Final ID: TAC115
Utilization and Cost Trends in Remote Patient Monitoring for Hypertension in the United States (2020-2022)
Abstract Body: Introduction
Self-measured blood pressure (SMBP) and remote patient monitoring (RPM; SMBP with readings wirelessly integrated into the electronic health record) improve BP control. Medicare introduced billing codes for SMBP (2020) and RPM (2019) to promote these services. This study aimed to assess use, reimbursement, and patient costs related to SMBP and RPM billing codes in enrollees with hypertension (HTN).
Methods
We examined outpatient claims from 2020 to 2022 in the Merative-MarketScan Database to identify SMBP and RPM claims in enrollees with and without an associated HTN diagnosis. The analysis included individuals with Commercial, Medicaid, and Medicare coverage, and excluded those with capitated plans. Descriptive statistics were used to assess the number of claims for SMBP or RPM per month, gross reimbursement by insurers, and patient out-of-pocket costs. Claims with zero gross payment, net payment, and out-of-pocket costs were considered denied and were excluded from median cost analyses.
Results
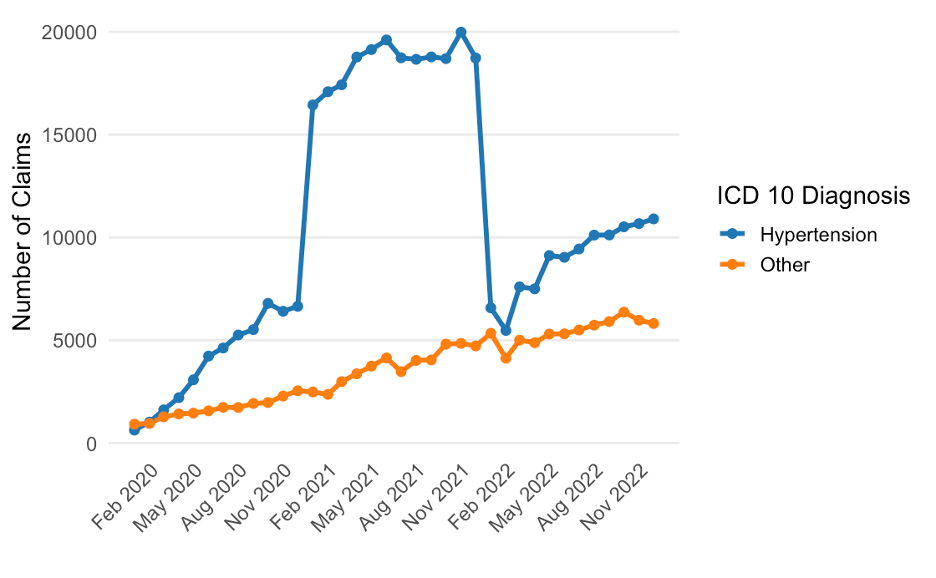
From 2020 to 2022, out of nearly 40 million eligible enrollees in the Merative database, only 1,682 had >1 SMBP billing code vs 36,774 with >1 RPM code associated with HTN. By the end of 2022, monthly RPM claims for HTN were roughly double those of all other diagnoses combined (Figure). A spike in RPM HTN claims in 2021 was driven by a transient increase in billing using CPT code 99091 in commercially insured patients. Median reimbursement per SMBP claim ranged from $9.45 (Medicaid) to $16.41 (Commercial). Median reimbursement per RPM HTN claim ranged from $14.30 (Medicaid) to $50.78 (Medicare). Median patient out-of-pocket costs for SMBP claims ranged from $0 (Medicaid) to $2.07 (Commercial). Median out-of-pocket cost for RPM HTN claims ranged from $0 (Medicaid) to $4.77 (Medicare). Overall, 5.5% of SMBP claims and 30.6% of RPM HTN claims were denied.
Conclusion
From 2020 and 2022, SMBP billing codes were infrequently used compared to RPM codes in enrollees with HTN. This may reflect low reimbursement or cumbersome requirements for SMBP billing. The greater growth in claims for RPM HTN suggests that the greater payment for RPM codes was incentivizing greater adoption of RPM HTN relative to SMBP. Future studies should examine the cost-effectiveness of RPM HTN and trends in RPM HTN billing following the expiration of telemedicine regulations related to the COVID-19 pandemic in 2023 that temporarily reduced RPM HTN billing requirements and waived co-pays.
Self-measured blood pressure (SMBP) and remote patient monitoring (RPM; SMBP with readings wirelessly integrated into the electronic health record) improve BP control. Medicare introduced billing codes for SMBP (2020) and RPM (2019) to promote these services. This study aimed to assess use, reimbursement, and patient costs related to SMBP and RPM billing codes in enrollees with hypertension (HTN).
Methods
We examined outpatient claims from 2020 to 2022 in the Merative-MarketScan Database to identify SMBP and RPM claims in enrollees with and without an associated HTN diagnosis. The analysis included individuals with Commercial, Medicaid, and Medicare coverage, and excluded those with capitated plans. Descriptive statistics were used to assess the number of claims for SMBP or RPM per month, gross reimbursement by insurers, and patient out-of-pocket costs. Claims with zero gross payment, net payment, and out-of-pocket costs were considered denied and were excluded from median cost analyses.
Results
From 2020 to 2022, out of nearly 40 million eligible enrollees in the Merative database, only 1,682 had >1 SMBP billing code vs 36,774 with >1 RPM code associated with HTN. By the end of 2022, monthly RPM claims for HTN were roughly double those of all other diagnoses combined (Figure). A spike in RPM HTN claims in 2021 was driven by a transient increase in billing using CPT code 99091 in commercially insured patients. Median reimbursement per SMBP claim ranged from $9.45 (Medicaid) to $16.41 (Commercial). Median reimbursement per RPM HTN claim ranged from $14.30 (Medicaid) to $50.78 (Medicare). Median patient out-of-pocket costs for SMBP claims ranged from $0 (Medicaid) to $2.07 (Commercial). Median out-of-pocket cost for RPM HTN claims ranged from $0 (Medicaid) to $4.77 (Medicare). Overall, 5.5% of SMBP claims and 30.6% of RPM HTN claims were denied.
Conclusion
From 2020 and 2022, SMBP billing codes were infrequently used compared to RPM codes in enrollees with HTN. This may reflect low reimbursement or cumbersome requirements for SMBP billing. The greater growth in claims for RPM HTN suggests that the greater payment for RPM codes was incentivizing greater adoption of RPM HTN relative to SMBP. Future studies should examine the cost-effectiveness of RPM HTN and trends in RPM HTN billing following the expiration of telemedicine regulations related to the COVID-19 pandemic in 2023 that temporarily reduced RPM HTN billing requirements and waived co-pays.
More abstracts on this topic:
Arterial Stiffness Mechanisms and Orthostatic Hypotension in The Systolic Blood Pressure Intervention Trial
Gepner Adam, Jaeger Byron, Hughes Timothy, Upadhya Bharathi, Kitzman Dalane, Supiano Mark, Pewowaruk Ryan
A machine learning model for individualized risk prediction of ischemic heart disease in people with hypertension in ThailandSakboonyarat Boonsub, Poovieng Jaturon, Rangsin Ram