Final ID: MP641
Widening Income-Based Disparities in Cardiovascular Mortality Among Working-Age US Adults 1999-2023
Abstract Body (Do not enter title and authors here): Background: After decades of progress, cardiovascular (CV) mortality among younger US adults is rising, but little is known about how these patterns vary by income.
Objective: To evaluate trends in cardiovascular mortality among working-age US adults by county-level income from 1999-2023.
Methods: We used American Community Survey data to assign US counties to quintiles by median household income (Q1: lowest; Q5: highest). Age-adjusted CV mortality rates (AAMRs) per 100,000 population in each quintile were obtained from CDC WONDER for adults age 25-64 using ICD codes I.00-99 as the primary cause of death. Annual percent changes (APCs) were determined for 1999-2009 and 2009-2019 using inverse variance-weighted log-linear regression models. Differential trends were assessed using interaction terms with Q1 and Q5 as reference groups. Given the short time period around the COVID-19 pandemic, absolute changes in AAMRs between 2019 and 2023 were calculated and compared using two-sample z-tests.
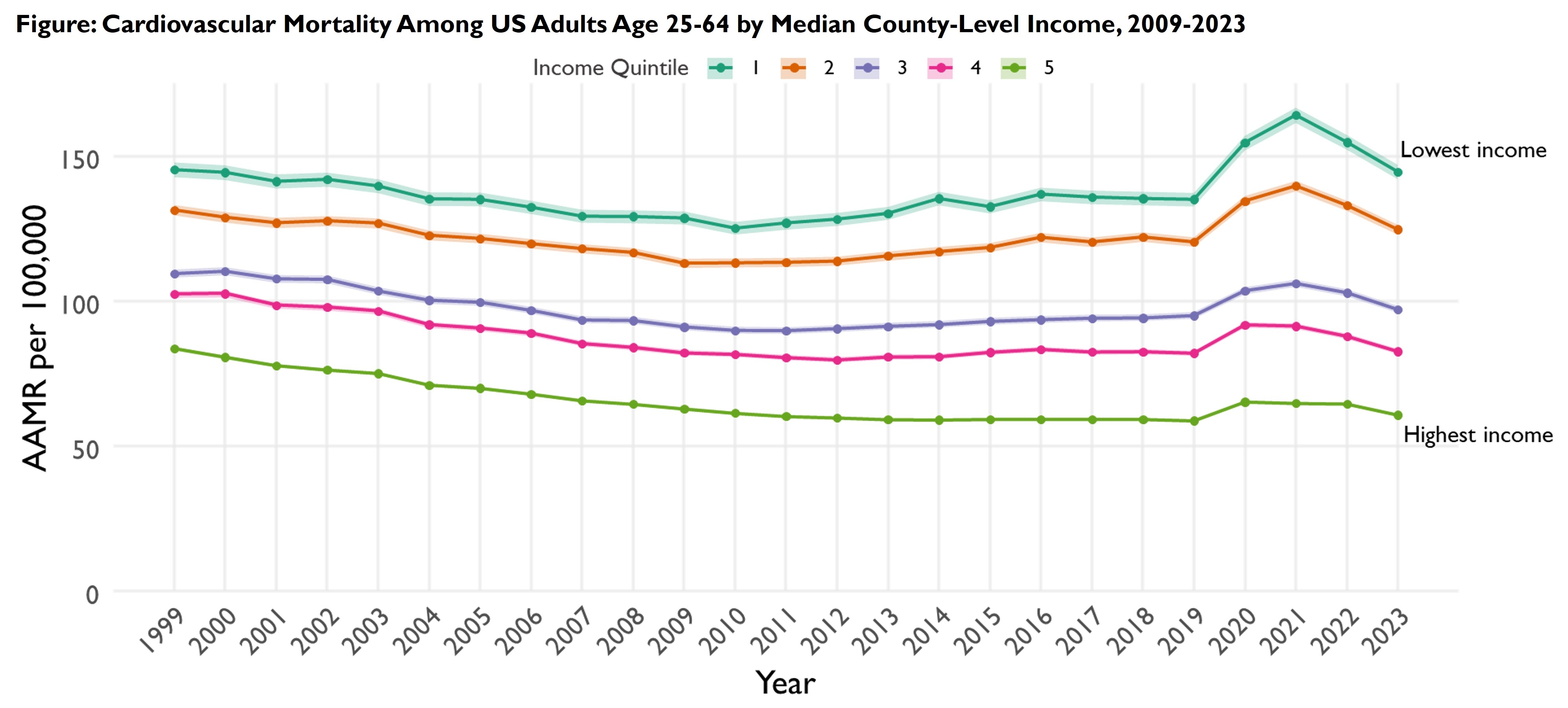
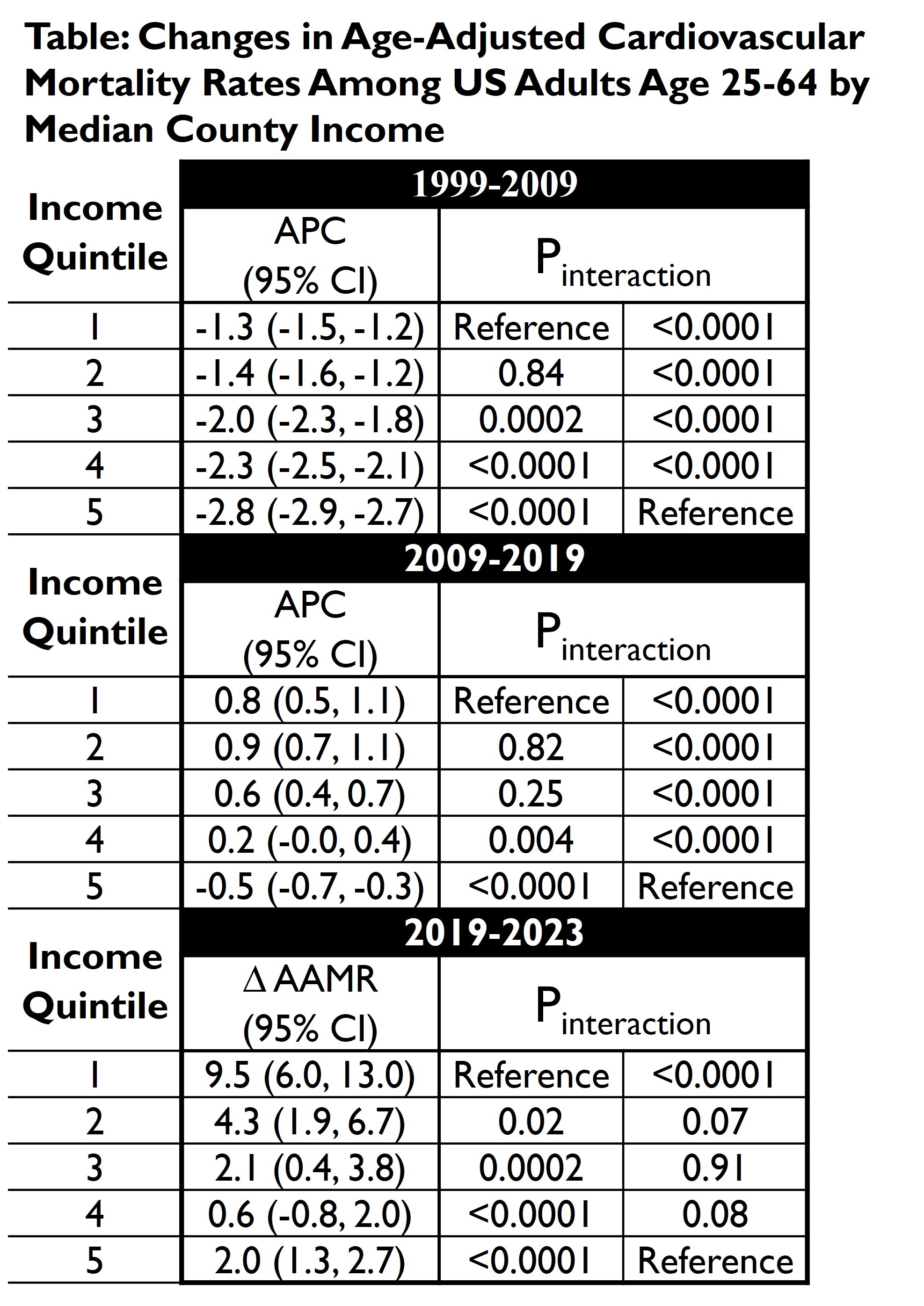
Results: From 1999-2023, cardiovascular mortality rates were consistently higher in lower-income counties (Figure). Between 1999-2009, CV mortality declined in all quintiles, but higher-income counties experienced a greater decline than lower-income counties (Q5 APC -2.8% [-2.9, -2.7] vs. Q1 APC -1.3% ([-1.5,-1.2]; p<0.0001). From 2009-2019, trends reversed and mortality increased for those in the lower income counties (Q1 APC +0.8% [0.5-1.1]; Q2 APC +0.9% [0.7-1.1];), whereas mortality continued to decline in the highest income counties (Q5: APC -0.5% [-0.7, -0.3]). From 2019-2023, CV mortality increased across all income quintiles, but increases were greatest in the lowest-income county (ΔAAMR +9.5 [6.0-13.0]) compared to all other income groups (p<0.05) (Table).
Conclusions: From 1999-2023, income-based disparities in cardiovascular (CV) mortality widened substantially among working-age U.S. adults. Although CV mortality declined across all income quintiles between 1999 and 2009, gains were more pronounced in higher-income counties. This progress stalled and reversed in 2009, with mortality rates rising among adults in the lowest-income counties while continuing to improve in the highest-income counties. From 2019 to 2023, CV mortality increased across all income groups, but the steepest rises occurred in the lowest-income quintiles. These findings highlight the urgent need to address rising CV mortality that is disproportionately impacting low-income, working-age adults.
Objective: To evaluate trends in cardiovascular mortality among working-age US adults by county-level income from 1999-2023.
Methods: We used American Community Survey data to assign US counties to quintiles by median household income (Q1: lowest; Q5: highest). Age-adjusted CV mortality rates (AAMRs) per 100,000 population in each quintile were obtained from CDC WONDER for adults age 25-64 using ICD codes I.00-99 as the primary cause of death. Annual percent changes (APCs) were determined for 1999-2009 and 2009-2019 using inverse variance-weighted log-linear regression models. Differential trends were assessed using interaction terms with Q1 and Q5 as reference groups. Given the short time period around the COVID-19 pandemic, absolute changes in AAMRs between 2019 and 2023 were calculated and compared using two-sample z-tests.
Results: From 1999-2023, cardiovascular mortality rates were consistently higher in lower-income counties (Figure). Between 1999-2009, CV mortality declined in all quintiles, but higher-income counties experienced a greater decline than lower-income counties (Q5 APC -2.8% [-2.9, -2.7] vs. Q1 APC -1.3% ([-1.5,-1.2]; p<0.0001). From 2009-2019, trends reversed and mortality increased for those in the lower income counties (Q1 APC +0.8% [0.5-1.1]; Q2 APC +0.9% [0.7-1.1];), whereas mortality continued to decline in the highest income counties (Q5: APC -0.5% [-0.7, -0.3]). From 2019-2023, CV mortality increased across all income quintiles, but increases were greatest in the lowest-income county (ΔAAMR +9.5 [6.0-13.0]) compared to all other income groups (p<0.05) (Table).
Conclusions: From 1999-2023, income-based disparities in cardiovascular (CV) mortality widened substantially among working-age U.S. adults. Although CV mortality declined across all income quintiles between 1999 and 2009, gains were more pronounced in higher-income counties. This progress stalled and reversed in 2009, with mortality rates rising among adults in the lowest-income counties while continuing to improve in the highest-income counties. From 2019 to 2023, CV mortality increased across all income groups, but the steepest rises occurred in the lowest-income quintiles. These findings highlight the urgent need to address rising CV mortality that is disproportionately impacting low-income, working-age adults.
More abstracts on this topic:
A Meta-analysis of Folic Acid Supplementation Efficacy in Cardiovascular Diseases Prevention.
Calderon Martinez Ernesto, Camacho Davila Karen Fabiola, Pinto-colmenarez Rafael, Arruarana Victor, Arvelaez Pascucci Joanne, Castillo Jaqueline Livier, Alonso Ramirez Angie Carolina, Ghattas Patricia, Giron De Marza Maria, Sosaya Zuñiga Briggitte Solange, Martinez Lilan Jonathan David, Paredes Romero Enrique
A Multicenter Study of Detection of Pulmonary Hypertension Based on Point-of-Care 12- Lead ECG DataDubrock Hilary, Wieczorek Mikolaj, Hackett Sarah, Alger Heather, Carlson Katherine, Klugherz Paul, Carter Rickey, Wagner Tyler, Johnson Patrick, Frantz Robert, Strom Jordan, Waks Jonathan, Agarwal Richa, Hemnes Anna, Steinberg Benjamin, Pandey Ambarish