Final ID: TU206
Multimorbidity and Obesity-related Associations with Variations in 24-hour Movement Cycles in Adults: The Dallas Heart and Minds 24-Hour Rest-Activity Cycle Study (DHS 24-REACT)
Abstract Body: Introduction: Multimorbidity (MM) increases healthcare costs and worsens quality of life. Obesity can further complicate care. The 24-h movement cycle (e.g., physical activity [PA] and sleep) is associated with health, but less is known about how MM and MM with obesity (MMxobesity) is related to differences in cycle composition.
Hypotheses: MM and obesity are independently associated with less PA and sleep compared to no chronic disease and MMxobesity would have stronger associations compared to either condition alone.
Methods: Data are from 1273 Dallas Heart & Minds participants (age 60.5±10.6 yrs; 59% women; 7% Asian; 45% Black; 13% Hispanic; 33% White) that wore an ActiGraph GT9X Link on the wrist for 24-h for 7 days between 2019-24. GGIR was used to process data using the sleep algorithm and Hildebrand cutpoints. Valid wear was ≤30 h in the wake-sleep window with ≥10 h waking and ≥1 to ≤17 h of sleep. MM included ≥2 conditions of reported: diabetes, hypertension, heart failure, transient ischemic attack, peripheral artery disease, kidney problems, hepatitis, cancer, Major Depressive Disorder, Seasonal Affective Disorder, or schizophrenia. Linear mixed effects models were used to examine differences in daily minutes of sleep, sedentary behavior (SED), light intensity PA (LIPA), and moderate to vigorous intensity PA (MVPA) by MM and obesity status controlling for covariates. An interaction term (MMxobesity) was included to assess whether the effect of MM on 24-h movement cycle components varied by weight status.
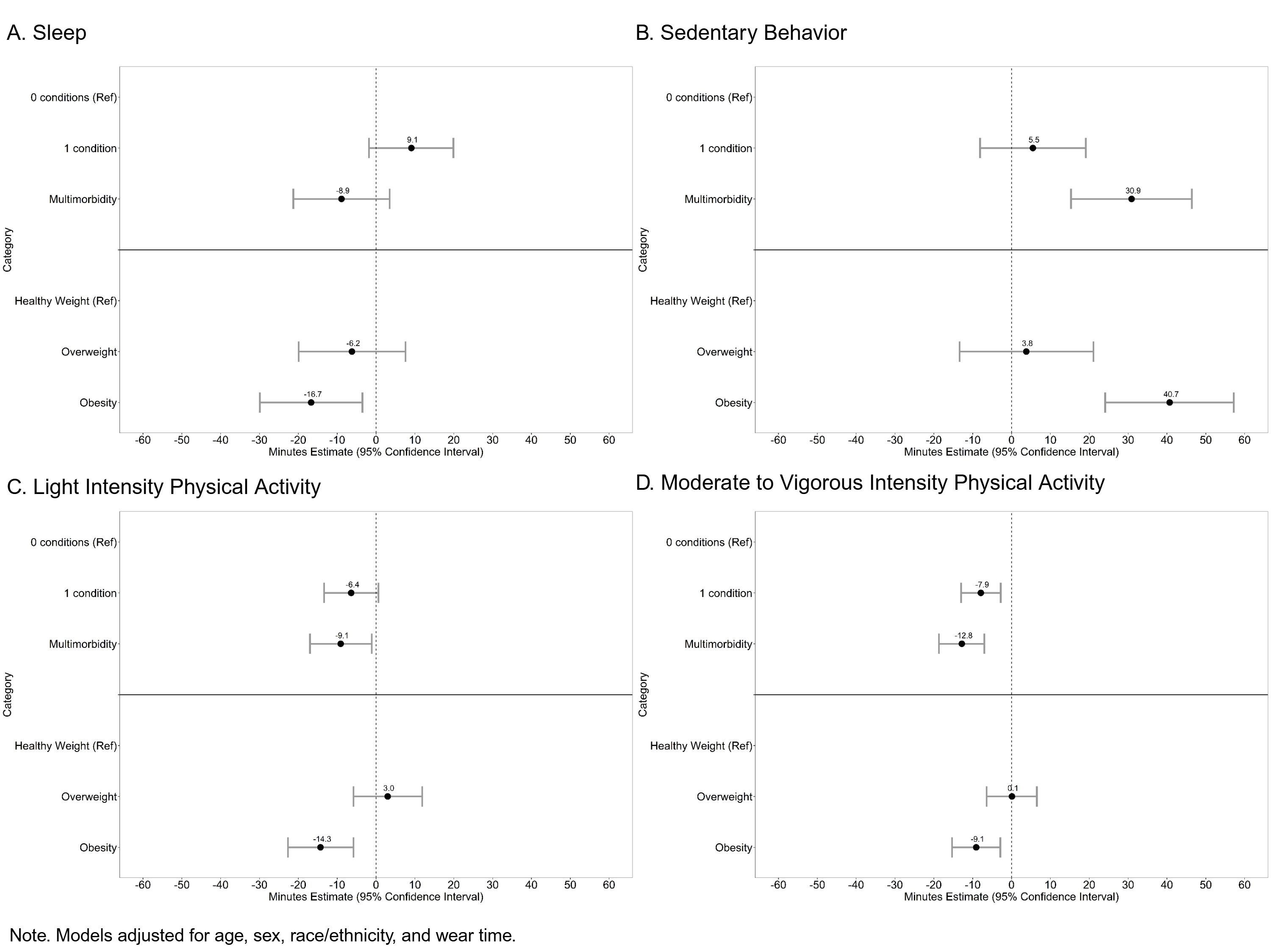
Results: On average (±SD), participants (28.4% had MM and 30.2% with obesity) spent 7.3±2.1 h in sleep, 13.1±2.5 h in SED, 2.5±1.1 h in LIPA, and 62.0±48.8 min in MVPA per day. For sleep (Fig. A), SED (Fig. B), LIPA (Fig. C) and MVPA (Fig. D), MM and obesity were both independently associated, however their combined effects (MMxobesity) did not modify the strength of these associations (all p > .05). Those with MM had had more minutes in SED (β: 30.9, 95% CI: 15.3, 46.4) to the expense of less LIPA (β: -9.1, 95% CI: -17.0, -1.1) and MVPA (β: -12.8, 95% CI: -18.7, -7.0). Those with obesity had more minutes in SED (β: 40.7, 95% CI: 24.1, 57.2) to the expense of less sleep (β: -16.7, 95% CI: -29.9, -3.5), LIPA (β: -14.3, 95% CI: -22.7, -5.8), and MVPA (β: -9.1, 95% CI: -15.3, -2.9).
Conclusions: Variations in the 24-h movement cycle across both MM and obesity highlight the importance of targeted interventions to combat inadequate movement profiles.
Hypotheses: MM and obesity are independently associated with less PA and sleep compared to no chronic disease and MMxobesity would have stronger associations compared to either condition alone.
Methods: Data are from 1273 Dallas Heart & Minds participants (age 60.5±10.6 yrs; 59% women; 7% Asian; 45% Black; 13% Hispanic; 33% White) that wore an ActiGraph GT9X Link on the wrist for 24-h for 7 days between 2019-24. GGIR was used to process data using the sleep algorithm and Hildebrand cutpoints. Valid wear was ≤30 h in the wake-sleep window with ≥10 h waking and ≥1 to ≤17 h of sleep. MM included ≥2 conditions of reported: diabetes, hypertension, heart failure, transient ischemic attack, peripheral artery disease, kidney problems, hepatitis, cancer, Major Depressive Disorder, Seasonal Affective Disorder, or schizophrenia. Linear mixed effects models were used to examine differences in daily minutes of sleep, sedentary behavior (SED), light intensity PA (LIPA), and moderate to vigorous intensity PA (MVPA) by MM and obesity status controlling for covariates. An interaction term (MMxobesity) was included to assess whether the effect of MM on 24-h movement cycle components varied by weight status.
Results: On average (±SD), participants (28.4% had MM and 30.2% with obesity) spent 7.3±2.1 h in sleep, 13.1±2.5 h in SED, 2.5±1.1 h in LIPA, and 62.0±48.8 min in MVPA per day. For sleep (Fig. A), SED (Fig. B), LIPA (Fig. C) and MVPA (Fig. D), MM and obesity were both independently associated, however their combined effects (MMxobesity) did not modify the strength of these associations (all p > .05). Those with MM had had more minutes in SED (β: 30.9, 95% CI: 15.3, 46.4) to the expense of less LIPA (β: -9.1, 95% CI: -17.0, -1.1) and MVPA (β: -12.8, 95% CI: -18.7, -7.0). Those with obesity had more minutes in SED (β: 40.7, 95% CI: 24.1, 57.2) to the expense of less sleep (β: -16.7, 95% CI: -29.9, -3.5), LIPA (β: -14.3, 95% CI: -22.7, -5.8), and MVPA (β: -9.1, 95% CI: -15.3, -2.9).
Conclusions: Variations in the 24-h movement cycle across both MM and obesity highlight the importance of targeted interventions to combat inadequate movement profiles.
More abstracts on this topic:
AI-Driven Gait Classification for Peripheral Artery Disease (PAD) Detection Using Machine Learning and Nonlinear Gait Dynamics
Mohammadzadeh Gonabadi Arash, Fallahtafti Farahnaz, Pipinos Iraklis, Burnfield Judith, Myers Sara
Association between Cardiometabolic Risk Factors and Future Multimorbidity Patterns: A K-means Clustering AnalysisOmoto Yuki, Miyagawa Naoko, Miyake Atsuko, Takebayashi Toru, Toki Ryota, Iba Chisato, Iida Miho, Edagawa Shun, Shibuki Takuma, Harada Sei, Hirata Aya, Matsumoto Minako