Final ID: MDP464
Health System Variability in Lipid Management for Patients with Atherosclerotic Cardiovascular Disease: An Analysis from Cv-MOBIUS
Methods: A cross sectional analysis was performed where lipid levels and lipid lowering therapies (LLT) were assessed using electronic health record data in patients with a previous diagnosis of ASCVD. The data was obtained across 14 US healthcare systems between 1/1/2021-12/31/2022. Proportions of patients with an active prescription of any statin, high intensity statin, ezetimibe, PCSK9i, and combination therapy (two or more agents) within 395 days of the most recent LDL-C value (index date) was evaluated overall and by participating site. Additionally, the proportion of patients with an LDL-C <70 mg/dL at the index date was also assessed.
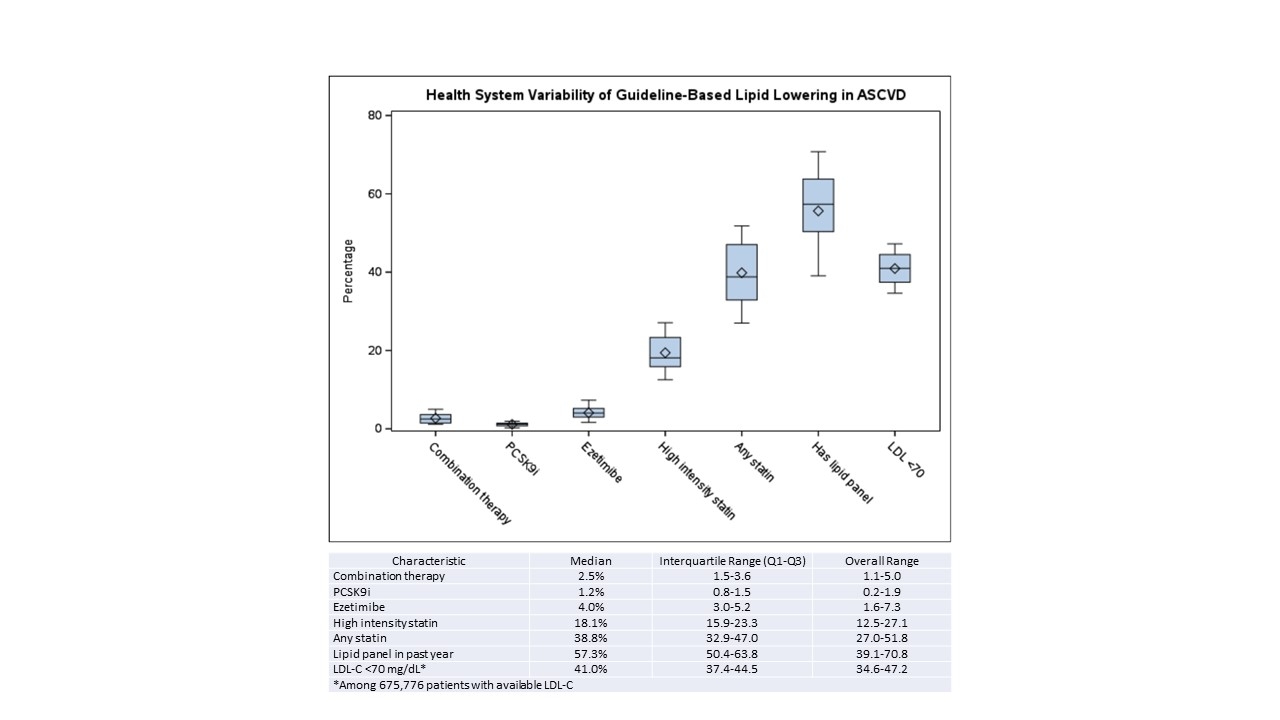
Results: Across 14 health systems, 1,118,623 patients with ASCVD were identified (median 61,840 per health system, range 8,161-182,315). Overall, 675,776 (60.4%) had an LDL-C level in the past year (range 39.1% - 70.8%). Of those with a lipid level, achievement of LDL-C <70 mg/dL ranged from 34.6-47.2%. In total, 42.6% were on any statin, 20.1% were on a high intensity statin, 4.3% on ezetimibe, and 1.2% on a PCSK9i. Only 2.9% were on combination therapy of a statin with ezetimibe or a PCSK9i. Variability was seen across health systems in utilization of each of these therapies, however even in the highest performing health systems, LLT uptake and achievement of LDL-C < 70mg/dL remained low (Figure).
Conclusion: Variability in utilization of LLT in ASCVD patients between health systems suggests that system-level factors may impact achieving guideline-based LDL-C goals. Despite the variability, the highest proportion of patients achieving an LDL-C <70mg/dL remained under 50% indicating the need for aggressive implementation efforts.
- Shah, Nishant ( Duke University Medical Center , Durham , North Carolina , United States )
- Shrader, Peter ( Duke University Medical Center , Durham , North Carolina , United States )
- Shoji, Satoshi ( Keio University School of Medicine , Shinjyuku, Tokyo , Japan )
- Martin, Seth ( Johns Hopkins School of Medicine , Baltimore , Maryland , United States )
- Fernandez, Soledad ( The Ohio State University , Columbus , Ohio , United States )
- Chamberlain, Alanna ( MAYO CLINIC , Rochester , Minnesota , United States )
- Arnold, Jonathan ( University of Pittsburgh, UPMC , McKeesport , Pennsylvania , United States )
- Shapiro, Michael ( Wake Forest Univ School of Medicine , Winston Salem , North Carolina , United States )
- Effron, Mark ( OCHSNER MEDICAL CENTER , New Orleans , Louisiana , United States )
- Chrischilles, Elizabeth ( University of Iowa , Iowa City , Iowa , United States )
- Allred, Clint ( St Luke's Health System , Meridian , Idaho , United States )
- Priest, Elisa ( Baylor Scott & White Research Institute , Dallas , Texas , United States )
- Syed, Mahanazuddin ( UTHSCSA , San Antonio , Texas , United States )
- Kirchner, H Lester ( Geisinger , Danville , Pennsylvania , United States )
- Leja, Monika ( University Of Michigan , Ann Arbor , Michigan , United States )
- Ahmad, Zahid ( UT SOUTHWESTERN MEDICAL CENTER , Dallas , Texas , United States )
- Kalich, Bethany ( Amgen , San Antonio , Texas , United States )
- Dhalwani, Nafeesa ( Amgen Ltd. , Uxbridge , United Kingdom )
- Jones, Laney ( Amgen , San Antonio , Texas , United States )
- Wojcik, Cezary ( AMGEN , Portland , Oregon , United States )
- Peterson, Eric ( UT Southwestern Medical Center , Dallas , Texas , United States )
- Navar, Ann Marie ( UT Southwestern Medical Center , Dallas , Texas , United States )
Meeting Info:
Session Info:
Lipids and Management - A Deep Dive
Saturday, 11/16/2024 , 11:10AM - 12:35PM
Moderated Digital Poster Session
More abstracts on this topic:
Reitan Christian, Watanabe Alexandre, Bash Lori, Galvain Thibaut, Arnet Urs, Jernberg Tomas
3-Minute Heart Health App: A Feasibility StudyAbdulkarim Iya, Metzger Joseph, Stovitz Steven, Van't Hof Jeremy
More abstracts from these authors:
Shoji Satoshi, Jones Laney, Peterson Eric, Navar Ann Marie, Shah Nishant, Shrader Peter, Freeman Nikki, Bittner Vera, Wilcox Tanya, Amanda C Doran, Wojcik Cezary, Jin Ran
Treatment Implications of LDL-Cholesterol and Apolipoprotein B Discordance: Insights from the Very Large Database of Lipids (VLDbL) and the National Health and Examination Survey (NHANES)Peng Allison, Blumenthal Roger, Martin Seth, Zahid Sohail, Gianos Eugenia, Shapiro Michael, Navar Ann Marie, Marvel Francoise, Rodriguez Fatima, Soffer Daniel, Morris Pamela