Final ID: P-134
Effects of Antihypertensive Medications on All-cause Dementia: Evidence from Target Trial Emulation of 3 Million US Veterans
Abstract Body: Introduction: Hypertension is a modifiable risk factor for all-cause dementia. Mechanistic and observational evidence suggest angiotensin receptor blockers (ARBs) and angiotensin converting enzyme inhibitors (ACEIs) may differentially affect dementia risk.
Objective and Methods: We used longitudinal electronic health records of over 3 million US Veterans to conduct a target trial emulation with a new-user, active comparator design. We compared the intention-to-treat effect of initiating ARBs vs ACEIs (1/1/2000-12/31/2022) on dementia risk. We controlled for >60 baseline covariates using inverse probability (IP) of treatment and overlap weighting. Dementia was ascertained using diagnosis codes and medications. We nonparametrically estimated the cause-specific cumulative incidence for each treatment group under the competing risk of death then computed treatment effects as weighted risk ratios with bootstrapped 95% confidence intervals. We also evaluated all-cause death and a composite outcome of dementia or death (dementia/Death) using Cox regression.
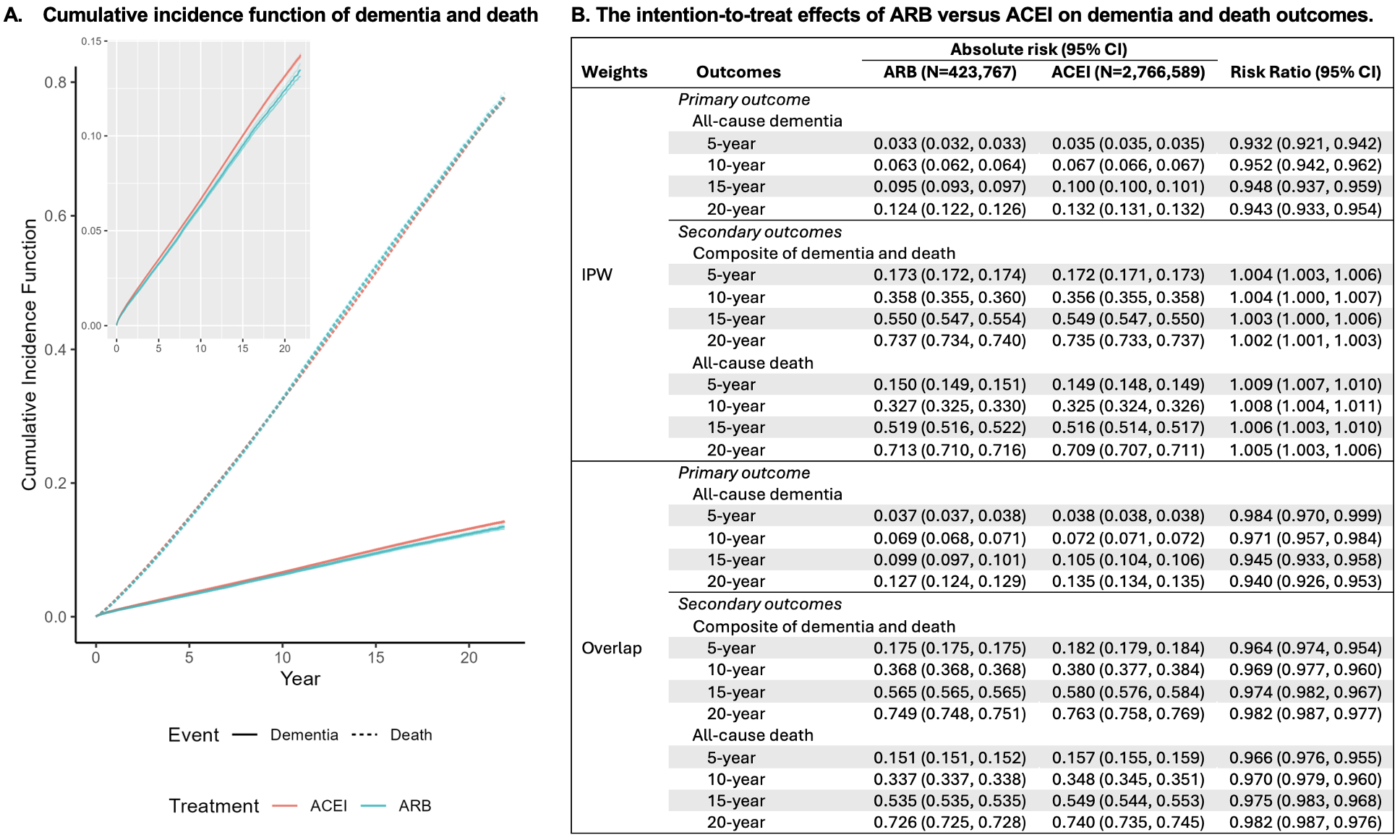
Results: Among the 3,190,356 included Veterans (mean age 63, 5% female, 64% White, and 15% Black), 13% initiated ARBs and 87% initiated ACEIs. Overall, 8% developed dementia and 35% died over a median follow-up of 8 years. The risk of dementia was lower among ARB vs ACEI initiators (10-year risk ratio: 0.95 (0.94, 0.96)). The risk of all-cause death and dementia/Death were also lower among ARB vs ACEI initiators with overlap weighting.
Conclusions: Among US Veterans with hypertension, ARB vs ACEI initiation was associated with a moderately lower risk of dementia. Future work assessing sustained treatment with ARB vs ACEI is needed to inform their use to reduce dementia risk.
Objective and Methods: We used longitudinal electronic health records of over 3 million US Veterans to conduct a target trial emulation with a new-user, active comparator design. We compared the intention-to-treat effect of initiating ARBs vs ACEIs (1/1/2000-12/31/2022) on dementia risk. We controlled for >60 baseline covariates using inverse probability (IP) of treatment and overlap weighting. Dementia was ascertained using diagnosis codes and medications. We nonparametrically estimated the cause-specific cumulative incidence for each treatment group under the competing risk of death then computed treatment effects as weighted risk ratios with bootstrapped 95% confidence intervals. We also evaluated all-cause death and a composite outcome of dementia or death (dementia/Death) using Cox regression.
Results: Among the 3,190,356 included Veterans (mean age 63, 5% female, 64% White, and 15% Black), 13% initiated ARBs and 87% initiated ACEIs. Overall, 8% developed dementia and 35% died over a median follow-up of 8 years. The risk of dementia was lower among ARB vs ACEI initiators (10-year risk ratio: 0.95 (0.94, 0.96)). The risk of all-cause death and dementia/Death were also lower among ARB vs ACEI initiators with overlap weighting.
Conclusions: Among US Veterans with hypertension, ARB vs ACEI initiation was associated with a moderately lower risk of dementia. Future work assessing sustained treatment with ARB vs ACEI is needed to inform their use to reduce dementia risk.
More abstracts on this topic:
A Key Role of Proximal Tubule Renin-Angiotensin System in The Kidney in The Development of Kidney Ischemia and Reperfusion Injury
Li Xiao, Hassan Rumana, Katsurada Akemi, Sato Ryosuke, Zhuo Jia
Combination Therapy with ACEIs/ARBs and β-Blockers Reduces Basal Inflammation in Heart Failure Patients: A Cross-Sectional Observational StudyKataya Rayan, Zouein Fouad, Ziade Joanna, Amin Ghadir, Mansour Sara, Elbejjani Martine, Fares Souha, Mudawwar Walid, Refaat Marwan, Mericskay Mathias