Final ID: TH907
Assessing the Impact of Unmet Social Needs on Clinical Outcomes in Reproductive-Aged Women with Atrial Fibrillation
Abstract Body: Objective
To explore the association between unmet social needs (USN) and atrial fibrillation (AF) outcomes in reproductive aged women.
Background
Individuals with USN often face barriers to regular medical care. In patients with AF, regular follow up with appropriate intervention is essential to mitigate long term complications. Thus, it is crucial to identify risk factors that limit monitoring and intervention of AF.
Methods
We included reproductive aged women (18-50 years) with hospital admissions due to AF from the 2013 to 2024 AHA Get With The Guidelines-AF registry. USN were defined as lacking or using public insurance (Medicaid and Medicare, which was used as a surrogate of low income and/or disability), homelessness, low education level, unemployment, financial strain, substance abuse and a lack of environmental safety. Rhythm control strategies included cardioversion, ablation, or anti-arrhythmic therapies. AF recurrence was defined as a discharge rhythm of AF and used as a marker of poor outcomes. Statistical analysis to compare baseline characteristics and outcomes between those with and without USN was performed with Chi-square test and t-test.
Results
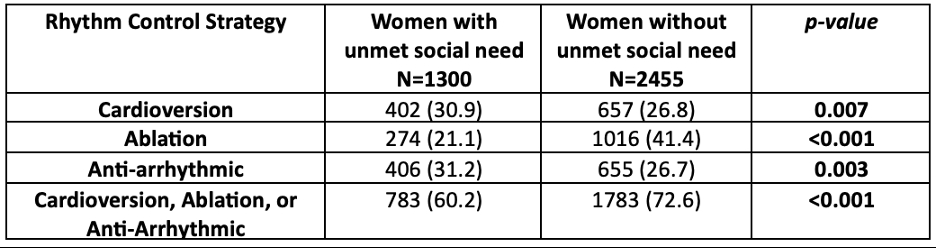
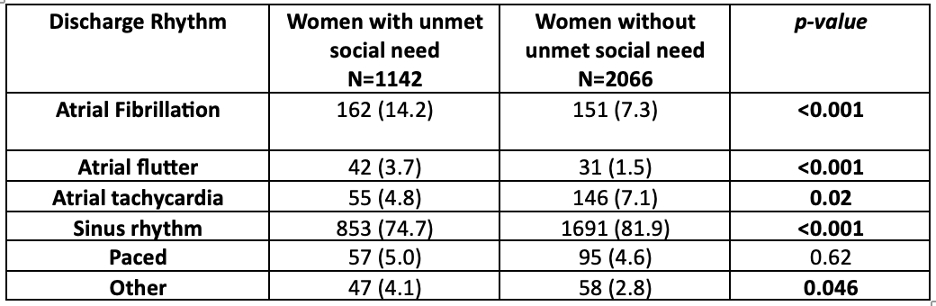
Our study included 3,755 reproductive age women with a mean age of 42.4 (SD 7.1). Of this cohort, 34.6% were identified to have USN and 65.4% did not have an USN. A higher proportion of rhythm control strategies were used in the women without USN group (72.6% vs. 60.2%, p<0.001). Women with USN were less likely to have an AF ablation than in women without USN (21.1% vs. 41.4%, p<0.001) (Table 1). Of those with USN, 14.2% had a discharge rhythm of AF versus 7.3% without a USN (p<0.001). Additionally, sinus rhythm at discharge was observed in 74.7% of women with USN compared to 81.9% in those without an USN (p <0.001, Table 2).
Conclusion
In our study, women with an USN had a significantly higher rate of AF at discharge and lower rate of AF ablation, suggesting a potential link between USN, worse AF-related outcomes, and inequities in rhythm control strategies. These findings underscore the importance of identifying USN and highlight the need for targeted interventions to support this vulnerable population.
To explore the association between unmet social needs (USN) and atrial fibrillation (AF) outcomes in reproductive aged women.
Background
Individuals with USN often face barriers to regular medical care. In patients with AF, regular follow up with appropriate intervention is essential to mitigate long term complications. Thus, it is crucial to identify risk factors that limit monitoring and intervention of AF.
Methods
We included reproductive aged women (18-50 years) with hospital admissions due to AF from the 2013 to 2024 AHA Get With The Guidelines-AF registry. USN were defined as lacking or using public insurance (Medicaid and Medicare, which was used as a surrogate of low income and/or disability), homelessness, low education level, unemployment, financial strain, substance abuse and a lack of environmental safety. Rhythm control strategies included cardioversion, ablation, or anti-arrhythmic therapies. AF recurrence was defined as a discharge rhythm of AF and used as a marker of poor outcomes. Statistical analysis to compare baseline characteristics and outcomes between those with and without USN was performed with Chi-square test and t-test.
Results
Our study included 3,755 reproductive age women with a mean age of 42.4 (SD 7.1). Of this cohort, 34.6% were identified to have USN and 65.4% did not have an USN. A higher proportion of rhythm control strategies were used in the women without USN group (72.6% vs. 60.2%, p<0.001). Women with USN were less likely to have an AF ablation than in women without USN (21.1% vs. 41.4%, p<0.001) (Table 1). Of those with USN, 14.2% had a discharge rhythm of AF versus 7.3% without a USN (p<0.001). Additionally, sinus rhythm at discharge was observed in 74.7% of women with USN compared to 81.9% in those without an USN (p <0.001, Table 2).
Conclusion
In our study, women with an USN had a significantly higher rate of AF at discharge and lower rate of AF ablation, suggesting a potential link between USN, worse AF-related outcomes, and inequities in rhythm control strategies. These findings underscore the importance of identifying USN and highlight the need for targeted interventions to support this vulnerable population.
More abstracts on this topic:
Adverse Outcomes Following Atrial Fibrillation Ablation in Patients With Connective Tissue Disease: A Propensity-Matched Real-World Analysis
Rayyan Abdallah, Obeidat Omar, Alqudah Qusai, Khasawneh Tawfiq, Alomari Ahmad, Mestarihi Aseed, Alnabahneh Nizar, Nasser Hesham, Tong Ann
1-Year Outcomes After Cardioversion With and Without Anticoagulation in Patients With Left Atrial Appendage Occlusion: A Propensity-Matched AnalysisThangjui Sittinun, Trongtorsak Angkawipa, Kewcharoen Jakrin, Thyagaturu Harshith, Watson Hangyu, Mensah Samuel, Balla Sudarshan, Navaravong Leenhapong