Final ID: FR508
Geographic and Demographic Trends in Malnutrition and Hypertension Related Mortality in the United States from 1999 to 2020: Insights from CDC WONDER databse.
Abstract Body: Introduction: Malnutrition can worsen cardiovascular outcomes and is often under-recognized in adults with hypertension. This study examined national trends and disparities in mortality involving both malnutrition and hypertension among United States(US) adults aged ≥25 years from 1999 to 2020.
Hypothesis: We hypothesized that mortality involving both malnutrition and hypertension has increased over time and that significant disparities exist by sex, race/ethnicity, and geographic region.
Methods: We conducted a retrospective analysis using CDC WONDER data among US adults aged ≥25 years from 1999 to 2020. Death certificates listing both malnutrition (ICD-10: E40–E46) and hypertension (ICD-10: I10–I15) as contributing causes were included. Age-adjusted mortality rates (AAMRs) per 100,000 persons and annual percent changes (APCs) were calculated using Joinpoint regression and stratified by sex, race/ethnicity, region, urbanization level, and state.
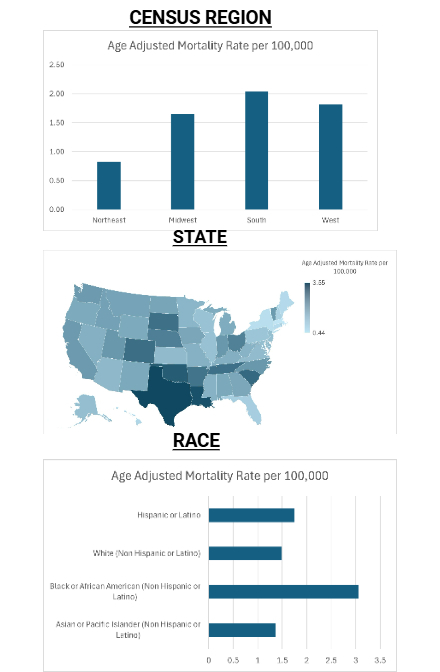
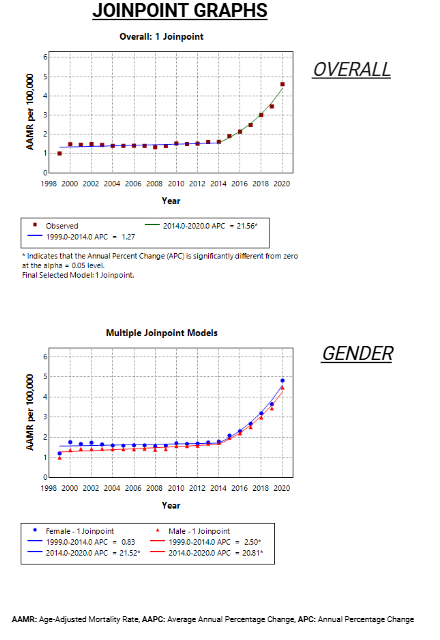
Results: Between 1999 and 2020, 79,419 deaths were attributed to coexisting malnutrition and hypertension in adults aged ≥25 years. The AAMR increased from 0.72 in 1999 to 4.33 in 2020 (AAPC: 7.0; 95% CI: 5.5–8.0). Notably, AAMR increased sharply from 2014 to 2020 (APC: 21.56; p < 0.000001). Males had a slightly lower AAMR than females (1.55 vs. 1.68), but experienced a steeper long-term increase (AAPC: 7.4, p < 0.000001) compared to females (AAPC:6.35, p < 0.000001). Racial disparities were evident, with Non-Hispanic (NH) Blacks having the highest AAMR (3.1), followed by Hispanics (1.7), NH Whites (1.5), and NH Asians/Pacific Islanders (1.4). AAMRs were highest in the South (2.04) and West (1.82), and lowest in the Northeast (0.83). At the state level, Texas reported the highest AAMR (3.55), while the lowest rates were observed in Massachusetts (0.44). Rural areas had slightly higher AAMRs (1.85) than urban areas (1.61).
Conclusion: Over the last 21 years, mortalities involving both malnutrition and hypertension have risen significantly across the US. These trends have not affected all groups equally. Men, NH Black adults, and individuals living in the southern region of the US and nonmetropolitan areas have had higher mortality rates. These trends call for enhanced public health initiatives focused on nutrition and chronic disease management, as well as coordinated efforts addressing social determinants of health.
Hypothesis: We hypothesized that mortality involving both malnutrition and hypertension has increased over time and that significant disparities exist by sex, race/ethnicity, and geographic region.
Methods: We conducted a retrospective analysis using CDC WONDER data among US adults aged ≥25 years from 1999 to 2020. Death certificates listing both malnutrition (ICD-10: E40–E46) and hypertension (ICD-10: I10–I15) as contributing causes were included. Age-adjusted mortality rates (AAMRs) per 100,000 persons and annual percent changes (APCs) were calculated using Joinpoint regression and stratified by sex, race/ethnicity, region, urbanization level, and state.
Results: Between 1999 and 2020, 79,419 deaths were attributed to coexisting malnutrition and hypertension in adults aged ≥25 years. The AAMR increased from 0.72 in 1999 to 4.33 in 2020 (AAPC: 7.0; 95% CI: 5.5–8.0). Notably, AAMR increased sharply from 2014 to 2020 (APC: 21.56; p < 0.000001). Males had a slightly lower AAMR than females (1.55 vs. 1.68), but experienced a steeper long-term increase (AAPC: 7.4, p < 0.000001) compared to females (AAPC:6.35, p < 0.000001). Racial disparities were evident, with Non-Hispanic (NH) Blacks having the highest AAMR (3.1), followed by Hispanics (1.7), NH Whites (1.5), and NH Asians/Pacific Islanders (1.4). AAMRs were highest in the South (2.04) and West (1.82), and lowest in the Northeast (0.83). At the state level, Texas reported the highest AAMR (3.55), while the lowest rates were observed in Massachusetts (0.44). Rural areas had slightly higher AAMRs (1.85) than urban areas (1.61).
Conclusion: Over the last 21 years, mortalities involving both malnutrition and hypertension have risen significantly across the US. These trends have not affected all groups equally. Men, NH Black adults, and individuals living in the southern region of the US and nonmetropolitan areas have had higher mortality rates. These trends call for enhanced public health initiatives focused on nutrition and chronic disease management, as well as coordinated efforts addressing social determinants of health.
More abstracts on this topic:
A Meta-Analysis on the Effect of Chronic Total Occlusion of Coronary Arteries on Cardiovascular Outcomes in Patients Undergoing Transcatheter Aortic Valve Replacement
Goyal Aman, Tariq Muhammad Daoud, Zahra Rubab, Jain Hritvik, Khan Rozi, Mahalwar Gauranga
A Retrospective Analysis of Chronic Kidney Disease and Arrhythmias-Related Mortality Among Adults in the United States (1999-2020): Insights into Disparities by Gender, Race/Ethnicity, and GeographyWaseem Neha, Nouman Zainab, Chaudhry Sohaib Aftab Ahmad, Tariq Waleed, Khan Iftikhar, Shah Mazhar, Farooqi Hanzala Ahmed, Faiz Muneeb