Final ID: TH802
Adverse Events Associated with Immune Checkpoint Inhibitors in a Real-World Hispanic Cohort: Analysis of Cardiovascular Outcomes
Abstract Body: Background
Immune checkpoint inhibitors (ICIs) have transformed cancer therapy, yet data on cardiovascular and thrombotic safety in Hispanic populations are limited. Evidence from the Hispanic Community Health Study (HCHS) shows disproportionate cardiometabolic risk for major adverse cardiovascular events (MACE) and thrombosis, likely influenced by social determinants.
Objective:
We aimed to describe the incidence and predictors of MACE and thrombosis in ICI-treated adults at a Colombian quaternary center.
Methods
We conducted an observational retrospective study including adults (≥18 y) treated with PD-1, PD-L1, or PD-1 + CTLA-4 inhibitors (2020–2024). Data were extracted from electronic records into REDCap. Outcomes were MACE, thrombosis, and irAEs. Event-free survival was estimated by Kaplan–Meier; predictors were assessed using multivariable Cox regression.
Results
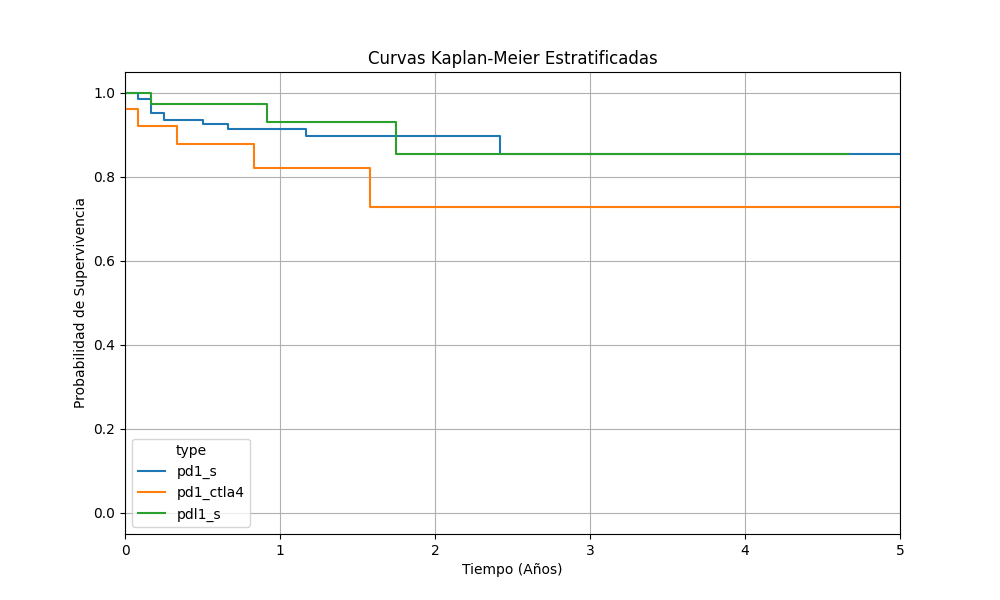
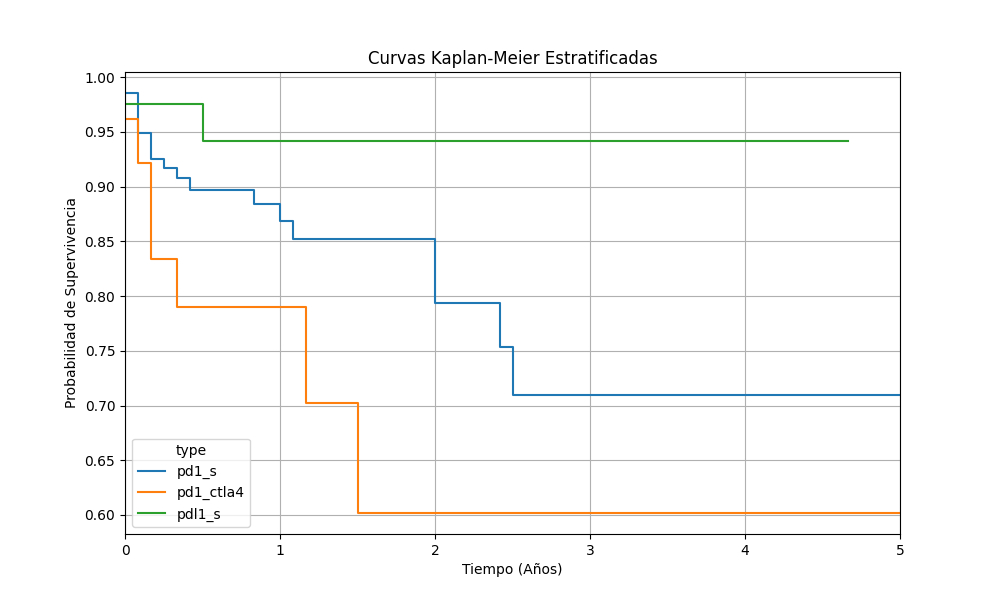
A total of 206 patients were included (median age 66 years, 59.7 % male). Most received PD-1 inhibitors (67.5 %), followed by PD-L1 (19.9 %) and combined PD-1 + CTLA-4 therapy (12.6 %). Overall, MACE occurred in 21 patients (10.2%), mainly myocardial infarction and heart failure, while thrombotic events were reported in 29 (14.1%), predominantly venous (11.7%). Median times to MACE and thrombosis were 302 and 274 days, respectively (Figure 1 and 2). The combination group showed the highest incidence of both complications (MACE 19.2%, thrombosis 26.9%) compared with PD-1 (9.4%, 14.4%) and PD-L1 (77.3% 4.9%), reaching statistical significance for thrombosis (p = 0.04). Concomitant chemotherapy independently increased thrombotic risk (HR 2.49, 95% CI 1.12–5.54, p = 0.025), whereas no covariates predicted MACE. Patients developing both MACE and thrombosis exhibited markedly reduced survival (HR 2.26, 95% CI 0.97–5.23, p = 0.058). Co-occurrence of these events was more frequent among high ASCVD-risk patients (30 %) than in intermediate (3.1 %) and low-risk (5.7 %) groups (p = 0.018), underscoring the prognostic value of baseline cardiovascular risk in ICI-treated populations.
Conclusion
In this real-world Hispanic cohort, ICIs were associated with notable thrombotic and cardiovascular toxicity, especially with PD-1 + CTLA-4 therapy. The coexistence of MACE and thrombosis as well as elevated baseline ASCVD risk, identified patients with poorer survival, underscoring the need for cardio-oncologic surveillance and preventive strategies as immunotherapy expands in Latin America.
Immune checkpoint inhibitors (ICIs) have transformed cancer therapy, yet data on cardiovascular and thrombotic safety in Hispanic populations are limited. Evidence from the Hispanic Community Health Study (HCHS) shows disproportionate cardiometabolic risk for major adverse cardiovascular events (MACE) and thrombosis, likely influenced by social determinants.
Objective:
We aimed to describe the incidence and predictors of MACE and thrombosis in ICI-treated adults at a Colombian quaternary center.
Methods
We conducted an observational retrospective study including adults (≥18 y) treated with PD-1, PD-L1, or PD-1 + CTLA-4 inhibitors (2020–2024). Data were extracted from electronic records into REDCap. Outcomes were MACE, thrombosis, and irAEs. Event-free survival was estimated by Kaplan–Meier; predictors were assessed using multivariable Cox regression.
Results
A total of 206 patients were included (median age 66 years, 59.7 % male). Most received PD-1 inhibitors (67.5 %), followed by PD-L1 (19.9 %) and combined PD-1 + CTLA-4 therapy (12.6 %). Overall, MACE occurred in 21 patients (10.2%), mainly myocardial infarction and heart failure, while thrombotic events were reported in 29 (14.1%), predominantly venous (11.7%). Median times to MACE and thrombosis were 302 and 274 days, respectively (Figure 1 and 2). The combination group showed the highest incidence of both complications (MACE 19.2%, thrombosis 26.9%) compared with PD-1 (9.4%, 14.4%) and PD-L1 (77.3% 4.9%), reaching statistical significance for thrombosis (p = 0.04). Concomitant chemotherapy independently increased thrombotic risk (HR 2.49, 95% CI 1.12–5.54, p = 0.025), whereas no covariates predicted MACE. Patients developing both MACE and thrombosis exhibited markedly reduced survival (HR 2.26, 95% CI 0.97–5.23, p = 0.058). Co-occurrence of these events was more frequent among high ASCVD-risk patients (30 %) than in intermediate (3.1 %) and low-risk (5.7 %) groups (p = 0.018), underscoring the prognostic value of baseline cardiovascular risk in ICI-treated populations.
Conclusion
In this real-world Hispanic cohort, ICIs were associated with notable thrombotic and cardiovascular toxicity, especially with PD-1 + CTLA-4 therapy. The coexistence of MACE and thrombosis as well as elevated baseline ASCVD risk, identified patients with poorer survival, underscoring the need for cardio-oncologic surveillance and preventive strategies as immunotherapy expands in Latin America.
More abstracts on this topic:
Air Pollution Induces Atrial Fibrosis via CARD9-Mediated Immune Response
Cui Yuqi, Ma Xiaochun, Patel Sheevang, Mraiyan Mohamed, Liu Zhenguo
Class IIa Histone Deacetylase Activity Mediates Increased Aortic Stiffness in a Mouse Model of Early Life StressKelly Gillian, Kellum Cailin, Edell Claudia, Heim Michael, Colson Jackson, Pollock Jennifer