joanna, Mcelwee Samuel, Clarkson Stephen, Scheinuk John, Josey Gina, Hyder Syed, Hasnie Usman, Saleh Ahmed, Hasnie Ammar, Sinkey Rachel, Cribbs Marc