Final ID: 25
Ultra-processed Food Consumption Magnifies Genetic Risk of Obesity: A Gene-Diet Interaction Analysis in the Women's Genome Health Study
Abstract Body: Introduction
Ultra-processed Foods (UPFs) are associated with obesity, a key modifiable factor of poor cardiovascular health. Although genetics contributes to the risk of obesity, it is unknown whether the effect of UPF consumption on body mass index (BMI) is greater among individuals with underlying genetic susceptibility.
Hypothesis
We conducted gene-diet interaction analyses to assess whether the genetic risk of obesity increases the positive association between UPF consumption and BMI.
Methods
We conducted a cross-sectional analysis in the Women’s Genome Health Study among women of European ancestry with complete genetic data, available FFQ data, and BMI at baseline enrollment in 1992. We derived UPF intake (as % total energy), classifying foods and beverages by NOVA based on the nature, extent, and purpose of processing. BMI-related genotypes were captured by genome-wide (gwPRS) and pathway-specific (pPRSs) polygenic risk scores from GWAS statistics. The multivariable-adjusted linear regression models with effective independent test number and Sidak-corrected thresholds multiple testing adjustment were conducted to analyze continuous PRS and UPFs exposures with BMI as the outcome.
Results
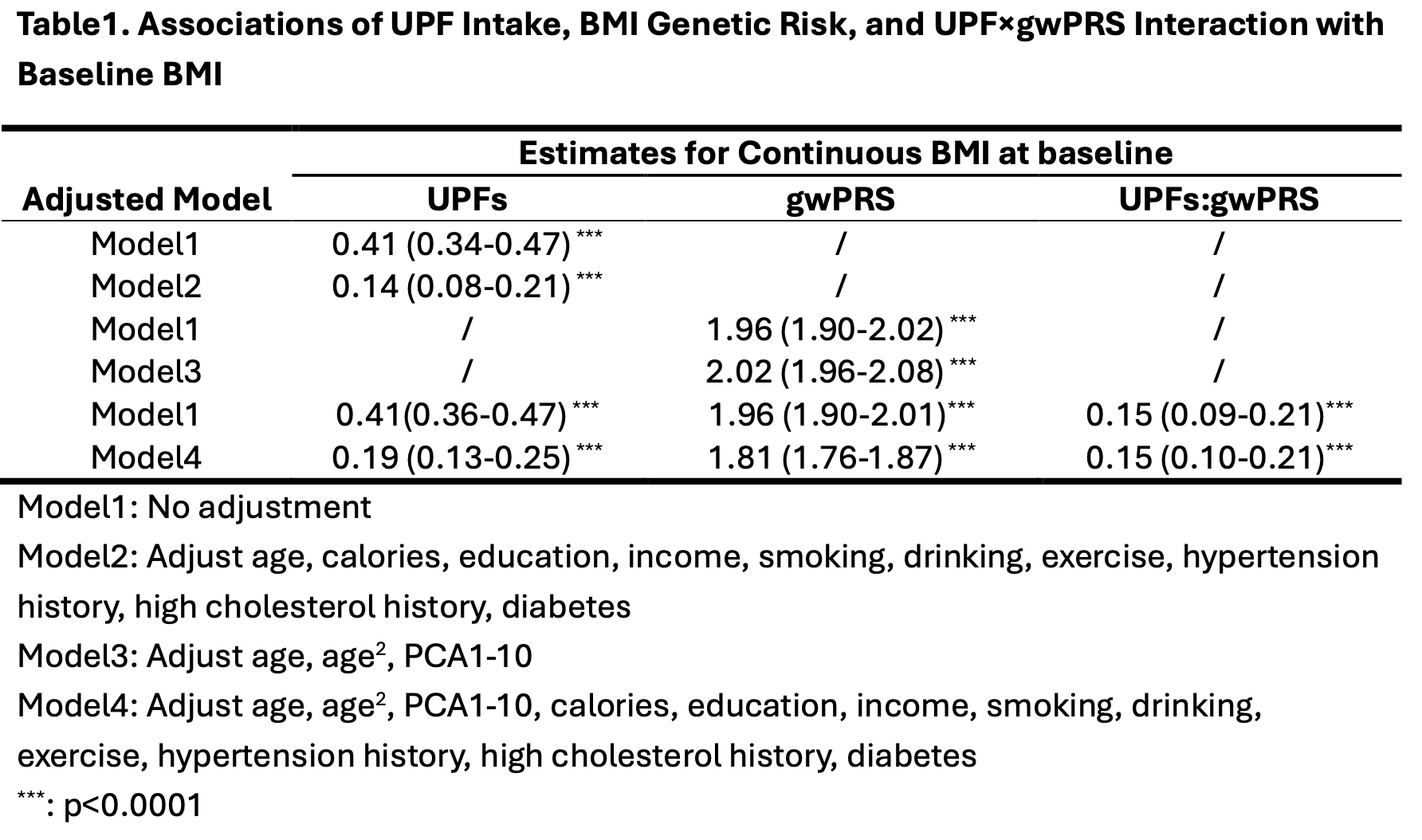
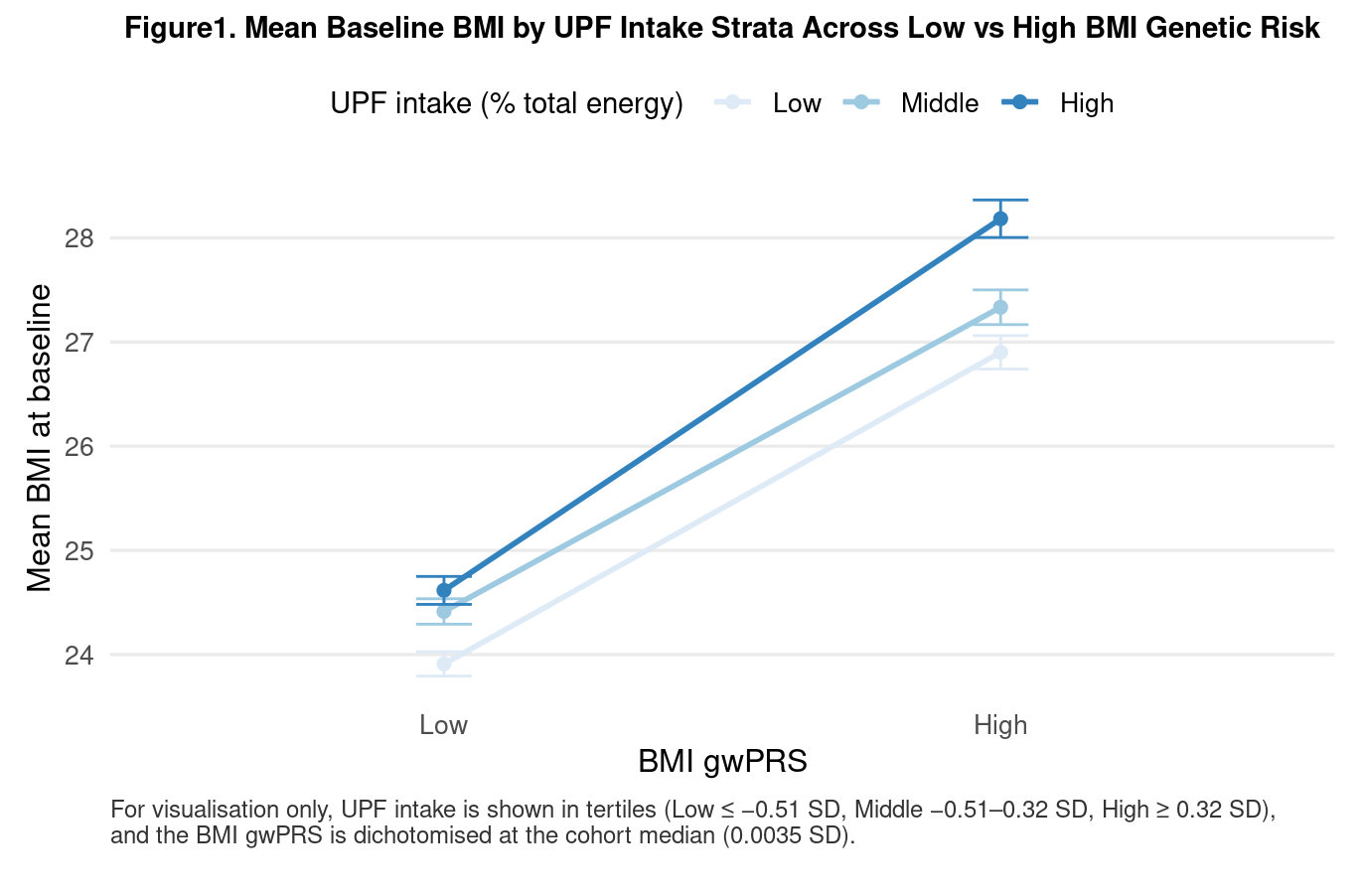
Among 22,471 WGHS participants, the mean UPF intake was 29.4 (SD 10.7) % total energy and BMI was 25.9 (4.9) kg/m2. In main effects models, higher gwPRS and UPF intake were linearly associated with higher BMI. We observed a significant positive interaction between gwPRS and UPF intake on BMI, with each 1-SD higher UPF intake associated with 0.15 kg/m2 higher BMI per 1-SD higher gwPRS (95% CI 0.10–0.21, p<0.0001) (Table 1). Women with higher UPF intake had an incrementally higher BMI, and the magnitude of this linear association was larger among women with higher genetic risk of obesity (Figure 1). There were no significant pPRS and UPF intake interactions among individual KEGG legacy pathways.
Conclusions
In this large US cohort of women, women who consumed a greater proportion of energy from UPFs or had greater genetic susceptibility to obesity had a higher BMI in midlife. A significant interaction between the overall BMI PRS and UPF intake indicated UPF intake further amplified the relationship of genetics with BMI, although insights for specific genetic pathways were limited. Next, we will test gene–diet interactions for UPF categories on weight trajectories to inform precision nutrition strategies to optimize cardiovascular health at individual and population levels.
Ultra-processed Foods (UPFs) are associated with obesity, a key modifiable factor of poor cardiovascular health. Although genetics contributes to the risk of obesity, it is unknown whether the effect of UPF consumption on body mass index (BMI) is greater among individuals with underlying genetic susceptibility.
Hypothesis
We conducted gene-diet interaction analyses to assess whether the genetic risk of obesity increases the positive association between UPF consumption and BMI.
Methods
We conducted a cross-sectional analysis in the Women’s Genome Health Study among women of European ancestry with complete genetic data, available FFQ data, and BMI at baseline enrollment in 1992. We derived UPF intake (as % total energy), classifying foods and beverages by NOVA based on the nature, extent, and purpose of processing. BMI-related genotypes were captured by genome-wide (gwPRS) and pathway-specific (pPRSs) polygenic risk scores from GWAS statistics. The multivariable-adjusted linear regression models with effective independent test number and Sidak-corrected thresholds multiple testing adjustment were conducted to analyze continuous PRS and UPFs exposures with BMI as the outcome.
Results
Among 22,471 WGHS participants, the mean UPF intake was 29.4 (SD 10.7) % total energy and BMI was 25.9 (4.9) kg/m2. In main effects models, higher gwPRS and UPF intake were linearly associated with higher BMI. We observed a significant positive interaction between gwPRS and UPF intake on BMI, with each 1-SD higher UPF intake associated with 0.15 kg/m2 higher BMI per 1-SD higher gwPRS (95% CI 0.10–0.21, p<0.0001) (Table 1). Women with higher UPF intake had an incrementally higher BMI, and the magnitude of this linear association was larger among women with higher genetic risk of obesity (Figure 1). There were no significant pPRS and UPF intake interactions among individual KEGG legacy pathways.
Conclusions
In this large US cohort of women, women who consumed a greater proportion of energy from UPFs or had greater genetic susceptibility to obesity had a higher BMI in midlife. A significant interaction between the overall BMI PRS and UPF intake indicated UPF intake further amplified the relationship of genetics with BMI, although insights for specific genetic pathways were limited. Next, we will test gene–diet interactions for UPF categories on weight trajectories to inform precision nutrition strategies to optimize cardiovascular health at individual and population levels.
More abstracts on this topic:
A blood test based on RNA-seq and machine learning for the detection of steatotic liver disease: A Pilot Study on Cardiometabolic Health
Poggio Rosana, Berdiñas Ignacio, La Greca Alejandro, Luzzani Carlos, Miriuka Santiago, Rodriguez-granillo Gaston, De Lillo Florencia, Rubilar Bibiana, Hijazi Razan, Solari Claudia, Rodríguez Varela María Soledad, Mobbs Alan, Manchini Estefania
Adverse Childhood Experiences (ACEs) and Cardiovascular Health: Future of Families and Child Wellbeing Study (FFCWS)__PRESENT
Pedamallu Havisha, Van Horn Linda, Stein James, Korcarz Claudia, Hansen Kristin, Mitchell Colter, Heard-garris Nia, Lloyd-jones Donald, Allen Norrina, Gauen Abigail, Ning Hongyan, Wilkins John, Goldman Noreen, Notterman Daniel, Hou Lifang, Zheng Yinan, Marma Amanda