Final ID: Mo4094
LL-37 autoantigen immune response differentiates myocardial infarction from other atherosclerotic cardiovascular disease phenotypes
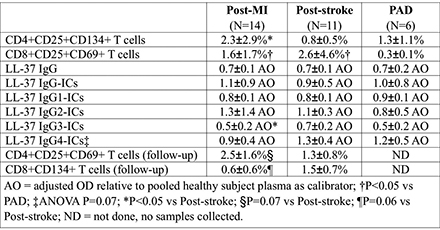
Abstract Body (Do not enter title and authors here): Background: Myocardial infarction (MI), stroke and peripheral artery disease (PAD) are viewed to have atherosclerosis as a common underlying pathology. Given the common underlying pathology, these atherosclerotic cardiovascular disease (ASCVD) phenotypes are thus expected to have shared immune responses to atherosclerosis-associated autoantigens. LL-37 is one such autoantigen that provokes a break in tolerance in acute coronary syndrome. Hypothesis: In this study, we hypothesized that ASCVD phenotypes MI, stroke and PAD will have a common immune profile directed against LL-37. Methods: PBMCs and plasma samples were collected from stable ASCVD patients enrolled within 12 months after myocardial infarction (MI) or stroke or diagnosed with peripheral artery disease (PAD). A subgroup of post-acute patients provided additional PBMCs at follow-up (14.7±3.6 months). PBMCs were stimulated with LL-37 and evaluated for activation induced markers by flow cytometry. Plasma levels of LL-37 IgG and LL-37 IgG-immune complexes (ICs) were tested using ELISA. LDL is a reported binding partner of LL-37 in plasma. Therefore, cross-reactivity of LL-37 IgG-ICs with native LL-37 or LL-37 complexed with LDL (LL-37_LDL) was assessed using immune depletion. Results: Post-MI patients had significantly increased CD4+CD25+CD134+ T cells in response to LL-37 stimulation compared to Post-stroke patients (Table 1). CD8+CD25+CD69+ T cells were significantly reduced in PAD patients in response to LL-37 compared to Post-MI and Post-stroke (Table 1). LL-37 IgG and LL-37 IgG-IC levels were comparable among the groups. However, IgG subclass analysis showed significantly reduced LL-37 IgG3-IC levels in Post-MI compared to Post-stroke, with a similar trend for LL-37 IgG4-IC levels (Table 1). Immune-depletion of plasma showed cross-reactivity of LL-37 IgG-ICs with both native LDL and LL-37_LDL in Post-MI while Post-stroke and PAD had cross-reactivity only with either one. At follow-up, CD4+CD25+CD69+ T cells were higher and CD8+CD134+ T cells were lower in Post-MI compared to Post-stroke patients. Conclusion: The differential immune profile among MI, stroke and PAD suggests the utility of profiling the immune response to LL-37 to differentiate ASCVD phenotypes and provides mechanistic insight.
More abstracts on this topic:
A major uremic toxin indoxyl sulfate impairs macrophage efferocytosis and accelerates atherogenesis: a potential mechanism for cardiovascular risk in chronic kidney disease
Jha Prabhash, Kasai Taku, Vromman Amelie, Holden Rachel, Libby Peter, Tabas Ira, Singh Sasha, Aikawa Elena, Aikawa Masanori, Lupieri Adrien, Sonawane Abhijeet, Le Thanh-dat, Becker-greene Dakota, Chelvanambi Sarvesh, Turner Mandy, Nakamura Yuto, Passos Livia
Altered inflammatory state and mitochondrial function identified by transcriptomics in paediatric congenital heart patients prior to surgical repairBartoli-leonard Francesca, Harris Amy, Caputo Massimo