Final ID: MP2542
Impact of Lipoprotein(a) on Aortic Valve Replacement in Chinese Patients with Mild-to-Moderate Calcific Aortic Valve Stenosis
Abstract Body (Do not enter title and authors here): Background: Lipoprotein(a) [Lp(a)] is an independent risk factor for calcific aortic valve stenosis (CAVS), but its association with aortic valve replacement (AVR) risk in the Chinese population remains unclear. This study aimed to evaluate the predictive value of Lp(a) levels for clinical outcomes in patients with mild-to-moderate aortic stenosis (AS).
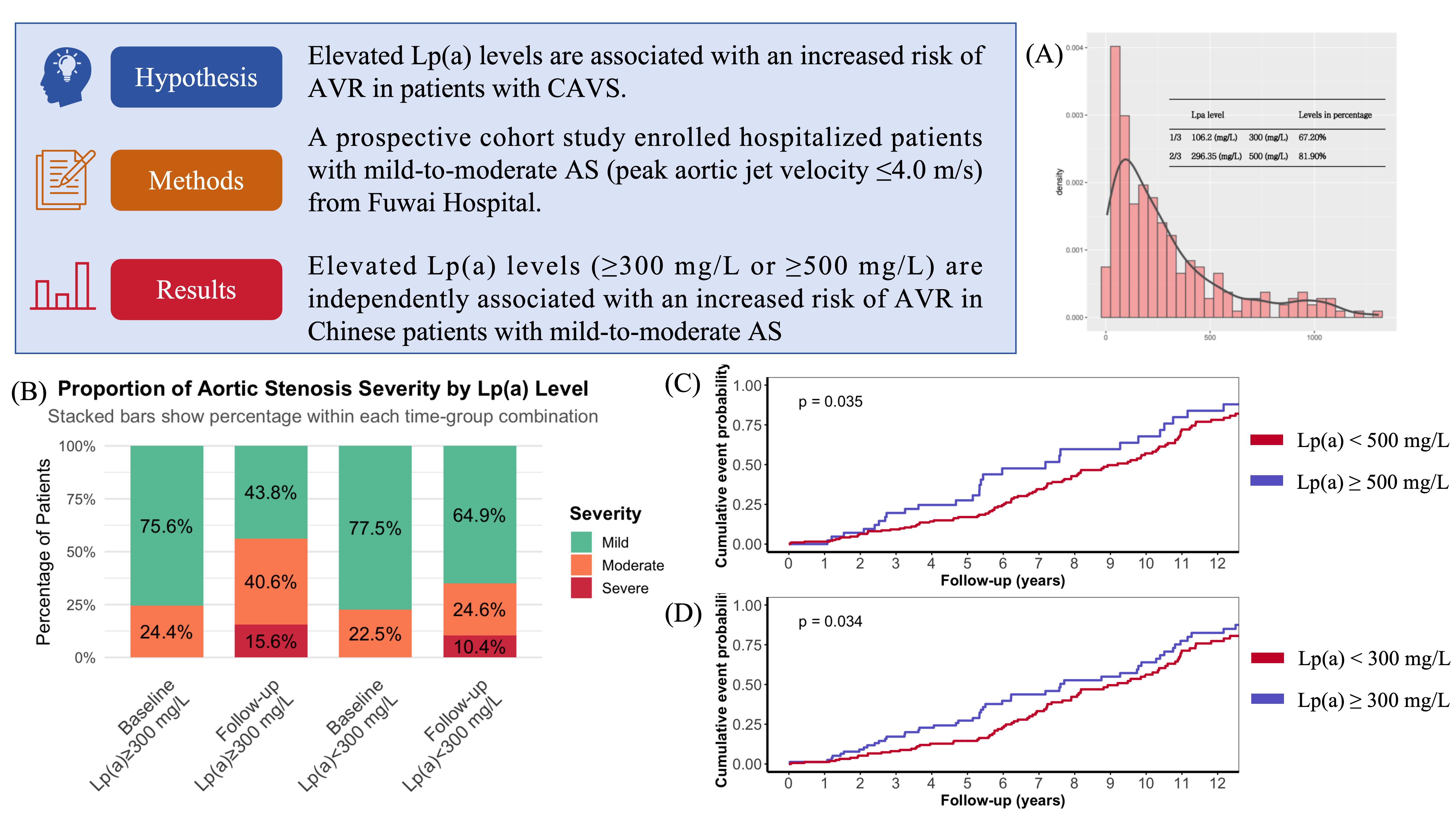
Hypothesis: Elevated Lp(a) levels are associated with an increased risk of AVR in patients with CAVS.
Methods: This prospective study enrolled hospitalized patients with mild-to-moderate CAVS (peak aortic jet velocity ≤4.0 m/s) from Fuwai Hospital between June 2013 and May 2014. Patients who had undergone baseline AVR or had severe comorbidities were excluded. Participants were stratified by baseline Lp(a) levels (cutoffs: 300 mg/L and 500 mg/L). The association between Lp(a) and the primary endpoint (AVR) was assessed using Kaplan-Meier survival analysis and multivariable Cox regression, adjusting for age, sex, hypertension, diabetes, and hyperlipidemia.
Results: Among 238 patients with complete follow-up (median follow-up: 6.2 years), the mean age of the patients was 66.0 ± 13.0 years, and 104 (43.7%) were females. The median baseline Lp(a) level was 197.2 mg/L (IQR: 78.8–398.5 mg/L). The high Lp(a) groups (≥300 mg/L or ≥500 mg/L) had a higher prevalence of hyperlipidemia (all P <0.01). Multivariable analysis revealed that patients with Lp(a) ≥500 mg/L had a 68% higher AVR risk compared to those with Lp(a) <500 mg/L (adjusted HR=1.688, 95% CI: 1.108–2.573, P=0.0149), while those with Lp(a) ≥300 mg/L had a 61% increased risk (adjusted HR=1.616, 95% CI: 1.135–2.300, P=0.0077). Additionally, the Lp(a) ≥300 mg/L group had a higher progression rate to moderate-to-severe AS (56.2% vs. 35%, P <0.05).
Conclusion: Elevated Lp(a) levels (≥300 mg/L or ≥500 mg/L) are independently associated with an increased risk of AVR in Chinese patients with mild-to-moderate AS, suggesting its potential role in risk stratification and prognostic assessment.
Hypothesis: Elevated Lp(a) levels are associated with an increased risk of AVR in patients with CAVS.
Methods: This prospective study enrolled hospitalized patients with mild-to-moderate CAVS (peak aortic jet velocity ≤4.0 m/s) from Fuwai Hospital between June 2013 and May 2014. Patients who had undergone baseline AVR or had severe comorbidities were excluded. Participants were stratified by baseline Lp(a) levels (cutoffs: 300 mg/L and 500 mg/L). The association between Lp(a) and the primary endpoint (AVR) was assessed using Kaplan-Meier survival analysis and multivariable Cox regression, adjusting for age, sex, hypertension, diabetes, and hyperlipidemia.
Results: Among 238 patients with complete follow-up (median follow-up: 6.2 years), the mean age of the patients was 66.0 ± 13.0 years, and 104 (43.7%) were females. The median baseline Lp(a) level was 197.2 mg/L (IQR: 78.8–398.5 mg/L). The high Lp(a) groups (≥300 mg/L or ≥500 mg/L) had a higher prevalence of hyperlipidemia (all P <0.01). Multivariable analysis revealed that patients with Lp(a) ≥500 mg/L had a 68% higher AVR risk compared to those with Lp(a) <500 mg/L (adjusted HR=1.688, 95% CI: 1.108–2.573, P=0.0149), while those with Lp(a) ≥300 mg/L had a 61% increased risk (adjusted HR=1.616, 95% CI: 1.135–2.300, P=0.0077). Additionally, the Lp(a) ≥300 mg/L group had a higher progression rate to moderate-to-severe AS (56.2% vs. 35%, P <0.05).
Conclusion: Elevated Lp(a) levels (≥300 mg/L or ≥500 mg/L) are independently associated with an increased risk of AVR in Chinese patients with mild-to-moderate AS, suggesting its potential role in risk stratification and prognostic assessment.
More abstracts on this topic:
A Remedy for the Heart and the Hemoglobin: Improvement in Anemia Post Transcatheter Aortic Valve Replacement
Matta Raghav, Roy Aanya, Hammad Bayan, Draffen Arvind, Natsheh Zachary, Tiu Daniel, Tiu David, Salem Edward, Balami Jesse, Kalagara Swetha, Gupta Neil, Uraizee Omar, Sahgal Savina, Mishra Atreya, Ene Adriana, Hattab Aleyah, Arora Aarushi, Sufyaan Humam, Dau Trang, Silberstein Jonathan, Yu Julia, Torres Kayla, Seshadri Suhas, Navarro Laura, Singam Manisha, Ismail Mariam, Rana Riya, Habeel Samer, Liu Simon, Chaganti Srinidhi, Gurbuxani Vidur, Dwyer Kaluzna Stephanie, Groo Vicki, Carlson Andrew, Shroff Adhir, Bhayani Siddharth, Khan Azmer, Bhattaram Rohan, Zhang Runze, Shah Pal
A Randomized Phase 2 Trial of Muvalaplin: An Oral Disrupter of the Assembly of Lipoprotein(a) ParticlesNicholls Stephen, Ni Wei, Rhodes Grace, Nissen Steven, Navar Ann Marie, Michael Laura, Krege John