Final ID: TU281
Associations Between Prepregnancy Lipoprotein(a) and Birth Outcomes: The Hispanic Community Health Study/Study of Latinos
Abstract Body: Background: Lipoprotein(a) [Lp(a)] is a highly atherogenic, prothrombotic, and proinflammatory atherosclerotic cardiovascular disease risk factor that may influence placenta-mediated pregnancy complications, although mechanisms remain poorly understood. Existing evidence linking Lp(a) with pregnancy outcomes is highly heterogeneous, reflecting several factors, including reliance on small cross-sectional studies, non-uniform Lp(a) measurement across pregnancy, and isoform-sensitive assays.
Methods: Among n=16,415 Hispanic Community Health Study/Study of Latinos participants, we identified 508 women with a singleton live birth occurring >43 weeks after the baseline visit (2008–2011). Pre-pregnancy Lp(a) was measured at baseline using a latex-enhanced turbidimetric method (Roche). Five self-reported outcomes were examined: gestational diabetes mellitus (GDM, n=80), hypertensive disorders of pregnancy (HDP, n=55), preterm birth (PTB, n=55), intrauterine growth restriction (IUGR, n=37), and birthweight Z-score for all births (BWZ, n=483). An adverse pregnancy outcome (APO, n=179) was defined as presence of GDM, HDP, PTB, or IUGR. Survey-weighted and confounder-adjusted (age, kidney function, background group) logistic (GDM, HDP, PTB, IUGR, APO) or linear (BWZ) regression was used to examine four Lp(a) dose-response patterns: linear, curvilinear, quartile categorized, and moderately increased risk threshold (≥75 nmol/L).
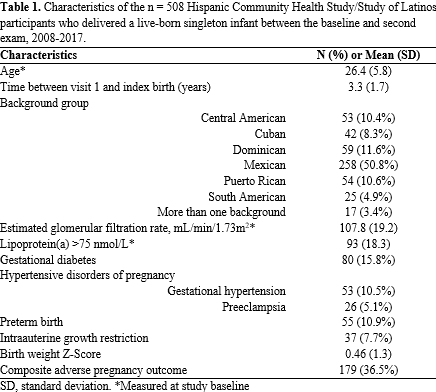
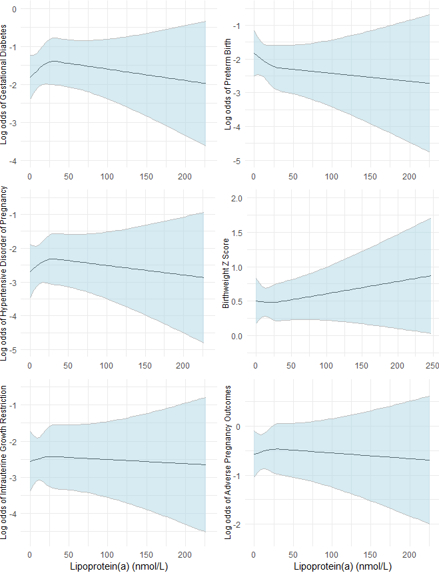
Results: Among women included, the mean age was 26.4 (SD=5.8), and almost half were of Mexican background. The distribution of pre-pregnancy Lp(a) was right skewed with a median of 16.9 nmol/L (IQR: 6.7 to 52.8 nmol/L). Lp(a) >75 nmol/L (n = 93, 18.3%) was associated with decreased odds of HDP (OR = 0.77, 95% CI = 0.31 – 1.92) and PTB (OR = 0.86, 95% CI = 0.32 – 2.32), although estimates were imprecise. The curvilinear model, though also imprecise, showed lower odds of GDM, HDP, and overall APO at both Lp(a) extremes, while higher Lp(a) was associated with lower odds of PTB and higher BWZ. All other associations tested were null without any discernible pattern.
Conclusions: Higher Lp(a) levels may reduce the odds of HDP and GDM, and lower Lp(a) levels may increase the odds of PTB, although results were not definitive. Future work with larger sample sizes is needed to better understand the physiological implications of Lp(a) for pregnancy.
Methods: Among n=16,415 Hispanic Community Health Study/Study of Latinos participants, we identified 508 women with a singleton live birth occurring >43 weeks after the baseline visit (2008–2011). Pre-pregnancy Lp(a) was measured at baseline using a latex-enhanced turbidimetric method (Roche). Five self-reported outcomes were examined: gestational diabetes mellitus (GDM, n=80), hypertensive disorders of pregnancy (HDP, n=55), preterm birth (PTB, n=55), intrauterine growth restriction (IUGR, n=37), and birthweight Z-score for all births (BWZ, n=483). An adverse pregnancy outcome (APO, n=179) was defined as presence of GDM, HDP, PTB, or IUGR. Survey-weighted and confounder-adjusted (age, kidney function, background group) logistic (GDM, HDP, PTB, IUGR, APO) or linear (BWZ) regression was used to examine four Lp(a) dose-response patterns: linear, curvilinear, quartile categorized, and moderately increased risk threshold (≥75 nmol/L).
Results: Among women included, the mean age was 26.4 (SD=5.8), and almost half were of Mexican background. The distribution of pre-pregnancy Lp(a) was right skewed with a median of 16.9 nmol/L (IQR: 6.7 to 52.8 nmol/L). Lp(a) >75 nmol/L (n = 93, 18.3%) was associated with decreased odds of HDP (OR = 0.77, 95% CI = 0.31 – 1.92) and PTB (OR = 0.86, 95% CI = 0.32 – 2.32), although estimates were imprecise. The curvilinear model, though also imprecise, showed lower odds of GDM, HDP, and overall APO at both Lp(a) extremes, while higher Lp(a) was associated with lower odds of PTB and higher BWZ. All other associations tested were null without any discernible pattern.
Conclusions: Higher Lp(a) levels may reduce the odds of HDP and GDM, and lower Lp(a) levels may increase the odds of PTB, although results were not definitive. Future work with larger sample sizes is needed to better understand the physiological implications of Lp(a) for pregnancy.
More abstracts on this topic:
Association of Preeclampsia with Long-Term Coronary Microvascular Dysfunction Utilizing Cardiac Stress Magnetic Resonance Imaging
Roy Rukmini, Rana Sarosh, Lang Roberto, Patel Amit, Shahul Sajid, Patel Hena, Wang Haonan, Huang Sherry, Minga Iva, Wang Shuo, O'hara Meaghan, Tang Maxine, Slivnick Jeremy, Polonsky Tamar
Advanced maternal age and association with major adverse cardiovascular events from NHANES from 1999 to 2018Mehta Adhya, Honigberg Michael, Kennedy Jamie, Spitz Jared, Sharma Garima, Agboola Olayinka, Satti Danish Iltaf, Harrington Colleen, Scott Nandita, Sarma Amy, Saad Antonio, Sullivan Scott, Epps Kelly