Final ID: TU115
Cardiovascular-Kidney-Metabolic Stage Three Prevalence in the Community: A Comparison of Different Criteria
Abstract Body: Background: The American Heart Association’s Cardiovascular-Kidney-Metabolic (CKM) Stages, introduced in 2023, highlight the progressive and interrelated nature of metabolic risk factors, chronic kidney disease (CKD), and cardiovascular disease (CVD). Stage 4 is defined by clinical CVD or CKD, while stage 3 represents subclinical disease or a high-risk profile. Increasingly, studies are investigating the epidemiology of CKM stages in the community. However, few have utilized all proposed stage 3 criteria, potentially leading to misclassification.
Methods: We compared CKM stage 3 classification using different criteria in Framingham Heart Study (FHS) participants. We classified participants as stage 4 if they had a history of coronary heart disease (CHD), heart failure (HF), stroke, peripheral artery disease (PAD), atrial fibrillation (AF), or CKD stage 4a/4b. From the remaining sample, we compared the prevalence of stage 3 CKM with the commonly used “epidemiologic criteria” (PREVENT CVD risk score ≥20% or very high-risk CKD) versus complete stage 3 criteria, which additionally include coronary artery calcium score (CAC) ≥100, elevated left ventricular (LV) mass, high cardiac biomarkers, or very-high risk CKD.
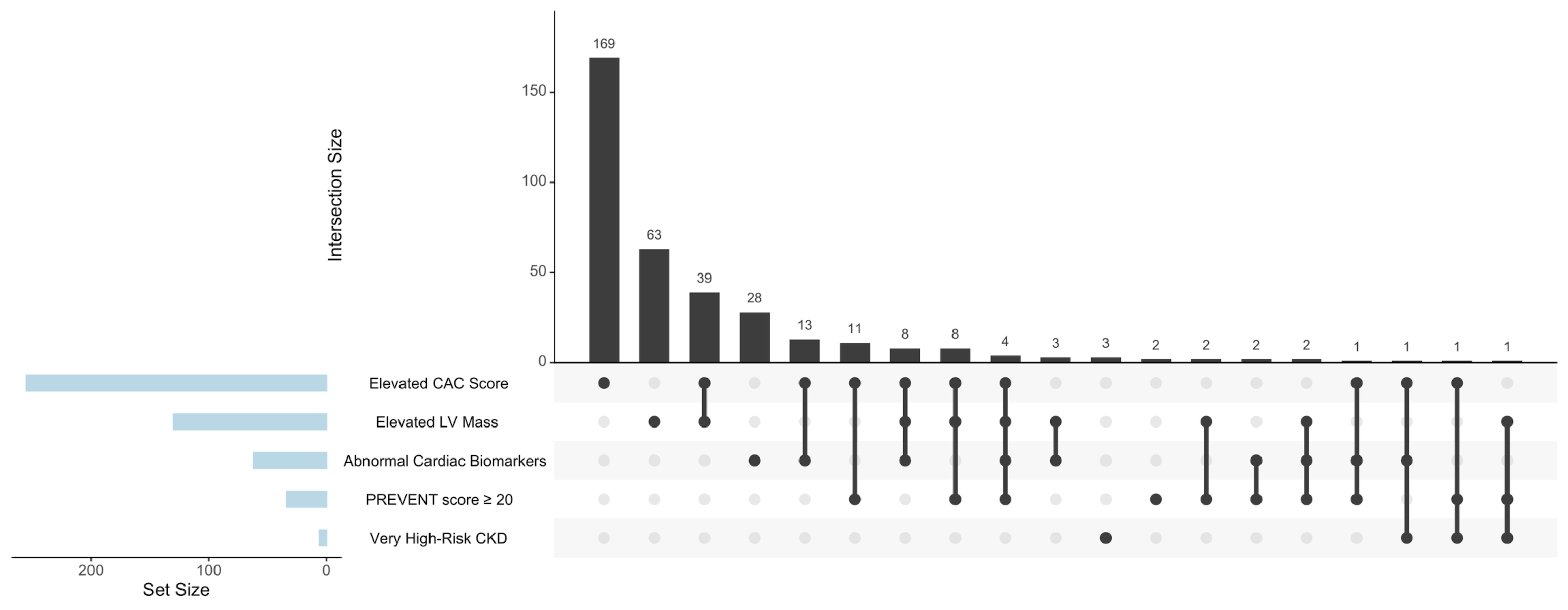
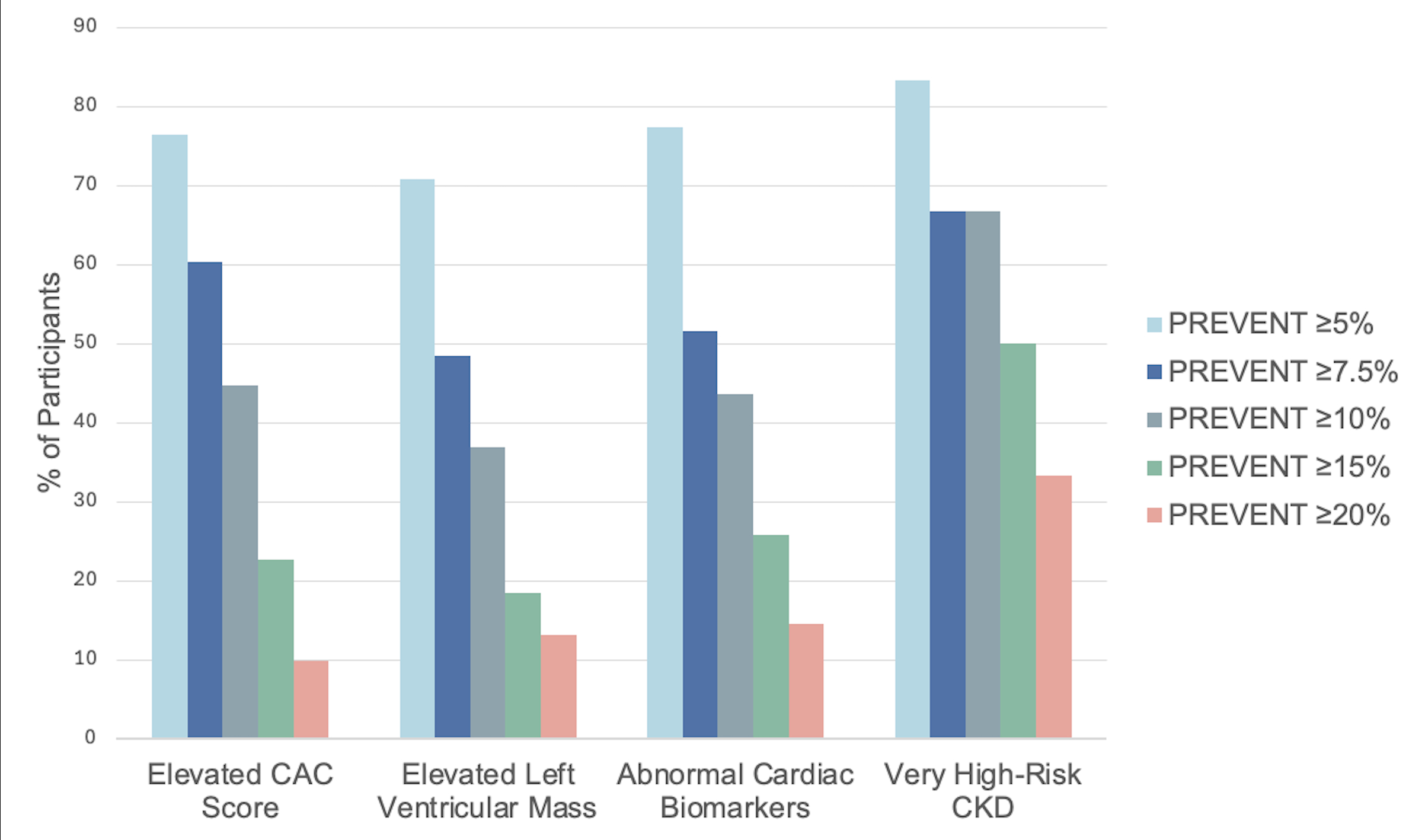
Results: Among 3424 participants (mean age 60±9 years, 53% female, with body mass index 28±5 kg/m2), 371 met criteria for CKM stage 4, including CHD (157), HF (40), stroke (87), PAD (107), AF (100), or CKD stage 4a/4b (17). Of the remaining 3053 participants, 1160 (38%) were classified as stage 3, using the complete criteria, compared with 304 (10%) using the “epidemiologic criteria.” In a subsample of 780 individuals with complete subclinical data, 361 (46%) met complete stage 3 criteria, compared with only 38 (5%) using the epidemiologic criteria. Most individuals with elevated CAC (90%), LV mass (87%), cardiac biomarkers (85%), or high-risk CKD (67%) do not have PREVENT scores of ≥20% and most have a single abnormal subclinical measure (Figure 1A). We then explored proportions of individuals identified by lower PREVENT thresholds (Figure 1B).
Conclusions: Categorization of stage 3 CKM in the absence of comprehensive subclinical disease domains is challenging and leads to misclassifying individuals’ true risk. Future studies should evaluate whether lowering the PREVENT score threshold would improve the classification of subclinical risk for stage 3 CKM in the absence of comprehensive subclinical CVD phenotypes.
Methods: We compared CKM stage 3 classification using different criteria in Framingham Heart Study (FHS) participants. We classified participants as stage 4 if they had a history of coronary heart disease (CHD), heart failure (HF), stroke, peripheral artery disease (PAD), atrial fibrillation (AF), or CKD stage 4a/4b. From the remaining sample, we compared the prevalence of stage 3 CKM with the commonly used “epidemiologic criteria” (PREVENT CVD risk score ≥20% or very high-risk CKD) versus complete stage 3 criteria, which additionally include coronary artery calcium score (CAC) ≥100, elevated left ventricular (LV) mass, high cardiac biomarkers, or very-high risk CKD.
Results: Among 3424 participants (mean age 60±9 years, 53% female, with body mass index 28±5 kg/m2), 371 met criteria for CKM stage 4, including CHD (157), HF (40), stroke (87), PAD (107), AF (100), or CKD stage 4a/4b (17). Of the remaining 3053 participants, 1160 (38%) were classified as stage 3, using the complete criteria, compared with 304 (10%) using the “epidemiologic criteria.” In a subsample of 780 individuals with complete subclinical data, 361 (46%) met complete stage 3 criteria, compared with only 38 (5%) using the epidemiologic criteria. Most individuals with elevated CAC (90%), LV mass (87%), cardiac biomarkers (85%), or high-risk CKD (67%) do not have PREVENT scores of ≥20% and most have a single abnormal subclinical measure (Figure 1A). We then explored proportions of individuals identified by lower PREVENT thresholds (Figure 1B).
Conclusions: Categorization of stage 3 CKM in the absence of comprehensive subclinical disease domains is challenging and leads to misclassifying individuals’ true risk. Future studies should evaluate whether lowering the PREVENT score threshold would improve the classification of subclinical risk for stage 3 CKM in the absence of comprehensive subclinical CVD phenotypes.
More abstracts on this topic:
A Community-Based Intervention to Improve Cardiovascular Health Understanding in the Dallas-Fort Worth South Asian Community
Deo Parminder, Rohatgi Anand, Sharma Parul, Sathyamoorthy Mohanakrishnan
A Scoping Review Exploring Cardiovascular Risk and Health Metrics and Cancer PredictionKim Ji-eun, Henriquez Santos Gretell, Kumar Sant, Livinski Alicia, Vo Jacqueline, Joo Jungnam, Shearer Joe, Hashemian Maryam, Roger Veronique