Final ID: MPTU14
Social Determinants of Health and Incident Heart Failure among Black and White Individuals: The REasons for Geographic And Racial Differences in Stroke Study
Abstract Body: Background:
Social determinants of health (SDOH), or the conditions in which people live, work, and play, profoundly impact cardiovascular outcomes. While SDOH often cluster within individuals, joint impact of specific SDOH on incident heart failure (HF) is unclear and may differ by race. We aimed to identify, rank, and test high-risk combinations of SDOH associated with incident HF among Black and White adults.
Methods:
We included REGARDS participants who were free of HF during second in-home visit in 2013–2016 and were followed through 2020 for adjudicated HF hospitalization or HF-related mortality. Using oblique random survival forests (ORSF) models, we estimated permutation-based variable importance to identify SDOH most predictive of incident HF, overall and by race. A classification and regression tree (CART) algorithm was used to form high-priority SDOH triads, and Cox models estimated hazard ratios (HR) for incident HF. Bootstrapping (1,000 iterations) generated robust, distribution-free 95% confidence intervals for HRs, capturing uncertainty from both sampling variation and the data-driven CART selection process.
Results:
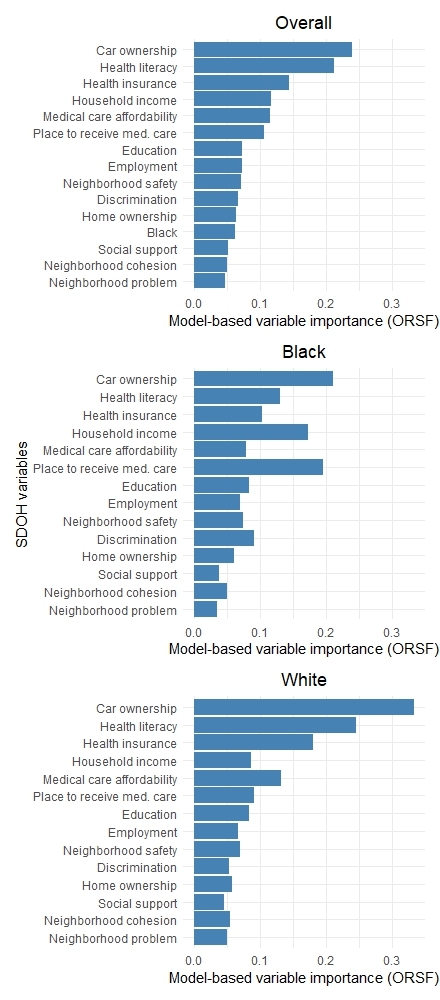
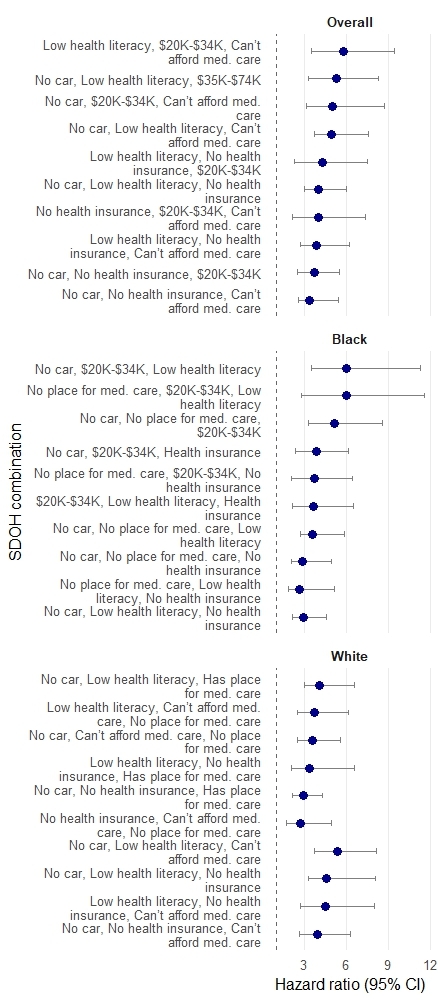
Among 13,042 participants (mean age 72.3 ± 9 years; 56% women; 36% Black), 486 had an incident HF event with a median follow-up of 5.9 years (IQR 4.7–6.5). Of 14 SDOH indicators considered, car ownership, health literacy, health insurance, household income, and ability to afford medical care were the strongest predictors of incident HF [Image 1]. Across high-priority triads, participants in the most adversely affected groups had markedly higher hazards of HF than the reference group [Image 2]. For example, compared with participants who owned a car, had adequate health literacy, and health insurance, those lacking all three had higher HF risk (HR 3.98; 95% CI 2.96–5.97). Among Black adults, the triad of no car, $20,000–$34,000 income, and limited health literacy conferred the highest risk (HR 6.00; 95% CI 3.46–11.24). Among White adults, the triad of no car, limited health literacy, and inability to afford medical care was most adverse (HR 5.37; 95% CI 3.71–8.10).
Conclusions:
Combinations of adverse SDOH, particularly transportation barriers, low health literacy, lack of insurance, lower income, and poor access to affordable care—were associated with substantially increased risk of incident HF. Patterns were consistent across racial groups, suggesting that addressing these access-to-care barriers may yield broad population benefits.
Social determinants of health (SDOH), or the conditions in which people live, work, and play, profoundly impact cardiovascular outcomes. While SDOH often cluster within individuals, joint impact of specific SDOH on incident heart failure (HF) is unclear and may differ by race. We aimed to identify, rank, and test high-risk combinations of SDOH associated with incident HF among Black and White adults.
Methods:
We included REGARDS participants who were free of HF during second in-home visit in 2013–2016 and were followed through 2020 for adjudicated HF hospitalization or HF-related mortality. Using oblique random survival forests (ORSF) models, we estimated permutation-based variable importance to identify SDOH most predictive of incident HF, overall and by race. A classification and regression tree (CART) algorithm was used to form high-priority SDOH triads, and Cox models estimated hazard ratios (HR) for incident HF. Bootstrapping (1,000 iterations) generated robust, distribution-free 95% confidence intervals for HRs, capturing uncertainty from both sampling variation and the data-driven CART selection process.
Results:
Among 13,042 participants (mean age 72.3 ± 9 years; 56% women; 36% Black), 486 had an incident HF event with a median follow-up of 5.9 years (IQR 4.7–6.5). Of 14 SDOH indicators considered, car ownership, health literacy, health insurance, household income, and ability to afford medical care were the strongest predictors of incident HF [Image 1]. Across high-priority triads, participants in the most adversely affected groups had markedly higher hazards of HF than the reference group [Image 2]. For example, compared with participants who owned a car, had adequate health literacy, and health insurance, those lacking all three had higher HF risk (HR 3.98; 95% CI 2.96–5.97). Among Black adults, the triad of no car, $20,000–$34,000 income, and limited health literacy conferred the highest risk (HR 6.00; 95% CI 3.46–11.24). Among White adults, the triad of no car, limited health literacy, and inability to afford medical care was most adverse (HR 5.37; 95% CI 3.71–8.10).
Conclusions:
Combinations of adverse SDOH, particularly transportation barriers, low health literacy, lack of insurance, lower income, and poor access to affordable care—were associated with substantially increased risk of incident HF. Patterns were consistent across racial groups, suggesting that addressing these access-to-care barriers may yield broad population benefits.
More abstracts on this topic:
A Comparison of English and Spanish AI Chatbot Responses to Online Cardiovascular Questions: Differences in Response Length, Readability, and Guidance
Benarroch Yoel, Gusdorf Jason, Isaza Nicolas, Rodman Adam
A Randomized Clinical Trial for Asymptomatic Elevated Blood Pressure in Patients Discharged from Emergency DepartmentPrendergast Heather, Khosla Shaveta, Kitsiou Spyros, Petzel Gimbar Renee, Freels Sally, Sanders Anissa, Daviglus Martha, Carter Barry, Del Rios Marina, Heinert Sara