Final ID: 03
Impact of SGLT 2 inhibitors and GLP-1 receptor agonists dual therapy on Cardiovascular Outcomes in patients with Heart Failure with Reduced Ejection Fraction and Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD): A Propensity-Matched Cohort
Abstract Body: Introduction:
Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) affects 20–30% of patients with heart failure (HF). Conversely, patients with MASLD have a 1.5-fold higher risk of developing HF of which about 24% is HFrEF. SGLT2 inhibitors (SGLT2i) and GLP-1 receptor agonists (GLP-1 RAs) have shown to offer benefits in patients with HFrEF. Moreover, GLP-1 RAs have also shown to be beneficial in MASLD. However, the impact of combined SGLT2i + GLP-1 RA therapy on patients with HFrEF coexisting with MASLD is not studied.
Objective:
To compare major adverse cardiovascular events (MACE), cardiac arrest, and all-cause mortality in HFrEF patients with MASLD treated with SGLT2i + GLP-1 RA vs. SGLT2i only.
Methods:
We conducted a propensity score-matched (PSM) retrospective cohort study using the TriNetX Global Network (160 organizations, 2005-2025). Using ICD-10 codes, we identified adults with systolic heart failure and MASLD (Defined as fatty liver plus ≥1 metabolic condition: hypertension, diabetes, obesity or dyslipidemia) and excluded those with diastolic HF and alcoholic liver disease. Patients were divided into two groups: combination therapy (SGLT2i + GLP-1 RA) and SGLT2i only. Outcomes included three-point MACE, cardiac arrest and all-cause mortality. PSM was based on demographics, comorbidities, HF risk factors, liver conditions, and HF background therapy.
Results:
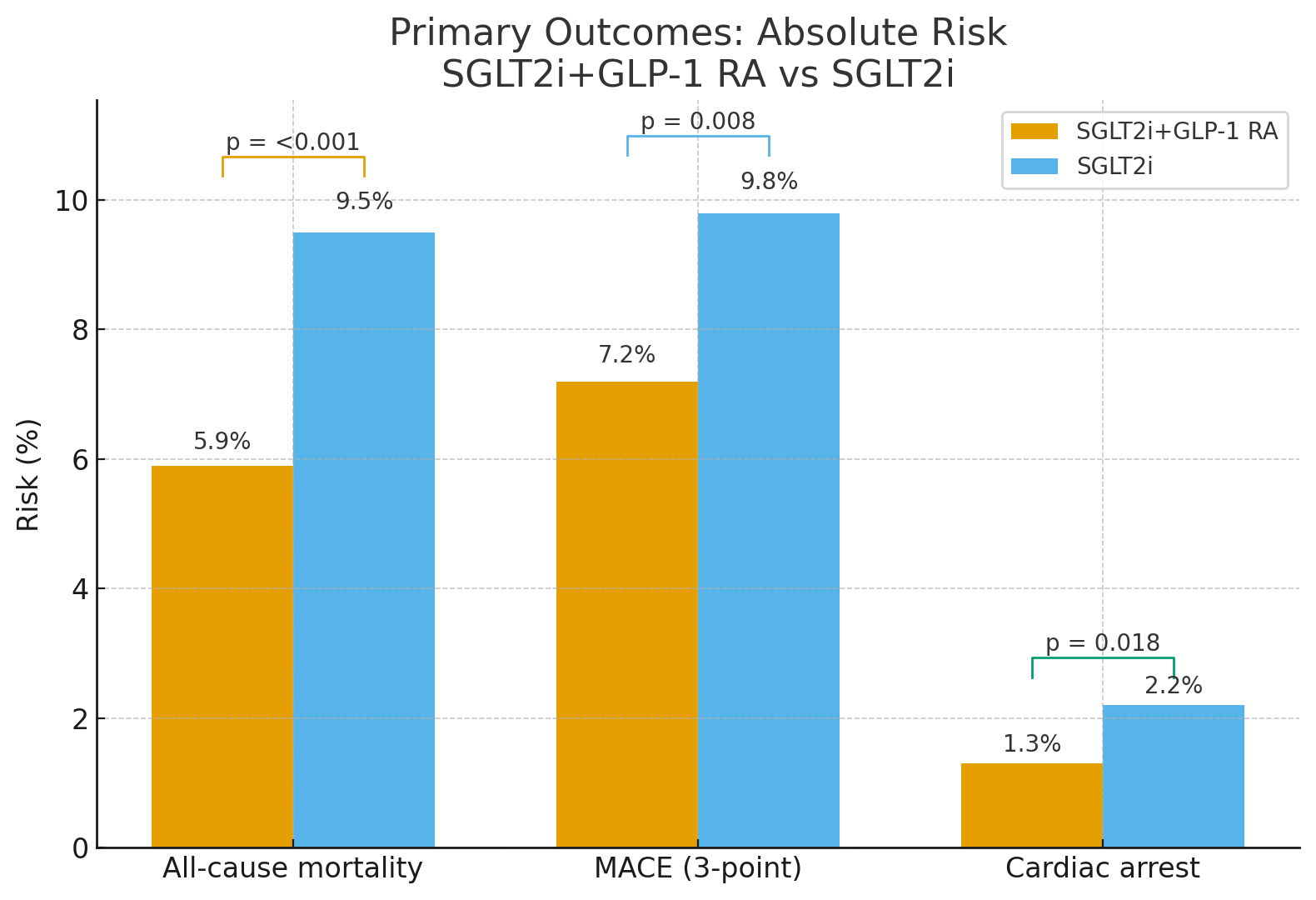
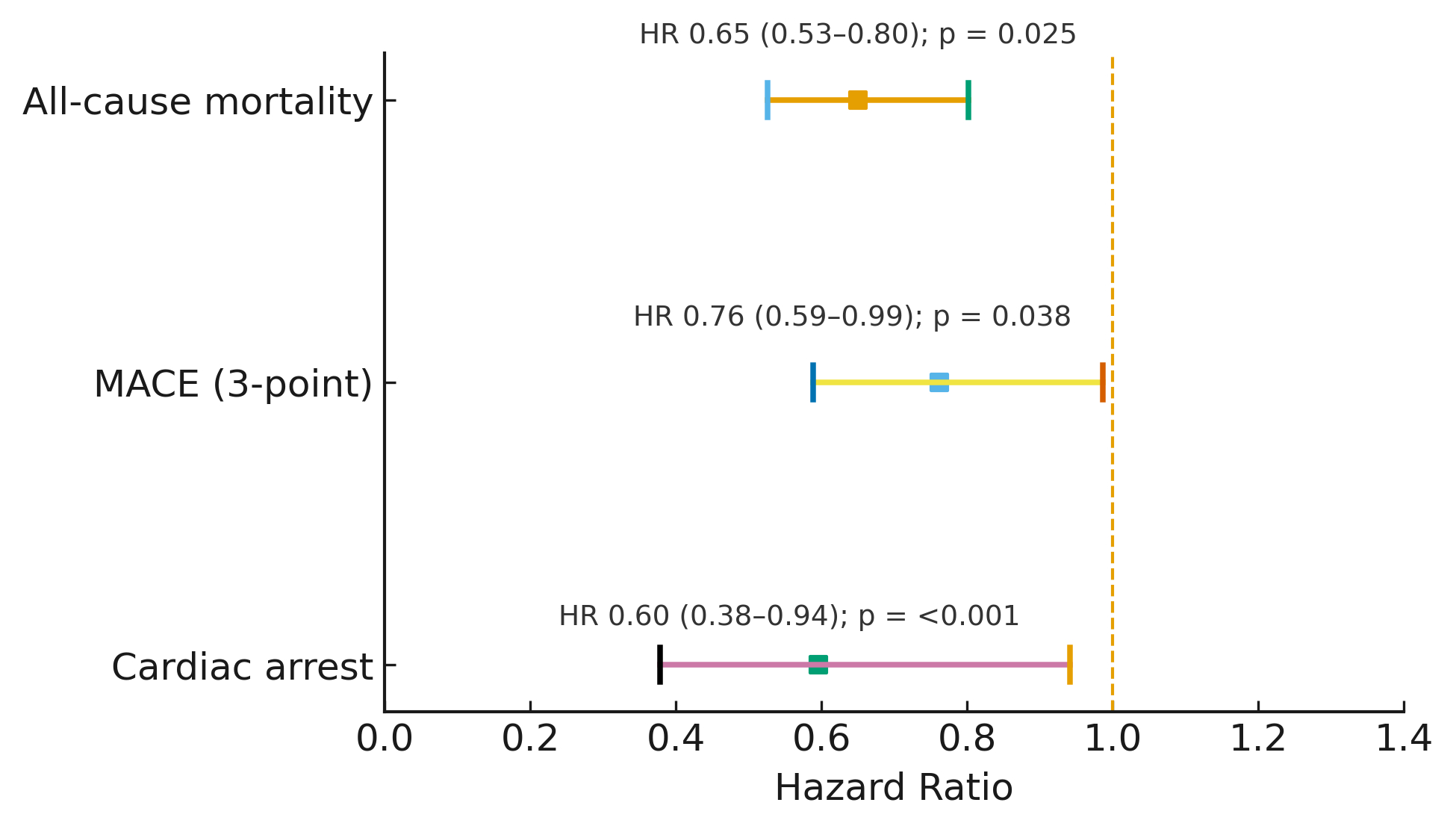
We identified 2,554 patients on combination therapy and 13,455 on monotherapy that were reduced to 2,544 per group after PSM. The mean age for both cohorts was ~ 59 years, with about 61% males, a mean BMI of 36.5, and mean follow-up of ~ 2 years. A significant reduction was found with combination therapy for three-point MACE (RR 0.732; 95% CI (0.571, 0.937); HR 0.762, 95% CI (0.588, 0.986) p 0.038), all-cause mortality (RR: 0.619, 95% CI (0.505, 0.759) HR 0.650, 95% CI (0.526, 0.802) p <0.001), and cardiac arrest (RR 0.570 , 95% CI (0.363, 0.896); HR 0.596 , 95% CI (0.378, 0.941) , p 0.025) despite the statistically insignificant difference in HbA1c reduction [0.142, 95% CI (-0.034, 0.318) , p = 0.11].
Conclusion:
In HFrEF patients with MASLD, SGLT2i + GLP-1 RA combined therapy had significantly better cardiovascular outcomes vs. those on SGLT2i alone that was not attributable to HbA1c reduction supporting the benefit of combination therapy and perhaps also exploring benefits of adding GLP-1 RA to GDMT in this high-risk population warranting further prospective studies.
Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) affects 20–30% of patients with heart failure (HF). Conversely, patients with MASLD have a 1.5-fold higher risk of developing HF of which about 24% is HFrEF. SGLT2 inhibitors (SGLT2i) and GLP-1 receptor agonists (GLP-1 RAs) have shown to offer benefits in patients with HFrEF. Moreover, GLP-1 RAs have also shown to be beneficial in MASLD. However, the impact of combined SGLT2i + GLP-1 RA therapy on patients with HFrEF coexisting with MASLD is not studied.
Objective:
To compare major adverse cardiovascular events (MACE), cardiac arrest, and all-cause mortality in HFrEF patients with MASLD treated with SGLT2i + GLP-1 RA vs. SGLT2i only.
Methods:
We conducted a propensity score-matched (PSM) retrospective cohort study using the TriNetX Global Network (160 organizations, 2005-2025). Using ICD-10 codes, we identified adults with systolic heart failure and MASLD (Defined as fatty liver plus ≥1 metabolic condition: hypertension, diabetes, obesity or dyslipidemia) and excluded those with diastolic HF and alcoholic liver disease. Patients were divided into two groups: combination therapy (SGLT2i + GLP-1 RA) and SGLT2i only. Outcomes included three-point MACE, cardiac arrest and all-cause mortality. PSM was based on demographics, comorbidities, HF risk factors, liver conditions, and HF background therapy.
Results:
We identified 2,554 patients on combination therapy and 13,455 on monotherapy that were reduced to 2,544 per group after PSM. The mean age for both cohorts was ~ 59 years, with about 61% males, a mean BMI of 36.5, and mean follow-up of ~ 2 years. A significant reduction was found with combination therapy for three-point MACE (RR 0.732; 95% CI (0.571, 0.937); HR 0.762, 95% CI (0.588, 0.986) p 0.038), all-cause mortality (RR: 0.619, 95% CI (0.505, 0.759) HR 0.650, 95% CI (0.526, 0.802) p <0.001), and cardiac arrest (RR 0.570 , 95% CI (0.363, 0.896); HR 0.596 , 95% CI (0.378, 0.941) , p 0.025) despite the statistically insignificant difference in HbA1c reduction [0.142, 95% CI (-0.034, 0.318) , p = 0.11].
Conclusion:
In HFrEF patients with MASLD, SGLT2i + GLP-1 RA combined therapy had significantly better cardiovascular outcomes vs. those on SGLT2i alone that was not attributable to HbA1c reduction supporting the benefit of combination therapy and perhaps also exploring benefits of adding GLP-1 RA to GDMT in this high-risk population warranting further prospective studies.
More abstracts on this topic:
Accelerometer-Measured Sedentary Behavior and Future Cardiovascular Disease
Ajufo Ezimamaka, Kany Shinwan, Ramo Joel, Churchill Timothy, Guseh James, Aragam Krishna, Ellinor Patrick, Khurshid Shaan
Acute Administration of The Novel Cardiac Sarcomere Modulator EDG-7500, Improves Ventricular Filling While Preserving LVEF In Dogs with Pacing Induced Left-Ventricular Systolic DysfunctionEvanchik Marc, Emter Craig, Del Rio Carlos, Roof Steve, St Clair Sydney, Russell Alan, Henze Marcus, Semigran Marc