Final ID: Su1082
Clinical Outcomes Of SGLT2 Inhibitors In Patients Hospitalized With Acute Heart Failure: A Meta-analysis Of Randomized Control Trials
Abstract Body (Do not enter title and authors here):
Introduction:
Acute heart failure (AHF) presents challenges due to its poor prognosis and limited therapeutic options compared to chronic heart failure (CHF). The potential benefits of SGLT2 inhibitors in AHF patients are being explored, yet systematic evaluation is lacking. Our meta-analysis aims to bridge this gap by comparing the efficacy and safety of SGLT2 inhibitors versus placebo in AHF patients.
Research question:
Clinical Outcomes Of SGLT2 Inhibitors In Patients Hospitalized With Acute Heart Failure
Methods:
We searched Medline, Embase, and Cochrane databases for randomized controlled trials involving adult patients hospitalized with AHF, who received SGLT2 inhibitors. Our primary outcomes were all-cause mortality, heart failure events, and readmissions. The secondary outcomes were change in KCCQ-TSS (Kansas City Cardiomyopathy Questionnaire), weight, length of stay and NT-proBNP levels. Safety outcomes included hypotension, hypoglycemia, UTI, DKA, and acute renal failure. We used Review Manager 5.4 for statistical analysis, employing standardized mean difference (SMD) and risk ratio (RR) with 95% confidence intervals (CI).
Results:
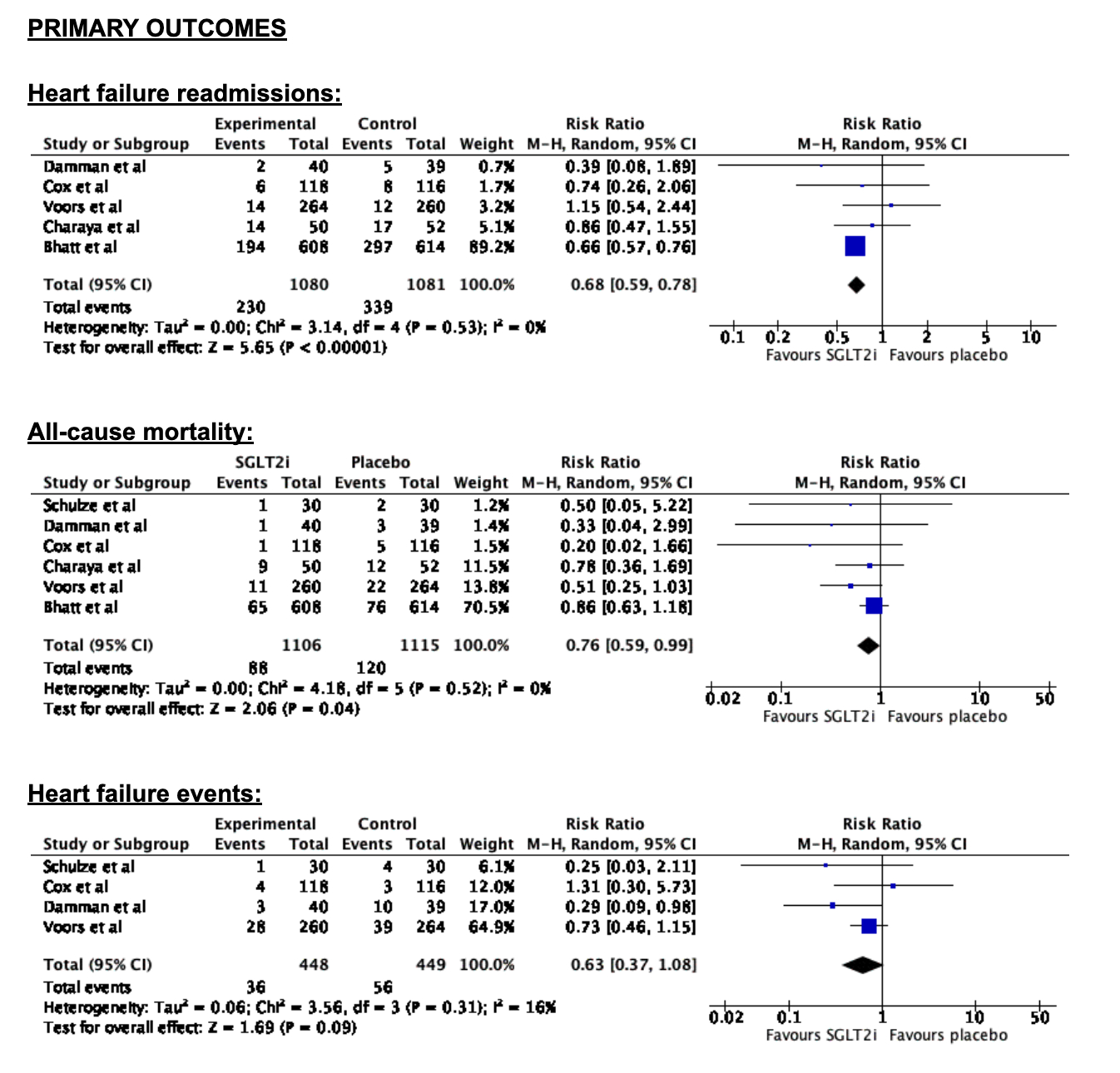
Seven RCTs were included, involving a total of 2321 patients, with 49.5% receiving SGLT2 inhibitors. Patients receiving SGLT2 inhibitors showed a significant reduction in the risk of readmissions by 32% (RR = 0.68, p < 0.00001). They also showed a non-significant but reduced risk of all-cause mortality by 24% (RR = 0.76, p = 0.04), and heart failure events by 27% (RR = 0.63, p = 0.09).
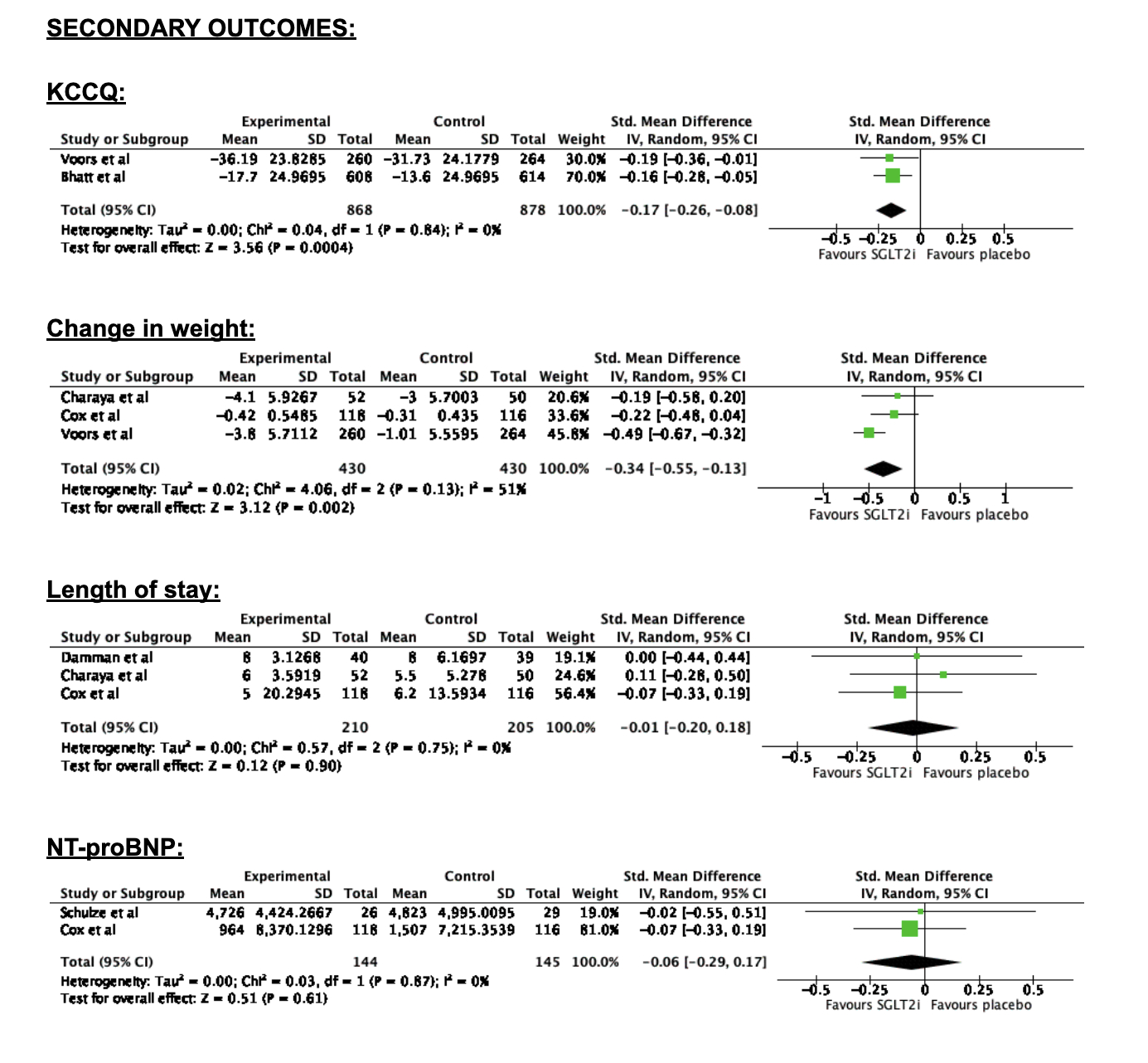
With respect to the secondary outcomes, there was a significant reduction in KCCQ-TSS (SMD= -0.17; 95% CI: -0.26 to -0.08; p=0.004) and weight (SMD= -0.34; 95% CI: -0.55 to -0.13; p=0.002) in the intervention group as compared to the placebo group. This group was also associated with a non-significant but reduced length of stay (SMD= -0.01; 95% CI: -0.20 to -0.18; p=0.90) and NT-proBNP levels (SMD= -0.06; 95% CI: -0.29 to -0.17; p=0.61).
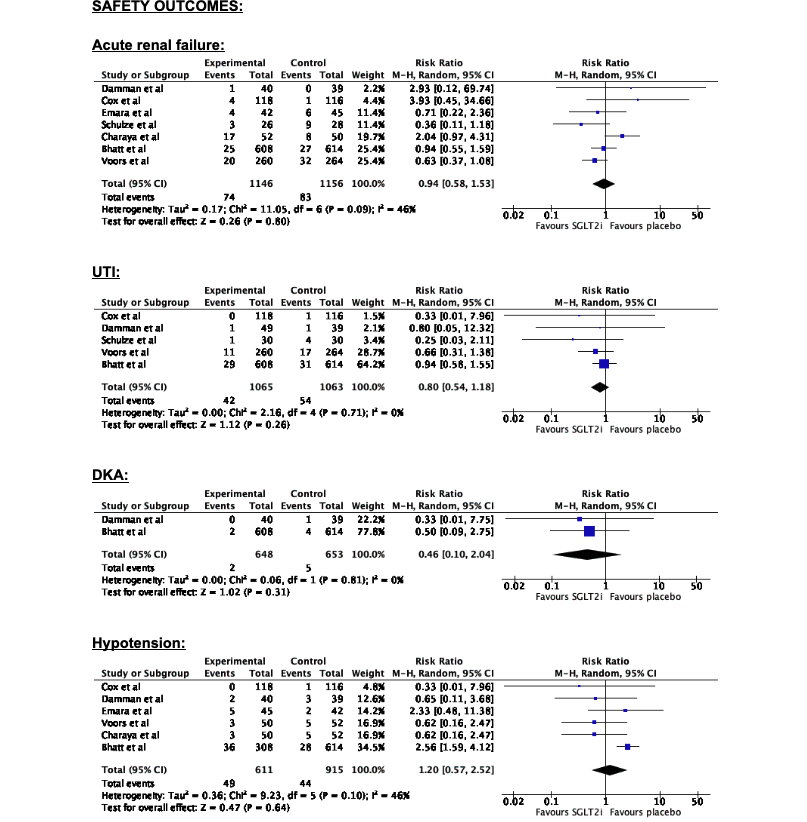
On analysis of the safety outcomes, there was a non significant difference in the risk of acute renal failure, UTI, and DKA.
Conclusion:
In patients with AHF, initiation of SGLT2 inhibitors showed a statistically significant reduction in heart failure rehospitalizations, improved weight-based diuretic efficiency, and KCCQ-TSS. These findings suggest that starting SGLT2 inhibitors in patients hospitalized for AHF is well tolerated and leads to clinical benefits.
Introduction:
Acute heart failure (AHF) presents challenges due to its poor prognosis and limited therapeutic options compared to chronic heart failure (CHF). The potential benefits of SGLT2 inhibitors in AHF patients are being explored, yet systematic evaluation is lacking. Our meta-analysis aims to bridge this gap by comparing the efficacy and safety of SGLT2 inhibitors versus placebo in AHF patients.
Research question:
Clinical Outcomes Of SGLT2 Inhibitors In Patients Hospitalized With Acute Heart Failure
Methods:
We searched Medline, Embase, and Cochrane databases for randomized controlled trials involving adult patients hospitalized with AHF, who received SGLT2 inhibitors. Our primary outcomes were all-cause mortality, heart failure events, and readmissions. The secondary outcomes were change in KCCQ-TSS (Kansas City Cardiomyopathy Questionnaire), weight, length of stay and NT-proBNP levels. Safety outcomes included hypotension, hypoglycemia, UTI, DKA, and acute renal failure. We used Review Manager 5.4 for statistical analysis, employing standardized mean difference (SMD) and risk ratio (RR) with 95% confidence intervals (CI).
Results:
Seven RCTs were included, involving a total of 2321 patients, with 49.5% receiving SGLT2 inhibitors. Patients receiving SGLT2 inhibitors showed a significant reduction in the risk of readmissions by 32% (RR = 0.68, p < 0.00001). They also showed a non-significant but reduced risk of all-cause mortality by 24% (RR = 0.76, p = 0.04), and heart failure events by 27% (RR = 0.63, p = 0.09).
With respect to the secondary outcomes, there was a significant reduction in KCCQ-TSS (SMD= -0.17; 95% CI: -0.26 to -0.08; p=0.004) and weight (SMD= -0.34; 95% CI: -0.55 to -0.13; p=0.002) in the intervention group as compared to the placebo group. This group was also associated with a non-significant but reduced length of stay (SMD= -0.01; 95% CI: -0.20 to -0.18; p=0.90) and NT-proBNP levels (SMD= -0.06; 95% CI: -0.29 to -0.17; p=0.61).
On analysis of the safety outcomes, there was a non significant difference in the risk of acute renal failure, UTI, and DKA.
Conclusion:
In patients with AHF, initiation of SGLT2 inhibitors showed a statistically significant reduction in heart failure rehospitalizations, improved weight-based diuretic efficiency, and KCCQ-TSS. These findings suggest that starting SGLT2 inhibitors in patients hospitalized for AHF is well tolerated and leads to clinical benefits.
More abstracts on this topic:
A Case of Steroid-Refractory Immune-checkpoint-inhibitor Induced Myocarditis Responsive to Mycophenolate and Anti-thymocyte globulin
Dabdoub Jorge, Wilson Michael, Gottbrecht Matthew, Salazar Ryan, Shih Jeffrey
Impact Of Admission Timing On Management And In-Hospital Outcomes In Acute Heart Failure: Insight From The CAN-HF RegistryAlshakhs Abdulmohsen, Moghaddam Nima, Makedonski Petko, Hawkins Nathaniel, Mckelvie Robert, Poon Stephanie, Honos George, Ezekowitz Justin, Zieroth Shelley, Virani Sean