Final ID: 76
Consistency of Meeting Physical Activity Guidelines and Long-term Risk of Cardiovascular Disease
Abstract Body: Background
The long-term consistency of meeting physical activity guidelines may be critical for cardiovascular health, yet its independent contribution beyond total physical activity amount remains unclear.
Methods
A total of 225,264 adults from 3 large prospective cohorts (Health Professionals Follow-up Study, 1988-16; Nurses’ Health Study, 1988-2018; Nurses’ Health Study II, 1991-2017) were included. Leisure-time physical activity was assessed biennially using validated questionnaires and expressed in metabolic equivalent (MET)-hours per week. Consistency was defined as the percentage of follow-up years meeting the recommended level (≥7.5 MET-hours/week) and was updated at each questionnaire cycle across three decades of follow-up. Cox proportional hazards regression was used to estimate hazard ratios (HRs) and 95% confidence intervals (CIs) for incident cardiovascular disease (CVD), myocardial infarction (MI), and stroke.
Results
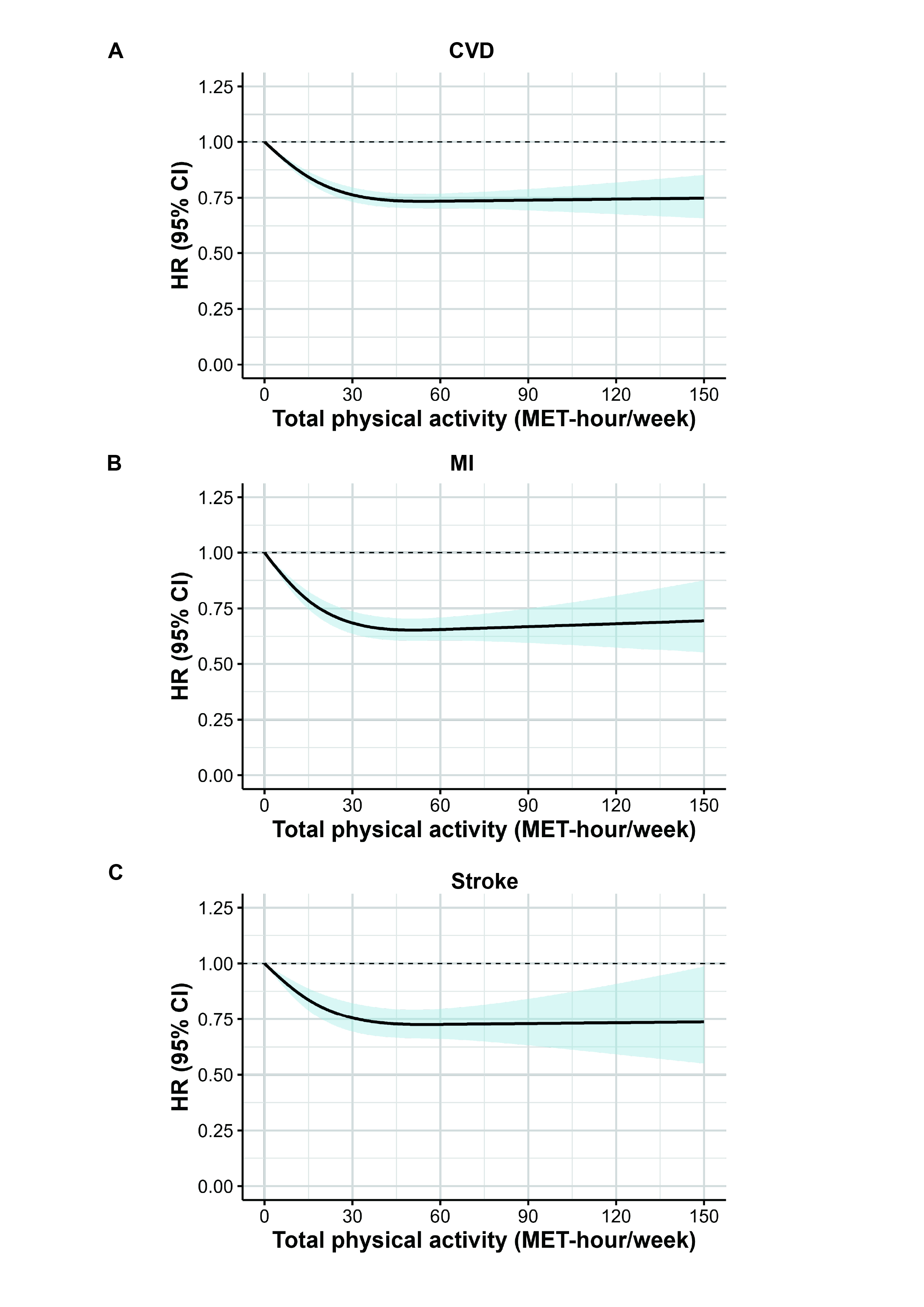
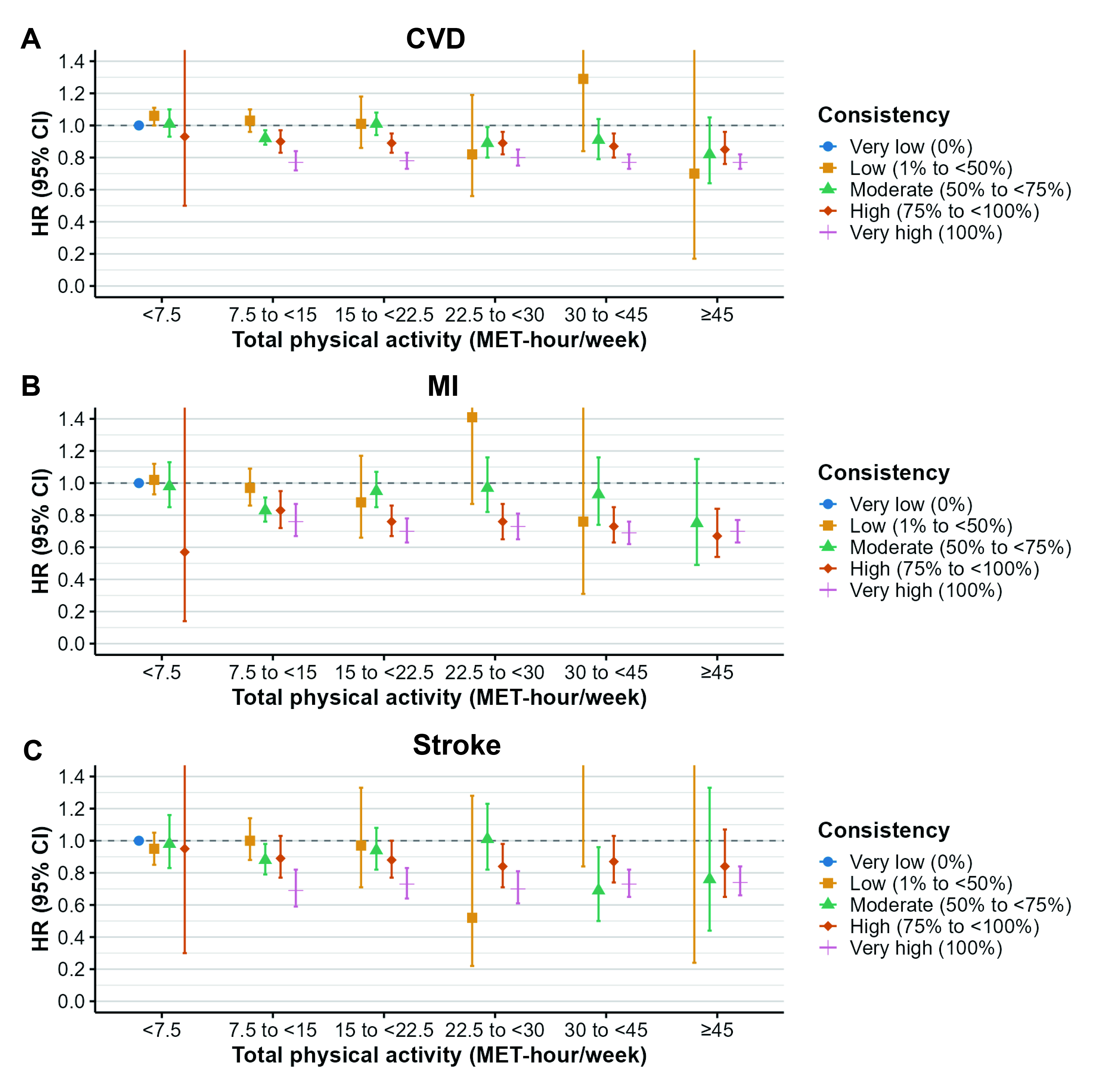
Over up to 30 years of follow-up, 24,766 CVD cases were documented. In traditional dose–response analyses, the lowest CVD risk was observed at 50.7 MET-hours/week (HR = 0.73; 95% CI, 0.70–0.77). After considering long-term consistency, consistently maintaining the guideline-recommended level at moderate intensity (median = 11.6 MET-hours/week) was associated with a 23% lower CVD risk (HR = 0.77; 95% CI, 0.72–0.84) compared with individuals with low activity (<7.5 MET-hours/week) and very low consistency. Consistently maintaining higher levels of physical activity was not associated with additional risk reduction (HRs [95% CIs]: 0.78 [0.73–0.83], 0.80 [0.75–0.85], 0.77 [0.73–0.82], and 0.77 [0.73–0.82] for median levels of 18.7, 26.0, 36.3, and 60.7 MET-hours/week, respectively). Similar associations were observed for MI and stroke and were consistent after adjustment for body mass index and across subgroups defined by age, gender, smoking status, and dietary quality.
Conclusions
Traditional dose-response analysis suggested that 50.7 MET-hours/week was needed for optimal mortality benefit. After incorporating long-term consistency, we found that maintaining a moderate level around 11.6 MET-hours/week over three decades was sufficient to achieve the optimal benefit in CVD risk reduction.
The long-term consistency of meeting physical activity guidelines may be critical for cardiovascular health, yet its independent contribution beyond total physical activity amount remains unclear.
Methods
A total of 225,264 adults from 3 large prospective cohorts (Health Professionals Follow-up Study, 1988-16; Nurses’ Health Study, 1988-2018; Nurses’ Health Study II, 1991-2017) were included. Leisure-time physical activity was assessed biennially using validated questionnaires and expressed in metabolic equivalent (MET)-hours per week. Consistency was defined as the percentage of follow-up years meeting the recommended level (≥7.5 MET-hours/week) and was updated at each questionnaire cycle across three decades of follow-up. Cox proportional hazards regression was used to estimate hazard ratios (HRs) and 95% confidence intervals (CIs) for incident cardiovascular disease (CVD), myocardial infarction (MI), and stroke.
Results
Over up to 30 years of follow-up, 24,766 CVD cases were documented. In traditional dose–response analyses, the lowest CVD risk was observed at 50.7 MET-hours/week (HR = 0.73; 95% CI, 0.70–0.77). After considering long-term consistency, consistently maintaining the guideline-recommended level at moderate intensity (median = 11.6 MET-hours/week) was associated with a 23% lower CVD risk (HR = 0.77; 95% CI, 0.72–0.84) compared with individuals with low activity (<7.5 MET-hours/week) and very low consistency. Consistently maintaining higher levels of physical activity was not associated with additional risk reduction (HRs [95% CIs]: 0.78 [0.73–0.83], 0.80 [0.75–0.85], 0.77 [0.73–0.82], and 0.77 [0.73–0.82] for median levels of 18.7, 26.0, 36.3, and 60.7 MET-hours/week, respectively). Similar associations were observed for MI and stroke and were consistent after adjustment for body mass index and across subgroups defined by age, gender, smoking status, and dietary quality.
Conclusions
Traditional dose-response analysis suggested that 50.7 MET-hours/week was needed for optimal mortality benefit. After incorporating long-term consistency, we found that maintaining a moderate level around 11.6 MET-hours/week over three decades was sufficient to achieve the optimal benefit in CVD risk reduction.
More abstracts on this topic:
Achieving Guidelines within a 24-Hour Movement Paradigm and Risk of Cardiovascular Disease and All-Cause Mortality in United States Adults
Boudreaux Benjamin, Xu Chang, Dooley Erin, Hornikel Bjoern, Munson Alexandra, Shechter Ari, Palta Priya, Gabriel Kelley, Diaz Keith
Accelerometer-derived physical activity, long-term exposure to ambient PM2.5 and risk of cardiovascular disease mortalityYuan Sheng, Lin Zhangyu, Song Yanjun, Dou Kefei