Final ID: MP114
Beyond the Periphery: Coronary Endothelial Dysfunction as a Distinct Marker of Cardiovascular Risk in HIV
Abstract Body (Do not enter title and authors here): Background: People living with HIV (PLWH) have an increased risk of cardiovascular events compared to persons without HIV (PWoH), even with optimal control of their infection with antiretroviral therapy. Coronary endothelial dysfunction is a known early marker of atherosclerosis and a predictor of adverse cardiovascular outcomes, and prior studies have demonstrated that coronary endothelial function (CEF) is impaired in PLWH. While systemic endothelial function is often used as a surrogate for CEF, it remains unclear whether PLWH also demonstrate worse systemic endothelial dysfunction compared with PWoH.
Research Question: How does systemic endothelial function differ between PLWH and PWoH? Is there an association between systemic endothelial function and CEF in PLWH?
Methods: PLWH and PWoH controls without known coronary artery disease (CAD) were prospectively enrolled in a cross-sectional study. CEF was quantified using cardiac magnetic resonance imaging to measure change in coronary cross-sectional area (CSA) and coronary blood flow (CBF) in response to isometric handgrip exercise. Systemic endothelial function was measured by reactive hyperemia index (RHI) using peripheral arterial tonometry (EndoPAT) device. Differences in endothelial function were assessed using independent samples t-tests, with a two-sided p-value < 0.05 considered statistically significant.
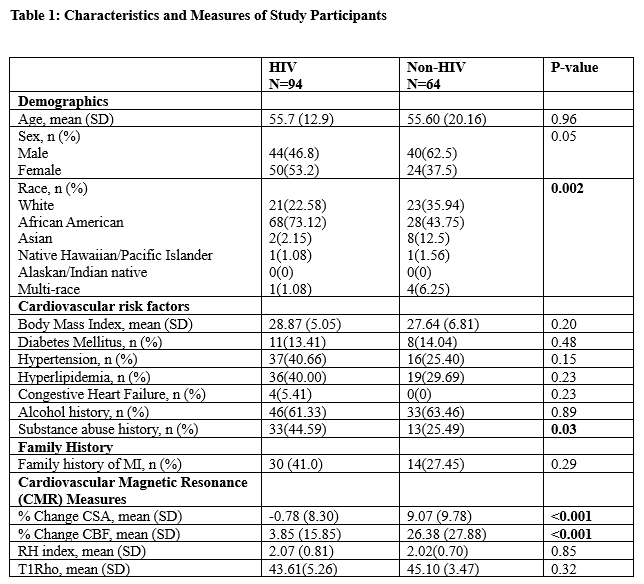
Results: Of the 158 participants, 94 were PLWH and 64 were age- and sex-matched controls. CEF was significantly reduced in PLWH compared to controls despite absence of CAD. The mean percent change in CSA was –0.78% (SD 8.30) in PLWH vs 9.07% (SD 9.78) in controls (p < 0.001), and the mean percent change in CBF was 3.85% (SD 15.85) vs 26.38% (SD 27.88), respectively (p < 0.001). In contrast, there was no significant difference in RHI between PLWH and controls (mean RHI: 2.07 [SD 0.81] vs 2.02 [SD 0.70], p = 0.85).
Conclusion: PLWH demonstrated impaired CEF compared to PWoH while there was no difference in systemic endothelial function between the two groups. This potentially highlights the limitation of systemic vascular measures in detecting coronary-specific endothelial impairment in PLWH. These findings suggest the importance of targeted coronary assessments in evaluating cardiovascular risk in PLWH.
Research Question: How does systemic endothelial function differ between PLWH and PWoH? Is there an association between systemic endothelial function and CEF in PLWH?
Methods: PLWH and PWoH controls without known coronary artery disease (CAD) were prospectively enrolled in a cross-sectional study. CEF was quantified using cardiac magnetic resonance imaging to measure change in coronary cross-sectional area (CSA) and coronary blood flow (CBF) in response to isometric handgrip exercise. Systemic endothelial function was measured by reactive hyperemia index (RHI) using peripheral arterial tonometry (EndoPAT) device. Differences in endothelial function were assessed using independent samples t-tests, with a two-sided p-value < 0.05 considered statistically significant.
Results: Of the 158 participants, 94 were PLWH and 64 were age- and sex-matched controls. CEF was significantly reduced in PLWH compared to controls despite absence of CAD. The mean percent change in CSA was –0.78% (SD 8.30) in PLWH vs 9.07% (SD 9.78) in controls (p < 0.001), and the mean percent change in CBF was 3.85% (SD 15.85) vs 26.38% (SD 27.88), respectively (p < 0.001). In contrast, there was no significant difference in RHI between PLWH and controls (mean RHI: 2.07 [SD 0.81] vs 2.02 [SD 0.70], p = 0.85).
Conclusion: PLWH demonstrated impaired CEF compared to PWoH while there was no difference in systemic endothelial function between the two groups. This potentially highlights the limitation of systemic vascular measures in detecting coronary-specific endothelial impairment in PLWH. These findings suggest the importance of targeted coronary assessments in evaluating cardiovascular risk in PLWH.
More abstracts on this topic:
Acetylation of Mitochondrial Cyclophilin D Increases vascular Oxidative Stress, Induces Glycolitic Switch, Promotes Endothelial Dysfunction and Hypertension
Dikalov Sergey, Sack Michael, Dikalova Anna, Fehrenbach Daniel, Mayorov Vladimir, Panov Alexander, Ao Mingfang, Lantier Louise, Amarnath Venkataraman, Lopez Marcos, Billings Frederic
A Functional Coronary Artery Disease Risk Variant at 3q25.31 Disrupts TEAD-Mediated Regulation of TIPARP in Vascular Smooth Muscle CellsBahia Gurmenjit, Kim Juyong