Final ID: 02
Systemic Inflammation and Traditional Cardiovascular-Kidney-Metabolic Risk Mediate the Association Between Social Determinants of Health and Incident Heart Failure: Insights from A Multi-Ethnic Cohort
Abstract Body: Background: Adverse social determinants of health (SDOH) are strongly associated with incident heart failure (HF), yet the associated biological mechanisms remain poorly defined. We examined whether systemic inflammation (hs-CRP) and traditional cardiovascular-kidney-metabolic (CKM) risk (AHA PREVENT HF risk score) mediate the relationship between SDOH and incident HF.
Methods: A validated 14-component composite SDOH index (scaled 0-100; 5 domains as per the WHO framework) was estimated among MESA cohort participants without HF at baseline. Sequential Cox regression and causal mediation analyses (using bootstrap confidence intervals) quantified the extent to which hs-CRP, AHA PREVENT HF risk score, CAC score, and hs-cTnT explained the association of SDOH index with adjudicated incident HF events over 15.3±5.7 years of follow-up (HRadj per 10-points: 1.08, 95% CI: 1.02-1.15; Fig 1). Indirect effects were estimated using non-parametric bootstrap resampling (5,000 replicates) with percentile-based 95% confidence intervals. Models controlled for race/ethnicity, subclinical atherosclerosis (CAC score), and myocardial injury (hs-cTnT).
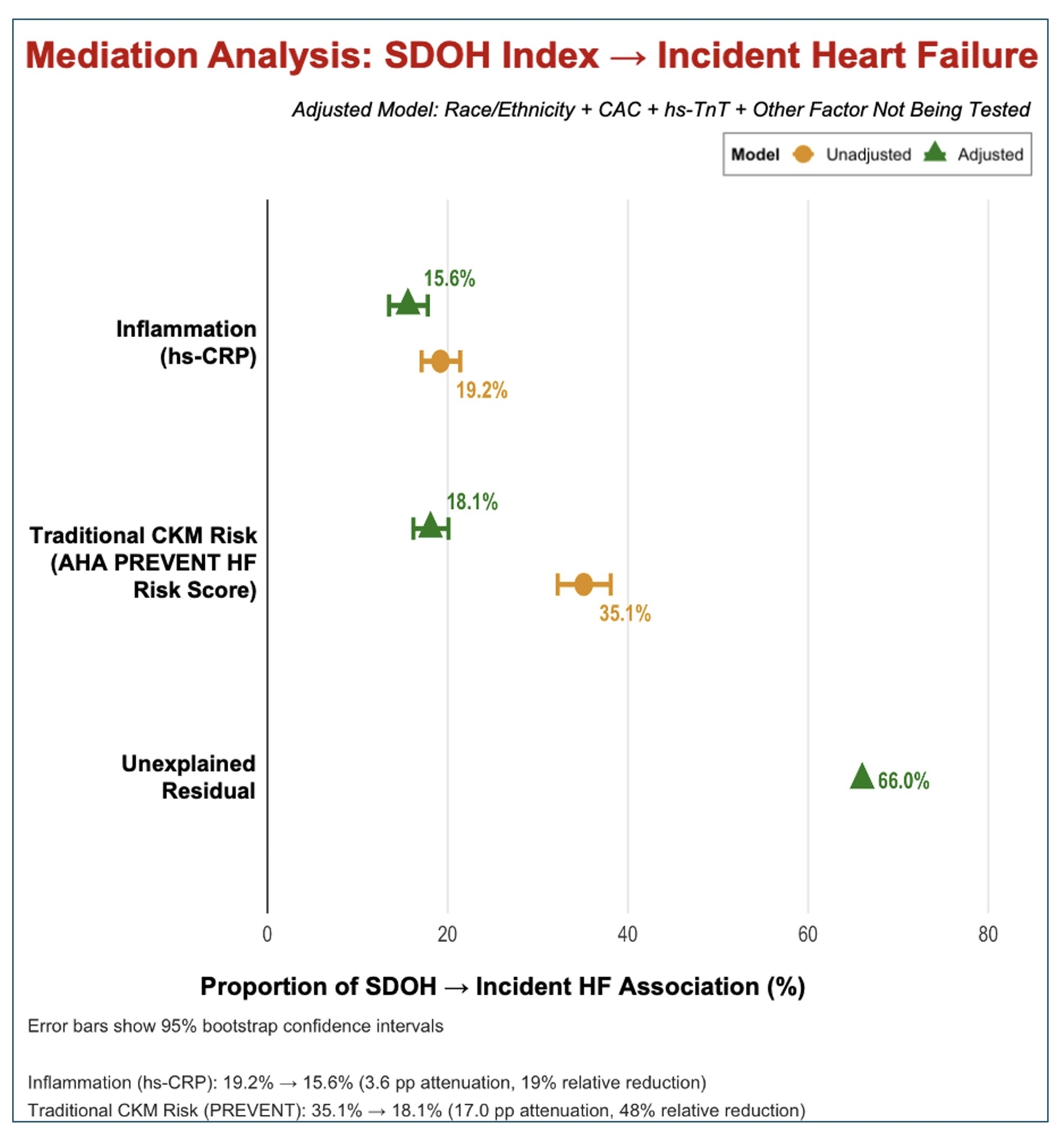
Results: Among participants (mean age 62±10 years; 52.8% women; 61.5% non-White), 462 developed HF. In fully adjusted models, systemic inflammation (hs-CRP) mediated 15.6% of the SDOH-HF association (indirect HR: 1.011, 95% CI: 1.006-1.018), demonstrating a robust inflammatory pathway linking social adversity to HF risk (unadjusted mediation: 19.2%). Traditional CKM risk (PREVENT score) mediated an additional 18.1% (indirect HR: 1.017, 95% CI: 1.012-1.024). Notably, CKM-mediated effects attenuated substantially from 35.1% in unadjusted models to 18.1% after adjusting for race and subclinical disease markers, suggesting confounding (Fig 2). Together, inflammation and traditional CKM risk explained approximately one-third of the SDOH-HF association, with substantial residual effects not yet examined (~66%), potentially attributable to genomic and exposomic pathways.
Conclusions: Adverse SDOH increase HF risk through both systemic inflammation and traditional CKM pathways, independent of subclinical atherosclerosis and myocardial injury. However, additional mediating pathways require further evaluation. These findings support inflammation as a key molecular interface through which SDOH shapes HF risk and emphasize targeting social–biological intersections to prevent HF in vulnerable populations.
Methods: A validated 14-component composite SDOH index (scaled 0-100; 5 domains as per the WHO framework) was estimated among MESA cohort participants without HF at baseline. Sequential Cox regression and causal mediation analyses (using bootstrap confidence intervals) quantified the extent to which hs-CRP, AHA PREVENT HF risk score, CAC score, and hs-cTnT explained the association of SDOH index with adjudicated incident HF events over 15.3±5.7 years of follow-up (HRadj per 10-points: 1.08, 95% CI: 1.02-1.15; Fig 1). Indirect effects were estimated using non-parametric bootstrap resampling (5,000 replicates) with percentile-based 95% confidence intervals. Models controlled for race/ethnicity, subclinical atherosclerosis (CAC score), and myocardial injury (hs-cTnT).
Results: Among participants (mean age 62±10 years; 52.8% women; 61.5% non-White), 462 developed HF. In fully adjusted models, systemic inflammation (hs-CRP) mediated 15.6% of the SDOH-HF association (indirect HR: 1.011, 95% CI: 1.006-1.018), demonstrating a robust inflammatory pathway linking social adversity to HF risk (unadjusted mediation: 19.2%). Traditional CKM risk (PREVENT score) mediated an additional 18.1% (indirect HR: 1.017, 95% CI: 1.012-1.024). Notably, CKM-mediated effects attenuated substantially from 35.1% in unadjusted models to 18.1% after adjusting for race and subclinical disease markers, suggesting confounding (Fig 2). Together, inflammation and traditional CKM risk explained approximately one-third of the SDOH-HF association, with substantial residual effects not yet examined (~66%), potentially attributable to genomic and exposomic pathways.
Conclusions: Adverse SDOH increase HF risk through both systemic inflammation and traditional CKM pathways, independent of subclinical atherosclerosis and myocardial injury. However, additional mediating pathways require further evaluation. These findings support inflammation as a key molecular interface through which SDOH shapes HF risk and emphasize targeting social–biological intersections to prevent HF in vulnerable populations.
More abstracts on this topic:
A Mast Cell-Specific Receptor Mediates Post-Stroke Brain Inflammation Via a Dural-Brain Axis
Kothari Ruchita, Caplan Justin, Gonzalez L. Fernando, Jackson Christopher, Bettegowda Chetan, Huang Judy, Koehler Raymond, Tamargo Rafael, Xu Risheng, Dong Xinzhong, Abdulrahim Mostafa, Oh Hyun Jong, Capuzzi Daniel, Nair Sumil, Zhang Yaowu, Limjunyawong Nathachit, Saini Sarbjit, Kim Jennifer
A machine learning approach to examining the associations of minority stressors and physical activity among sexual and gender minority adultsLopez Veneros David, Ensari Ipek, Bhilegaonkar Riya, Sharma Yashika, Caceres Billy