Final ID: MP1371
Elevated Peri-coronary Adipose Tissue attenuation association with Coronary Plaque Progression in Type 2 Diabetes Mellitus Patients
Abstract Body (Do not enter title and authors here): Introduction:
Peri-coronary adipose tissue (PCAT) attenuation, quantified by Coronary Computed Tomography Angiography (CCTA), is a validated non-invasive marker for assessing coronary inflammation. It has been predictive of adverse outcomes including myocardial infarction and cardiovascular death. This is pertinent especially for type 2 diabetic patients given increased systemic inflammation and increased risk of coronary artery disease. Given that increased inflammation has been associated with coronary atherogenesis, our aim was to investigate whether progression in PCAT attenuation was associated with coronary plaque burden progression.
Hypothesis:
We hypothesize that elevated PCAT attenuation, suggestive of increased vascular inflammation, is associated with increased coronary plaque burden and progression, in a high-risk cohort of patients with type 2 diabetes mellitus enrolled in STOP (Semaglutide Treatment Effect On Coronary Atherosclerosis Progression In Diabetes) trial.
Methods:
We performed a retrospective analysis of participants with type 2 diabetes mellitus from the STOP trial who underwent serial CCTA at baseline visit and 12-month follow up. PCAT attenuation (HU) was measured around the proximal right coronary artery from the 10-50th mm from the ostium, the current standardized method for PCAT analysis. Compositional plaque changes were measured as change in percent atheroma volume (PAV%) comparing baseline to 12-month follow up through analysis with QAngio and Medis. Spearman correlation and multivariable linear regression models assessed the association between PCAT and change in PAV. In addition, multivariable models adjusted for traditional cardiovascular risk factors.
Results:
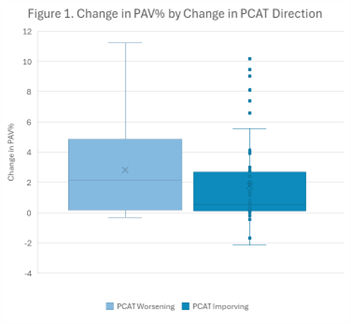
We analyzed 98 participants (mean age 57.1±8.2 years, 62% male). Patients with an increase in PCAT attenuation (measures as higher HU) showed an increase in PAV progression (r=0.259, p=0.01). Changes in PCAT attenuation correlated with changes in the burden of total plaque (r=0.22, p=0.029) and calcified plaque (r=0.219, p=0.03), but not with other morphologies.
Conclusion:
In this high-risk cohort of patients with diabetes and extensive atherosclerosis, we found that an increase in PCAT was associated with rapid progression of total plaque volumes. These findings support the role of vascular inflammation in the progression of atherosclerosis and the need to characterize vascular inflammation, as potential therapeutic targets.
Peri-coronary adipose tissue (PCAT) attenuation, quantified by Coronary Computed Tomography Angiography (CCTA), is a validated non-invasive marker for assessing coronary inflammation. It has been predictive of adverse outcomes including myocardial infarction and cardiovascular death. This is pertinent especially for type 2 diabetic patients given increased systemic inflammation and increased risk of coronary artery disease. Given that increased inflammation has been associated with coronary atherogenesis, our aim was to investigate whether progression in PCAT attenuation was associated with coronary plaque burden progression.
Hypothesis:
We hypothesize that elevated PCAT attenuation, suggestive of increased vascular inflammation, is associated with increased coronary plaque burden and progression, in a high-risk cohort of patients with type 2 diabetes mellitus enrolled in STOP (Semaglutide Treatment Effect On Coronary Atherosclerosis Progression In Diabetes) trial.
Methods:
We performed a retrospective analysis of participants with type 2 diabetes mellitus from the STOP trial who underwent serial CCTA at baseline visit and 12-month follow up. PCAT attenuation (HU) was measured around the proximal right coronary artery from the 10-50th mm from the ostium, the current standardized method for PCAT analysis. Compositional plaque changes were measured as change in percent atheroma volume (PAV%) comparing baseline to 12-month follow up through analysis with QAngio and Medis. Spearman correlation and multivariable linear regression models assessed the association between PCAT and change in PAV. In addition, multivariable models adjusted for traditional cardiovascular risk factors.
Results:
We analyzed 98 participants (mean age 57.1±8.2 years, 62% male). Patients with an increase in PCAT attenuation (measures as higher HU) showed an increase in PAV progression (r=0.259, p=0.01). Changes in PCAT attenuation correlated with changes in the burden of total plaque (r=0.22, p=0.029) and calcified plaque (r=0.219, p=0.03), but not with other morphologies.
Conclusion:
In this high-risk cohort of patients with diabetes and extensive atherosclerosis, we found that an increase in PCAT was associated with rapid progression of total plaque volumes. These findings support the role of vascular inflammation in the progression of atherosclerosis and the need to characterize vascular inflammation, as potential therapeutic targets.
More abstracts on this topic:
A Novel RNA Interference Agent RN0191 Lowering Proprotein Convertase Subtilisin/Kexin Type 9, Low-density Lipoprotein Cholesterol and Other Lipid Biomarkers in Healthy Volunteers with Elevated LDL Cholesterol: A Randomized, Single-blind, Placebo-controlled, Phase 1 Trial
Wang Fangfang, Li Haiyan, Zeng Jie, Shi Yibin, Li Hongmei
A Non-odorant Olfactory Receptor Ligand Depolymerizes the Platelet Actin Cytoskeleton to Prevent ThrombosisAggarwal Anu, Godwin Matthew, Ali Mariya, Jennings Courtney, Rajasekar Bhairavi, Scalise Alliefair, Stauffer Shaun, Mccrae Keith, Mcintyre Thomas, Cameron Scott, Wang Nancy, Josyula Vara Prasad, Yang Moua, Young Shim, Kennedy Quinn, Samuel Reina, Sangwan Naseer, Guntupalli Suman