Final ID: MP637
Classifying Chest Pain as Typical vs. Atypical Fails to Discriminate Acute Coronary Occlusion and Does Not Predict Mortality
Abstract Body (Do not enter title and authors here): Background: Current US guidelines discourage classifying chest pain as ‘typical’ or ‘atypical,’ yet this dichotomous approach remains widespread in clinical practice. We aimed to determine if this common classification has meaningful diagnostic or prognostic value for identifying acute coronary occlusion (ACO) in the emergency department (ED).
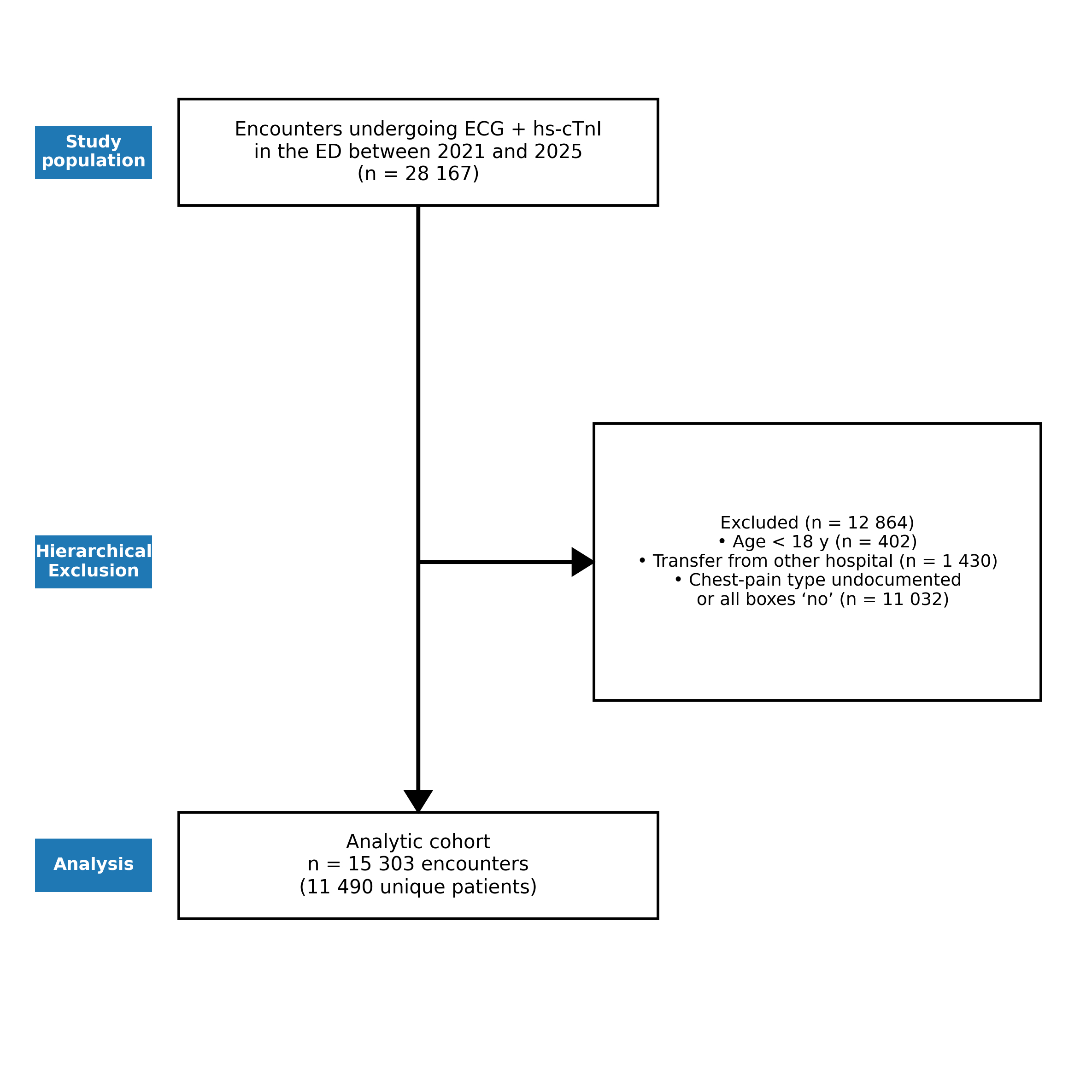
Methods: In a large, retrospective cohort of 15,303 ED encounters for chest pain, we evaluated the diagnostic performance of classifying pain as 'typical' (definite or probable angina) versus 'atypical'. Our primary outcome was ACO, defined by emergent catheterization lab activation or a peak high-sensitivity troponin I level ≥5000 ng/L. We calculated sensitivity, specificity, and likelihood ratios (LRs). Multivariable logistic regression was used to assess the association between pain type and in-hospital mortality.
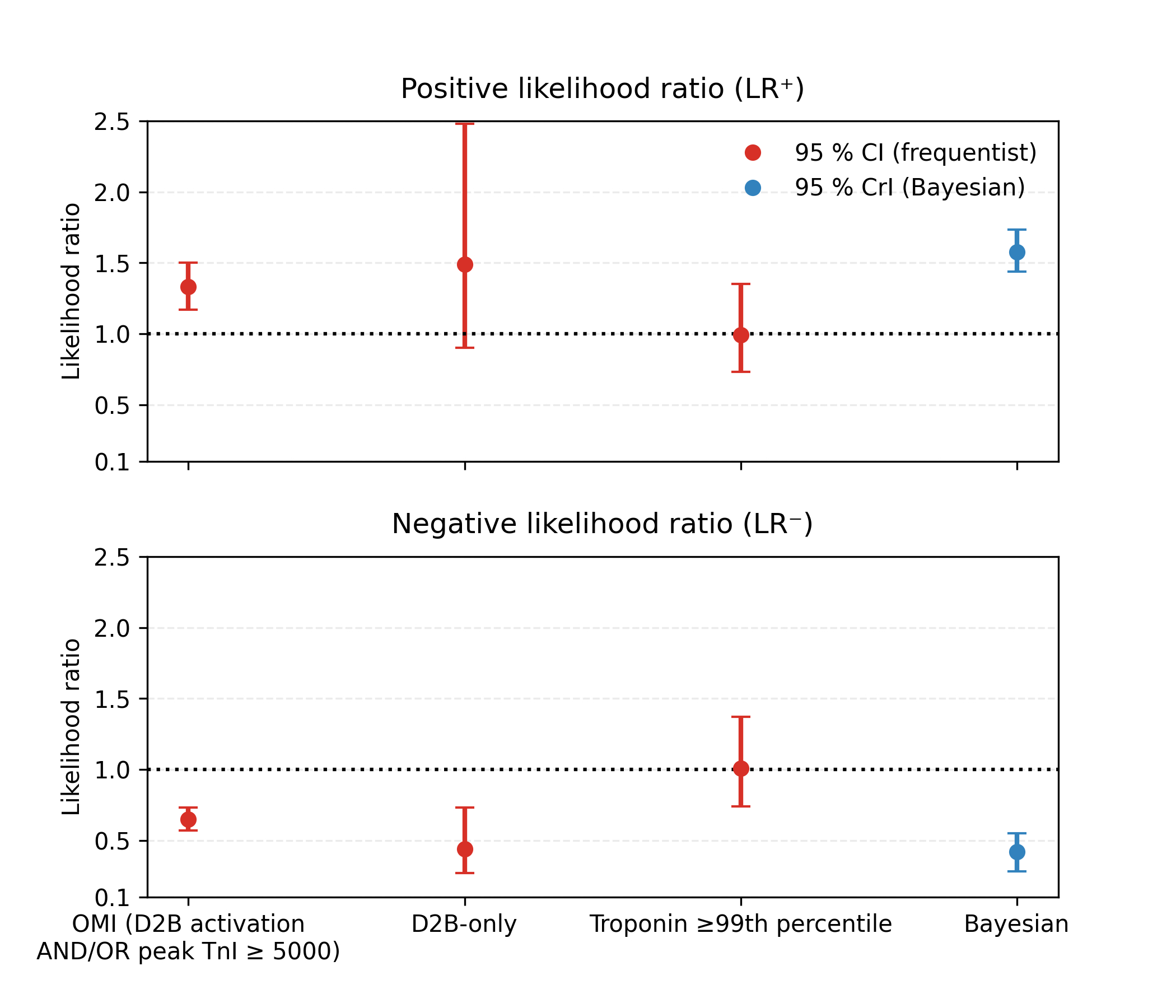
Results: Classifying pain as 'typical' demonstrated poor diagnostic utility for ACO, with a sensitivity of 0.69 (95% CI 0.66–0.71) and a specificity of 0.48 (95% CI 0.47–0.49). The resulting likelihood ratios were unhelpful for altering clinical probability (LR+ 1.33; LR- 0.65). These findings remained poor even after analysis with a Bayesian latent-class model designed to correct for an imperfect reference standard (posterior median LR+ 1.57; LR- 0.42). While associated with higher mortality in univariate analysis, 'typical' pain did not independently predict in-hospital death after multivariable adjustment (adjusted OR 1.28; 95% CI 0.91–1.81).
Conclusion: In this large, contemporary ED cohort, the common practice of labeling chest pain as 'typical' versus 'atypical' offers negligible value for either ruling in or ruling out ACO and fails to independently predict short-term mortality. This evidence strongly supports guideline recommendations to abandon these overly simplistic, dichotomous labels. Clinical evaluation should instead prioritize granular symptom descriptors, rapid biomarker testing, and validated risk assessment tools.
Methods: In a large, retrospective cohort of 15,303 ED encounters for chest pain, we evaluated the diagnostic performance of classifying pain as 'typical' (definite or probable angina) versus 'atypical'. Our primary outcome was ACO, defined by emergent catheterization lab activation or a peak high-sensitivity troponin I level ≥5000 ng/L. We calculated sensitivity, specificity, and likelihood ratios (LRs). Multivariable logistic regression was used to assess the association between pain type and in-hospital mortality.
Results: Classifying pain as 'typical' demonstrated poor diagnostic utility for ACO, with a sensitivity of 0.69 (95% CI 0.66–0.71) and a specificity of 0.48 (95% CI 0.47–0.49). The resulting likelihood ratios were unhelpful for altering clinical probability (LR+ 1.33; LR- 0.65). These findings remained poor even after analysis with a Bayesian latent-class model designed to correct for an imperfect reference standard (posterior median LR+ 1.57; LR- 0.42). While associated with higher mortality in univariate analysis, 'typical' pain did not independently predict in-hospital death after multivariable adjustment (adjusted OR 1.28; 95% CI 0.91–1.81).
Conclusion: In this large, contemporary ED cohort, the common practice of labeling chest pain as 'typical' versus 'atypical' offers negligible value for either ruling in or ruling out ACO and fails to independently predict short-term mortality. This evidence strongly supports guideline recommendations to abandon these overly simplistic, dichotomous labels. Clinical evaluation should instead prioritize granular symptom descriptors, rapid biomarker testing, and validated risk assessment tools.
More abstracts on this topic:
A Personal Risk Assessment Device in Patients with Chest Pain
Shvilkin Alexei, Zlatic Natasa, Atanasoski Vladimir, Grujovic Zdolsek Sanja, Popovic Maneski Lana, Miletic Marjan, Vukcevic Vladan
A Machine Learning-Based Novel Risk Score Model for Spontaneous Coronary Artery DissectionAgrawal Ankit, Arockiam Aro Daniela, Bhagat Umesh, Haroun Elio, Majid Muhammad, Wang Tom Kai Ming