Final ID: TH905
Social Drivers of Health Screening and In-Hospital Outcomes for Cardiovascular Patients in Oregon
Abstract Body: Background: Social drivers of health (SDOH) are tied to cardiovascular disease (CVD) prevalence, disease progression, and outcomes. Federal requirements mandate SDOH screening in inpatient settings.
Objective: Examine rates and predictors of in-hospital SDOH screening, positive screens, and outcomes for CVD patients.
Methods: Retrospective cohort study of CVD patients from 7 Providence Oregon hospitals between 10/01/2023 – 4/24/25. In-hospital admissions with a CVD primary diagnosis were included. SDOH screening included the following domains: food, housing, transportation, utilities, financial strain, and intimate partner violence. Patient characteristics, SDOH screening data, and in-hospital outcomes were obtained from the electronic medical record. Rural-urban commuting area (RUCA) and the Center for Disease Control & Prevention social vulnerability index (SVI) were linked to patient zip code. The primary outcome was a positive screen in ≥1 SDOH domain. Secondary outcomes were receiving care by a CVD physician or advanced practice clinician, cardiac ICU stay, length of stay (LOS), mortality, and readmission. Logistic regression models accounting for age, sex, race, ethnicity, primary language, BMI, insurance, RUCA, SVI, and SDOH screening were run, with a random effect for screening hospital.
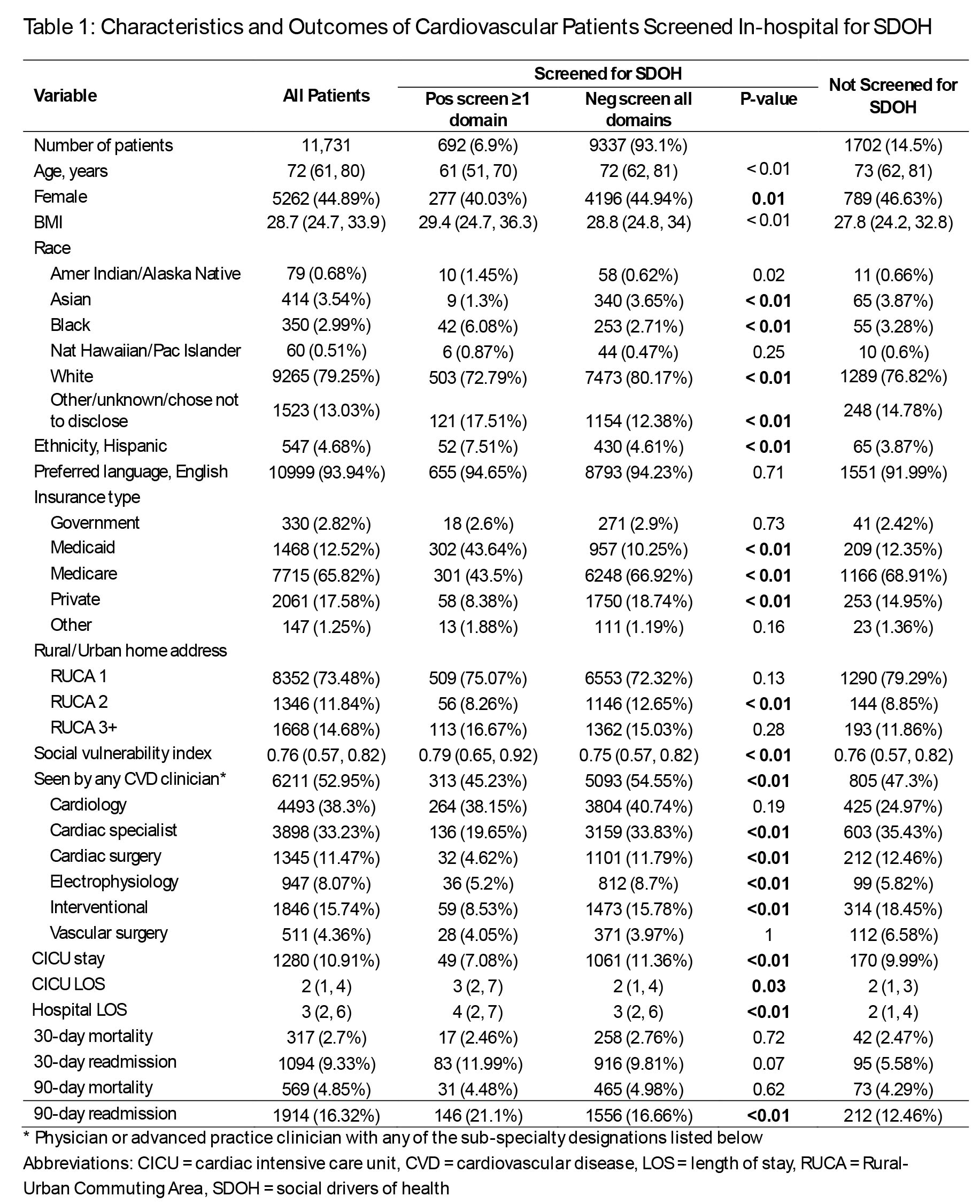
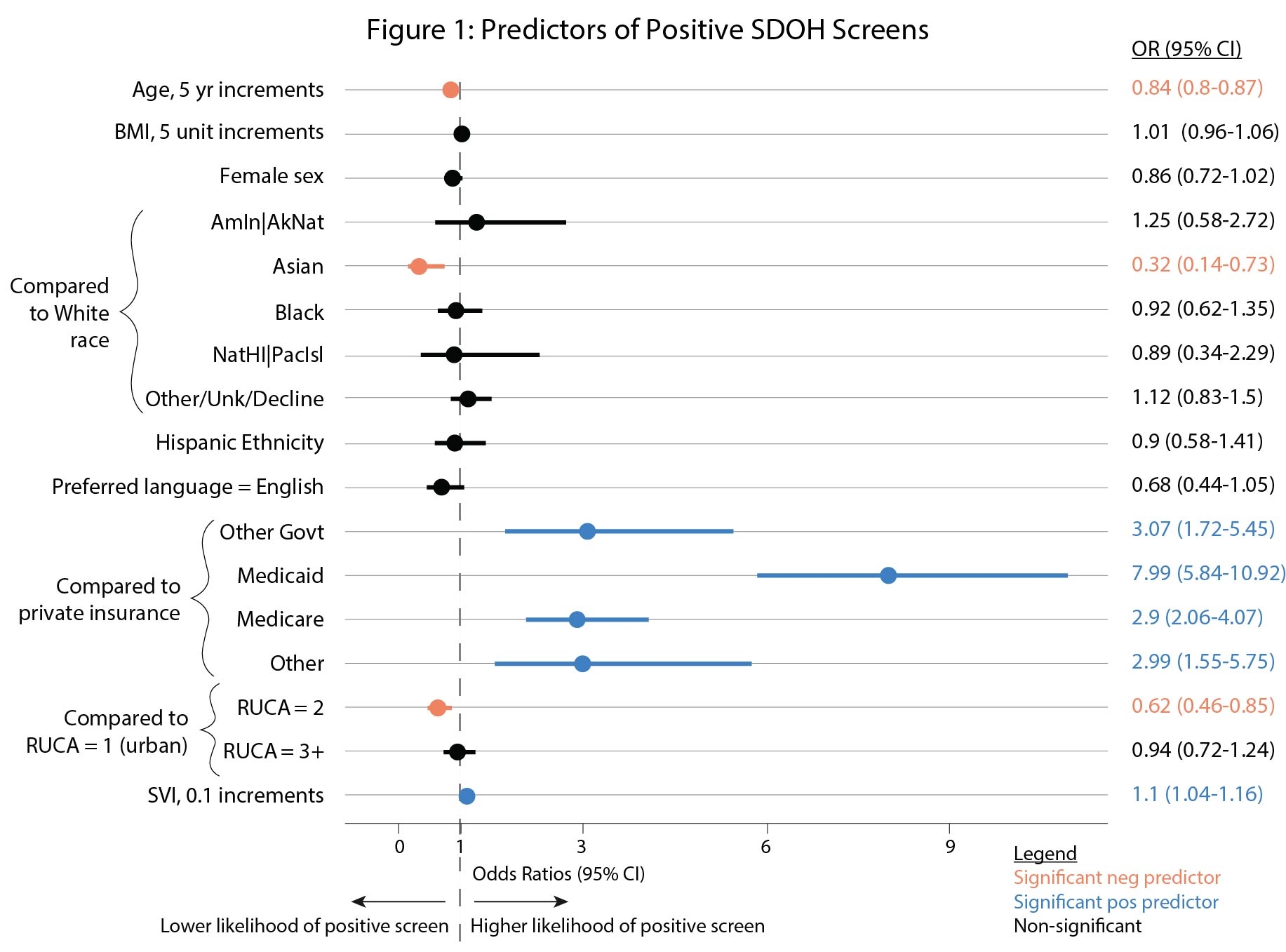
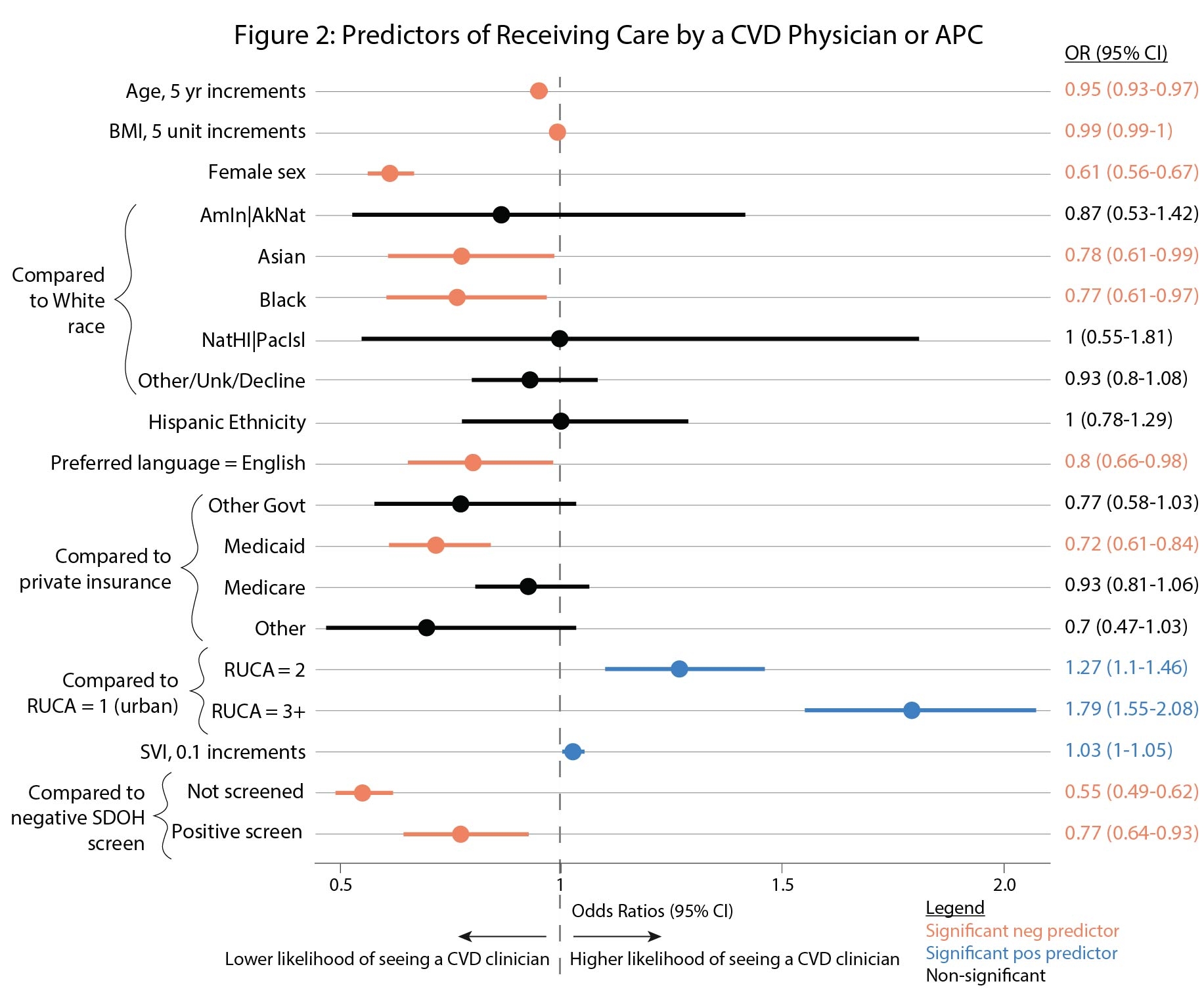
Results: There were 11,731 CVD patients, the majority of whom were screened for SDOH (85.5%) (Table 1). Of screened patients, 6.9% screened positive in any domain, with the highest rates in housing (3.6%) and food (2.1%). Patients with positive screens were younger, more often Black, of other or unknown races, Hispanic, with higher rates of Medicaid insurance, and higher SVI (Table 1). Patients with positive screens had lower rates of receiving care by a CVD clinician (45% vs 55%), longer LOS, and higher 90-day readmission (Table 1). Patients with Medicaid were 8x more likely to screen positive than patients with private insurance, and those with Medicare, other government, or other insurance were ~3x more likely (Figure 1). Patients who screened positive were 23% less likely to see a CVD clinician, as were female (39%), Asian (22%), Black (23%), non-English speaking (20%), and Medicaid patients (28%, Figure 2).
Conclusions: High rates of in-patient SDOH screening were observed. Positive screens were associated with lower rates of specialty care, longer LOS, and higher readmissions, suggesting room for improvement in care processes following a positive screen.
Objective: Examine rates and predictors of in-hospital SDOH screening, positive screens, and outcomes for CVD patients.
Methods: Retrospective cohort study of CVD patients from 7 Providence Oregon hospitals between 10/01/2023 – 4/24/25. In-hospital admissions with a CVD primary diagnosis were included. SDOH screening included the following domains: food, housing, transportation, utilities, financial strain, and intimate partner violence. Patient characteristics, SDOH screening data, and in-hospital outcomes were obtained from the electronic medical record. Rural-urban commuting area (RUCA) and the Center for Disease Control & Prevention social vulnerability index (SVI) were linked to patient zip code. The primary outcome was a positive screen in ≥1 SDOH domain. Secondary outcomes were receiving care by a CVD physician or advanced practice clinician, cardiac ICU stay, length of stay (LOS), mortality, and readmission. Logistic regression models accounting for age, sex, race, ethnicity, primary language, BMI, insurance, RUCA, SVI, and SDOH screening were run, with a random effect for screening hospital.
Results: There were 11,731 CVD patients, the majority of whom were screened for SDOH (85.5%) (Table 1). Of screened patients, 6.9% screened positive in any domain, with the highest rates in housing (3.6%) and food (2.1%). Patients with positive screens were younger, more often Black, of other or unknown races, Hispanic, with higher rates of Medicaid insurance, and higher SVI (Table 1). Patients with positive screens had lower rates of receiving care by a CVD clinician (45% vs 55%), longer LOS, and higher 90-day readmission (Table 1). Patients with Medicaid were 8x more likely to screen positive than patients with private insurance, and those with Medicare, other government, or other insurance were ~3x more likely (Figure 1). Patients who screened positive were 23% less likely to see a CVD clinician, as were female (39%), Asian (22%), Black (23%), non-English speaking (20%), and Medicaid patients (28%, Figure 2).
Conclusions: High rates of in-patient SDOH screening were observed. Positive screens were associated with lower rates of specialty care, longer LOS, and higher readmissions, suggesting room for improvement in care processes following a positive screen.
More abstracts on this topic:
Association of Sociodemographic Characteristics on Costs of Care in Patients with Obstructive Hypertrophic Cardiomyopathy
Reza Nosheen, Butzner Michael, Batra Kirti, Amos Qiana, Buikema Ami, Anderson Amy, Shreay Sanatan, Owens Anjali
A Measurement Model of Socioeconomic Status and its Association with Cardiovascular Disease in the Hispanic Community Health Study/Study of LatinosCordero Christina, Llabre Maria, Romaker Emma, Kobayashi Marissa, Gianola Morgan, Gallo Linda, Isasi Carmen, Perreira Krista, Corsino Leonor, Zhou Laura