Final ID: MPWE30
Sublingual Microvascular Features and Cognition in Midlife Among Women with a History of Vascular Injury in the Placenta
Abstract Body: Objective: Women with preeclampsia (PE) or placental evidence of maternal vascular malperfusion (MVM) have excess risk for cardiovascular and cerebrovascular disease years after delivery, perhaps related to microvascular dysfunction.
Methods: Women (n=176; mean age 43.4 y ±6; 34% Black) were enrolled in the Window Brain study, designed to disentangle the cognitive sequelae following PE vs MVM, ~ 15 years after delivery. PE and MVM were abstracted from the medical record. We related sublingual microvasculature features (GlycoCheck) to maternal self-report of cognition complaints (Everyday Cognition, eCog). Linear regression models related microvascular features (per z-score standard deviation (SD) increase) to higher cognitive complaints (eCog), adjusted for race and age, BMI and systolic BP at follow-up. Effect modification by MVM or PE history with microvascular features was evaluated and results stratified when p-interaction <0.1.
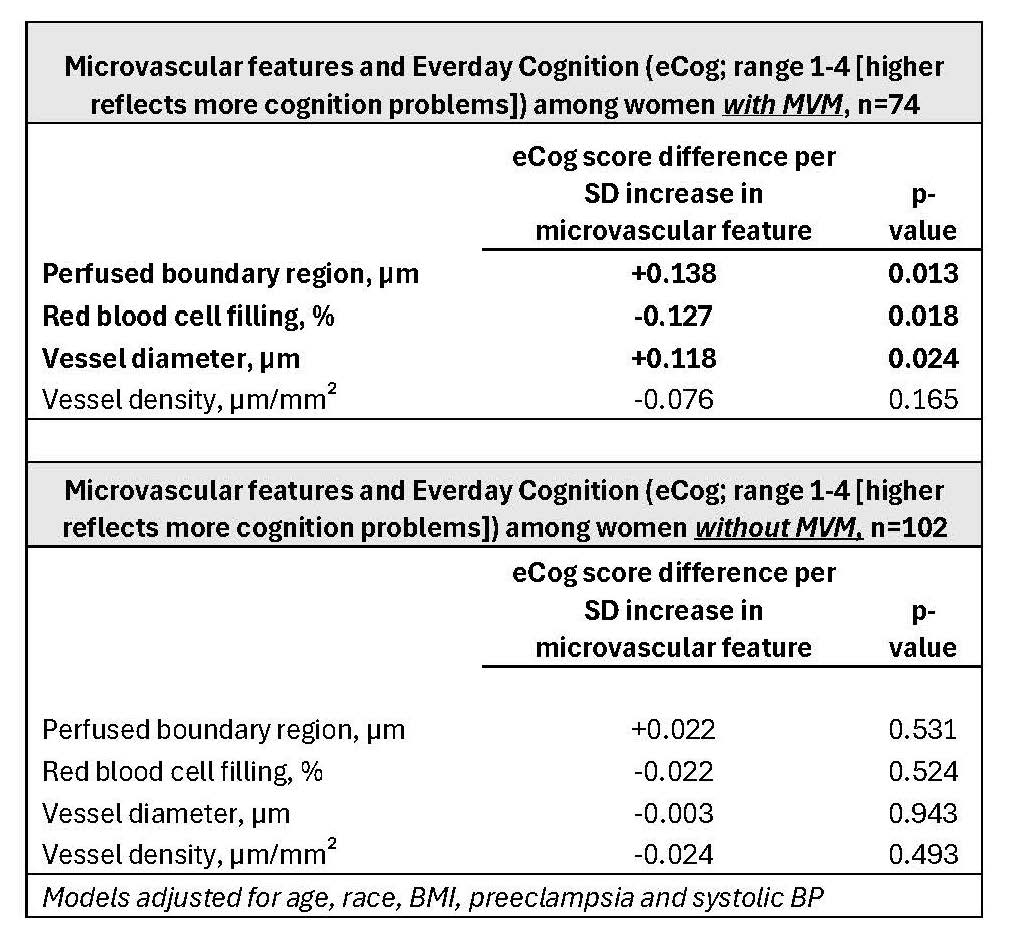
Results: A total of 52 women had prior PE, 74 had placental evidence of MVM, of whom 36 had +PE/+MVM. Overall, a larger perfused boundary region (PBR; marker of damaged or dysfunctional glycocalyx, the protective surface of the endothelium) was related to more cognitive complaints (+eCog score per SD increase, p=0.048). There was evidence of effect modification by MVM (p-interaction=0.09 for PBR) but not PE (p-interaction=0.66). In MVM-stratified models, among those with evidence of prior placental MVM, each SD increase in PBR and vessel diameter (damaged glycocalyx) was associated with more cognitive complaints. Related, each SD increase in red blood cell filling (healthier perfusion) was linked to fewer complaints (PBR, +0.138 eCog ± 0.05, p=0.015; Vessel diameter +0.118 eCog ±.05, p=0.024; RBC filling, -0.127 eCog± 0.05, p=0.018; TABLE). Microvascular features were unrelated to cognition among those without placental evidence of vascular injury; co-occurrence of PE did not influence estimates.
Conclusion: Our results indicate that small vessel damage in the placenta during pregnancy may be a marker of vascular susceptibility to impaired cognition at midlife, perhaps related to microvascular pathology. Interestingly, preeclampsia was not linked to cognition absent evidence of placental vascular injury, raising the possibility that the placenta may offer a more precise assessment of small vessel impairments and cognition.
Methods: Women (n=176; mean age 43.4 y ±6; 34% Black) were enrolled in the Window Brain study, designed to disentangle the cognitive sequelae following PE vs MVM, ~ 15 years after delivery. PE and MVM were abstracted from the medical record. We related sublingual microvasculature features (GlycoCheck) to maternal self-report of cognition complaints (Everyday Cognition, eCog). Linear regression models related microvascular features (per z-score standard deviation (SD) increase) to higher cognitive complaints (eCog), adjusted for race and age, BMI and systolic BP at follow-up. Effect modification by MVM or PE history with microvascular features was evaluated and results stratified when p-interaction <0.1.
Results: A total of 52 women had prior PE, 74 had placental evidence of MVM, of whom 36 had +PE/+MVM. Overall, a larger perfused boundary region (PBR; marker of damaged or dysfunctional glycocalyx, the protective surface of the endothelium) was related to more cognitive complaints (+eCog score per SD increase, p=0.048). There was evidence of effect modification by MVM (p-interaction=0.09 for PBR) but not PE (p-interaction=0.66). In MVM-stratified models, among those with evidence of prior placental MVM, each SD increase in PBR and vessel diameter (damaged glycocalyx) was associated with more cognitive complaints. Related, each SD increase in red blood cell filling (healthier perfusion) was linked to fewer complaints (PBR, +0.138 eCog ± 0.05, p=0.015; Vessel diameter +0.118 eCog ±.05, p=0.024; RBC filling, -0.127 eCog± 0.05, p=0.018; TABLE). Microvascular features were unrelated to cognition among those without placental evidence of vascular injury; co-occurrence of PE did not influence estimates.
Conclusion: Our results indicate that small vessel damage in the placenta during pregnancy may be a marker of vascular susceptibility to impaired cognition at midlife, perhaps related to microvascular pathology. Interestingly, preeclampsia was not linked to cognition absent evidence of placental vascular injury, raising the possibility that the placenta may offer a more precise assessment of small vessel impairments and cognition.
More abstracts on this topic:
Association Between Health Care Access and Cardiovascular Health Risk Among Reproductive-Aged Women in the SAFE HEART Study
Dankwa Kwabena, Vaidya Dhananjay, Ouyang Pamela, Hladek Melissa, Sharma Garima, Commodore-mensah Yvonne, Metlock Faith, Odei-kumi Kwabena, Ateh Stanislas Ketum, Rayani Asma, Baez Mateo Ana, Hernandez Lilian, Etelier Feodora, Ezuma Chioma
ACUTE ISCHEMIC STROKE IN YOUNG CANNABIS USERS: A NATIONWIDE ANALYSISJoseph Varughese Vivek, Anil Peethambar Gowri, Jayaraj Ranjini Nived, Mummadisetty Anvitha