Final ID: TU187
Serum Metabolomic Signature of the EAT-Lancet Diet and Incident Cardiovascular Disease and All-cause Mortality: Evidence from the Atherosclerosis Risk in Communities (ARIC) Study
Abstract Body: Backgroud
Greater adherence to the Planetary Health Diet Index (PHDI) is associated with lower risks of incident cardiovascular disease (CVD) and all-cause mortality; however, the underlying metabolic pathways remain to be elucidated.
Objective
We hypothesized that adherence to the PHDI would be reflected in serum metabolomic profiles that are associated with lower risks of incident CVD and all-cause mortality.
Methods
Analyses were conducted in two independent subgroups of participants (n1 = 1,594; n2 = 1,776) at Visit 1 (1987-1989) in the Atherosclerosis Risk in Communities study, each with available dietary and serum metabolomic data. The PHDI score (0-135) was derived from baseline 66-item food frequency questionnaires. Multivariable linear regression was used to identify metabolites associated with the PHDI score using a Bonferroni-corrected threshold. Associations between PHDI-related metabolites and the risk of incident CVD and all-cause mortality were examined using Cox proportional hazards models. Linear trends were assessed by including the quartile group as an ordinal variable in the Cox model. Results from the two subgroups were combined through meta-analysis.
Results
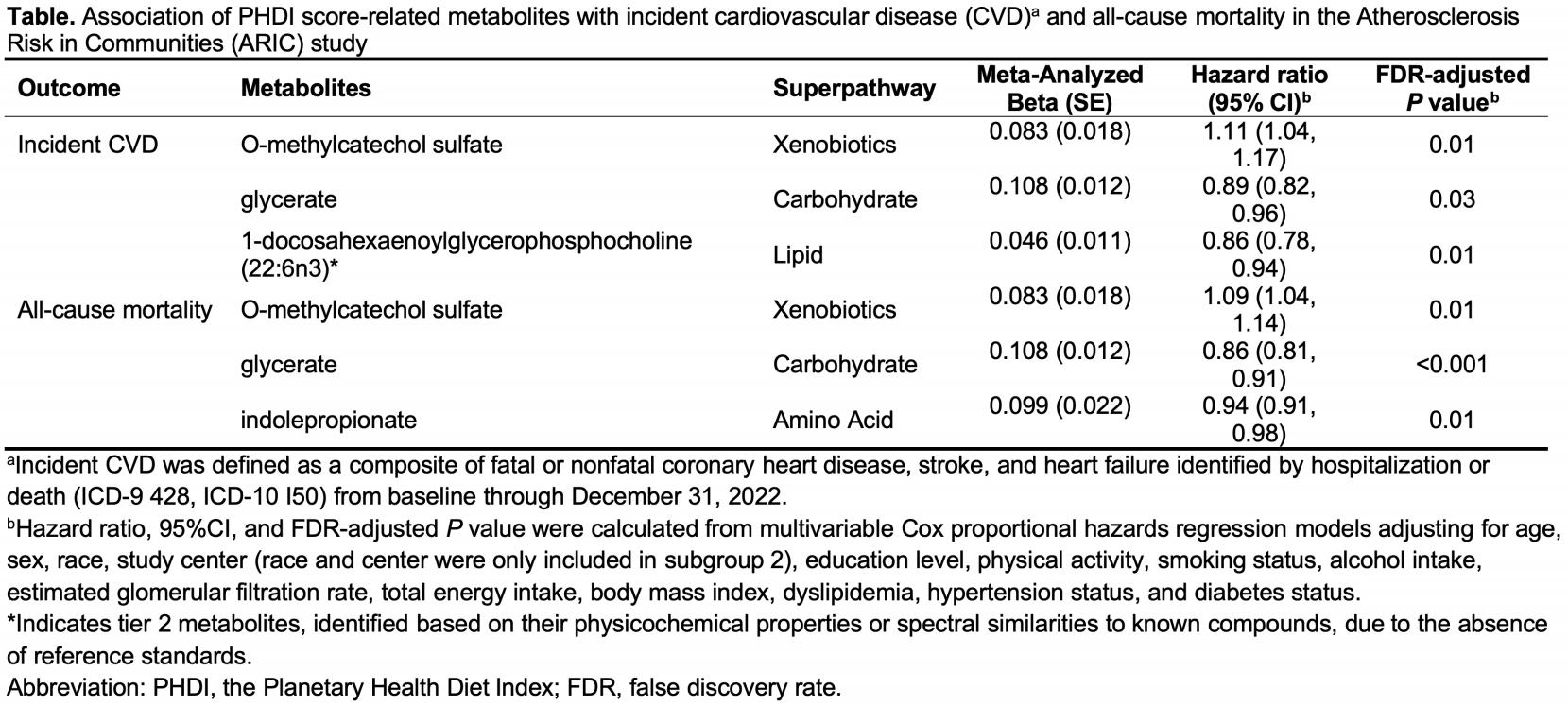
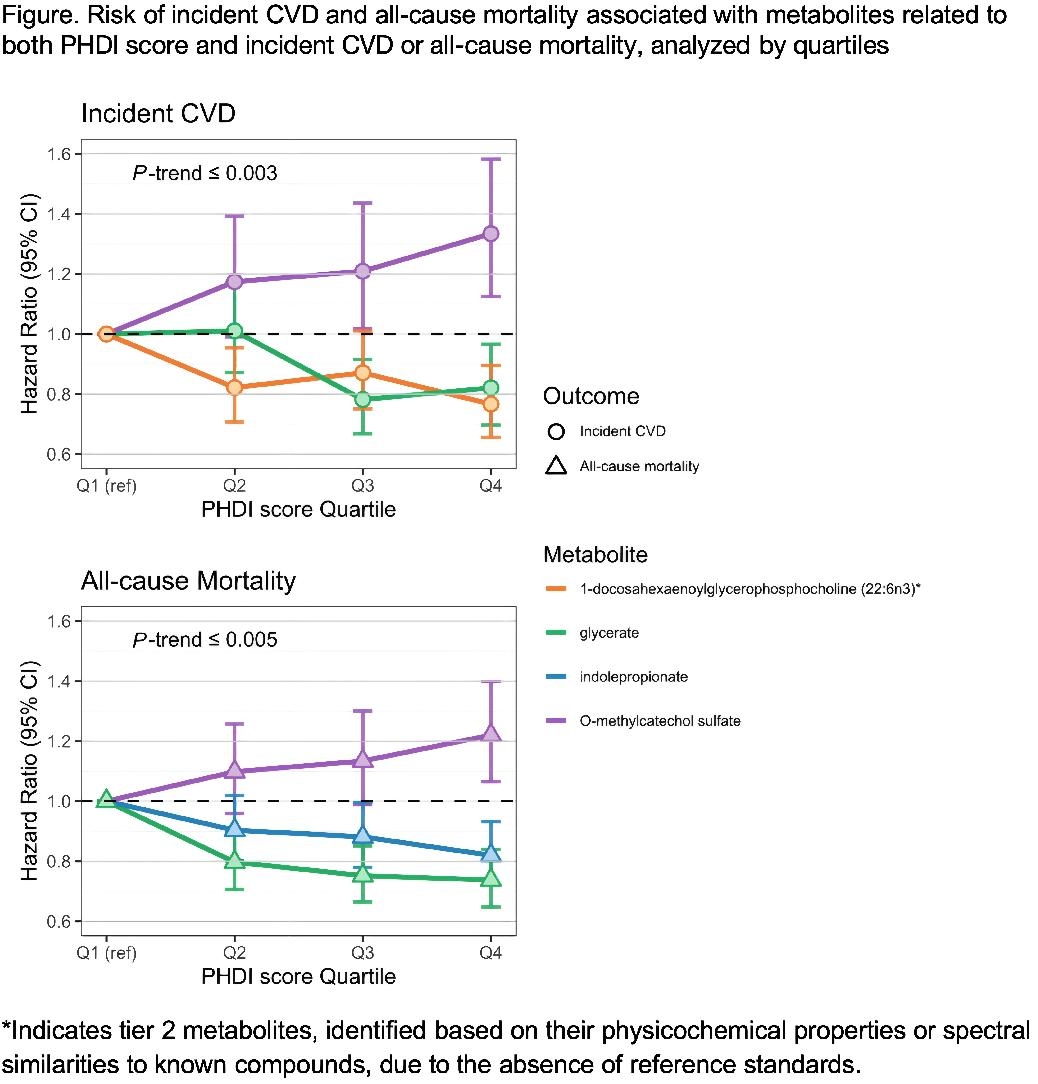
Over a median follow-up of 24 years for CVD and 29 years for mortality, 620 and 732 incident CVD cases and 930 and 1,158 deaths occurred in subgroups 1 and 2, respectively. We evaluated 359 metabolites, identified 29 associated with the PHDI score, and found that 4 of these were significantly related to incident CVD or all-cause mortality. Higher glycerate was linked to lower risks of both incident CVD and all-cause mortality, whereas higher indolepropionate were only associated with lower risk of all-cause mortality. Additionally, 1-docosahexaenoylglycerophosphocholine (22:6n3) was associated with lower CVD risk. O-methylcatechol sulfate was related to higher risks of both incident CVD and all-cause mortality (Table). All of the identified metabolites were positively associated with the PHDI score, and each showed clear dose-response relationships with either incident CVD or all-cause mortality (all FDR-adjusted P-trends ≤ 0.005) (Figure).
Conclusion
In this large community-based cohort of US adults, adherence to PHDI was reflected in distinct metabolic profiles linked to CVD and mortality risk. The identified metabolites implicate pathways related to carbohydrate, amino acid, lipid, and xenobiotic metabolism, providing mechanistic insight into the health benefits of EAT-Lancet diet.
Greater adherence to the Planetary Health Diet Index (PHDI) is associated with lower risks of incident cardiovascular disease (CVD) and all-cause mortality; however, the underlying metabolic pathways remain to be elucidated.
Objective
We hypothesized that adherence to the PHDI would be reflected in serum metabolomic profiles that are associated with lower risks of incident CVD and all-cause mortality.
Methods
Analyses were conducted in two independent subgroups of participants (n1 = 1,594; n2 = 1,776) at Visit 1 (1987-1989) in the Atherosclerosis Risk in Communities study, each with available dietary and serum metabolomic data. The PHDI score (0-135) was derived from baseline 66-item food frequency questionnaires. Multivariable linear regression was used to identify metabolites associated with the PHDI score using a Bonferroni-corrected threshold. Associations between PHDI-related metabolites and the risk of incident CVD and all-cause mortality were examined using Cox proportional hazards models. Linear trends were assessed by including the quartile group as an ordinal variable in the Cox model. Results from the two subgroups were combined through meta-analysis.
Results
Over a median follow-up of 24 years for CVD and 29 years for mortality, 620 and 732 incident CVD cases and 930 and 1,158 deaths occurred in subgroups 1 and 2, respectively. We evaluated 359 metabolites, identified 29 associated with the PHDI score, and found that 4 of these were significantly related to incident CVD or all-cause mortality. Higher glycerate was linked to lower risks of both incident CVD and all-cause mortality, whereas higher indolepropionate were only associated with lower risk of all-cause mortality. Additionally, 1-docosahexaenoylglycerophosphocholine (22:6n3) was associated with lower CVD risk. O-methylcatechol sulfate was related to higher risks of both incident CVD and all-cause mortality (Table). All of the identified metabolites were positively associated with the PHDI score, and each showed clear dose-response relationships with either incident CVD or all-cause mortality (all FDR-adjusted P-trends ≤ 0.005) (Figure).
Conclusion
In this large community-based cohort of US adults, adherence to PHDI was reflected in distinct metabolic profiles linked to CVD and mortality risk. The identified metabolites implicate pathways related to carbohydrate, amino acid, lipid, and xenobiotic metabolism, providing mechanistic insight into the health benefits of EAT-Lancet diet.
More abstracts on this topic:
Carbohydrate Quality and Cardiovascular Disease: Findings From the Women’s Health Initiative Prospective Cohort Study
Kavanagh Meaghan, Jenkins David, Liu Simin, Glenn Andrea, Yang Bo, Zurbau Andreea, Lo Kenneth, Van Horn Linda, Allison Matthew, Snetselaar Linda, Manson Joann, Sievenpiper John
A Multicentre Study for Hands Only CPR (HOCPR) training assessment towards building a ‘Nation of Life Savers” in IndiaRavikumar Thanjavur, Sarma Kvs, Ravikumar Thanjavur, Sarkar Manuj, Debnath Dhrubajyoti, Behera Priyamadhaba, Ghate Jayshri, Trikha Divay, Samantaray A, Madhavi K