Final ID: MPWE45
Proteomic-Based Biological Aging Clocks Are Associated with Cognitive Aging: The Atherosclerosis Risk in Community Study
Abstract Body: Background:
Proteomic aging clocks (PACs) reflect multifactorial biological aging and have shown strong associations with dementia risk. However, it remains unclear whether PACs can track cognitive aging trajectories among non-demented people. We examined associations between previously developed PACs and cognitive aging and also tested senescence-specific PACs (SASP-PACs), based on senescence-associated secretory phenotype (SASP) proteins, to assess their relevance compared with non-pathway-specific PACs.
Methods:
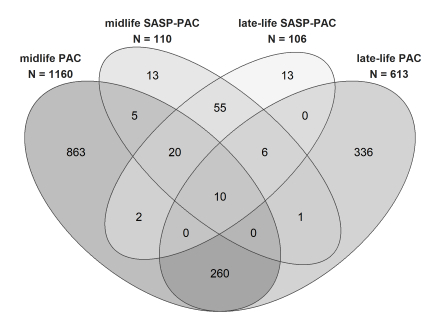
Participants from the Atherosclerosis Risk in Communities (ARIC) cohort, a U.S. population-based study, who remained dementia-free by 2022 were included in this analysis at two time points: midlife (Visit 2, 1990-92; N=3,510; mean age 54 y; 58% female, 17% Black) and late-life (Visit 5, 2011-13; N=3,745; mean age 75 y; 58% female, 17% Black). Non-pathway-specific PACs based on ~5,000 proteins measured by SomaScan were previously developed by training proteins against chronological age using elastic net regression and calculated as weighted sums (midlife: 1,160 and late-life: 613 proteins). SASP-PACs were created using the same method but included only SASP proteins (midlife:110 and late-life:106 proteins). The numbers of overlapping proteins are shown in Figure 1. Age acceleration (PAA for PACs and SASP-PAA for SASP-PACs) at each life stage was defined as the residual from regressing each PAC on chronological age. Cognitive aging from Visit 5 to 9 (2011–22) was defined as the percentage difference in an individual’s cognitive decline slope from the sample median, estimated using linear mixed models. To account for loss to follow-up, missing cognitive scores were imputed using multilevel joint modeling with predictors and auxiliary variables (e.g., mid-visit cognitive screening test scores). Associations between midlife and late-life PAA/SASP-PAA and cognitive aging were assessed using linear regression, adjusting for demographic and cardiovascular risk factors.
Results:
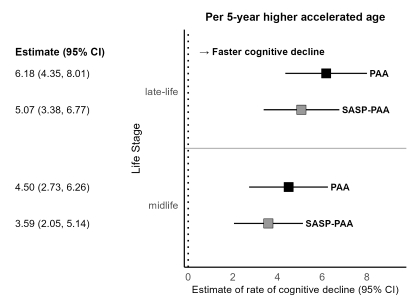
Each five-year increase in PAA was associated with a faster rate of cognitive decline relative to the sample median (β [95% CI]; midlife=4.50% [2.73%, 6.26%]; late-life=6.18% [4.35%, 8.01%]). SASP-PAA, despite using fewer proteins, showed comparable results (midlife=3.59% [2.05%, 5.14%]; late-life=5.07% [3.38%, 6.77%]) (Figure 2).
Conclusions:
PACs show potential to support monitoring of cognitive aging trajectories and early risk stratification for clinical cognitive impairment.
Proteomic aging clocks (PACs) reflect multifactorial biological aging and have shown strong associations with dementia risk. However, it remains unclear whether PACs can track cognitive aging trajectories among non-demented people. We examined associations between previously developed PACs and cognitive aging and also tested senescence-specific PACs (SASP-PACs), based on senescence-associated secretory phenotype (SASP) proteins, to assess their relevance compared with non-pathway-specific PACs.
Methods:
Participants from the Atherosclerosis Risk in Communities (ARIC) cohort, a U.S. population-based study, who remained dementia-free by 2022 were included in this analysis at two time points: midlife (Visit 2, 1990-92; N=3,510; mean age 54 y; 58% female, 17% Black) and late-life (Visit 5, 2011-13; N=3,745; mean age 75 y; 58% female, 17% Black). Non-pathway-specific PACs based on ~5,000 proteins measured by SomaScan were previously developed by training proteins against chronological age using elastic net regression and calculated as weighted sums (midlife: 1,160 and late-life: 613 proteins). SASP-PACs were created using the same method but included only SASP proteins (midlife:110 and late-life:106 proteins). The numbers of overlapping proteins are shown in Figure 1. Age acceleration (PAA for PACs and SASP-PAA for SASP-PACs) at each life stage was defined as the residual from regressing each PAC on chronological age. Cognitive aging from Visit 5 to 9 (2011–22) was defined as the percentage difference in an individual’s cognitive decline slope from the sample median, estimated using linear mixed models. To account for loss to follow-up, missing cognitive scores were imputed using multilevel joint modeling with predictors and auxiliary variables (e.g., mid-visit cognitive screening test scores). Associations between midlife and late-life PAA/SASP-PAA and cognitive aging were assessed using linear regression, adjusting for demographic and cardiovascular risk factors.
Results:
Each five-year increase in PAA was associated with a faster rate of cognitive decline relative to the sample median (β [95% CI]; midlife=4.50% [2.73%, 6.26%]; late-life=6.18% [4.35%, 8.01%]). SASP-PAA, despite using fewer proteins, showed comparable results (midlife=3.59% [2.05%, 5.14%]; late-life=5.07% [3.38%, 6.77%]) (Figure 2).
Conclusions:
PACs show potential to support monitoring of cognitive aging trajectories and early risk stratification for clinical cognitive impairment.
More abstracts on this topic:
Association between adherence to the Dietary Approaches to Stop Hypertension and cognitive performance in individuals with and without diabetes: data from a large population-based study from Germany
Stuermer Paula, Leitzmann Michael, Nauck Matthias, Berger Klaus, Knueppel Sven, Wawro Nina, Weber Katharina, Lieb Wolfgang, Oevermoehle Cara, Strathmann Eike, Jaber Max, Schlesinger Sabrina, Noethlings Ute, Linseisen Jakob, Schulze Matthias, Pischon Tobias
A PROtein Signature of PlatelEt Reactivity (PROSPER) Associated with Cardiovascular EventsHamo Carine, Muller Matthew, Luttrell-williams Elliot, Ruggles Kelly, Barrett Tessa, Berger Jeffrey