Final ID: TU125
Lessons Learned from Assessing Body Composition in 24-Month-Old Children Using Air Displacement Plethysmography
Abstract Body: Background: The pediatric option of BOD POD Body Composition System (COSMED USA) utilizes air displacement plethysmography to provide a fast, non-invasive assessment of body composition; however, its feasibility and operational challenges in young children are poorly documented. Understanding rates of and factors influencing successful measurement are essential for planning future studies.
Objective: To describe the feasibility of body composition assessment using the Bod Pod in 24-month-old children, comparing completers with non-completers, and summarizing lessons learned.
Methods: This descriptive study included 47 children (23–24 months; 42.6% girls). Parents consented to BOD POD assessment of their children, including a maximum of three trials assessing body volume. Assessment outcome was categorized as refusal, attempted test without a result (e.g., error message), or completed test with a computed result by the device. The technician recorded movement and crying/vocalization in each trial. Group comparisons used permutation t-tests and chi-squared tests. The coefficient of variation across repeated body volume measurements assessed device precision.
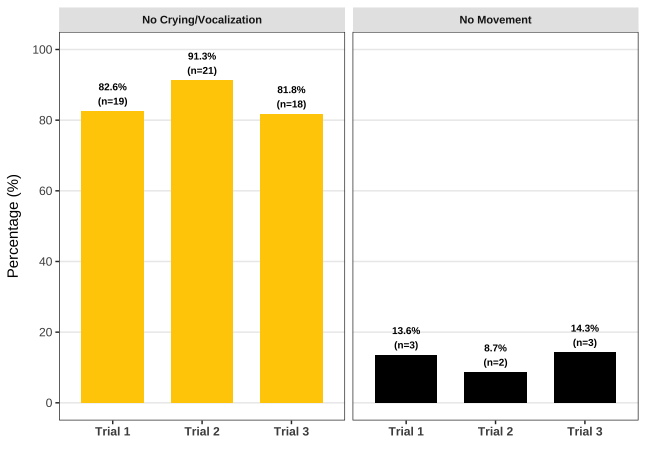
Results: Of the 47 children, 33 (70.2%) entered the chamber for at least one attempt, while 14 (29.8%) refused. Only 23 (48.9%) obtained a computed result; ten had invalid data due to insufficient trials (n=9) or error message (n=1). Completers had higher BMI-for-age z-score (difference, 0.45; 95% CI, 0.02–0.89) than non-completers. No other differences were observed between groups (Table). Most children remained quiet without crying/vocalization events (78.3–91.3% across trials), but movement was frequent, with only 13–26% remaining still in each trial (Figure). Despite this, device precision was high, with a low coefficient of variation across the body volume measurements (mean 0.3 ± 0.2%, range 0.1–0.7%).
Conclusion: Feasibility of BOD POD measurements in 24-month-olds was low, with only half completing tests with computed results. Refusal to enter and insufficient trials were the main barriers. Although most children did not cry/vocalize, movement was typical. For those who completed all trials, the method proved precise despite motion, though accuracy could not be assessed. Future studies could include familiarization strategies to enhance feasibility and should plan for larger sample sizes to account for non-participation.
Objective: To describe the feasibility of body composition assessment using the Bod Pod in 24-month-old children, comparing completers with non-completers, and summarizing lessons learned.
Methods: This descriptive study included 47 children (23–24 months; 42.6% girls). Parents consented to BOD POD assessment of their children, including a maximum of three trials assessing body volume. Assessment outcome was categorized as refusal, attempted test without a result (e.g., error message), or completed test with a computed result by the device. The technician recorded movement and crying/vocalization in each trial. Group comparisons used permutation t-tests and chi-squared tests. The coefficient of variation across repeated body volume measurements assessed device precision.
Results: Of the 47 children, 33 (70.2%) entered the chamber for at least one attempt, while 14 (29.8%) refused. Only 23 (48.9%) obtained a computed result; ten had invalid data due to insufficient trials (n=9) or error message (n=1). Completers had higher BMI-for-age z-score (difference, 0.45; 95% CI, 0.02–0.89) than non-completers. No other differences were observed between groups (Table). Most children remained quiet without crying/vocalization events (78.3–91.3% across trials), but movement was frequent, with only 13–26% remaining still in each trial (Figure). Despite this, device precision was high, with a low coefficient of variation across the body volume measurements (mean 0.3 ± 0.2%, range 0.1–0.7%).
Conclusion: Feasibility of BOD POD measurements in 24-month-olds was low, with only half completing tests with computed results. Refusal to enter and insufficient trials were the main barriers. Although most children did not cry/vocalize, movement was typical. For those who completed all trials, the method proved precise despite motion, though accuracy could not be assessed. Future studies could include familiarization strategies to enhance feasibility and should plan for larger sample sizes to account for non-participation.
More abstracts on this topic:
Improving School Food: A Novel Tool to Identify Priorities for Effective Policy Change in Nepal School Environments
Henry Megan, Shrestha Namuna, Pradhananga Priza, Ide Nicole, Curtis Christine, Lederer Ashley, Shrestha Archana, Benjamin-neelon Sara
Cardiovascular Health Among Youth with Neurodevelopmental Disability: Analysis of National Survey of Children's Health (NSCH) – 2021Baker-smith Carissa, Zhang Zugui, Robson Shannon, Patterson Freda, Brewer Benjamin, Tsai Jung Mei, Bhat Anjana