Final ID: 34
Quantifying Pulse Arrival Time Changes Across Sleep-Disordered Breathing Events: Insights from the MESA Sleep Study
Abstract Body: Introduction: Pulse arrival time (PAT), the interval between cardiac electrical activity and peripheral pulse detection, reflects beat-to-beat vascular reactivity and autonomic tone. Sleep-related respiratory events, including apneas, hypopneas, and oxygen desaturations, may transiently alter PAT via changes in intrathoracic pressure and sympathetic activation. However, relationships between event type, sleep-apnea status, and PAT remain unclear.
Hypothesis: We hypothesized that PAT decreases during respiratory disturbances and that these changes differ across respiratory event types.
Methods: We analyzed 203 participants in the MESA Sleep Study, each with respiratory events scored by technicians. Sleep-apnea status was defined by the apnea–hypopnea index (AHI). Per-patient mean PAT was compared between respiratory-event and non-event segments using the Wilcoxon signed-rank test. A mixed-effects model evaluated PAT across event types, using non-event segments as reference. Subgroup comparisons by sex, BMI, race, and sleep-apnea status used nonparametric tests.
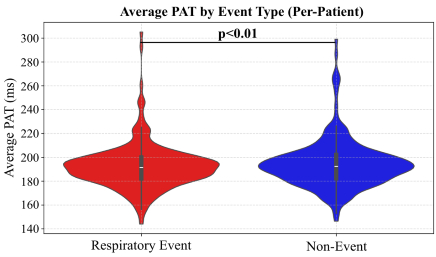
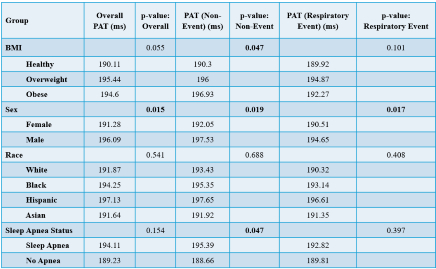
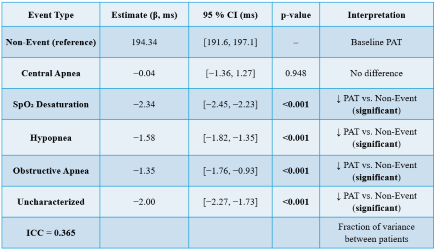
Results: Average PAT was significantly lower during respiratory-event versus non-event segments (p<0.01). In mixed-effects modeling, PAT was reduced during SpO2 desaturations (−2.34 ms), hypopneas (−1.58 ms), obstructive apneas (−1.35 ms), and other uncharacterized sleep disturbance events (−2.00 ms), all p<0.001 relative to non-event segments (194.3 ms). Between-patient variance accounted for 36.5% of total variability (ICC=0.365). PAT was shorter among males (191.3 vs 196.1 ms, p=0.015) and trended lower with higher BMI (p=0.055). During non-event periods, shorter PAT persisted among males (p=0.019), those with sleep apnea (195.4 vs 188.7 ms, p=0.047), and higher BMI (p=0.047). PAT during respiratory events showed minimal group differences except for sex (p=0.017), suggesting baseline rather than event-specific variation.
Conclusions: PAT decreases during respiratory disturbances, particularly during desaturation and obstructive events, consistent with transient autonomic and vascular responses. Sex, BMI, and sleep-apnea status modify baseline PAT but have weaker effects during respiratory events. The stronger association of sleep-apnea status with PAT during non-respiratory periods likely reflects chronic vascular remodeling and autonomic dysregulation in those with higher AHI. These findings support PAT as a physiologic biomarker of sleep-disordered-breathing severity and cardiovascular stress.
Hypothesis: We hypothesized that PAT decreases during respiratory disturbances and that these changes differ across respiratory event types.
Methods: We analyzed 203 participants in the MESA Sleep Study, each with respiratory events scored by technicians. Sleep-apnea status was defined by the apnea–hypopnea index (AHI). Per-patient mean PAT was compared between respiratory-event and non-event segments using the Wilcoxon signed-rank test. A mixed-effects model evaluated PAT across event types, using non-event segments as reference. Subgroup comparisons by sex, BMI, race, and sleep-apnea status used nonparametric tests.
Results: Average PAT was significantly lower during respiratory-event versus non-event segments (p<0.01). In mixed-effects modeling, PAT was reduced during SpO2 desaturations (−2.34 ms), hypopneas (−1.58 ms), obstructive apneas (−1.35 ms), and other uncharacterized sleep disturbance events (−2.00 ms), all p<0.001 relative to non-event segments (194.3 ms). Between-patient variance accounted for 36.5% of total variability (ICC=0.365). PAT was shorter among males (191.3 vs 196.1 ms, p=0.015) and trended lower with higher BMI (p=0.055). During non-event periods, shorter PAT persisted among males (p=0.019), those with sleep apnea (195.4 vs 188.7 ms, p=0.047), and higher BMI (p=0.047). PAT during respiratory events showed minimal group differences except for sex (p=0.017), suggesting baseline rather than event-specific variation.
Conclusions: PAT decreases during respiratory disturbances, particularly during desaturation and obstructive events, consistent with transient autonomic and vascular responses. Sex, BMI, and sleep-apnea status modify baseline PAT but have weaker effects during respiratory events. The stronger association of sleep-apnea status with PAT during non-respiratory periods likely reflects chronic vascular remodeling and autonomic dysregulation in those with higher AHI. These findings support PAT as a physiologic biomarker of sleep-disordered-breathing severity and cardiovascular stress.
More abstracts on this topic:
A Focus for Improvement - Factors for Lab Adherence in a Pediatric Preventive Cardiology Program
Holsinger Hunter, Porterfield Ronna, Taylor Makenna, Dresbach Bethany, Seipel Brittany, Igwe Chukwuemeka, Alvarado Chance, Tran Andrew
3-Minute Heart Health App: A Feasibility StudyAbdulkarim Iya, Metzger Joseph, Stovitz Steven, Van't Hof Jeremy