Final ID: TU154
Apparent Resistant Hypertension in US Adults: Temporal Trends, Renal Denervation Eligibility, and the Impact of Isolated Systolic Hypertension
Abstract Body: Background:
The 2025 AHA/ACC (American Heart Association/American College of Cardiology) and ESC/ESH (European Society of Cardiology/European Society of Hypertension) guidelines introduced new diagnostic and risk-based blood pressure (BP) thresholds, while renal denervation (RDN) has emerged as a device-based therapy for resistant hypertension. The impact of these guidelines on the prevalence, trends, and RDN eligibility among US adults with apparent resistant hypertension (aTRH) remains unclear.
Methods:
We analyzed adults aged ≥20 years treated for hypertension from NHANES 2005–2020. aTRH was defined by AHA/ACC (uncontrolled BP on ≥3 antihypertensive medications including a diuretic, or controlled BP on ≥4) and ESC/ESH (office BP ≥140/90 mmHg on ≥3 drug classes including a diuretic) criteria. aTRH cases were stratified by 2025 AHA/ACC risk-based thresholds. RDN eligibility was assessed using strict (SBP ≥140 and DBP ≥90 mmHg) and inclusive (including isolated systolic hypertension) criteria among patients on optimal therapy with eGFR ≥40 mL/min/1.73m2. Survey-weighted and multivariable regression analyses estimated national prevalence, temporal trends, and predictors of RDN eligibility.
Results:
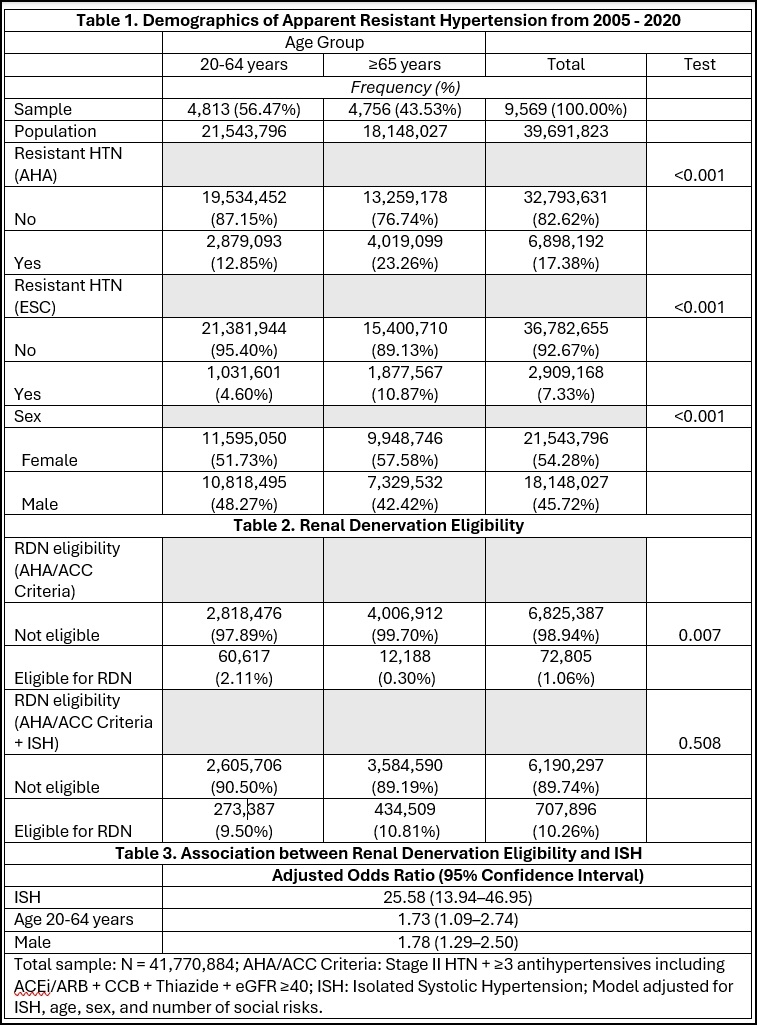
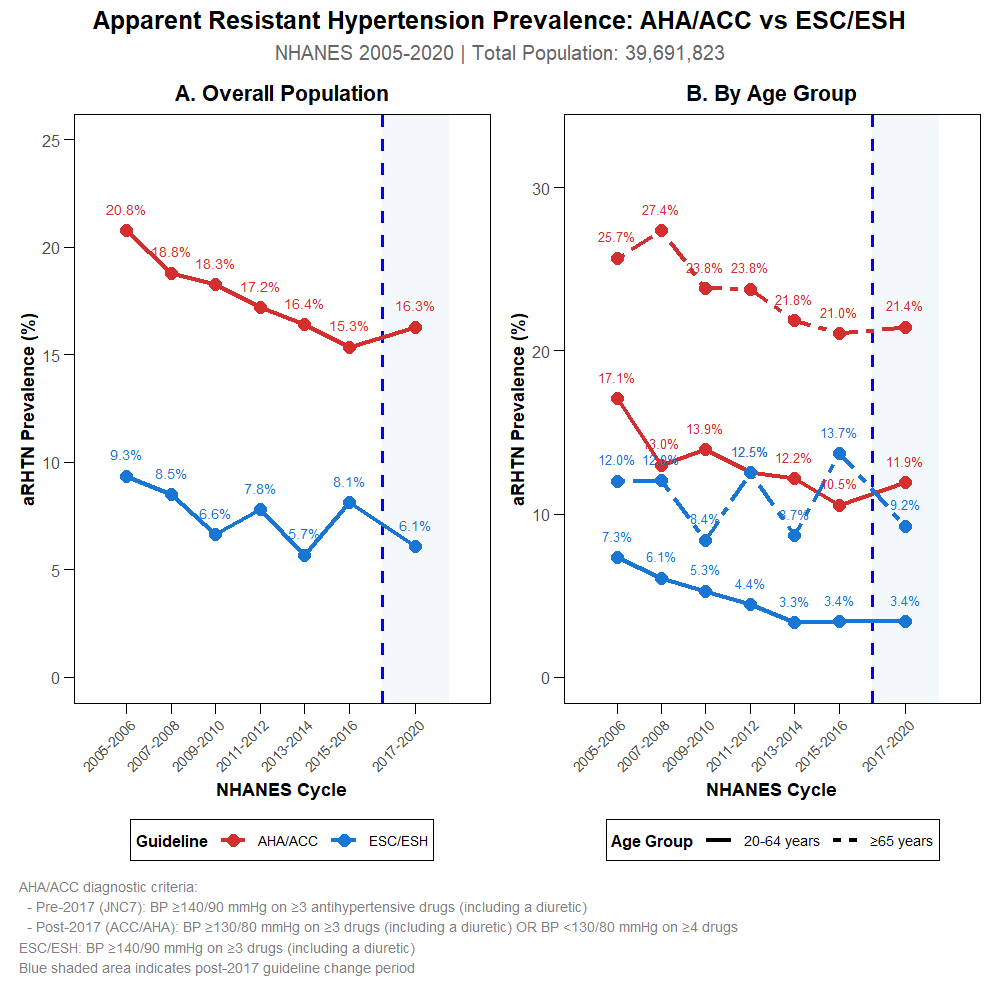
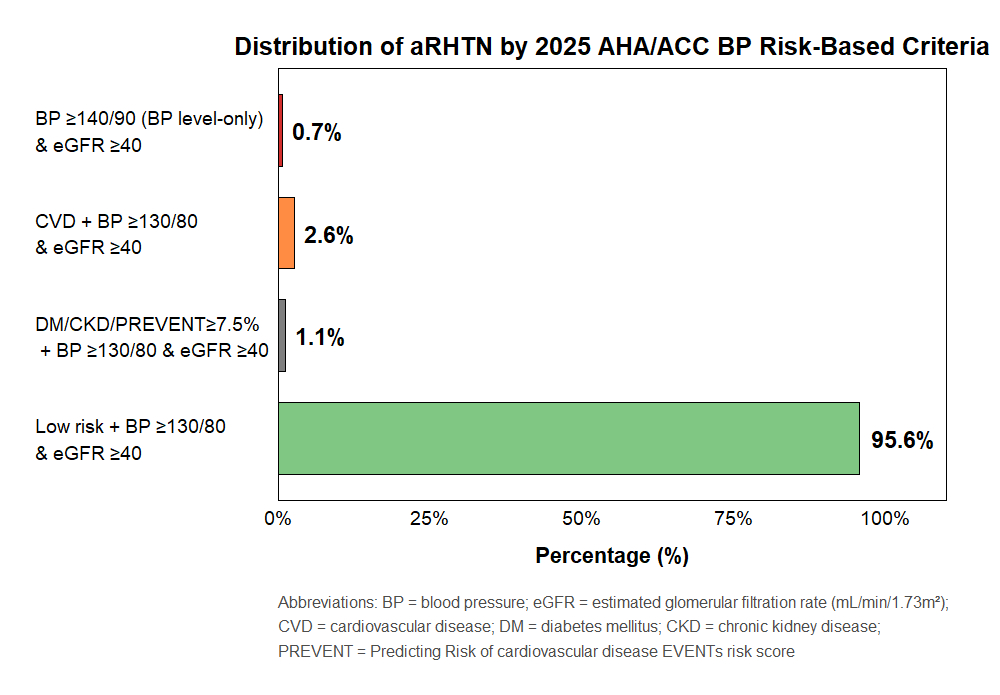
Among 39.7 million US adults with treated hypertension, aTRH prevalence by AHA/ACC criteria declined from 21.6% (2005–06) to 16.6% (2017–20); ESC/ESH criteria yielded lower rates (6.4–9.6%). The AHA/ACC definition identified 2.4 times more cases than ESC/ESH (17.2% vs 7.3%). The prevalence was higher in adults ≥65 years versus 20–64 years (23.3% vs 12.9%, p<0.001). Multivariable regression showed older age ≥65 years (adjusted OR 1.73, 95% CI: 1.09–2.74) and male sex (OR 1.78, 95% CI: 1.29–2.50) were significantly associated with RDN eligibility. By 2025 risk stratification, 95.9% of aTRH cases were low-risk, 3.7% had CVD, 1.8% had diabetes/CKD/elevated PREVENT score, and 0.1% met BP-only criteria. Among 1,899 aTRH patients, 72,805 (1.06%) met strict RDN eligibility; inclusion of isolated systolic hypertension increased eligibility tenfold (10.26%; adjusted OR 25.58, 95% CI 8.5–12.3).
Conclusions:
aTRH prevalence in US adults varies substantially by guideline definition and has declined over time. Regression analysis identified age and sex as predictors of RDN eligibility. Integrating risk-based thresholds into aTRH management and expanding RDN criteria to include isolated systolic hypertension may enhance patient selection and optimize hypertension control.
The 2025 AHA/ACC (American Heart Association/American College of Cardiology) and ESC/ESH (European Society of Cardiology/European Society of Hypertension) guidelines introduced new diagnostic and risk-based blood pressure (BP) thresholds, while renal denervation (RDN) has emerged as a device-based therapy for resistant hypertension. The impact of these guidelines on the prevalence, trends, and RDN eligibility among US adults with apparent resistant hypertension (aTRH) remains unclear.
Methods:
We analyzed adults aged ≥20 years treated for hypertension from NHANES 2005–2020. aTRH was defined by AHA/ACC (uncontrolled BP on ≥3 antihypertensive medications including a diuretic, or controlled BP on ≥4) and ESC/ESH (office BP ≥140/90 mmHg on ≥3 drug classes including a diuretic) criteria. aTRH cases were stratified by 2025 AHA/ACC risk-based thresholds. RDN eligibility was assessed using strict (SBP ≥140 and DBP ≥90 mmHg) and inclusive (including isolated systolic hypertension) criteria among patients on optimal therapy with eGFR ≥40 mL/min/1.73m2. Survey-weighted and multivariable regression analyses estimated national prevalence, temporal trends, and predictors of RDN eligibility.
Results:
Among 39.7 million US adults with treated hypertension, aTRH prevalence by AHA/ACC criteria declined from 21.6% (2005–06) to 16.6% (2017–20); ESC/ESH criteria yielded lower rates (6.4–9.6%). The AHA/ACC definition identified 2.4 times more cases than ESC/ESH (17.2% vs 7.3%). The prevalence was higher in adults ≥65 years versus 20–64 years (23.3% vs 12.9%, p<0.001). Multivariable regression showed older age ≥65 years (adjusted OR 1.73, 95% CI: 1.09–2.74) and male sex (OR 1.78, 95% CI: 1.29–2.50) were significantly associated with RDN eligibility. By 2025 risk stratification, 95.9% of aTRH cases were low-risk, 3.7% had CVD, 1.8% had diabetes/CKD/elevated PREVENT score, and 0.1% met BP-only criteria. Among 1,899 aTRH patients, 72,805 (1.06%) met strict RDN eligibility; inclusion of isolated systolic hypertension increased eligibility tenfold (10.26%; adjusted OR 25.58, 95% CI 8.5–12.3).
Conclusions:
aTRH prevalence in US adults varies substantially by guideline definition and has declined over time. Regression analysis identified age and sex as predictors of RDN eligibility. Integrating risk-based thresholds into aTRH management and expanding RDN criteria to include isolated systolic hypertension may enhance patient selection and optimize hypertension control.
More abstracts on this topic:
A Systems-Level Intervention Improved Alignment of Initial Hypertension Pharmacotherapy with Clinical Practice Guidelines at a Veterans Affairs Medical Center
Jain Bijal, Dada Adedoyin, Gaddam Meghana, Grabos Lauren, Atoe Eghosa, Escalona Matthew, White Samantha, Rivera Eleanor
Aldosterone Dysregulation After Antihypertensive Treatments Among Patients With Hypertension in the United States: Findings From the Breakthrough Aldosterone Real-World StudyRader Florian, Chertow Glenn, Agiro Abiy, Satija Ambika, Chen Jingyi, Lemus Wirtz Esteban, Brahmbhatt Ashish, Luan Shan, Kang Zoey, Mu Fan