Final ID: MPTU11
Prediabetes Progression In Young American Adults: A Pooling Project
Abstract Body: Introduction: There is growing clinical concern about increases in prediabetes and type 2 diabetes in young adults. Novel weight-loss medications, e.g., glucagon-like peptide-1-receptor agonist (GLP1-RA), can prevent progression from prediabetes to diabetes. Characterizing risk and risk factors for progression to diabetes could help identify high-risk subgroups to prioritize for intensive lifestyle interventions and novel medications in the growing population of young adults with prediabetes.
Objective: To characterize 5-year risk and risk factors for progression from prediabetes to diabetes in adults <40 years.
Methods: We pooled and harmonized data from participants aged 18 to 40 years with prediabetes (fasting glucose [FG] 100-125 mg/dL) from three cohorts (HCHS/SOL, CARDIA, FHS-Gen3). We used Poisson regression to estimate 5-year risk and age- and cohort-adjusted rate ratios (95%CI) for incident diabetes (FG ≥126 mg/dL or medication use), overall and according to demographics, FG categories (FG 100-109 mg/dL,110-125 mg/dL), and GLP1-RA eligibility criteria for weight loss (body mass index ≥30 kg/m2 or body mass index ≥27 kg/m2 with dyslipidemia or hypertension) during a median follow-up of 6.2 years.
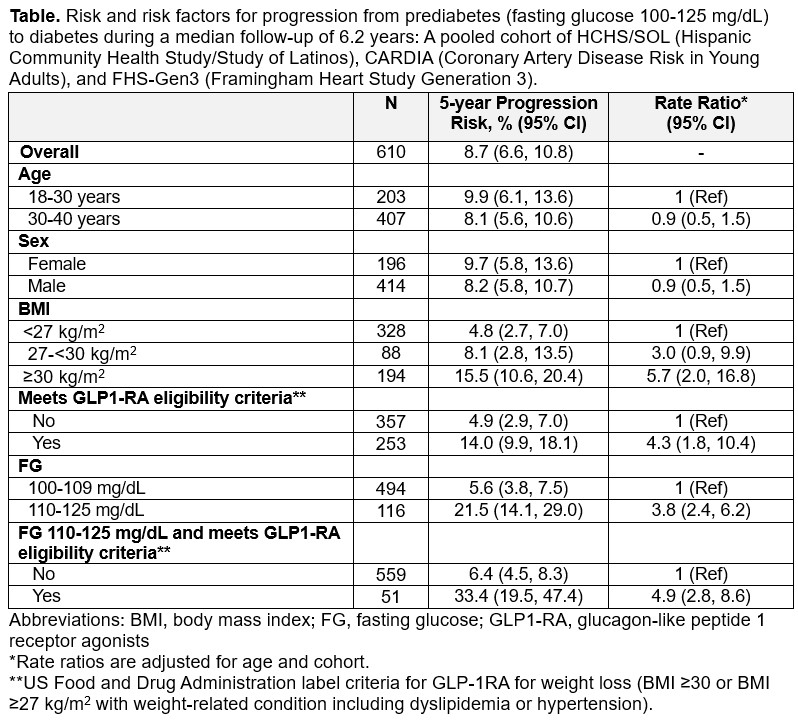
Results: The 610 young adults with prediabetes had a mean age of 32 (SD, 6) years, 32% were women, and 38% self-identified as Hispanic/Latino. The 5-year risk of progression from prediabetes to diabetes was 8.7% (95%CI: 6.6, 10.8) (Table). The 5-year risk of diabetes for young adults with prediabetes who met GLP-1RA eligibility criteria for weight loss was 14.0% (95% CI: 9.9, 18.1), and for those with FG between 110 to 125 mg/dL was 21.5% (95% CI: 14.1, 29.0). The 5-year risk of diabetes was highest for young adults who met GLP1-RA eligibility criteria and FG between 110 to 125 mg/dL (36.1%), which was ~5-times (95% CI: 2.8, 8.6) the risk for those meeting neither criteria.
Conclusion: In young adults with prediabetes, we identified subgroups with elevated risk of progression, with a 5-year diabetes risk of 33% in the highest risk group. This highlights opportunities for targeted approaches for intensive lifestyle and pharmacologic interventions for diabetes prevention.
Objective: To characterize 5-year risk and risk factors for progression from prediabetes to diabetes in adults <40 years.
Methods: We pooled and harmonized data from participants aged 18 to 40 years with prediabetes (fasting glucose [FG] 100-125 mg/dL) from three cohorts (HCHS/SOL, CARDIA, FHS-Gen3). We used Poisson regression to estimate 5-year risk and age- and cohort-adjusted rate ratios (95%CI) for incident diabetes (FG ≥126 mg/dL or medication use), overall and according to demographics, FG categories (FG 100-109 mg/dL,110-125 mg/dL), and GLP1-RA eligibility criteria for weight loss (body mass index ≥30 kg/m2 or body mass index ≥27 kg/m2 with dyslipidemia or hypertension) during a median follow-up of 6.2 years.
Results: The 610 young adults with prediabetes had a mean age of 32 (SD, 6) years, 32% were women, and 38% self-identified as Hispanic/Latino. The 5-year risk of progression from prediabetes to diabetes was 8.7% (95%CI: 6.6, 10.8) (Table). The 5-year risk of diabetes for young adults with prediabetes who met GLP-1RA eligibility criteria for weight loss was 14.0% (95% CI: 9.9, 18.1), and for those with FG between 110 to 125 mg/dL was 21.5% (95% CI: 14.1, 29.0). The 5-year risk of diabetes was highest for young adults who met GLP1-RA eligibility criteria and FG between 110 to 125 mg/dL (36.1%), which was ~5-times (95% CI: 2.8, 8.6) the risk for those meeting neither criteria.
Conclusion: In young adults with prediabetes, we identified subgroups with elevated risk of progression, with a 5-year diabetes risk of 33% in the highest risk group. This highlights opportunities for targeted approaches for intensive lifestyle and pharmacologic interventions for diabetes prevention.
More abstracts on this topic:
A Measure of Residential Segregation and Thrombo-inflammation in Black and White Americans
Manogaran Erin, Cushman Mary, Kamin Mukaz Debora, Sparks Andrew, Packer Ryan, Brochu Paige, Judd Suzanne, Howard Virginia, Plante Timothy, Long Leann, Cheung Katherine
3D Chromatin Architectures and Transcription Regulation in Diabetic Endothelial DysfunctionFeng Yuliang, Cai Liuyang, Wang Yigang, Huang Wei, Jiang Lei