Final ID: MP1050
The Valve That Wasn't: Unraveling a Diagnostic Mystery
Abstract Body (Do not enter title and authors here): Background
Dynamic left ventricular outflow tract (LVOT) obstruction can clinically and echocardiographically mimic aortic stenosis (AS). We report an elderly patient with presumed AS ultimately diagnosed with dynamic LVOT obstruction via invasive hemodynamic assessment, highlighting diagnostic pitfalls and management implications.
Case
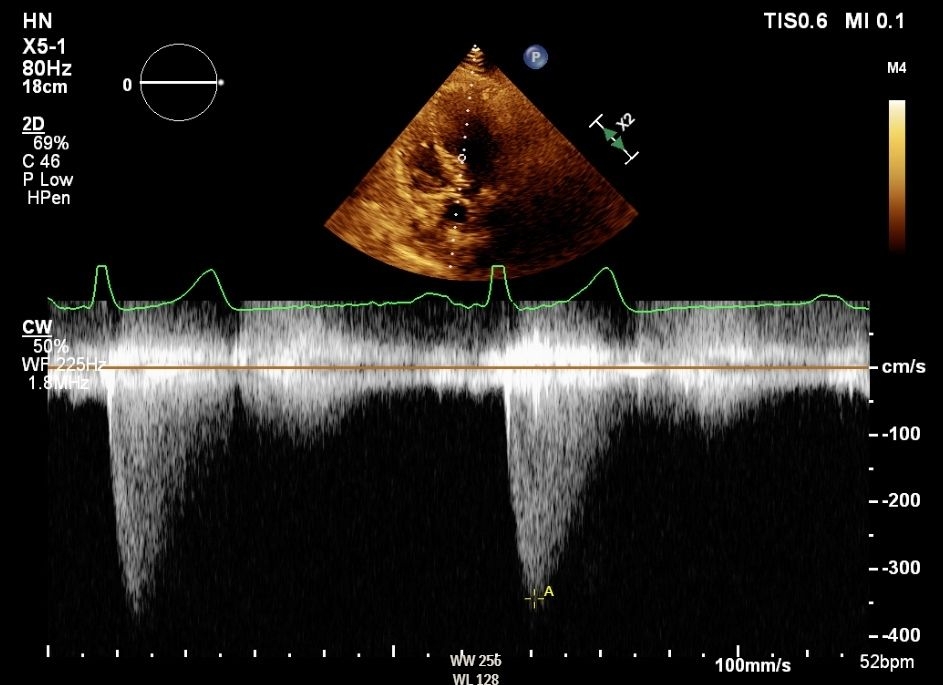
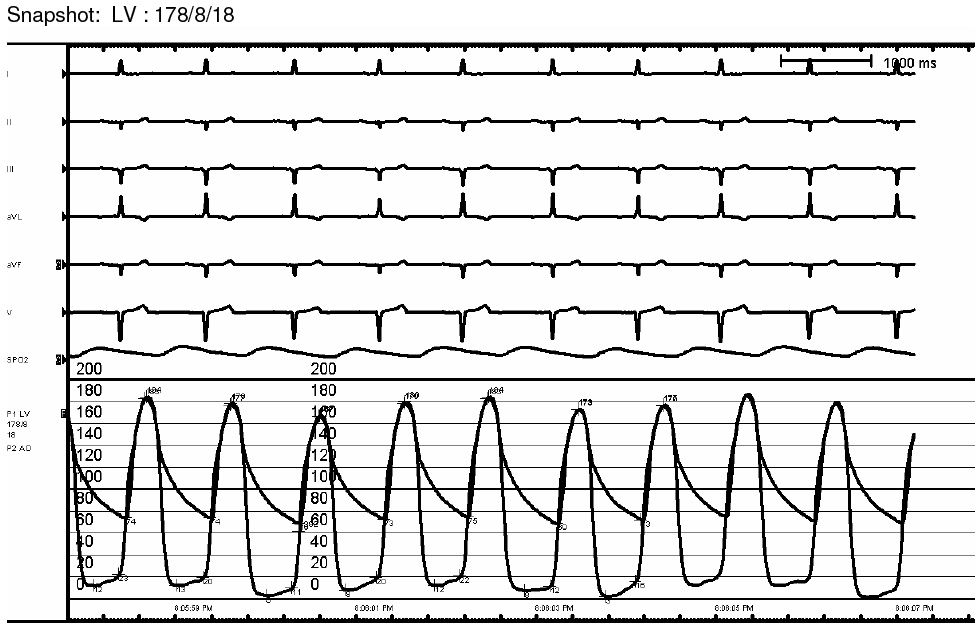
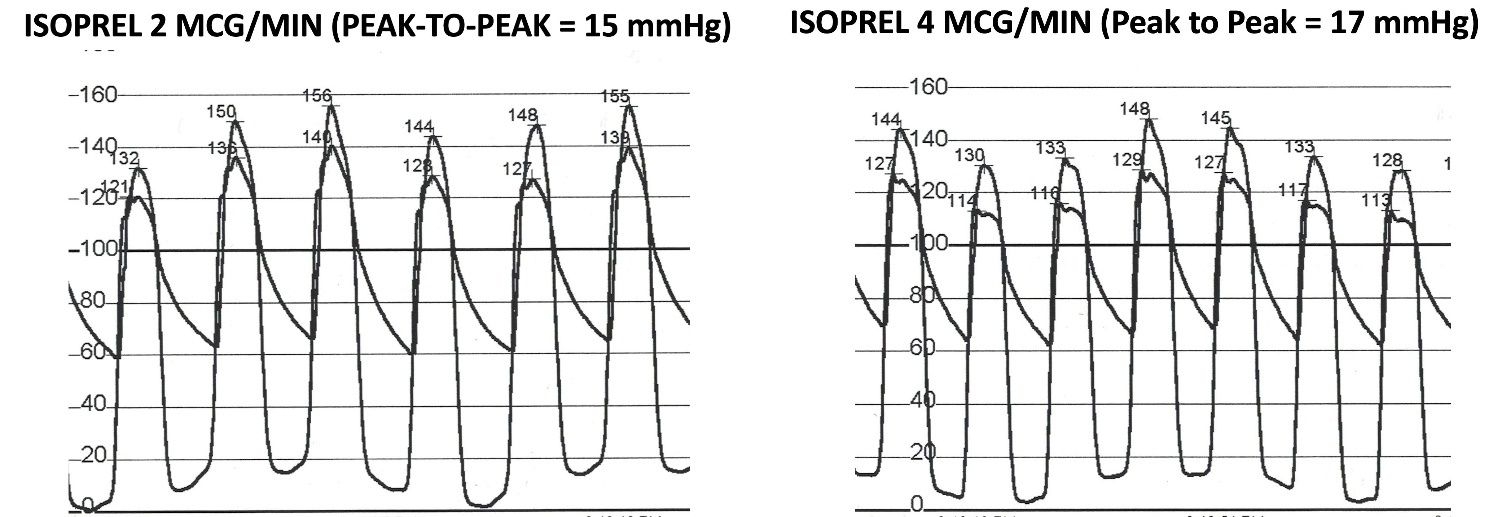
A 68-year-old male with history of hypertension was referred from another hospital for aortic valve (AV) replacement evaluation due to a few months of progressively worsening exertional chest pain and dyspnea. Exam was notable for a crescendo decrescendo systolic murmur; the patient was otherwise hemodynamically stable. ECG on arrival revealed left axis deviation and voltage criteria for left ventricular hypertrophy. Transthoracic echocardiography (TTE) report from the outside hospital mentioned “moderate to severe AS”. On admission repeat TTE revealed chordal systolic anterior motion with flow acceleration and significant LVOT pressure gradient up to 60-65mmHg while AV was hard to visualize but did not appear severely stenosed. Significant gradients were noted on continuous wave (CW) doppler of AV (Figure 1) while stepwise pulsed wave (PW) doppler was unrevealing. Based on obstructive physiology noted on TTE, therapy with a beta blocker was initiated. To further evaluate an invasive hemodynamic study was performed which did not reveal a resting gradient (Figure 2) however provocation with isoproterenol revealed LV-Ao (left ventricle to aorta) gradient which was higher with increasing doses (Figure 3). Furthermore, aortic waveform morphology and post PVC (premature ventricular contraction) response also revealed dynamic LVOT obstruction. Transducers were switched to verify findings and catheter pullback did not demonstrate any zero error. A final diagnosis of dynamic LVOT obstruction with no hemodynamically significant AV stenosis was made and patient was discharged on beta blockers with plan to consider septal reduction strategies if symptoms persist despite optimal medical therapy. He stayed asymptomatic and follow up echo did not reveal any gradient.
Discussion
This case highlights diagnostic limitations of noninvasive imaging especially with suboptimal valve visualization. In patients with equivocal TTE findings of AS and elevated LVOT pressure gradient, invasive hemodynamic testing with provocation maneuvers is essential to reach appropriate diagnosis to ensure targeted management and avoid unnecessary valve interventions.
Dynamic left ventricular outflow tract (LVOT) obstruction can clinically and echocardiographically mimic aortic stenosis (AS). We report an elderly patient with presumed AS ultimately diagnosed with dynamic LVOT obstruction via invasive hemodynamic assessment, highlighting diagnostic pitfalls and management implications.
Case
A 68-year-old male with history of hypertension was referred from another hospital for aortic valve (AV) replacement evaluation due to a few months of progressively worsening exertional chest pain and dyspnea. Exam was notable for a crescendo decrescendo systolic murmur; the patient was otherwise hemodynamically stable. ECG on arrival revealed left axis deviation and voltage criteria for left ventricular hypertrophy. Transthoracic echocardiography (TTE) report from the outside hospital mentioned “moderate to severe AS”. On admission repeat TTE revealed chordal systolic anterior motion with flow acceleration and significant LVOT pressure gradient up to 60-65mmHg while AV was hard to visualize but did not appear severely stenosed. Significant gradients were noted on continuous wave (CW) doppler of AV (Figure 1) while stepwise pulsed wave (PW) doppler was unrevealing. Based on obstructive physiology noted on TTE, therapy with a beta blocker was initiated. To further evaluate an invasive hemodynamic study was performed which did not reveal a resting gradient (Figure 2) however provocation with isoproterenol revealed LV-Ao (left ventricle to aorta) gradient which was higher with increasing doses (Figure 3). Furthermore, aortic waveform morphology and post PVC (premature ventricular contraction) response also revealed dynamic LVOT obstruction. Transducers were switched to verify findings and catheter pullback did not demonstrate any zero error. A final diagnosis of dynamic LVOT obstruction with no hemodynamically significant AV stenosis was made and patient was discharged on beta blockers with plan to consider septal reduction strategies if symptoms persist despite optimal medical therapy. He stayed asymptomatic and follow up echo did not reveal any gradient.
Discussion
This case highlights diagnostic limitations of noninvasive imaging especially with suboptimal valve visualization. In patients with equivocal TTE findings of AS and elevated LVOT pressure gradient, invasive hemodynamic testing with provocation maneuvers is essential to reach appropriate diagnosis to ensure targeted management and avoid unnecessary valve interventions.
More abstracts on this topic:
A Remedy for the Heart and the Hemoglobin: Improvement in Anemia Post Transcatheter Aortic Valve Replacement
Matta Raghav, Roy Aanya, Hammad Bayan, Draffen Arvind, Natsheh Zachary, Tiu Daniel, Tiu David, Salem Edward, Balami Jesse, Kalagara Swetha, Gupta Neil, Uraizee Omar, Sahgal Savina, Mishra Atreya, Ene Adriana, Hattab Aleyah, Arora Aarushi, Sufyaan Humam, Dau Trang, Silberstein Jonathan, Yu Julia, Torres Kayla, Seshadri Suhas, Navarro Laura, Singam Manisha, Ismail Mariam, Rana Riya, Habeel Samer, Liu Simon, Chaganti Srinidhi, Gurbuxani Vidur, Dwyer Kaluzna Stephanie, Groo Vicki, Carlson Andrew, Shroff Adhir, Bhayani Siddharth, Khan Azmer, Bhattaram Rohan, Zhang Runze, Shah Pal
A Novel Cardiac Simulator "ped UT-Heart" to Support Decision-Making in Surgical Procedures for Complex Congenital Heart DiseaseShiraishi Isao, Kurosaki Kenichi, Iwai Shigemitsu, Washio Takumi, Sugiura Seiryo, Hisada Toshiaki