Final ID: TU252
Hospital-level Disparities and Long-term Survival in Patients With STEMI: Evidence from the China Acute Myocardial Infarction Registry
Abstract Body: Objective: We aimed to examine the association between hospital level and 5-year mortality among ST-segment elevation myocardial infarction (STEMI) patients in China, and identify factors explaining these differences.
Methods: We analyzed data from the China Acute Myocardial Infarction (CAMI) registry, which enrolled 12,697 STEMI patients from 108 hospitals across 31 provinces in mainland China between January 2013 and September 2014, with follow-up through January 1, 2020. Patients were categorized according to initial admission at provincial-, prefecture-, or county-level hospitals. The primary outcome was 5-year all-cause mortality. Kaplan–Meier estimates and multivariable Cox proportional hazards models were used to assess mortality risk across hospital levels, with competing risk models applied for cardiovascular deaths. Prespecified subgroup analyses evaluated effect modification by demographic and clinical factors. In addition, a multiple mediation framework was employed to quantify the contribution of patient characteristics and treatment differences to hospital-level disparities in long-term survival.
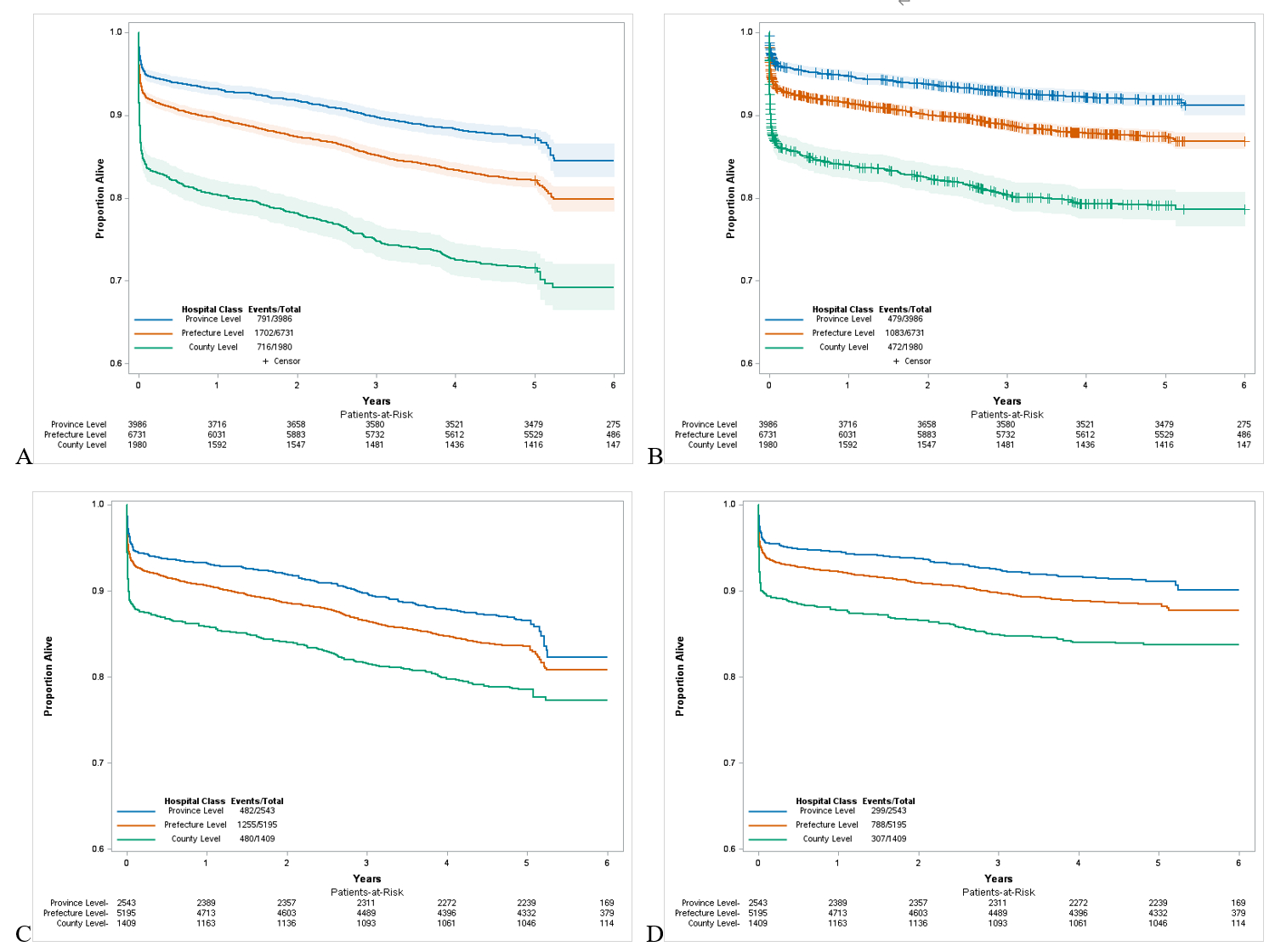
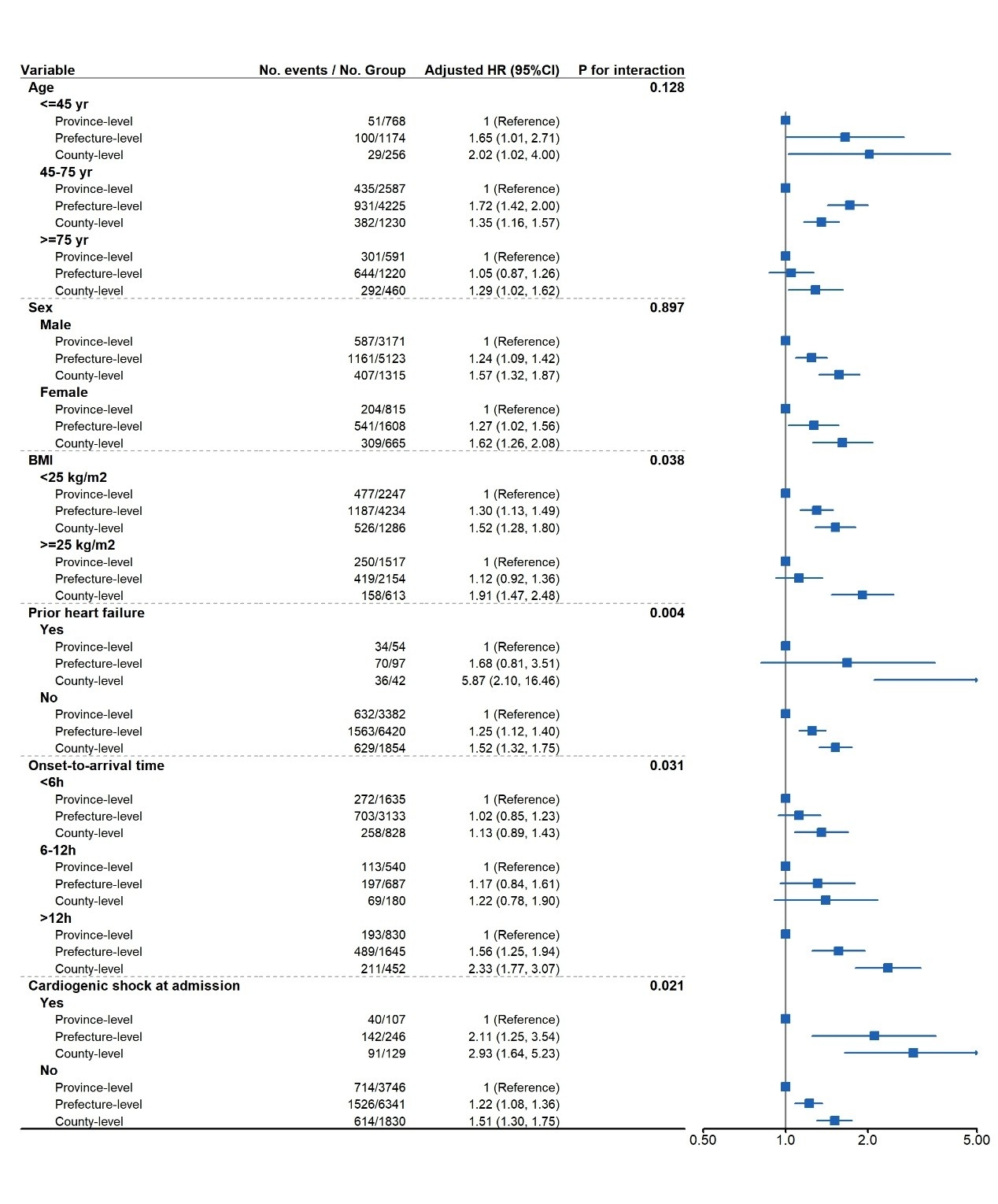
Results: Among 12,697 patients (mean age, 62.8 years; 75.7% male), the 5-year all-cause mortality was 19.8%, 25.3%, and 36.2% at provincial-level, prefecture-level, and county-level hospitals, respectively. After multi-variable adjustment, compared with patients treated at provincial-level hospitals, the adjusted HRs for all-cause mortality were 1.24 (95% CI, 1.11-1.39) at prefecture-level hospitals and 1.54 (95% CI, 1.34-1.78) at county-level hospitals (P for trend <.001). Similar trends were observed for cardiovascular mortality. Subgroup analyses indicated that the disparities were most pronounced among patients with overweight or obesity, history of prior heart failure, those with cardiogenic shock at admission, and those with onset-to-arrival time>12h. Mediation analysis suggested that primary PCI use, age, and socioeconomic factors contributed substantially to the observed differences in mortality.
Conclusions: In this nationwide cohort of STEMI patients, initial treatment at lower-level hospitals was associated with significantly higher long-term mortality. These findings highlight the need to improve access to timely, evidence-based care and to strengthen regional referral systems and treatment capacity at lower-tier hospitals to reduce outcome disparities.
Methods: We analyzed data from the China Acute Myocardial Infarction (CAMI) registry, which enrolled 12,697 STEMI patients from 108 hospitals across 31 provinces in mainland China between January 2013 and September 2014, with follow-up through January 1, 2020. Patients were categorized according to initial admission at provincial-, prefecture-, or county-level hospitals. The primary outcome was 5-year all-cause mortality. Kaplan–Meier estimates and multivariable Cox proportional hazards models were used to assess mortality risk across hospital levels, with competing risk models applied for cardiovascular deaths. Prespecified subgroup analyses evaluated effect modification by demographic and clinical factors. In addition, a multiple mediation framework was employed to quantify the contribution of patient characteristics and treatment differences to hospital-level disparities in long-term survival.
Results: Among 12,697 patients (mean age, 62.8 years; 75.7% male), the 5-year all-cause mortality was 19.8%, 25.3%, and 36.2% at provincial-level, prefecture-level, and county-level hospitals, respectively. After multi-variable adjustment, compared with patients treated at provincial-level hospitals, the adjusted HRs for all-cause mortality were 1.24 (95% CI, 1.11-1.39) at prefecture-level hospitals and 1.54 (95% CI, 1.34-1.78) at county-level hospitals (P for trend <.001). Similar trends were observed for cardiovascular mortality. Subgroup analyses indicated that the disparities were most pronounced among patients with overweight or obesity, history of prior heart failure, those with cardiogenic shock at admission, and those with onset-to-arrival time>12h. Mediation analysis suggested that primary PCI use, age, and socioeconomic factors contributed substantially to the observed differences in mortality.
Conclusions: In this nationwide cohort of STEMI patients, initial treatment at lower-level hospitals was associated with significantly higher long-term mortality. These findings highlight the need to improve access to timely, evidence-based care and to strengthen regional referral systems and treatment capacity at lower-tier hospitals to reduce outcome disparities.
More abstracts on this topic:
30-Day Outcomes of Dual vs Triple Antithrombotic Therapy After PCI
Meeks William, Slone Sarah, Barringhaus Kurt
Artificial Intelligence ECG-Extracted Features Predict Microvascular Obstruction in ST-segment Elevation Myocardial InfarctionTraverse Jay, Meyers Pendell, Sharkey Scott, Schwager Sarah, Stanberry Larissa, Herman Robert