Final ID: WE471
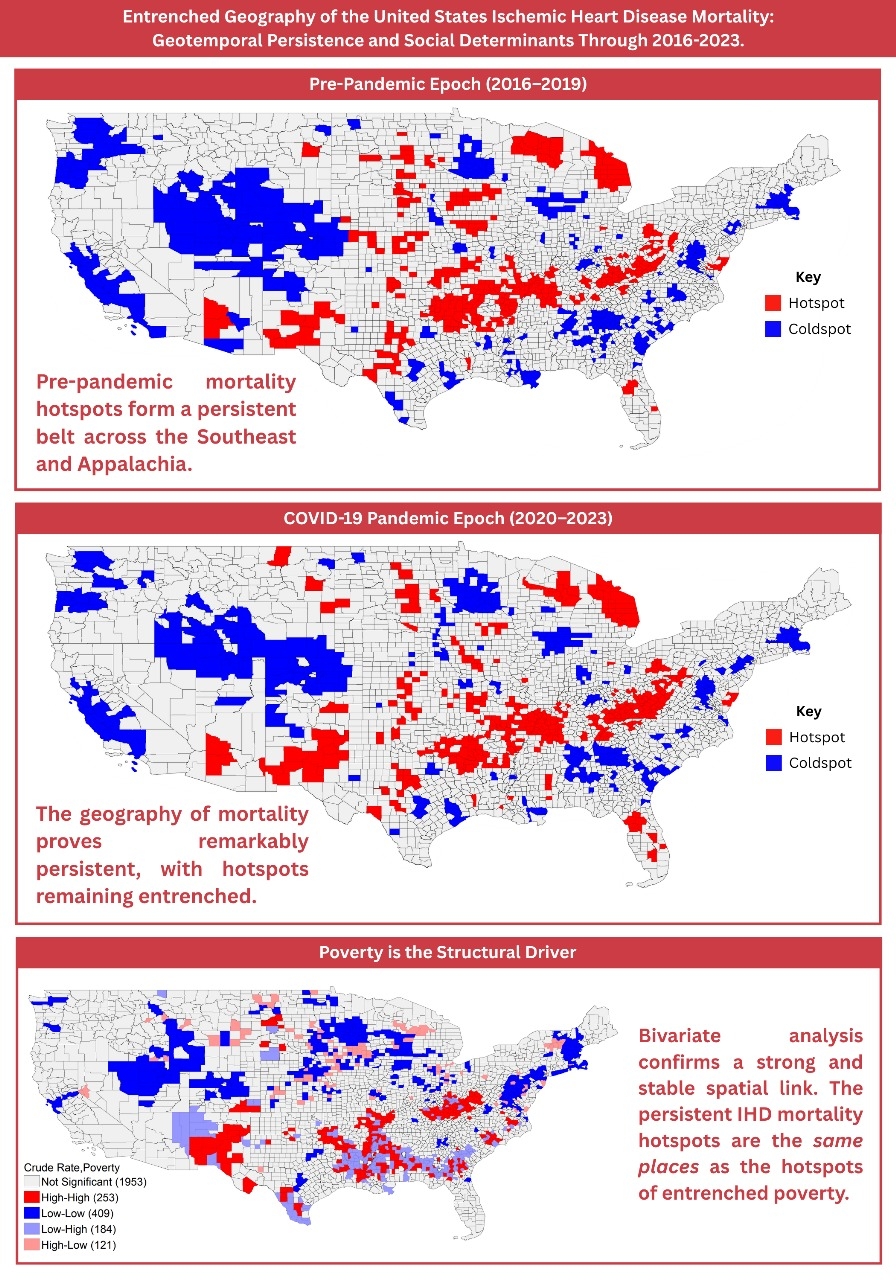
Entrenched Geography of the United States Ischemic Heart Disease Mortality: Geotemporal Persistence and Social Determinants Through 2016-2023.
Abstract Body: Background
Ischemic heart disease (IHD) remains the leading cause of death in the United States, with longstanding geographic disparities. The COVID-19 pandemic disrupted care delivery and exposed systemic vulnerabilities, raising questions about whether cardiovascular mortality patterns changed post- pandemic. This study examined pandemic-era IHD mortality hotspots and evaluated their persistence in relation to social determinants of health (SDoH).
Methods
County-level geospatial analysis of IHD mortality (ICD-10: I20–I25) using CDC WONDER data, comparing pre-pandemic (2016–2019) and pandemic-era (2020–2023) epochs was conducted using crude mortality rates (CMR). Poverty, insurance, and primary care physician density was analyzed as SDoH. Univariate Getis-Ord Gi* (p<0.05) identified hotspots and coldspots, while bivariate Local Moran’s I assessed spatial overlap of high-CMR clusters with adverse SDoH and with median age to evaluate age-related confounding.
Results
County-level comparison revealed remarkable persistence in the geography of the IHD mortality. Hotspots and coldspots decreased slightly from 379 to 373 and 423 to 408, respectively. Reflecting spatial stability with modest consolidation. High-burden clusters remained concentrated across the Mississippi Delta, central and southern Appalachia, and the rural Southeast, with smaller persistent pockets in the Midwest and Southwest. Coldspots persisted in the Mountain West, Pacific Northwest, and New England. Mean hotspot CMRs were nearly unchanged (207.25 vs. 206.90 per 100,000), while coldspot means rose marginally (95.34 vs. 95.73), indicating ongoing concentration within entrenched regions. Bivariate mapping showed overlap between older populations and IHD hotspots; however, median age increased more in coldspots (38.71 to 39.38) than hotspots (43.16 to 43.21), suggesting age alone does not explain disparities. Poverty exhibited the strongest, most stable spatial concordance with mortality hotspots, especially across the Southeast and Appalachia. Limited primary care access showed a similar but narrower alignment, while uninsuredness showed weaker, region-specific overlap in the South-Central region.
Conclusion
The pandemic reinforced rather than restructured the geography of IHD mortality. Persistent hotspot belts, aligned with entrenched poverty and constrained healthcare access, underscore the structural durability of regional inequities in cardiovascular outcomes despite nationwide systemic shock.
Ischemic heart disease (IHD) remains the leading cause of death in the United States, with longstanding geographic disparities. The COVID-19 pandemic disrupted care delivery and exposed systemic vulnerabilities, raising questions about whether cardiovascular mortality patterns changed post- pandemic. This study examined pandemic-era IHD mortality hotspots and evaluated their persistence in relation to social determinants of health (SDoH).
Methods
County-level geospatial analysis of IHD mortality (ICD-10: I20–I25) using CDC WONDER data, comparing pre-pandemic (2016–2019) and pandemic-era (2020–2023) epochs was conducted using crude mortality rates (CMR). Poverty, insurance, and primary care physician density was analyzed as SDoH. Univariate Getis-Ord Gi* (p<0.05) identified hotspots and coldspots, while bivariate Local Moran’s I assessed spatial overlap of high-CMR clusters with adverse SDoH and with median age to evaluate age-related confounding.
Results
County-level comparison revealed remarkable persistence in the geography of the IHD mortality. Hotspots and coldspots decreased slightly from 379 to 373 and 423 to 408, respectively. Reflecting spatial stability with modest consolidation. High-burden clusters remained concentrated across the Mississippi Delta, central and southern Appalachia, and the rural Southeast, with smaller persistent pockets in the Midwest and Southwest. Coldspots persisted in the Mountain West, Pacific Northwest, and New England. Mean hotspot CMRs were nearly unchanged (207.25 vs. 206.90 per 100,000), while coldspot means rose marginally (95.34 vs. 95.73), indicating ongoing concentration within entrenched regions. Bivariate mapping showed overlap between older populations and IHD hotspots; however, median age increased more in coldspots (38.71 to 39.38) than hotspots (43.16 to 43.21), suggesting age alone does not explain disparities. Poverty exhibited the strongest, most stable spatial concordance with mortality hotspots, especially across the Southeast and Appalachia. Limited primary care access showed a similar but narrower alignment, while uninsuredness showed weaker, region-specific overlap in the South-Central region.
Conclusion
The pandemic reinforced rather than restructured the geography of IHD mortality. Persistent hotspot belts, aligned with entrenched poverty and constrained healthcare access, underscore the structural durability of regional inequities in cardiovascular outcomes despite nationwide systemic shock.
More abstracts on this topic:
A Real-world Evaluation of Longitudinal Healthcare Expenses in a Health System Registry of Type-2 Diabetes Mellitus and Cardiovascular Disease Enabled by the 21st Century Cures Act
Dhingra Lovedeep, Aminorroaya Arya, Pedroso Aline, Rajpura Jigar, Mehanna Sherif, Tonnu-mihara Ivy, Khera Rohan
A Comprehensive Study on Machine Learning Models Combining with Oversampling for One-year Persistent Coronary Artery Aneurysm in Kawasaki DiseaseLiang Kaizhi, Pang Yusheng, Su Danyan