Final ID: TH831
Association of food security status with healthcare utilization in HRTSA (Heart FailuRe Transitional Care Services for Adults) Clinic Patients
Abstract Body: Background: In the United States, heart failure (HF) mortality is associated with the food environment, among other area-level measures of social risk. The HRTSA Clinic at the University of Alabama at Birmingham serves vulnerable adults with HF and high social risk. We sought to explore the relationship of food security status on healthcare utilization in this unique population.
Methods: Patients with HF referred to the HRTSA Clinic who were screened for food insecurity status were included. Complete data on demographics, neighborhood social vulnerability index (SVI), and health care encounters (2013-2023) were extracted from the health record. The exposure of interest was food insecurity at Visit 1 based on the validated Hunger Vital Sign, a two-item food insecurity screening tool utilized at the clinic. The outcomes of interest were number of inpatient encounters (IE), number of emergency room encounters (EE), defined as any encounter in the ER that resulted in discharge without inpatient admission, and total number of encounters. Total encounter number was defined as the sum of IE and EE. Both unadjusted and adjusted logistic regression models were constructed to estimate the odds ratio of health care encounters for those with food insecurity versus those that were food secure.
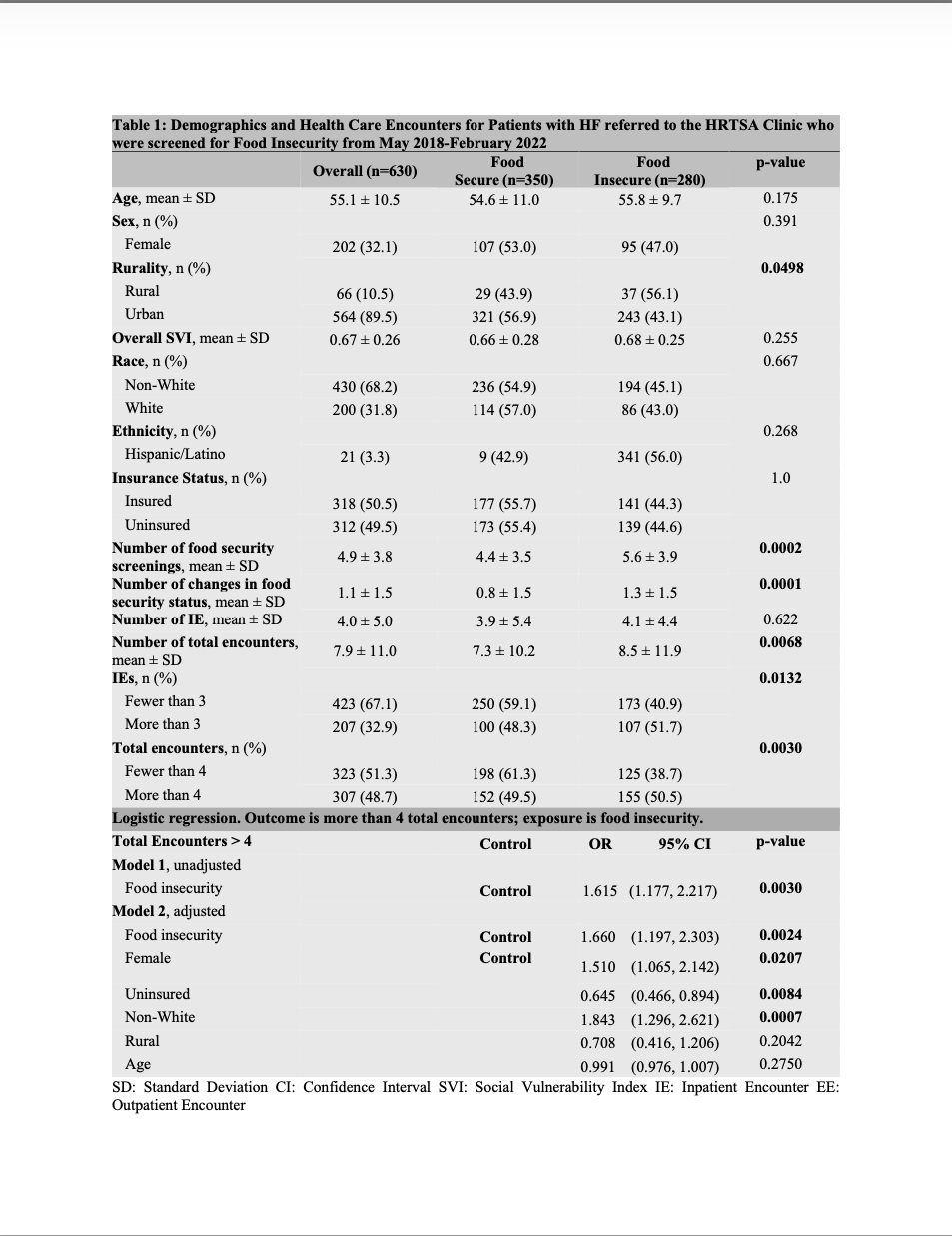
Results: Of the 1155 patients referred to HRTSA, 630 patients had complete data and were included in this analysis. For the entire population, the median number of EE was 3, median number of IE was 2, and mean time of observation was 3.96 ± 2.98 years. Patients were similar between groups in SVI score, but differed in rurality, number of food security screenings, and number of changes in food security status. In the unadjusted logistic regression model, being food insecure was associated with having more than 4 total healthcare encounters than being food secure. This association persists when adjusted for sex, insurance status, race, age, and rurality (Table 1).
Conclusion: Food insecurity is an important measure of social risk and is associated with increased healthcare utilization among underserved patients with HF, even in adjusted analysis. Additionally, patients in rural communities with high social risk have a higher likelihood of food insecurity, influencing their increased healthcare utilization and providing a target for future community-based interventions.
Methods: Patients with HF referred to the HRTSA Clinic who were screened for food insecurity status were included. Complete data on demographics, neighborhood social vulnerability index (SVI), and health care encounters (2013-2023) were extracted from the health record. The exposure of interest was food insecurity at Visit 1 based on the validated Hunger Vital Sign, a two-item food insecurity screening tool utilized at the clinic. The outcomes of interest were number of inpatient encounters (IE), number of emergency room encounters (EE), defined as any encounter in the ER that resulted in discharge without inpatient admission, and total number of encounters. Total encounter number was defined as the sum of IE and EE. Both unadjusted and adjusted logistic regression models were constructed to estimate the odds ratio of health care encounters for those with food insecurity versus those that were food secure.
Results: Of the 1155 patients referred to HRTSA, 630 patients had complete data and were included in this analysis. For the entire population, the median number of EE was 3, median number of IE was 2, and mean time of observation was 3.96 ± 2.98 years. Patients were similar between groups in SVI score, but differed in rurality, number of food security screenings, and number of changes in food security status. In the unadjusted logistic regression model, being food insecure was associated with having more than 4 total healthcare encounters than being food secure. This association persists when adjusted for sex, insurance status, race, age, and rurality (Table 1).
Conclusion: Food insecurity is an important measure of social risk and is associated with increased healthcare utilization among underserved patients with HF, even in adjusted analysis. Additionally, patients in rural communities with high social risk have a higher likelihood of food insecurity, influencing their increased healthcare utilization and providing a target for future community-based interventions.
More abstracts on this topic:
6-Nitrodopamine potentiates the positive chronotopic and inotropic effect induced by noradrenaline in the rat isolated heart
Lima Antonio, Sobanski Joao Fernando, Antunes Edson, De Nucci Gilberto
5-oxoproline/ OPLAH Axis Alleviates Doxorubicin-induced Cardiomyopathy By Inhibiting FerroptosisJiang Meng, Guo Xinning