Final ID: TH954
High, even more than low, ankle-brachial index (ABI) associated with elevated risk of incident cardiovascular disease and all-cause mortality: The Hispanic Community Health Study/Study of Latinos (HCHS/SOL).
Abstract Body: Background: Low and high ankle-brachial index (ABI) values are associated with increased cardiovascular disease (CVD) risk, yet their prognostic value in Hispanics/Latinos has not been specifically studied, despite having unique vascular risk factor profiles compared to other races/ethnicities.
Aim: We aimed to assess the prospective association of ABI with incident CVD and all-cause mortality in Hispanics/Latinos.
Methods: We analyzed data from 8,000 adults (mean age 56, years; range, 45–74 years, 56% female) from the Hispanic Community Health Study/Study of Latinos (HCHS/SOL). The ABI was calculated from relevant extremity systolic blood pressures obtained at baseline (2008–2011) and modeled both continuously (cubic splines) and categorically (≤0.90, 0.91–1.00, 1.01–1.10 1.11–1.20 [reference], 1.21–1.30, and >1.30). Incident fatal and nonfatal CVD events (myocardial infarction, stroke, or heart failure) and all-cause mortality were assessed through 2021. Hazard ratios (HRs) were estimated using Cox models adjusting for confounders. We also conducted subgroup analysis by age, sex, smoking, diabetes, systolic blood pressure and kidney function.
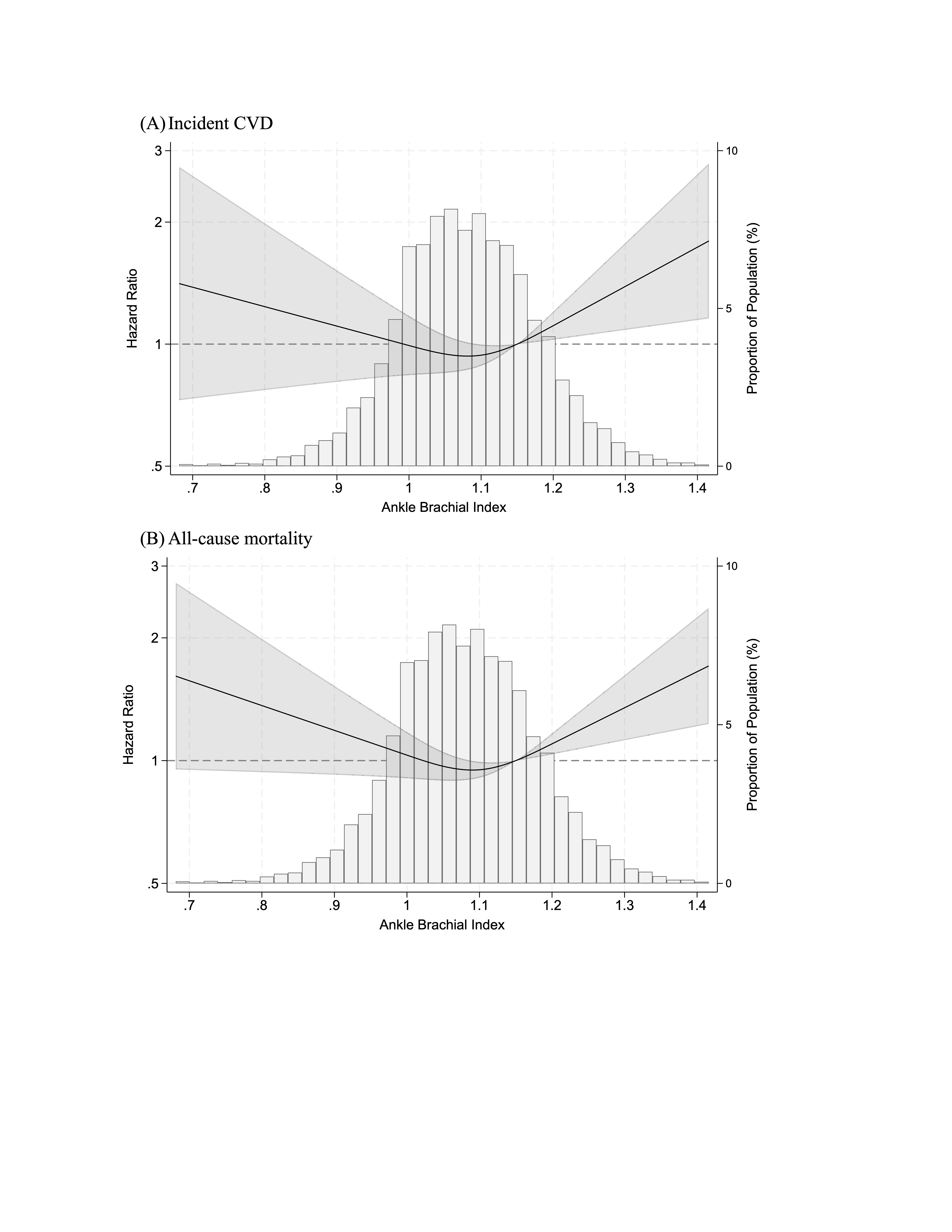
Results: Over a median follow-up of 11.6 years, there were 312 CVD events and 601 deaths. The average ABI was 1.08. High ABI (>1.30) vs. ABI 1.11–1.20 was significantly associated with an increased risk of incident CVD and all-cause mortality independently of potential confounders (HR 3.00, [95%CI: 1.40–6.44] and 2.70 [1.57–4.63], respectively). In contrast, low ABI (≤0.9) was significantly associated with all-cause mortality (HR 1.62 [1.04–2.54] but not with incident CVD. The results were largely similar when ABI was modeled continuously (Figure) with lowest risk at approximately ABI 1.10. The results were generally consistent across subgroups.
Conclusion: High ABI was more strongly associated with mortality and incident CVD than low ABI in this Hispanic/Latino cohort. These findings have implications for interpreting ABI in this underrepresented population.
Aim: We aimed to assess the prospective association of ABI with incident CVD and all-cause mortality in Hispanics/Latinos.
Methods: We analyzed data from 8,000 adults (mean age 56, years; range, 45–74 years, 56% female) from the Hispanic Community Health Study/Study of Latinos (HCHS/SOL). The ABI was calculated from relevant extremity systolic blood pressures obtained at baseline (2008–2011) and modeled both continuously (cubic splines) and categorically (≤0.90, 0.91–1.00, 1.01–1.10 1.11–1.20 [reference], 1.21–1.30, and >1.30). Incident fatal and nonfatal CVD events (myocardial infarction, stroke, or heart failure) and all-cause mortality were assessed through 2021. Hazard ratios (HRs) were estimated using Cox models adjusting for confounders. We also conducted subgroup analysis by age, sex, smoking, diabetes, systolic blood pressure and kidney function.
Results: Over a median follow-up of 11.6 years, there were 312 CVD events and 601 deaths. The average ABI was 1.08. High ABI (>1.30) vs. ABI 1.11–1.20 was significantly associated with an increased risk of incident CVD and all-cause mortality independently of potential confounders (HR 3.00, [95%CI: 1.40–6.44] and 2.70 [1.57–4.63], respectively). In contrast, low ABI (≤0.9) was significantly associated with all-cause mortality (HR 1.62 [1.04–2.54] but not with incident CVD. The results were largely similar when ABI was modeled continuously (Figure) with lowest risk at approximately ABI 1.10. The results were generally consistent across subgroups.
Conclusion: High ABI was more strongly associated with mortality and incident CVD than low ABI in this Hispanic/Latino cohort. These findings have implications for interpreting ABI in this underrepresented population.
More abstracts on this topic:
Achieving Guidelines within a 24-Hour Movement Paradigm and Risk of Cardiovascular Disease and All-Cause Mortality in United States Adults
Boudreaux Benjamin, Xu Chang, Dooley Erin, Hornikel Bjoern, Munson Alexandra, Shechter Ari, Palta Priya, Gabriel Kelley, Diaz Keith
Accelerometer-Measured Sedentary Behavior and Future Cardiovascular DiseaseAjufo Ezimamaka, Kany Shinwan, Ramo Joel, Churchill Timothy, Guseh James, Aragam Krishna, Ellinor Patrick, Khurshid Shaan