Final ID: MP07
Derivations of Supine and Standing Blood Pressure and Their Associations with Adverse Cardiovascular and Hypotension-Related Events
Abstract Body: Background: Postural drops in systolic blood pressure (SBP) are associated with cardiovascular and hypotension-related adverse events (falls, syncope). These associations are traditionally thought to be secondary to low standing blood pressure; however, the role of both high and low SBP in supine and standing positions has not been thoroughly characterized.
Objectives: To compare traditional and alternative derivations of supine and standing SBP with adverse cardiovascular and hypotension-related outcomes.
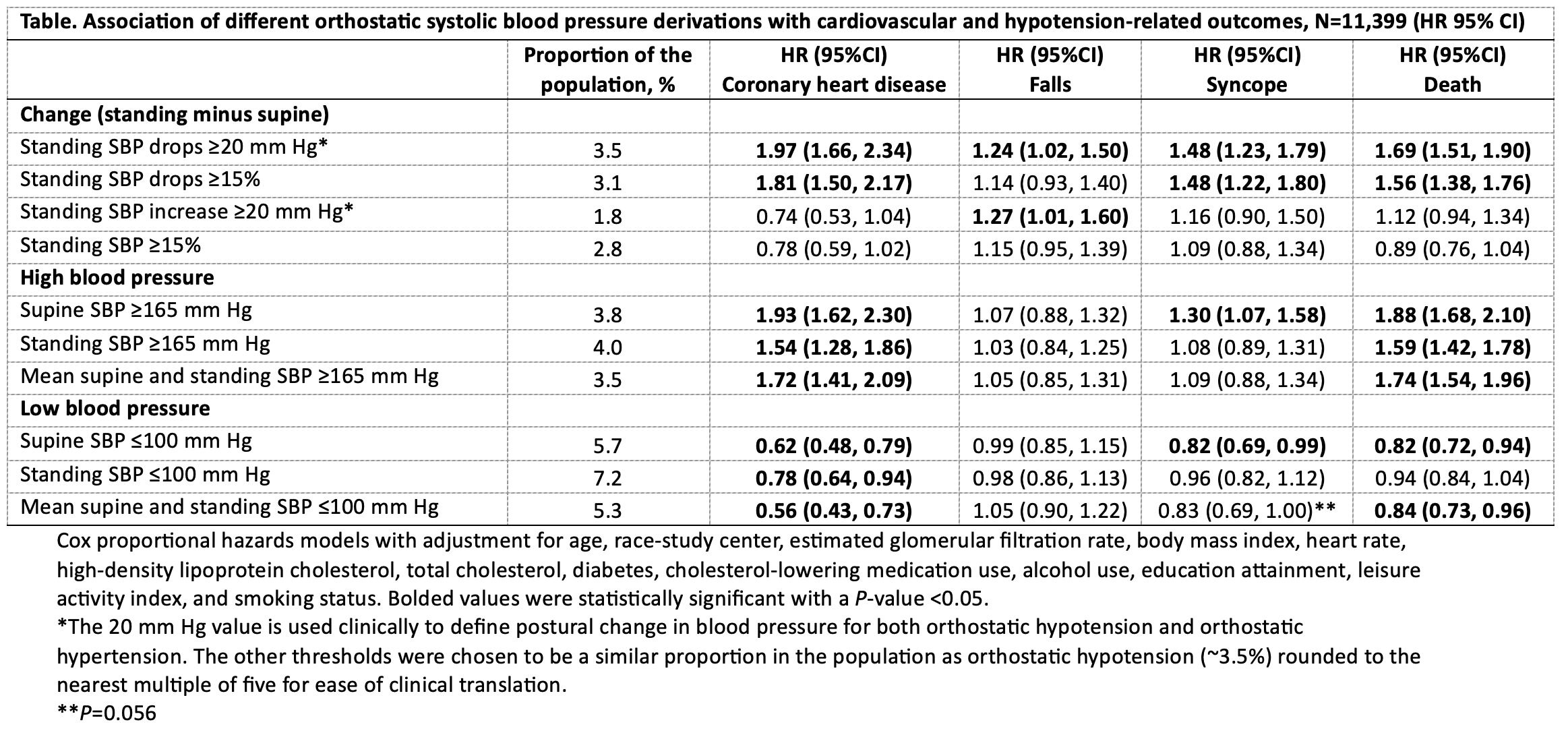
Methods: The Atherosclerosis Risk in Communities (ARIC) study measured supine and standing SBP in adult participants aged 45-64 between 1987–1989 and followed them for over 30 years. We examined low and high values (see Table) of supine SBP, standing SBP, absolute and relative differences in SBP after standing, and mean SBP between both positions in relation to adjudicated coronary heart disease (CHD) or all-cause mortality events as well as medical claims-based falls and syncope. We used Cox regression with adjustment for CVD risk factors. Cutpoints were chosen to match a population percentile approximating a 20 mm Hg difference between supine and standing SBP (the traditional definition for orthostatic hypotension).
Results: Among 11,399 participants (mean age 54 yr [SD, 5.7]; 56% female; 25% Black adults), relative or absolute drops in SBP were associated with CHD and mortality. Higher mean supine and standing BP was also associated with CHD (HR 1.72; 1.41, 2.09) and all-cause mortality (HR 1.74; 1.54, 1.96). An absolute decrease (HR 1.24; 1.02, 1.50) or increase (HR 1.27; 1.01, 1.60) in SBP was associated with falls. An absolute or relative decrease (both HRs 1.48) and higher supine SBP (HR 1.30; 1.07, 1.58) were associated with syncope. Lower supine SBP was inversely associated with CHD (HR 0.62) and all-cause mortality (HR 0.82). Lower standing SBP was also inversely associated with CHD (HR 0.78; 0.64, 0.94) but not with falls or syncope.
Conclusion: While both cardiovascular and hypotension-related outcomes were associated with postural drops in SBP, these outcomes were not consistently associated with low standing SBP. Rather, high supine SBP was associated with a greater risk of CHD, syncope, and death. Moreover, a rise in SBP with standing was associated with falls. These findings call attention to high SBP as a risk factor for both cardiovascular and hypotension-related outcomes and may have implications for treatment strategies if replicated.
Objectives: To compare traditional and alternative derivations of supine and standing SBP with adverse cardiovascular and hypotension-related outcomes.
Methods: The Atherosclerosis Risk in Communities (ARIC) study measured supine and standing SBP in adult participants aged 45-64 between 1987–1989 and followed them for over 30 years. We examined low and high values (see Table) of supine SBP, standing SBP, absolute and relative differences in SBP after standing, and mean SBP between both positions in relation to adjudicated coronary heart disease (CHD) or all-cause mortality events as well as medical claims-based falls and syncope. We used Cox regression with adjustment for CVD risk factors. Cutpoints were chosen to match a population percentile approximating a 20 mm Hg difference between supine and standing SBP (the traditional definition for orthostatic hypotension).
Results: Among 11,399 participants (mean age 54 yr [SD, 5.7]; 56% female; 25% Black adults), relative or absolute drops in SBP were associated with CHD and mortality. Higher mean supine and standing BP was also associated with CHD (HR 1.72; 1.41, 2.09) and all-cause mortality (HR 1.74; 1.54, 1.96). An absolute decrease (HR 1.24; 1.02, 1.50) or increase (HR 1.27; 1.01, 1.60) in SBP was associated with falls. An absolute or relative decrease (both HRs 1.48) and higher supine SBP (HR 1.30; 1.07, 1.58) were associated with syncope. Lower supine SBP was inversely associated with CHD (HR 0.62) and all-cause mortality (HR 0.82). Lower standing SBP was also inversely associated with CHD (HR 0.78; 0.64, 0.94) but not with falls or syncope.
Conclusion: While both cardiovascular and hypotension-related outcomes were associated with postural drops in SBP, these outcomes were not consistently associated with low standing SBP. Rather, high supine SBP was associated with a greater risk of CHD, syncope, and death. Moreover, a rise in SBP with standing was associated with falls. These findings call attention to high SBP as a risk factor for both cardiovascular and hypotension-related outcomes and may have implications for treatment strategies if replicated.
More abstracts on this topic:
Advanced maternal age and association with major adverse cardiovascular events from NHANES from 1999 to 2018
Mehta Adhya, Honigberg Michael, Kennedy Jamie, Spitz Jared, Sharma Garima, Agboola Olayinka, Satti Danish Iltaf, Harrington Colleen, Scott Nandita, Sarma Amy, Saad Antonio, Sullivan Scott, Epps Kelly
Absence of standard modifiable risk factors (SMuRF-less) among 5002 Middle Eastern patients with atherosclerotic cardiovascular disease: (Interim analysis from the Jo-SMuRF Study)Aldalal'ah Mo'men, Hammoudeh Ayman, Hamza Ibrahem, Alqudah Mohammad, Khasawneh Hasan, Alomari Sawsan, Alomari Ahmad, H. Assaf Sarah, Zaqqa Ayah, Khatatbeh Moawiah