Final ID: Su2107
Clinical Outcomes of Postoperative Atrial Fibrillation Following Non-Cardiovascular Procedures: A Three-Year Study
Abstract Body (Do not enter title and authors here): Background
Postoperative atrial fibrillation (AF) is common, often brief, and may recur, with some studies reporting a recurrence rate lower than 30% at one year. The initiation of anticoagulation (AC) in these patients, particularly those at lower stroke risk, remains debatable due to insufficient evidence. This study aims to assess outcomes in postoperative non-cardiovascular procedures with acute AF, focusing on patients at lower stroke risk, comparing those treated with and without AC.
Method
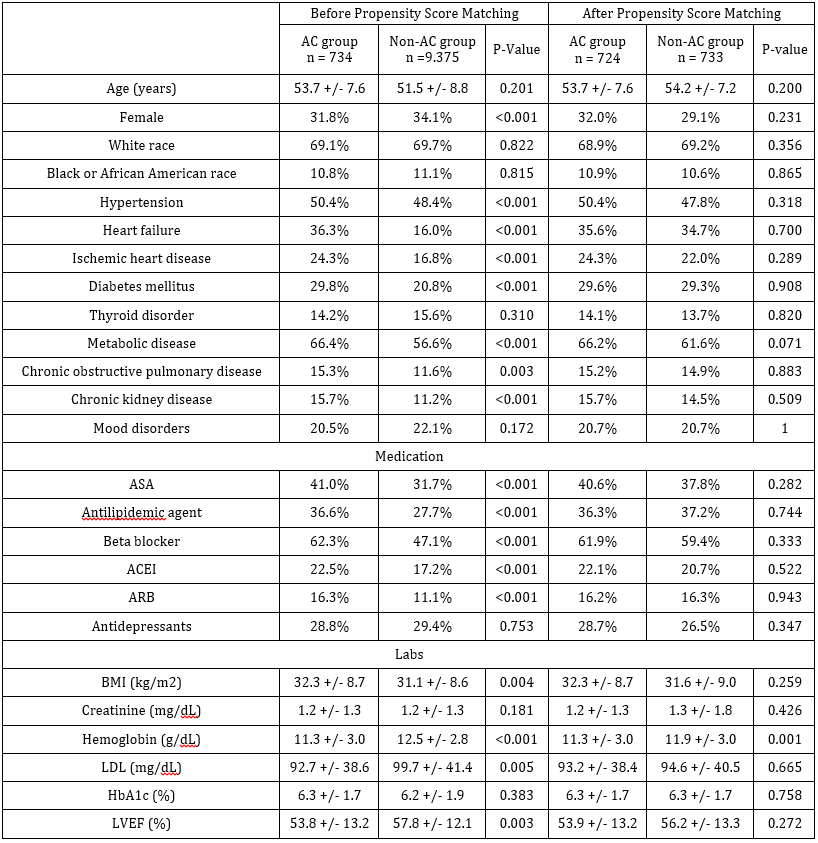
Using the TriNetX database, we identified patients aged 18 to 64 years with new-onset AF following non-cardiovascular procedures, excluding those with a history of stroke or other indications for anticoagulation. Patients were divided into AC and Non-AC groups based on AC initiation within two weeks of AF onset, then followed for three years. Propensity score matching (PSM) balanced confounders between groups. Thromboembolic and bleeding outcomes were assessed.
Results
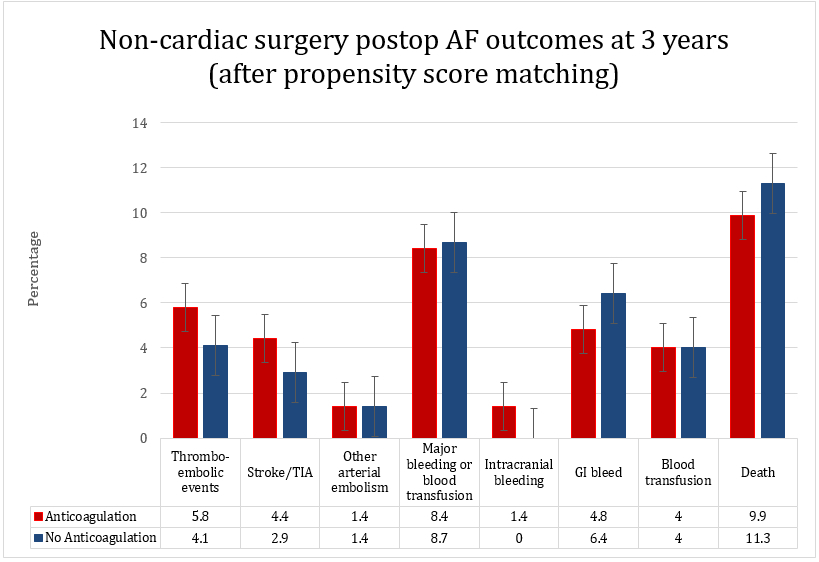
Among 10,108 patients, 734 (7%) received anticoagulation within two weeks of postop AF. After PSM, mean ages were 53.7±7.6 years for the AC group and 54.2±7.17 years for the Non-AC group. At 3 years, the incidence of composite thromboembolic events did not significantly differ between AC and Non-AC groups (5.8% vs. 4.1%, OR 0.70 (95% CI: 0.43-1.14)). Most thromboembolic events occurred within one month of AF onset. There were no significant differences in the composite of intracranial bleeding, gastrointestinal bleeding, retroperitoneal bleeding, or need for blood transfusion between the AC and Non-AC groups at 3 years (OR 1.04 (95% CI 0.72-1.50)).
Conclusion
At three years, there is no significant difference in thromboembolic and bleeding outcomes in patients undergoing non-cardiovascular procedures who develop new-onset AF. Further randomized controlled trial is needed to determine the necessity of anticoagulation in this patient population.
Postoperative atrial fibrillation (AF) is common, often brief, and may recur, with some studies reporting a recurrence rate lower than 30% at one year. The initiation of anticoagulation (AC) in these patients, particularly those at lower stroke risk, remains debatable due to insufficient evidence. This study aims to assess outcomes in postoperative non-cardiovascular procedures with acute AF, focusing on patients at lower stroke risk, comparing those treated with and without AC.
Method
Using the TriNetX database, we identified patients aged 18 to 64 years with new-onset AF following non-cardiovascular procedures, excluding those with a history of stroke or other indications for anticoagulation. Patients were divided into AC and Non-AC groups based on AC initiation within two weeks of AF onset, then followed for three years. Propensity score matching (PSM) balanced confounders between groups. Thromboembolic and bleeding outcomes were assessed.
Results
Among 10,108 patients, 734 (7%) received anticoagulation within two weeks of postop AF. After PSM, mean ages were 53.7±7.6 years for the AC group and 54.2±7.17 years for the Non-AC group. At 3 years, the incidence of composite thromboembolic events did not significantly differ between AC and Non-AC groups (5.8% vs. 4.1%, OR 0.70 (95% CI: 0.43-1.14)). Most thromboembolic events occurred within one month of AF onset. There were no significant differences in the composite of intracranial bleeding, gastrointestinal bleeding, retroperitoneal bleeding, or need for blood transfusion between the AC and Non-AC groups at 3 years (OR 1.04 (95% CI 0.72-1.50)).
Conclusion
At three years, there is no significant difference in thromboembolic and bleeding outcomes in patients undergoing non-cardiovascular procedures who develop new-onset AF. Further randomized controlled trial is needed to determine the necessity of anticoagulation in this patient population.
More abstracts on this topic:
1-Year Outcomes After Cardioversion With and Without Anticoagulation in Patients With Left Atrial Appendage Occlusion: A Propensity-Matched Analysis
Thangjui Sittinun, Trongtorsak Angkawipa, Kewcharoen Jakrin, Thyagaturu Harshith, Watson Hangyu, Mensah Samuel, Balla Sudarshan, Navaravong Leenhapong
A novel risk score predicts the prevalence of left atrial low-voltage areas and rhythm outcome in patients undergoing long-standing persistent atrial fibrillation ablationOoka Hirotaka, Nakao Sho, Kusuda Masaya, Ariyasu Wataru, Kudo Satoshi, Fujii Subaru, Mano Toshiaki, Matsuda Yasuhiro, Masuda Masaharu, Okamoto Shin, Ishihara Takayuki, Nanto Kiyonori, Tsujimura Takuya, Hata Yosuke, Uematsu Hiroyuki