Final ID: TH890
Urinary Metabolomics Signature for Cognitive Function among African American Patients with Chronic Kidney Disease
Abstract Body: Introduction: Patients with chronic kidney disease (CKD) have a substantially higher risk of cognitive impairment. Metabolic dysregulation and accumulation of uremic toxins in CKD may contribute to neurocognitive decline through oxidative stress, inflammation, and blood–brain barrier (BBB) dysfunction. Because the kidney and BBB share solute transport mechanisms, urine metabolomics provides a noninvasive approach to capture systemic metabolic alterations relevant to brain health. However, urinary metabolomic correlates of cognitive function in CKD remain largely unexplored. This study examined associations between urine metabolites and cognitive function measures among African American patients with CKD.
Methods: We analyzed data from 1,681 African American participants in the Chronic Renal Insufficiency Cohort (CRIC). Baseline metabolites were quantified from 24-hour urine samples using the untargeted Metabolon platform. Cognitive function was assessed using the Mini-Mental State Examination (MMSE) at baseline and annually over a median follow-up of 9.1 years. Multivariable linear mixed-effects models were used to estimate associations of each metabolite with repeatedly measured cognitive scores, adjusting for age, sex, education, study site in the base model and additionally for hypertension, diabetes, depression, LDL cholesterol, BMI, ACE inhibitors or ARB use, smoking, and alcohol use in the full model. False discovery rate (FDR) correction was applied. To evaluate the predictive value of the metabolite profile, we developed a composite metabolite score using LASSO regression with 10-fold cross-validation to select the optimal penalty parameter. We then compared two regression models: Model 1 included all covariates from the full model, and Model 2 additionally included the metabolite score.
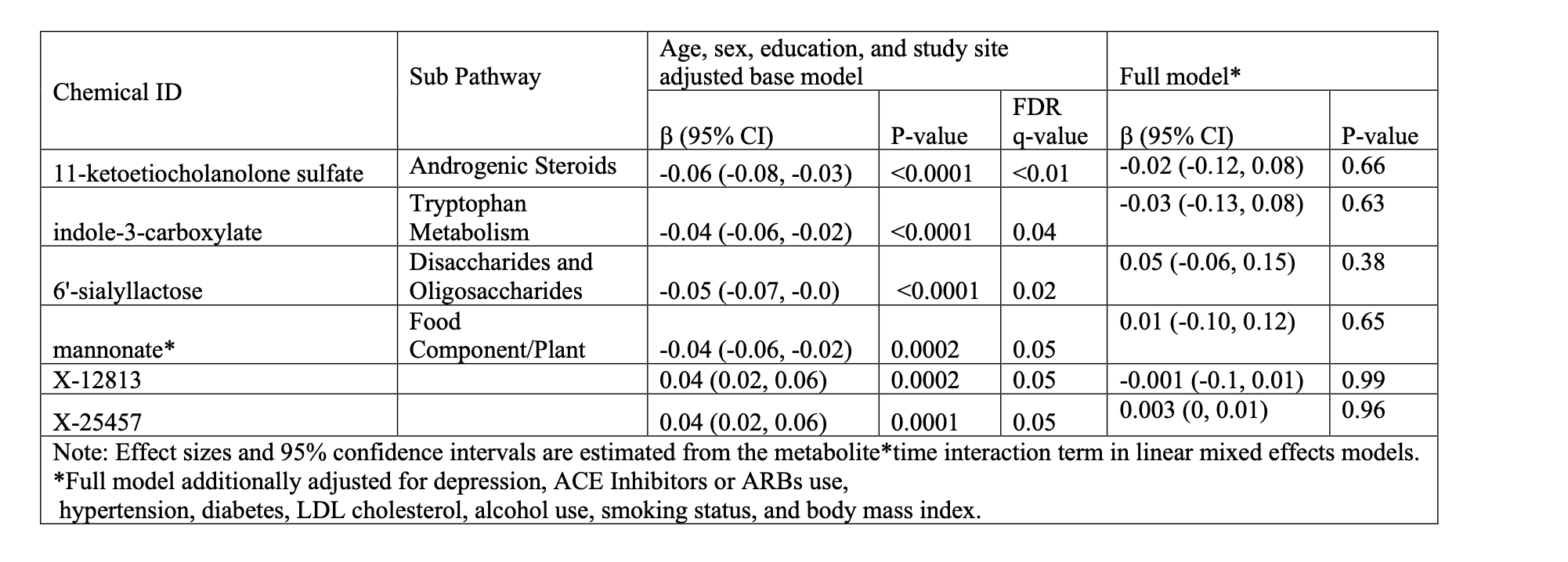
Results: Six metabolites were significantly associated with MMSE scores in the base model (Table). However, these associations were attenuated and not significant in the full model. Nineteen metabolites were selected by LASSO to construct the composite metabolite score. The score was strongly associated with MMSE decline (β = 0.031 per SD, P < 0.001) and modestly but significantly improved model fit, explaining an additional 3.9% of variance over the fully adjusted model (P < 0.001).
Conclusions: A composite metabolite score integrating 19 urinary metabolites modestly but significantly improved the prediction of cognitive decline beyond conventional risk factors.
Methods: We analyzed data from 1,681 African American participants in the Chronic Renal Insufficiency Cohort (CRIC). Baseline metabolites were quantified from 24-hour urine samples using the untargeted Metabolon platform. Cognitive function was assessed using the Mini-Mental State Examination (MMSE) at baseline and annually over a median follow-up of 9.1 years. Multivariable linear mixed-effects models were used to estimate associations of each metabolite with repeatedly measured cognitive scores, adjusting for age, sex, education, study site in the base model and additionally for hypertension, diabetes, depression, LDL cholesterol, BMI, ACE inhibitors or ARB use, smoking, and alcohol use in the full model. False discovery rate (FDR) correction was applied. To evaluate the predictive value of the metabolite profile, we developed a composite metabolite score using LASSO regression with 10-fold cross-validation to select the optimal penalty parameter. We then compared two regression models: Model 1 included all covariates from the full model, and Model 2 additionally included the metabolite score.
Results: Six metabolites were significantly associated with MMSE scores in the base model (Table). However, these associations were attenuated and not significant in the full model. Nineteen metabolites were selected by LASSO to construct the composite metabolite score. The score was strongly associated with MMSE decline (β = 0.031 per SD, P < 0.001) and modestly but significantly improved model fit, explaining an additional 3.9% of variance over the fully adjusted model (P < 0.001).
Conclusions: A composite metabolite score integrating 19 urinary metabolites modestly but significantly improved the prediction of cognitive decline beyond conventional risk factors.
More abstracts on this topic:
Adoptive transfer of placental CD4+ T Cells from preeclamptic patients with a history of COVID-19 causes hypertension and cognitive dysfunction postpartum in a pregnant rat model of preeclampsia
Deer Evangeline, Simmons Kimberly, Herrock Owen, Campbell Nathan, Roman Richard, Zheng Baoying, Morris Rachael, Lamarca Babbette
Burden of Non-Rheumatic Valvular Heart Disease in High-income Asia Pacific from 1990-2019: A Benchmarking analysisShaikh Salomi, Amin Vishrant, Desai Hardik, Sharma Kamal, Shandilya Ashwinikumar, Patel Khushbu, Waqas Muhammad, Syed Saif, Lakkimsetti Mohit, Bhalodia Paritaben, Islam Hamza, Patel Juhi