Final ID: 62
Resolving Orthostatic Hypotension in the Hospital: A Retrospective Observational Study
Abstract Body: Introduction
Orthostatic hypotension (OH) is a common issue in the inpatient setting, often prompting multimodal intervention aimed at resolution. However, OH may be caused by a range of conditions, and the effectiveness of interventions may differ based on the etiology of OH.
Hypothesis
Causes and manifestations of OH among inpatients are heterogeneous, and the association of interventions with OH resolution will vary by strategy and etiology.
Method
This retrospective cohort study examined the electronic medical records (EMR) of patients who experienced OH during admission to Beth Israel Deaconess Medical Center between April 1, 2015, and June 30, 2021. Data were extracted via chart review by four reviewers. Logistic regression models, adjusted for age, sex, and race, were employed to explore associations between OH symptoms, etiologies, interventions and resolution. Resolution of OH was defined by improvement or resolution based on EMR documentation.
Results
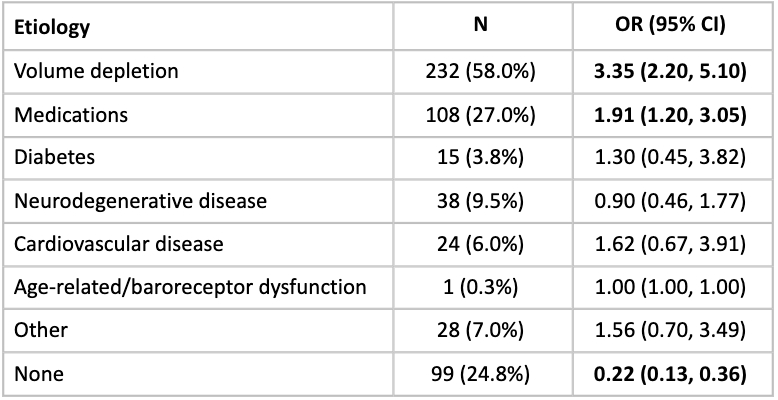
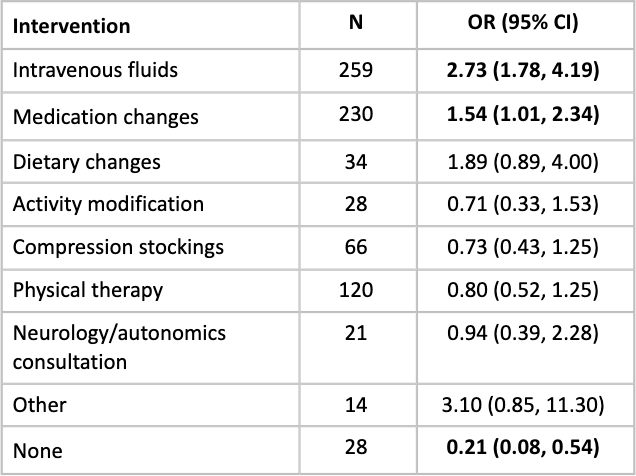
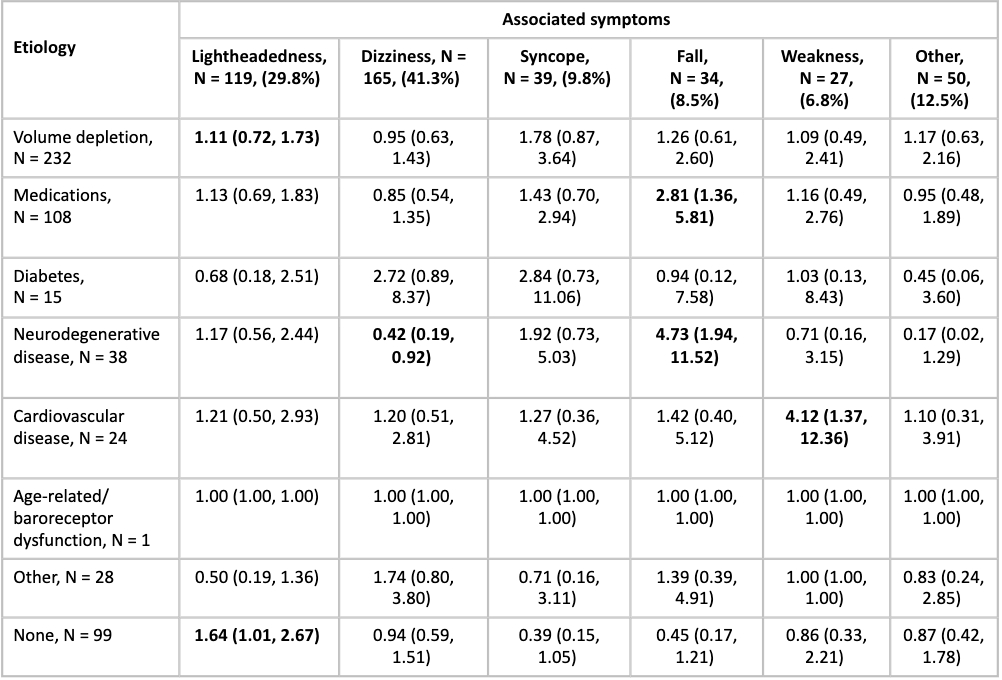
Among 400 patients (mean age: 69.9 years, 43.8% female, 10.5% Black), the most common etiology of OH was volume depletion (58%), followed by medications (27%); resolution of OH was more common in patients with these etiologies and less common in unknown etiologies (Table 1). Resolution of OH was more likely with intravenous fluids (OR: 2.73; 95% CI: 1.78, 4.19) or medication adjustments (OR: 1.54; 95% CI: 1.01, 2.34) and OH was less likely to resolve without intervention (OR: 0.21; 95% CI: 0.08, 0.54; Table 2). Neurogenic OH was inversely related to dizziness (OR: 0.42; 95% CI:0.19, 0.92) but strongly related to falls (OR: 4.73; 95% CI:1.94, 11.52; Table 3). Medication-related OH was also strongly associated with falls (OR: 4.73; 95% CI: 1.94, 11.52). Weakness was strongly related to cardiovascular etiology of OH (OR: 4.12; 95% CI: 1.37, 12.36).
Conclusions
In hospitalized patients, different types of OH were linked to distinct clinical presentations and outcomes. OH from volume depletion and from medication effects were more likely to resolve with targeted interventions—namely intravenous fluids and medication adjustments—whereas neurogenic and cardiovascular-related OH may reflect chronic disease rather than reversible causes. Accurate identification of OH etiology is important to guide inpatient management and set expectations for recovery.
Orthostatic hypotension (OH) is a common issue in the inpatient setting, often prompting multimodal intervention aimed at resolution. However, OH may be caused by a range of conditions, and the effectiveness of interventions may differ based on the etiology of OH.
Hypothesis
Causes and manifestations of OH among inpatients are heterogeneous, and the association of interventions with OH resolution will vary by strategy and etiology.
Method
This retrospective cohort study examined the electronic medical records (EMR) of patients who experienced OH during admission to Beth Israel Deaconess Medical Center between April 1, 2015, and June 30, 2021. Data were extracted via chart review by four reviewers. Logistic regression models, adjusted for age, sex, and race, were employed to explore associations between OH symptoms, etiologies, interventions and resolution. Resolution of OH was defined by improvement or resolution based on EMR documentation.
Results
Among 400 patients (mean age: 69.9 years, 43.8% female, 10.5% Black), the most common etiology of OH was volume depletion (58%), followed by medications (27%); resolution of OH was more common in patients with these etiologies and less common in unknown etiologies (Table 1). Resolution of OH was more likely with intravenous fluids (OR: 2.73; 95% CI: 1.78, 4.19) or medication adjustments (OR: 1.54; 95% CI: 1.01, 2.34) and OH was less likely to resolve without intervention (OR: 0.21; 95% CI: 0.08, 0.54; Table 2). Neurogenic OH was inversely related to dizziness (OR: 0.42; 95% CI:0.19, 0.92) but strongly related to falls (OR: 4.73; 95% CI:1.94, 11.52; Table 3). Medication-related OH was also strongly associated with falls (OR: 4.73; 95% CI: 1.94, 11.52). Weakness was strongly related to cardiovascular etiology of OH (OR: 4.12; 95% CI: 1.37, 12.36).
Conclusions
In hospitalized patients, different types of OH were linked to distinct clinical presentations and outcomes. OH from volume depletion and from medication effects were more likely to resolve with targeted interventions—namely intravenous fluids and medication adjustments—whereas neurogenic and cardiovascular-related OH may reflect chronic disease rather than reversible causes. Accurate identification of OH etiology is important to guide inpatient management and set expectations for recovery.
More abstracts on this topic:
A Blood(y) Pressure Crisis: Diffuse Alveolar Hemorrhage as a Rare Manifestation of Severely Uncontrolled Hypertension
Nandyal Shreyas, Amdetsion Gedion Yilma, Varma Revati, Kohli Saksham, Hammo Hasan
A Community Outreach Program Focused on Hypertension Awareness Reaches 600+ People in Rural Georgia and Works to Build the Next Generation of Biomedical ScientistsDent Elena, Ilatovskaya Daria, Pinkerton Brittany, Crider Emily, Ryan Michael, Sullivan Jennifer