Final ID: MP1759
Characteristics and outcomes of fetuses with intrauterine ductus arteriosus constriction.
Abstract Body (Do not enter title and authors here): Introduction:Fetal ductus arteriosus constriction (DAC) can cause hydrops, pulmonary arterial (PA) hypertension and even death. Maternal drug/dietary factors can cause DAC and resolve with withdrawal. Data on DAC postnatal outcomes is limited. In the current study we sought to explore the pre- and postnatal evolution and outcomes of DAC.
Methods: We identified all pregnancies with structurally normal hearts and DAC in our program from 2009-2024. Those with ductal systolic velocity >1.4 m/s, diastolic velocity >0.35 m/s, pulsatility index <1.9 were included. Fetal and neonatal clinical/echo parameters were collected. Right ventricular systolic dysfunction (RVDys) was defined as fractional area change (FAC) <35%.
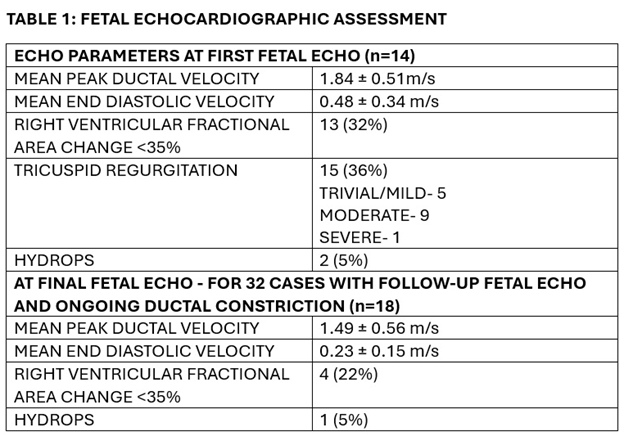
Results: Of 41 fetuses with DAC, 17(41%) were referred for suspected fetal heart disease. Only 7 (17%) had an identifiable cause (5 drug related, 2 dietary). See Table 1 for fetal echo data. At diagnosis 2 had hydrops (1 with a non-cardiac cause) and none developed hydrops at review. The majority (9/15, 60%) with tricuspid regurgitation had gradients >1/2 estimated systemic pressure. Four of 13 (31%) with RVDys received prenatal treatment (3 digoxin, 1 oxygen). Four fetuses had complete ductal closure (DC), all idiopathic and diagnosed at > 33 weeks gestational age (GA). Of 32 with serial fetal echo, 14(43%) had resolution of DAC, including 5 with known cause, and of 6 with RVDys, 3(50%) improved when the cause was discontinued and 4 had ongoing RVDys. The fetus with hydrops due to DAC was delivered urgently on presentation at 36 weeks GA. Two of the 4 with DC required urgent preterm delivery due to RVDys and abnormal venous Dopplers.
Postnatal data were available for 32(78%), all were admitted to the neonatal intensive care unit. One died from noncardiac causes. Three(9%) required invasive ventilation (including 2 with DC) and 18(56%) required CPAP. Only 2 received pulmonary vasodilators (2 nitric oxide, 1 sildenafil for <2 weeks).
Of 26(81%) postnatal echoes, 21(81%) had >1/2 systemic PA pressure at 1st echo, of whom 7(33%) normalized prior to discharge and a further 8(38%) on follow-up, with no follow up in 6(29%). Of 12 with prenatal RVDys and neonatal followup, all normalised by discharge. Five had genetic abnormalities and 9 had significant extracardiac pathologies.
CONCLUSIONS: Despite a worse trajectory in cases with idiopathic DAC, postnatal outcomes are favorable in both subsets with resolved RVDys and resolved PA hypertension in infancy.
Methods: We identified all pregnancies with structurally normal hearts and DAC in our program from 2009-2024. Those with ductal systolic velocity >1.4 m/s, diastolic velocity >0.35 m/s, pulsatility index <1.9 were included. Fetal and neonatal clinical/echo parameters were collected. Right ventricular systolic dysfunction (RVDys) was defined as fractional area change (FAC) <35%.
Results: Of 41 fetuses with DAC, 17(41%) were referred for suspected fetal heart disease. Only 7 (17%) had an identifiable cause (5 drug related, 2 dietary). See Table 1 for fetal echo data. At diagnosis 2 had hydrops (1 with a non-cardiac cause) and none developed hydrops at review. The majority (9/15, 60%) with tricuspid regurgitation had gradients >1/2 estimated systemic pressure. Four of 13 (31%) with RVDys received prenatal treatment (3 digoxin, 1 oxygen). Four fetuses had complete ductal closure (DC), all idiopathic and diagnosed at > 33 weeks gestational age (GA). Of 32 with serial fetal echo, 14(43%) had resolution of DAC, including 5 with known cause, and of 6 with RVDys, 3(50%) improved when the cause was discontinued and 4 had ongoing RVDys. The fetus with hydrops due to DAC was delivered urgently on presentation at 36 weeks GA. Two of the 4 with DC required urgent preterm delivery due to RVDys and abnormal venous Dopplers.
Postnatal data were available for 32(78%), all were admitted to the neonatal intensive care unit. One died from noncardiac causes. Three(9%) required invasive ventilation (including 2 with DC) and 18(56%) required CPAP. Only 2 received pulmonary vasodilators (2 nitric oxide, 1 sildenafil for <2 weeks).
Of 26(81%) postnatal echoes, 21(81%) had >1/2 systemic PA pressure at 1st echo, of whom 7(33%) normalized prior to discharge and a further 8(38%) on follow-up, with no follow up in 6(29%). Of 12 with prenatal RVDys and neonatal followup, all normalised by discharge. Five had genetic abnormalities and 9 had significant extracardiac pathologies.
CONCLUSIONS: Despite a worse trajectory in cases with idiopathic DAC, postnatal outcomes are favorable in both subsets with resolved RVDys and resolved PA hypertension in infancy.
More abstracts on this topic:
Artificial Intelligence in Non-Invasive Fetal ECG: A Systematic Review of Extraction and Analysis Techniques
Marouf Mahmoud, Daas Omar, Alrabadi Bassel, Refai Yamen, Badran Zaid, Bandak Natalie, Alshujaieh Nour, Abu-irsheid Loay
A Multicenter Friedreich Ataxia Registry Identifies Posterior Wall Thickness as a Predictor of Major Adverse Cardiac EventsLin Kimberly, Johnson Jonathan, Mccormack Shana, Lynch David, Tate Barbara, Feng Yixuan, Huang Jing, Mercer-rosa Laura, Dedio Anna, Mcsweeney Kara, Fournier Anne, Yoon Grace, Payne Ronald, Cripe Linda, Patel Aarti, Niaz Talha